Abstract
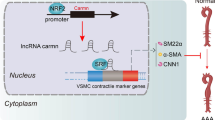
Cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy (CADASIL) is an inherited form of cerebral small vessel disease caused by mutations in conserved residues of NOTCH3. Affected arteries of CADASIL feature fibrosis and accumulation of NOTCH3. A variety of collagen subtypes (types I, III, IV, and VI) have been identified in fibrotic CADASIL vessels. Biglycan (BGN) and decorin (DCN) are class I members of the small leucine-rich proteoglycan (SLRP) family that regulate collagen fibril size. Because DCN has been shown to deposit in arteries in cerebral small vessel disease, we tested whether BGN accumulates in arteries of CADASIL brains. BGN was strongly expressed in both small penetrating and leptomeningeal arteries of CADASIL brain. BGN protein was localized to all three layers of arteries (intima, media, and adventitia). Substantially, more immunoreactivity was observed in CADASIL brains compared to controls. Immunoblotting of brain lysates showed a fourfold increase in CADASIL brains (compared to controls). Messenger RNA encoding BGN was also increased in CADASIL and was localized by in situ hybridization to all three vascular layers in CADASIL. Human cerebrovascular smooth muscle cells exposed to purified NOTCH3 ectodomain upregulated BGN, DCN, and COL4A1 through mechanisms that are sensitive to rapamycin, a potent mTOR inhibitor. In addition, BGN protein interacted directly with NOTCH3 protein in cell culture and in direct protein interaction assays. In conclusion, BGN is a CADASIL-enriched protein that potentially accumulates in vessels by mTOR-mediated transcriptional activation and/or post-translational accumulation via protein interactions with NOTCH3 and collagen.




Similar content being viewed by others
References
Pantoni L. Cerebral small vessel disease: from pathogenesis and clinical characteristics to therapeutic challenges. Lancet Neurol. 2010;9(7):689–701. doi:10.1016/S1474-4422(10)70104-6.
Joutel A, Corpechot C, Ducros A, Vahedi K, Chabriat H, Mouton P, et al. Notch3 mutations in CADASIL, a hereditary adult-onset condition causing stroke and dementia. Nature. 1996;383(6602):707–10. doi:10.1038/383707a0.
Dong H, Ding H, Young K, Blaivas M, Christensen PJ, Wang MM. Advanced intimal hyperplasia without luminal narrowing of leptomeningeal arteries in CADASIL. Stroke. 2013;44(5):1456–8. doi:10.1161/STROKEAHA.111.000721.
Miao Q, Paloneva T, Tuominen S, Poyhonen M, Tuisku S, Viitanen M, et al. Fibrosis and stenosis of the long penetrating cerebral arteries: the cause of the white matter pathology in cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy. Brain Pathol. 2004;14(4):358–64.
Joutel A, Andreux F, Gaulis S, Domenga V, Cecillon M, Battail N, et al. The ectodomain of the Notch3 receptor accumulates within the cerebrovasculature of CADASIL patients. J Clin Invest. 2000;105(5):597–605. doi:10.1172/JCI8047.
Dong H, Blaivas M, Wang MM. Bidirectional encroachment of collagen into the tunica media in cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy. Brain Res. 2012;1456:64–71. doi:10.1016/j.brainres.2012.03.037.
Baudrimont M, Dubas F, Joutel A, Tournier-Lasserve E, Bousser MG. Autosomal dominant leukoencephalopathy and subcortical ischemic stroke. A clinicopathological study. Stroke. 1993;24(1):122–5.
Estes ML, Chimowitz MI, Awad IA, McMahon JT, Furlan AJ, Ratliff NB. Sclerosing vasculopathy of the central nervous system in nonelderly demented patients. Arch Neurol. 1991;48(6):631–6.
Yamamoto Y, Craggs LJ, Watanabe A, Booth T, Attems J, Low RW, et al. Brain microvascular accumulation and distribution of the NOTCH3 ectodomain and granular osmiophilic material in CADASIL. J Neuropathol Exp Neurol. 2013;72(5):416–31. doi:10.1097/NEN.0b013e31829020b5.
Brulin-Fardoux P, Godfrain C, Maurage CA, De Reuck J, Hauw JJ, Kaltner H, et al. Glycohistochemical characterization of vascular muscle cell destruction in CADASIL subjects by lectins, neoglycoconjugates and galectin-specific antibodies. Neuropathol Appl Neurobiol. 2003;29(4):400–10.
Nastase MV, Young MF, Schaefer L. Biglycan: a multivalent proteoglycan providing structure and signals. J Histochem Cytochem: Off J Histochem Soc. 2012;60(12):963–75. doi:10.1369/0022155412456380.
Schonherr E, Witsch-Prehm P, Harrach B, Robenek H, Rauterberg J, Kresse H. Interaction of biglycan with type I collagen. J Biol Chem. 1995;270(6):2776–83.
Wiberg C, Heinegard D, Wenglen C, Timpl R, Morgelin M. Biglycan organizes collagen VI into hexagonal-like networks resembling tissue structures. J Biol Chem. 2002;277(51):49120–6. doi:10.1074/jbc.M206891200.
Wiberg C, Klatt AR, Wagener R, Paulsson M, Bateman JF, Heinegard D, et al. Complexes of matrilin-1 and biglycan or decorin connect collagen VI microfibrils to both collagen II and aggrecan. J Biol Chem. 2003;278(39):37698–704. doi:10.1074/jbc.M304638200.
Xu T, Bianco P, Fisher LW, Longenecker G, Smith E, Goldstein S, et al. Targeted disruption of the biglycan gene leads to an osteoporosis-like phenotype in mice. Nat Genet. 1998;20(1):78–82. doi:10.1038/1746.
Ameye L, Aria D, Jepsen K, Oldberg A, Xu T, Young MF. Abnormal collagen fibrils in tendons of biglycan/fibromodulin-deficient mice lead to gait impairment, ectopic ossification, and osteoarthritis. FASEB J: Off Publ Fed Am Soc Exp Biol. 2002;16(7):673–80. doi:10.1096/fj.01-0848com.
Bi Y, Ehirchiou D, Kilts TM, Inkson CA, Embree MC, Sonoyama W, et al. Identification of tendon stem/progenitor cells and the role of the extracellular matrix in their niche. Nat Med. 2007;13(10):1219–27. doi:10.1038/nm1630.
Casar JC, McKechnie BA, Fallon JR, Young MF, Brandan E. Transient up-regulation of biglycan during skeletal muscle regeneration: delayed fiber growth along with decorin increase in biglycan-deficient mice. Dev Biol. 2004;268(2):358–71. doi:10.1016/j.ydbio.2003.12.025.
Young MF, Fallon JR. Biglycan: a promising new therapeutic for neuromuscular and musculoskeletal diseases. Current Opin genetics Dev. 2012;22(4):398–400. doi:10.1016/j.gde.2012.07.008.
Goldberg M, Septier D, Rapoport O, Iozzo RV, Young MF, Ameye LG. Targeted disruption of two small leucine-rich proteoglycans, biglycan and decorin, excerpts divergent effects on enamel and dentin formation. Calcif Tissue Int. 2005;77(5):297–310. doi:10.1007/s00223-005-0026-7.
Berendsen AD, Fisher LW, Kilts TM, Owens RT, Robey PG, Gutkind JS, et al. Modulation of canonical Wnt signaling by the extracellular matrix component biglycan. Proc Natl Acad Sci U S A. 2011;108(41):17022–7. doi:10.1073/pnas.1110629108.
Bi Y, Stuelten CH, Kilts T, Wadhwa S, Iozzo RV, Robey PG, et al. Extracellular matrix proteoglycans control the fate of bone marrow stromal cells. J Biol Chem. 2005;280(34):30481–9. doi:10.1074/jbc.M500573200.
Chen XD, Fisher LW, Robey PG, Young MF. The small leucine-rich proteoglycan biglycan modulates BMP-4-induced osteoblast differentiation. FASEB J: Off Publ Fed Am Soc Exp Biol. 2004;18(9):948–58. doi:10.1096/fj.03-0899com.
Schaefer L, Babelova A, Kiss E, Hausser HJ, Baliova M, Krzyzankova M, et al. The matrix component biglycan is proinflammatory and signals through Toll-like receptors 4 and 2 in macrophages. J Clin Invest. 2005;115(8):2223–33. doi:10.1172/JCI23755.
Westermann D, Mersmann J, Melchior A, Freudenberger T, Petrik C, Schaefer L, et al. Biglycan is required for adaptive remodeling after myocardial infarction. Circulation. 2008;117(10):1269–76. doi:10.1161/CIRCULATIONAHA.107.714147.
Nielsen KL, Allen MR, Bloomfield SA, Andersen TL, Chen XD, Poulsen HS, et al. Biglycan deficiency interferes with ovariectomy-induced bone loss. J Bone Min Res: Off J Am Soc Bone Min Res. 2003;18(12):2152–8. doi:10.1359/jbmr.2003.18.12.2152.
Berendsen AD, Pinnow EL, Maeda A, Brown AC, McCartney-Francis N, Kram V, et al. Biglycan modulates angiogenesis and bone formation during fracture healing. Matrix biol: J Int Soc Matrix Biol. 2014;35:223–31. doi:10.1016/j.matbio.2013.12.004.
Lee SJ, Zhang X, Wang MM. Vascular accumulation of the small leucine-rich proteoglycan decorin in CADASIL. Neuroreport. 2014;25(13):1059–63. doi:10.1097/WNR.0000000000000230.
Zhang X, Meng H, Blaivas M, Rushing EJ, Moore BE, Schwartz J, et al. Von Willebrand Factor permeates small vessels in CADASIL and inhibits smooth muscle gene expression. Transl Stroke Res. 2012;3(1):138–45. doi:10.1007/s12975-011-0112-2.
Meng H, Zhang X, Hankenson KD, Wang MM. Thrombospondin 2 potentiates notch3/jagged1 signaling. J Biol Chem. 2009;284(12):7866–74.
Meng H, Zhang X, Yu G, Lee SJ, Chen YE, Prudovsky I, et al. Biochemical characterization and cellular effects of CADASIL mutants of NOTCH3. PLoS One. 2012;7(9):e44964. doi:10.1371/journal.pone.0044964.
Meng H, Zhang X, Lee SJ, Strickland DK, Lawrence DA, Wang MM. Low density lipoprotein receptor-related protein-1 (LRP1) regulates thrombospondin-2 (TSP2) enhancement of Notch3 signaling. J Biol Chem. 2010;285(30):23047–55. doi:10.1074/jbc.M110.144634.
Chung IM, Gold HK, Schwartz SM, Ikari Y, Reidy MA, Wight TN. Enhanced extracellular matrix accumulation in restenosis of coronary arteries after stent deployment. J Am Coll Cardiol. 2002;40(12):2072–81.
Yamakawa T, Bai HZ, Masuda J, Sawa Y, Shirakura R, Ogata J, et al. Differential expression of proteoglycans biglycan and decorin during neointima formation after stent implantation in normal and atherosclerotic rabbit aortas. Atherosclerosis. 2000;152(2):287–97.
Monet-Lepretre M, Haddad I, Baron-Menguy C, Fouillot-Panchal M, Riani M, Domenga-Denier V, et al. Abnormal recruitment of extracellular matrix proteins by excess Notch3 ECD: a new pathomechanism in CADASIL. Brain. 2013;136(Pt 6):1830–45. doi:10.1093/brain/awt092 awt092.
O’Brien KD, Olin KL, Alpers CE, Chiu W, Ferguson M, Hudkins K, et al. Comparison of apolipoprotein and proteoglycan deposits in human coronary atherosclerotic plaques: colocalization of biglycan with apolipoproteins. Circulation. 1998;98(6):519–27.
Riessen R, Isner JM, Blessing E, Loushin C, Nikol S, Wight TN. Regional differences in the distribution of the proteoglycans biglycan and decorin in the extracellular matrix of atherosclerotic and restenotic human coronary arteries. Am J Pathol. 1994;144(5):962–74.
Arboleda-Velasquez JF, Manent J, Lee JH, Tikka S, Ospina C, Vanderburg CR, et al. Hypomorphic notch 3 alleles link notch signaling to ischemic cerebral small-vessel disease. Proc Natl Acad Sci U S A. 2011;108(21):E128–35. doi:10.1073/pnas.1101964108.
Gregory CR, Huie P, Billingham ME, Morris RE. Rapamycin inhibits arterial intimal thickening caused by both alloimmune and mechanical injury. Its effect on cellular, growth factor, and cytokine response in injured vessels. Transplantation. 1993;55(6):1409–18.
Sousa JE, Costa MA, Abizaid A, Abizaid AS, Feres F, Pinto IM, et al. Lack of neointimal proliferation after implantation of sirolimus-coated stents in human coronary arteries: a quantitative coronary angiography and three-dimensional intravascular ultrasound study. Circulation. 2001;103(2):192–5.
Meng H, Zhang X, Lee SJ, Wang MM. Von Willebrand factor inhibits mature smooth muscle gene expression through impairment of Notch signaling. PLoS One. 2013;8(9):e75808. doi:10.1371/journal.pone.0075808.
Zhang X, Meng H, Wang MM. Collagen represses canonical notch signaling and binds to notch ectodomain. Int J Biochem Cell Biol. 2013;45(7):1274–80. doi:10.1016/j.biocel.2013.03.020.
Corsi A, Xu T, Chen XD, Boyde A, Liang J, Mankani M, et al. Phenotypic effects of biglycan deficiency are linked to collagen fibril abnormalities, are synergized by decorin deficiency, and mimic Ehlers-Danlos-like changes in bone and other connective tissues. J Bone Min Res: Official J Am Soc Bone Min Res. 2002;17(7):1180–9. doi:10.1359/jbmr.2002.17.7.1180.
Heegaard AM, Corsi A, Danielsen CC, Nielsen KL, Jorgensen HL, Riminucci M, et al. Biglycan deficiency causes spontaneous aortic dissection and rupture in mice. Circulation. 2007;115(21):2731–8. doi:10.1161/CIRCULATIONAHA.106.653980.
Hildebrand A, Romaris M, Rasmussen LM, Heinegard D, Twardzik DR, Border WA, et al. Interaction of the small interstitial proteoglycans biglycan, decorin and fibromodulin with transforming growth factor beta. Biochem J. 1994;302(Pt 2):527–34.
Kolb M, Margetts PJ, Sime PJ, Gauldie J. Proteoglycans decorin and biglycan differentially modulate TGF-beta-mediated fibrotic responses in the lung. Am J Physiol Lung Cell Mol Physiol. 2001;280(6):L1327–34.
Hara K, Shiga A, Fukutake T, Nozaki H, Miyashita A, Yokoseki A, et al. Association of HTRA1 mutations and familial ischemic cerebral small-vessel disease. N Engl J Med. 2009;360(17):1729–39. doi:10.1056/NEJMoa0801560.
Acknowledgments
NIH (NS052681, NS054724, and NS062816) and the Department of Veterans Affairs (5I01BX000375) provided funding for these studies. This research was supported, in part, by the DIR, NIDCR of the IRP, NIH, DHHS.
Conflict of Interest
The authors declare that they have no conflict of interest.
Compliance with Ethics Requirements
This article does not contain any studies with living human or animal subjects.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, X., Lee, S.J., Young, M.F. et al. The Small Leucine-Rich Proteoglycan BGN Accumulates in CADASIL and Binds to NOTCH3. Transl. Stroke Res. 6, 148–155 (2015). https://doi.org/10.1007/s12975-014-0379-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-014-0379-1