Abstract
Background
Weight loss, which is an effective method for reducing visceral fat, may cause a concomitant loss of skeletal muscle mass. The aim of this study was to elucidate the changes in visceral fat and skeletal muscle mass in response to diabetes treatment including weight control.
Methods
For 6 months we observed the changes in the body compositions of 72 Japanese patients with type 2 diabetes who underwent multifaceted treatment including educational hospitalization. Visceral fat area (VFA) and appendicular skeletal muscle mass (ASM) were measured using a bioelectrical impedance method and dual-energy X-ray absorptiometry, respectively.
Results
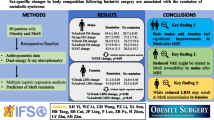
During the follow-up period, VFA reduced significantly whereas the average ASM did not change. Changes in ASM were strongly positively associated with changes in body weight (r = 0.50). Additionally, in an analysis of covariance, an above-median BMI (27 kg/m2) and above-median VFA (110 cm2) at baseline were found to be independent predictors of ASM reduction prevention. Of the 55 patients who lost weight, those who had a baseline VFA of ≥110 cm2 had significantly greater reductions in VFA than those with a baseline VFA of <110 cm2 (p < 0.01). ASM reduced significantly in patients with a VFA of <110 cm2 (p < 0.01), but not in those with a VFA of ≥110 cm2 (p = 0.98).
Conclusions
Baseline accumulation of visceral fat may predict a preferential reduction of visceral fat rather than skeletal muscle during weight control programs in type 2 diabetes patients.



Similar content being viewed by others
Abbreviations
- VFA:
-
Visceral fat area
- ASM:
-
Appendicular skeletal muscle mass
- ADA:
-
American Diabetes Association
- BMI:
-
Body mass index
- DXA:
-
Dual-energy X-ray absorptiometry
- JDS:
-
Japan Diabetes Society
- HbA1c:
-
Hemoglobin A1c
- UCP:
-
Urinary C-peptide
- eGFR:
-
Estimated glomerular filtration rate
- SMI:
-
Skeletal muscle index
- SFA:
-
Subcutaneous fat area
References
UK Prospective Diabetes Study 7. Response of fasting plasma glucose to diet therapy in newly presenting type II diabetic patients, UKPDS Group. Metabolism. 1990;39:905–12.
Goldstein DJ. Beneficial health effects of modest weight loss. Int J Obes Relat Metab Disord. 1992;16:397–415.
Pastors JG, Warshaw H, Daly A, Franz M, Kulkarni K. The evidence for the effectiveness of medical nutrition therapy in diabetes management. Diabetes Care. 2002;25:608–13.
American Diabetes Association. 6. Obesity management for the treatment of type 2 diabetes. Diabetes Care. 2016;39(Suppl 1):S47–51.
Pownall HJ, Bray GA, Wagenknecht LE, Walkup MP, Heshka S, Hubbard VS, Hill J, Kahn SE, Nathan DM, Schwartz AV, Johnson KC. Changes in body composition over 8 years in a randomized trial of a lifestyle intervention: the Look AHEAD study. Obesity (Silver Spring). 2015;23:565–72.
Jendle J, Nauck MA, Matthews DR, Frid A, Hermansen K, During M, Zdravkovic M, Strauss BJ, Garber AJ. Weight loss with liraglutide, a once-daily human glucagon-like peptide-1 analogue for type 2 diabetes treatment as monotherapy or added to metformin, is primarily as a result of a reduction in fat tissue. Diabetes Obes Metab. 2009;11:1163–72.
Cefalu WT, Leiter LA, Yoon KH, Arias P, Niskanen L, Xie J, Balis DA, Canovatchel W, Meininger G. Efficacy and safety of canagliflozin versus glimepiride in patients with type 2 diabetes inadequately controlled with metformin (CANTATA-SU): 52 week results from a randomised, double-blind, phase 3 non-inferiority trial. Lancet. 2013;382:941–50.
Bolinder J, Ljunggren O, Kullberg J, Johansson L, Wilding J, Langkilde AM, Sugg J, Parikh S. Effects of dapagliflozin on body weight, total fat mass, and regional adipose tissue distribution in patients with type 2 diabetes mellitus with inadequate glycemic control on metformin. J Clin Endocrinol Metab. 2012;97:1020–31.
Garciacaballero M, Reyes-Ortiz A, Garcia M, Martinez-Moreno JM, Toval JA, Garcia A, Minguez A, Osorio D, Mata JM, Miralles F. Changes of body composition in patients with BMI 23–50 after tailored one anastomosis gastric bypass (BAGUA): influence of diabetes and metabolic syndrome. Obes Surg. 2014;24:2040–7.
Park SW, Goodpaster BH, Lee JS, Kuller LH, Boudreau R, de Rekeneire N, Harris TB, Kritchevsky S, Tylavsky FA, Nevitt M, Cho YW, Newman AB. Excessive loss of skeletal muscle mass in older adults with type 2 diabetes. Diabetes Care. 2009;32:1993–7.
Wannamethee SG, Shaper AG, Lennon L, Whincup PH. Decreased muscle mass and increased central adiposity are independently related to mortality in older men. Am J Clin Nutr. 2007;86:1339–46.
Lee CG, Boyko EJ, Barrett-Connor E, Miljkovic I, Hoffman AR, Everson-Rose SA, Lewis CE, Cawthon PM, Strotmeyer ES, Orwoll ES. Insulin sensitizers may attenuate lean mass loss in older men with diabetes. Diabetes Care. 2011;34:2381–6.
Yamada M, Moriguch Y, Mitani T, Aoyama T, Arai H. Age-dependent changes in skeletal muscle mass and visceral fat area in Japanese adults from 40 to 79 years-of-age. Geriatr Gerontol Int. 2014;14(Suppl 1):8–14.
Seino Y, Nanjo K, Tajima N, Kadowaki T, Kashiwagi A, Araki E, Ito C, Inagaki N, Iwamoto Y, Kasuga M, Hanafusa T, Haneda M, Ueki K. Report of the Committee on the Classification and Diagnostic Criteria of Diabetes Mellitus. J Diabetes Investig. 2010;1:212–28.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K, Yamagata K, Tomino Y, Yokoyama H, Hishida A. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53:982–92.
Hind K, Oldroyd B, Truscott JG. In vivo precision of the GE Lunar iDXA densitometer for the measurement of total body composition and fat distribution in adults. Eur J Clin Nutr. 2011;65:140–2.
Heymsfield SB, Smith R, Aulet M, Bensen B, Lichtman S, Wang J, Pierson RN Jr. Appendicular skeletal muscle mass: measurement by dual-photon absorptiometry. Am J Clin Nutr. 1990;52:214–8.
Chen LK, Liu LK, Woo J, Assantachai P, Auyeung TW, Bahyah KS, Chou MY, Chen LY, Hsu PS, Krairit O, Lee JS, Lee WJ, Lee Y, Liang CK, Limpawattana P, Lin CS, Peng LN, Satake S, Suzuki T, Won CW, Wu CH, Wu SN, Zhang T, Zeng P, Akishita M, Arai H. Sarcopenia in Asia: consensus report of the Asian Working Group for Sarcopenia. J Am Med Dir Assoc. 2014;15:95–101.
Ryo M, Maeda K, Onda T, Katashima M, Okumiya A, Nishida M, Yamaguchi T, Funahashi T, Matsuzawa Y, Nakamura T, Shimomura I. A new simple method for the measurement of visceral fat accumulation by bioelectrical impedance. Diabetes Care. 2005;28:451–3.
Yamakage H, Ito R, Tochiya M, Muranaka K, Tanaka M, Matsuo Y, Odori S, Kono S, Shimatsu A, Satoh-Asahara N. The utility of dual bioelectrical impedance analysis in detecting intra-abdominal fat area in obese patients during weight reduction therapy in comparison with waist circumference and abdominal CT. Endocr J. 2014;61:807–19.
Li Y, Bujo H, Takahashi K, Shibasaki M, Zhu Y, Yoshida Y, Otsuka Y, Hashimoto N, Saito Y. Visceral fat: higher responsiveness of fat mass and gene expression to calorie restriction than subcutaneous fat. Exp Biol Med (Maywood). 2003;228:1118–23.
Kim TN, Park MS, Ryu JY, Choi HY, Hong HC, Yoo HJ, Kang HJ, Song W, Park SW, Baik SH, Newman AB, Choi KM. Impact of visceral fat on skeletal muscle mass and vice versa in a prospective cohort study: the Korean Sarcopenic Obesity Study (KSOS). PLoS One. 2014;9:e115407.
Koster A, Ding J, Stenholm S, Caserotti P, Houston DK, Nicklas BJ, You T, Lee JS, Visser M, Newman AB, Schwartz AV, Cauley JA, Tylavsky FA, Goodpaster BH, Kritchevsky SB, Harris TB. Does the amount of fat mass predict age-related loss of lean mass, muscle strength, and muscle quality in older adults? J Gerontol A Biol Sci Med Sci. 2011;66:888–95.
Yagi S, Kadota M, Aihara K, Nishikawa K, Hara T, Ise T, Ueda Y, Iwase T, Akaike M, Shimabukuro M, Katoh S, Sata M. Association of lower limb muscle mass and energy expenditure with visceral fat mass in healthy men. Diabetol Metab Syndr. 2014;6:27.
Schaap LA, Pluijm SM, Deeg DJ, Harris TB, Kritchevsky SB, Newman AB, Colbert LH, Pahor M, Rubin SM, Tylavsky FA, Visser M. Higher inflammatory marker levels in older persons: associations with 5-year change in muscle mass and muscle strength. J Gerontol A Biol Sci Med Sci. 2009;64:1183–9.
Roubenoff R. Sarcopenic obesity: the confluence of two epidemics. Obes Res. 2004;12:887–8.
Abdelhafiz AH, Koay L, Sinclair AJ. The effect of frailty should be considered in the management plan of older people with type 2 diabetes. Future Sci OA. 2016;2:FSO102.
Castaneda C, Layne JE, Munoz-Orians L, Gordon PL, Walsmith J, Foldvari M, Roubenoff R, Tucker KL, Nelson ME. A randomized controlled trial of resistance exercise training to improve glycemic control in older adults with type 2 diabetes. Diabetes Care. 2002;25:2335–41.
Ito S, Harada A, Kasai T, Sakai Y, Takemura M, Matsui Y, Hida T, Ishiguro N. Use of alfacalcidol in osteoporotic patients with low muscle mass might increase muscle mass: an investigation using a patient database. Geriatr Gerontol Int. 2014;14(Suppl 1):122–8.
Kim HK, Suzuki T, Saito K, Yoshida H, Kobayashi H, Kato H, Katayama M. Effects of exercise and amino acid supplementation on body composition and physical function in community-dwelling elderly Japanese sarcopenic women: a randomized controlled trial. J Am Geriatr Soc. 2012;60:16–23.
Acknowledgements
This work was supported in part by Grants-in-Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology of Japan [Grant Number 25860403].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have any conflicts of interest associated with this research.
Ethical standards
This study was carried out in accordance with the Declaration of Helsinki of 1964 and later versions and approved by the ethics committee of Tokyo Medical and Dental University (approval no. M2000-1573, approval date: 23 July 2013).
Informed consent
The patients gave their written informed consent to participate in this study and for its results to be published.
About this article
Cite this article
Ohara, N., Minami, I., Bouchi, R. et al. Loss of skeletal muscle mass and its predictors in type 2 diabetes patients under a multifaceted treatment approach. Diabetol Int 8, 366–374 (2017). https://doi.org/10.1007/s13340-017-0325-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13340-017-0325-z