Abstract
BACKGROUND:
Skeletal muscles play many important roles in the human body and any malfunction or disorder of the skeletal muscles can lead to a reduced quality of life. Some skeletal dysfunctions are acquired, such as sarcopenia but others are congenital. Duchenne muscular dystrophy (DMD) is one of the most common forms of hereditary muscular dystrophy and is caused by a deficiency of the protein, Dystrophin. Currently, there is no clear treatment for DMD, there are only methods that can alleviate the symptoms of the disease. Mesenchymal stem cells, including tonsil-derived mesenchymal stem cells (TMSCs) have been shown to differentiate into skeletal muscle cells (TMSC-myocyte) and can be one of the resources for the treatment of DMD. Skeletal muscle cell characteristics of TMSC-myocytes have been confirmed through changes in morphology and expression of skeletal muscle markers such as Myogenin, Myf6, and MYH families after differentiation.
MEOTHDS:
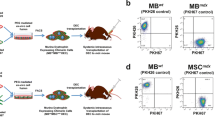
Based on these characteristics, TMSC-myocytes have been transplanted into mdx mice, a mouse model of DMD, to investigate whether they can help improve the symptoms of DMD. The red fluorescent protein gene was transduced into TMSC (TMSC-R) for tracking transplanted cells.
RESULTS:
Prior to transplantation (TP), it was confirmed whether TMSC-R-myocytes had the same differentiation potential as TMSC-myocytes. Increased expression of dystrophin and autophagy markers in the TP group compared with the sham group was confirmed in the gastrocnemius muscle 12 weeks after TP.
CONCLUSION:
These results demonstrate muscle regeneration and functional recovery of mdx via autophagy activation following TMSC-myocyte TP.







Similar content being viewed by others
References
Sui SX, Williams LJ, Holloway-Kew KL, Hyde KN, Pasco JA. Skeletal muscle health and cognitive function: a narrative review. Int J Mol Sci. 2021;22:255.
Yamakawa H, Kusumoto D, Hashimoto H, Yuasa S. Stem cell aging in skeletal muscle regeneration and disease. Int J Mol Sci. 2020;21:1830.
Truskey GA. Development and application of human skeletal muscle microphysiological systems. Lab Chip. 2018;18:3061–73.
Park S, Choi Y, Jung N, Yu Y, Ryu KH, Kim HS, et al. Myogenic differentiation potential of human tonsil-derived mesenchymal stem cells and their potential for use to promote skeletal muscle regeneration. Int J Mol Med. 2016;37:1209–20.
Nakamura Y, Miyaki S, Ishitobi H, Matsuyama S, Nakasa T, Kamei N, et al. Mesenchymal-stem-cell-derived exosomes accelerate skeletal muscle regeneration. FEBS Lett. 2015;589:1257–65.
Wang QQ, Jing XM, Bi YZ, Cao XF, Wang YZ, Li YX, et al. Human umbilical cord Wharton’s jelly derived mesenchymal stromal cells may attenuate sarcopenia in aged mice induced by hindlimb suspension. Med Sci Monit. 2018;24:9272–81.
Oh SY, Choi YM, Kim HY, Park YS, Jung SC, Park JW, et al. Application of tonsil-derived mesenchymal stem cells in tissue regeneration: concise review. Stem Cells. 2019;37:1252–60.
Yu Y, Park YS, Kim HS, Kim HY, Jin YM, Jung SC, et al. Characterization of long-term in vitro culture-related alterations of human tonsil-derived mesenchymal stem cells: role for CCN1 in replicative senescence-associated increase in osteogenic differentiation. J Anat. 2014;225:510–8.
Lee HJ, Jung H, Kim DK. IDO and CD40 may be key molecules for immunomodulatory capacity of the primed tonsil-derived mesenchymal stem cells. Int J Mol Sci. 2021;22:5772.
Yiu EM, Kornberg AJ. Duchenne muscular dystrophy. J Paediatr Child Health. 2015;51:759–64.
Spurney CF, Gordish-Dressman H, Guerron AD, Sali A, Pandey GS, Rawat R, et al. Preclinical drug trials in the mdx mouse: assessment of reliable and sensitive outcome measures. Muscle Nerve. 2009;39:591–602.
Rooney JE, Gurpur PB, Burkin DJ. Laminin-111 protein therapy prevents muscle disease in the mdx mouse model for Duchenne muscular dystrophy. Proc Natl Acad Sci U S A. 2009;106:7991–6.
Aminzadeh MA, Rogers RG, Fournier M, Tobin RE, Guan X, Childers MK, et al. Exosome-mediated benefits of cell therapy in mouse and human models of Duchenne muscular dystrophy. Stem Cell Reports. 2018;10:942–55.
Bengtsson NE, Hall JK, Odom GL, Phelps MP, Andrus CR, Hawkins RD, et al. Muscle-specific CRISPR/Cas9 dystrophin gene editing ameliorates pathophysiology in a mouse model for Duchenne muscular dystrophy. Nat Commun. 2017;8:14454.
Parzych KR, Klionsky DJ. An overview of autophagy: morphology, mechanism, and regulation. Antioxid Redox Signal. 2014;20:460–73.
Fiacco E, Castagnetti F, Bianconi V, Madaro L, De Bardi M, Nazio F, D’Amico A, Bertini E, Cecconi F, Puri PL, Latella L. Autophagy regulates satellite cell ability to regenerate normal and dystrophic muscles. Cell Death Differ. 2016;23:1839–49.
De Palma C, Morisi F, Cheli S, Pambianco S, Cappello V, Vezzoli M, et al. Autophagy as a new therapeutic target in Duchenne muscular dystrophy. Cell Death Dis. 2012;3:e418.
Whitehead NP, Kim MJ, Bible KL, Adams ME, Froehner SC. A new therapeutic effect of simvastatin revealed by functional improvement in muscular dystrophy. Proc Natl Acad Sci U S A. 2015;112:12864–9.
Rubinsztein DC, Marino G, Kroemer G. Autophagy and aging. Cell. 2011;146:682–95.
Schiaffino S, Rossi AC, Smerdu V, Leinwand LA, Reggiani C. Developmental myosins: expression patterns and functional significance. Skelet Muscle. 2015;5:22.
Hernández-Hernández JM, García-González EG, Brun CE, Rudnicki MA. The myogenic regulatory factors, determinants of muscle development, cell identity and regeneration. Semin Cell Dev Biol. 2017;72:10–8.
Farini A, Sitzia C, Villa C, Cassani B, Tripodi L, Legato M, et al. Defective dystrophic thymus determines degenerative changes in skeletal muscle. Nat Commun. 2021;12:2099.
Masiero E, Agatea L, Mammucari C, Blaauw B, Loro E, Komatsu M, et al. Autophagy is required to maintain muscle mass. Cell Metab. 2009;10:507–15.
Klionsky DJ, Abdel-Aziz AK, Abdelfatah S, Abdellatif M, Abdoli A, Abel S, et al. Guidelines for the use and interpretation of assays for monitoring autophagy (4th edition). Autophagy. 2021;17:1–382.
van Putten M, Putker K, Overzier M, Adamzek WA, Pasteuning-Vuhman S, Plomp JJ, et al. Natural disease history of the D2 -mdx mouse model for Duchenne muscular dystrophy. FASEB J. 2019;33:8110–24.
Sun C, Shen L, Zhang Z, Xie X. Therapeutic strategies for Duchenne muscular dystrophy: an update. Genes (Basel). 2020;11:837.
Yao S, Chen Z, Yu Y, Zhang N, Jiang H, Zhang G, et al. Current pharmacological strategies for duchenne muscular dystrophy. Front Cell Dev Biol. 2021;9:689533.
Happi Mbakam C, Lamothe G, Tremblay JP. Therapeutic strategies for dystrophin replacement in duchenne muscular dystrophy. Front Med (Lausanne). 2022;9:859930.
Jung N, Park S, Choi Y, Park JW, Hong YB, Park HH, et al. Tonsil-derived mesenchymal stem cells differentiate into a Schwann cell phenotype and promote peripheral nerve regeneration. Int J Mol Sci. 2016;17:1867.
Kim JY, Park S, Oh SY, Nam YH, Choi YM, Choi Y, et al. Density-dependent differentiation of tonsil-derived mesenchymal stem cells into parathyroid-hormone-releasing cells. Int J Mol Sci. 2022;23:715.
Park S, Choi Y, Kwak G, Hong YB, Jung N, Kim J, et al. Application of differentiated human tonsil-derived stem cells to trembler-J mice. Muscle Nerve. 2018;57:478–86.
Bansal V, De D, An J, Kang TM, Jeong HJ, Kang JS, et al. Chemical induced conversion of mouse fibroblasts and human adipose-derived stem cells into skeletal muscle-like cells. Biomaterials. 2019;193:30–46.
Chen W, Xie M, Yang B, Bharadwaj S, Song L, Liu G, et al. Skeletal myogenic differentiation of human urine-derived cells as a potential source for skeletal muscle regeneration. J Tissue Eng Regen Med. 2017;11:334–41.
Ganassi M, Badodi S, Wanders K, Zammit PS, Hughes SM. Myogenin is an essential regulator of adult myofibre growth and muscle stem cell homeostasis Elife. 2020;9:e60445.
Tajsharghi H, Oldfors A. Myosinopathies: pathology and mechanisms. Acta Neuropathol. 2013;125:3–18.
Herzog W. The role of titin in eccentric muscle contraction. J Exp Biol. 2014;217:2825–33.
Guo Y, Xiao P, Lei S, Deng F, Xiao GG, Liu Y, et al. How is mRNA expression predictive for protein expression? A correlation study on human circulating monocytes. Acta Biochim Biophys Sin (Shanghai). 2008;40:426–36.
Li J, Zhang Y. Li J, Zhang Y, Yang C, Rong R. Discrepant mRNA and protein expression in immune cells. Curr Genomics. 2020;21:560–3.
Yu J, Su X, Zhu C, Pan Q, Yang J, Ma J, et al. GFP labeling and hepatic differentiation potential of human placenta-derived mesenchymal stem cells. Cell Physiol Biochem. 2015;35:2299–308.
Islam I, Sriram G, Li M, Zou Y, Li L, Handral HK, et al. In Vitro osteogenic potential of green fluorescent protein labelled human embryonic stem cell-derived osteoprogenitors. Stem Cells Int. 2016;2016:1659275.
Swist S, Unger A, Li Y, Vöge A, von Frieling-Salewsky M, Skärlén Å. Maintenance of sarcomeric integrity in adult muscle cells crucially depends on Z-disc anchored titin. Nat Commun. 2020;11:4479.
Moorwood C, Barton ER. Caspase-12 ablation preserves muscle function in the mdx mouse. Hum Mol Genet. 2014;23:5325–41.
Odom GL, Gregorevic P, Allen JM, Finn E, Chamberlain JS. Microutrophin delivery through rAAV6 increases lifespan and improves muscle function in dystrophic dystrophin/utrophin-deficient mice. Mol Ther. 2008;16:1539–45.
Klyen BR, Shavlakadze T, Radley-Crabb HG, Grounds MD, Sampson DD. Identification of muscle necrosis in the mdx mouse model of duchenne muscular dystrophy using three-dimensional optical coherence tomography. J Biomed Opt. 2011;16:076013.
Park S, Choi Y, Jung N, Kim J, Oh S, Yu Y, et al. Autophagy induction in the skeletal myogenic differentiation of human tonsil-derived mesenchymal stem cells. Int J Mol Med. 2017;39:831–40.
Zhang Y, Zhang Y, Jin XF, Zhou XH, Dong XH, Yu WT, et al. The role of astragaloside IV against cerebral ischemia/reperfusion injury: suppression of apoptosis via promotion of p62-LC3-autophagy. Molecules. 2019;24:1838.
Decuypere JP, Parys JB, Bultynck G. Regulation of the autophagic bcl-2/beclin 1 interaction. Cells. 2012;1:284–312.
Jiang P, Mizushima N. LC3- and p62-based biochemical methods for the analysis of autophagy progression in mammalian cells. Methods. 2015;75:13–8.
Acknowledgements
This study was supported by a grant from the Bio & Medical Technology Development Program of the National Research Foundation of Korea (NRF) funded by the Ministry of Science & ICT (grant number, 2017M3A9B3063636), the Basic Science Research Pro-gram through the NRF funded by the Ministry of Education (2019R1I1A1A01060308) and the RP-Grant 2021 of Ewha Womans University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
The authors declare no conflict of interest.
Ethical statement
The study protocol was approved by the Ewha Womans University Medical Center (EWUMC) institutional review board (IRB number: ECT-2011–09-003). All the experimental procedures were reviewed and approved by the ethics committee for animal research at Ewha Woman’s University (EUM20-051). Informed Consent Statement: Informed written consent was obtained from all the patients participating in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Park, S., Jeong, S., Nam, Y.H. et al. Transplantation of Differentiated Tonsil-Derived Mesenchymal Stem Cells Ameliorates Murine Duchenne Muscular Dystrophy via Autophagy Activation. Tissue Eng Regen Med 19, 1283–1294 (2022). https://doi.org/10.1007/s13770-022-00489-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13770-022-00489-7