Abstract
Insulin and incretin-based drugs are important antidiabetic agents with complex effects on cell growth and metabolism. Emerging evidence shows that insulin and incretin-based drugs are associated with altered risk of biliary tract cancer (BTC). Observational study reveals that insulin is associated with an increased risk of extrahepatic cholangiocarcinoma (ECC), but not intrahepatic cholangiocarcinoma (ICC) or gallbladder cancer (GBC). This type-specific effect can be partly explained by the cell of origin and heterogeneous genome landscape of the three subtypes of BTC. Similar to insulin, incretin-based drugs also exhibit very interesting contradictions and inconsistencies in response to different cancer phenotypes, including BTC. Both epidemiological and experimental evidence suggests that incretin-based drugs can be a promoter of some cancers and an inhibitor of others. It is now more apparent that this type of drugs has a broader range of physiological effects on the body, including regulation of endoplasmic reticulum stress, autophagy, metabolic reprogramming, and gene expression. In particular, dipeptidyl peptidase-4 inhibitors (DPP-4i) have a more complex effect on cancer due to the multi-functional nature of DPP-4. DPP-4 exerts both catalytic and non-enzymatic functions to regulate metabolic homeostasis, immune reaction, cell migration, and proliferation. In this review, we collate the epidemiological and experimental evidence regarding the effect of these two classes of drugs on BTC to provide valuable information.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Biliary tract cancer (BTC) consists of intrahepatic cholangiocarcinoma (ICC), extrahepatic cholangiocarcinoma (ECC), and gallbladder cancer (GBC) [1, 2]. BTC is rare but lethal and prevalent in some areas all around the world, such as several countries in Asia, Eastern Europe, and Latin America [3, 4]. Several risk factors are already established for BTC which include parasitic infections, primary sclerosing cholangitis (PSC), choledochal cyst, hepatolithiasis, and toxins. Other potential risk factors include inflammatory bowel disease (IBD), hepatitis B virus (HBV), hepatitis C virus (HCV), cirrhosis, diabetes, obesity, and smoking [5,6,7]. Among them, close attention should be paid to diabetes mellitus (DM) because of its rapid growth worldwide today.
According to the latest report from the International Diabetes Federation, the global diabetes prevalence in 20 ~ 79-year-olds in 2021 was estimated to be 10.5% (536.6 million people), rising to 12.2% (783.2 million) in 2045 [8]. More importantly, as a chronic and progressive metabolic disease, DM needs to be treated with antidiabetic drugs to maintain stable blood glucose levels and avoid the serious consequences of long-term hyperglycemia. However, in addition to their hypoglycemic effects, antidiabetic drugs may have several side effects, including an increased risk of certain types of cancer.
Among hypoglycemic agents, insulin and incretin-based drugs are two important drugs that are widely used in clinical practice. Considering their complex regulatory role in cell growth and metabolism, the influence of insulin and incretin-based drugs on the cancer profile of diabetic patients has attracted widespread attention. In the past few years, many studies have shown that insulin and incretin-based drugs are associated with an increased risk of multiple cancer types, such as pancreatic cancer, breast cancer, and thyroid cancer [9,10,11,12,13,14]. Recently, some important findings related to insulin/incretin-based drugs and BTC have been reported, which provide new evidence for further study. A study from China showed that insulin was associated with an increased risk of ECC but not ICC or GBC [15], indicating a type-specific relationship between insulin and BTC. A comprehensive meta-analysis of randomized clinical trials showed that incretin-based drugs were not associated with an increased risk of BTC [16]. This result is inconsistent with previous findings which have shown that incretin-based drugs played a facilitative role in the development of BTC [17].
The limited and inconsistent results pose a challenge to the clarification of the effect of insulin and incretin-based drugs on BTC. To facilitate research progress in this area, here we update the epidemiological and experimental evidence on the association of insulin and incretin-based drugs with BTC risk and explore the involving molecular mechanisms.
2 Insulin and BTC: limited evidence from only one cohort study
2.1 The mitogenic effect of insulin and its molecular mechanisms
Since first identified by Canadian scientists Frederick G. Banting and Charles H in 1921, insulin has marked one of the most important breakthroughs in the history of diabetic treatment. Insulin is secreted by the beta cells of the islets of Langerhans in the pancreas to regulate the level of glucose in the blood. Upon binding to the insulin receptor (IR), insulin activates its tyrosine kinase and initiates downstream signaling including the phosphatidylinositol 3-kinase/protein kinase B (PI3K/Akt) [18,19,20], mammalian target of rapamycin (mTOR) [21,22,23], and Ras/mitogen-activated protein kinase (MAPK) pathways [20, 24, 25]. Noteworthy, besides the metabolic effect, insulin plays an important role in the regulation of cell growth and exerts a mitogenic effect on tumor development. Firstly, through the insulin receptor substrates (IRSs), an adaptor protein of the IR, the insulin signaling pathway recruits multiple signaling complexes to connect with other signaling pathways [26,27,28,29]. For instance, the recruiting of growth factor receptor-bound protein 2 (Grb2) to the binding motif on IRS forms a complex with guanine nucleotide exchange factor Son of Sevenless and phosphorylates Ras [30, 31], thus activating the MAPK signaling cascade [32, 33]. In addition, the upregulation of Rac1, another important signaling pathway downstream of the IR [34], promoted cell proliferation and migration as well as angiogenesis in multiple cancer types [34,35,36,37,38]. Moreover, insulin also promotes tumor cell growth by altering the energy metabolism of tumor cells through the aberrant mTOR pathway to upregulate glucose uptake [39] and glycogenolysis [22]. Finally, the signaling crosstalk between insulin and insulin-like growth factor-1 receptor (IGF-1R) is closely related to tumor development. Since insulin with 40–80% homology to the insulin-like growth factor-1 (IGF-1) [40] and IGF-1R with a 70% homology to the IR [41], in the condition of hyperinsulinemia, insulin can overcome the restriction of lower affinity to the IGF-1R and activate the downstream signaling of the IRS/PI3K/Akt and Ras/Raf/extracellular-signal-regulated kinase (ERK) pathways, thus augments its mitogenic and antiapoptotic effects [42,43,44]. In addition, hyperinsulinemia also exerts its proliferative effects indirectly by reducing the liver production of IGF-1-binding proteins [45] to increase the biologically active free IGF-1. Noticeably, increased insulin levels can also bind to the hybrid receptors IR/IGF-1Rs (HRs) [46] and activate the insulin/IGF signaling system (Fig. 1 shows the insulin signaling and crosstalk with the IGF-1 systems).
Insulin signaling and crosstalk with the IGF-1 systems. Insulin regulates the Ras/Raf/MAPK and PI3K/AKT/mTOR pathways to influence the development of BTC. In the condition of hyperinsulinemia, insulin can directly bind to IGF-1R and IR/IGF-1Rs or indirectly increase the biologically active free IGF-1 to augment its mitogenic and antiapoptotic effects. IGF-I insulin-like growth factor-1, MAPK mitogen-activated protein kinase, PI3K phosphatidylinositol-3-kinase, Akt protein kinase B, mTOR mammalian target of rapamycin, BTC biliary tract cancer, IGF-1R insulin-like growth factor-1 receptor, IR/IGF-1Rs hybrid receptors of insulin receptor and insulin-like growth factor-1 receptor, IRS insulin receptor substrates, IRs(A/B) insulin receptor A or B isoform, IGFBPs insulin-like growth factor-binding proteins, ULK Unc-51 like autophagy activating kinase, MEK mitogen-activated protein kinase kinase, ERK extracellular signal-regulated kinase
2.2 Insulin and increased risk of BTC
Previous epidemiological studies indicated that insulin promotes higher rates of some cancer types presentation in patients with type 2 diabetes mellitus (T2DM), such as colorectal cancer [47, 48], lung cancer [49], breast cancer [50], pancreatic cancer [10, 51], liver cancer [52,53,54], bladder cancer [55] and neuroendocrine tumors [55]. In addition to the observational evidence, many experimental studies provided solid confirmation of the positive relationship between insulin and cancer. Saisana et al. reported that insulin has direct tumor-promoting effects on the gastric adenocarcinoma cells [56]. In the case of breast cancer, evidence revealed that insulin stimulates the proliferation of some human breast cancer cell lines in vitro by activating both the PI3K/Akt and the MAPK signaling pathways [57]. Although there have been many studies investigating the association between insulin and cancer, research on BTC is still very sparse. It is very challenging to conduct large-scale epidemiological investigations to clarify the relationship between insulin and BTC due to the relatively low incidence of BTC worldwide (0.3-6 per 100,000 inhabitants per year) [58, 59].
Back in 2013, Schlesinger and colleagues attempted to assess the risk of BTC in diabetic patients treated with insulin, but they were unable to conclude because only two cases of BTC were observed in 2,156 insulin users [60]. To fill this knowledge gap in this area, we conducted a study in 2021 using electronic medical record data, which showed that insulin therapy was associated with an increased hazard ratio (HR) of ECC (HR, 4.10; 95% CI, 1.54–10.92) but not ICC (HR, 1.36; 95% CI, 0.30–6.09) or GBC (HR, 1.28; 95% CI, 0.61–2.66) (Table 1) [15]. However, only this study has yielded some statistically significant results, and due to residual confounding factors, it is still unable to draw definitive conclusions about the relationship between insulin and BTC. More results from other studies are urgently needed to elucidate the effect of insulin on BTC in diabetic patients.
2.3 Possible reasons for insulin and BTC risk discrepancy
According to our previous findings, the association of insulin with BTC seems to be type-specific. Based on available evidence, the reasons for the type-specific nature lie in two aspects: different cells of origin (COO) and different molecular alterations.
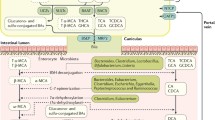
Firstly, BTC consists of a heterogenetic group of cancers that originate from different cell types throughout the biliary tree (Fig. 2). ICC originates from hepatic progenitor cells, hepatocytes, or cholangiocytes, GBC originates from cholangiocytes, and ECC originates from cholangiocyte precursor cells and cholangiocytes [61]. The difference between COO lays the biological foundation for the risk discrepancy between subtypes of BTC. In particular, the COO of ECC chiefly originates from peribiliary glands (PBGs), which contain stem/progenitor cells (BTSCs) for the regeneration of the biliary tree and can differentiate toward pancreatic islet beta-cell in T2DM 62, 63]. This phenomenon indicates that when exposed to hyperinsulinemia and hyperglycemia for a prolonged period, the continuous stimulation will contribute to the proliferation of PBGs cells. In turn, both in vivo and in vitro evidence suggests that hyperinsulinemia can stimulate preneoplastic and tumor cells with genetic mutations to become clinically manifest tumors and more aggressive malignancies [64,65,66]. Therefore, the reason why insulin can significantly increase the risk of ECC may be that insulin is highly carcinogenic to the cells of PBGs.
Cell of origin and molecular alterations of three subtypes of BTC. The difference in the cell of origin and molecular alterations lays the foundation of the risk discrepancy between insulin and three subtypes of BTC. Compared to ICC and GBC, ECC originates mainly from cells residing in PBGs and has more frequent mutations in P53, KRAS, and SMAD4, resulting in greater sensitivity to insulin stimulation. BTC biliary tract cancer, ICC intrahepatic cholangiocarcinoma, ECC extrahepatic cholangiocarcinoma, GBC gallbladder cancer, PBGs peribiliary glands, FGFR 1–3 fibroblast growth factor receptor 1–3, IDH 1/2 isocitrate dehydrogenase, BAP1 BRCA1-associated-protein 1,ubiquitin carboxyl-terminal hydrolase, ARID1A AT-rich interactive domain-containing protein 1 A, EPHA2 ephrin type-A receptor 2, TP53 tumor protein P53, KRAS kirsten rat sarcoma viral oncogene homolog, SMAD4 mothers against decapentaplegic homolog 4, PRKACA protein kinase cyclic adenosine monophosphate (cAMP)-activated catalytic subunit alpha, PRKACB protein kinase cAMP-activated catalytic subunit beta, ELF3 E74 like ETS transcription factor 3, ARID1B/A AT-rich interactive domain-containing protein 1 B/A, GNAS guanine nucleotide-binding protein-alpha stimulating, BRCA1/2 breast cancer gene 1/2, PIK3CA phosphatidylinositol-4,5-bisphosphate 3-kinase catalytic subunit alpha, EGFR epidermal growth factor receptor, ERBB3 erythroblastic leukemia viral oncogene homologue3, PTEN phosphatase and tensin homolog, ARID2 AT-rich interactive domain 2, MLL2/3 histone-lysine N-methyltransferase, TERT telomerase reverse transcriptase. (Fig. 2 is created with BioRender.com)
Secondly, the molecular alterations of BTC subtypes differ based on different COO (Fig. 2). The frequent mutations in ICC are fibroblast growth factor receptor 1–3 (FGFR 1–3), isocitrate dehydrogenase (IDH 1/2), BRCA1-associated-protein 1 (BAP1, ubiquitin carboxyl-terminal hydrolase), AT-rich interactive domain-containing protein 1 A (ARID1A), and ephrin type-A receptor 2 (EPHA2), in ECC are tumor protein P53 (TP53), kirsten rat sarcoma viral oncogene homolog (KRAS), mothers against decapentaplegic homolog 4 (SMAD4), protein kinase cyclic adenosine monophosphate (cAMP)-activated catalytic subunit alpha (PRKACA), and protein kinase cAMP-activated catalytic subunit beta (PRKACB) fusion, E74 like ETS transcription factor 3 (ELF3), AT-rich interactive domain-containing protein 1 B/A (ARID1B/A), guanine nucleotide-binding protein-alpha stimulating (GNAS), breast cancer gene 1/2 (BRCA1/2), and phosphatidylinositol-4,5-bisphosphate 3-kinase catalytic subunit alpha (PIK3CA), and in GBC are epidermal growth factor receptor (EGFR), erythroblastic leukemia viral oncogene homologue 3 (ERBB3), phosphatase and tensin homolog (PTEN), AT-rich interactive domain 2 (ARID2), histone-lysine N-methyltransferase (MLL2/3), and telomerase reverse transcriptase (TERT) [67]Specifically, there are some mutations only occurring on a certain subtype of BTC. For example, IDH1/2 mutations and FGFR2 fusions frequently occur in ICC [68] and ERBB2 mutations frequently occur in GBC [69]. Subsequently, the various molecular alterations can lead to various deregulation of PI3K/Akt and MAPK pathways. Moreover, compared to ICC and GBC, ECC harbors more frequent mutations in the regulation of cell metabolism, growth, and proliferation, such as P53, KRAS, and SMAD4. These molecular mutations can form a complicated network with the insulin signaling pathway. For example, insulin can activate the effect of RAS [70] and interact with SMAD4 through some classical pathways, such as MAPK and PI3K/Akt [71, 72].
3 Incretin-based drugs and BTC: inconsistency and conflicts
3.1 The function of incretin-based drugs and cancer development
3.1.1 Incretin-based drugs and insulin regulation
Glucagon-like peptide-1 (GLP-1) is an incretin hormone secreted by enteroendocrine L cells in the distal intestine, alpha cells in the pancreas, and the central nervous system [73]. Since its discovery research began in 1979, GLP-1 has been recognized as an important stimulator of insulin secretion and a crucial regulator of energy homeostasis [74]. GLP-1 protects against hyperglycemia mainly by two mechanisms: enhancement of insulin secretion in beta-cells and inhibition of glucagon secretion in alpha-cells. In addition to immediately increasing the synthesis and release of insulin, its role in promoting insulin secretion by increasing proliferation and decreasing apoptosis of beta-cells at the late stage is particularly striking [75,76,77,78].
Firstly, as one of the most important substances in glucose-induced insulin secretion (GIIS), GLP-1 elicits its incretin effects via an acute elevation in cAMP levels, and subsequent activation of protein kinase A (PKA) and exchange protein directly activated by cAMP 2 (EPAC2) when binding to GLP-1 receptors on beta-cells (Fig. 3). Activation of PKA by cAMP results in phosphorylation of the sulphonylurea receptor (SUR1, a KATP channel subunit) [79] and subsequent membrane depolarization, then triggering the insulin secretory pathway. Activation of another cAMP effector, EPAC2, promotes membrane depolarization in lower concentrations of adenosine triphosphate (ATP) and subsequently stimulates insulin granule exocytosis and maturation by sensitizing the ryanodine receptors and activating the calcium-sensing complex [80,81,82].
Signaling pathways of GLP-1 and DPP-4. GLP-1 elicits its incretin effects via an acute elevation in cAMP levels and subsequent activation of PKA and EPAC when binding to GLP-1 receptors on beta-cells. GLP-1 slows the progressive loss of beta-cell function by the activation of pro-survival CREB signaling. This figure shows two of the common ways by which DPP-4 promotes cancer progression: truncating CCL11 to decrease the migration of eosinophils and CXCL10 to inhibit the migration of T and NK cells. GLP-1 glucagon-like peptide-1, DPP-4 dipeptidyl peptidase-4, cAMP cyclic adenosine monophosphate, PKA protein kinase A, PKC Protein kinase C, Akt/PKB Protein kinase B, EPAC exchange protein directly activated by cAMP, CREB cAMP-response element binding protein, NK natural killer cells, DPP-4i dipeptidyl peptidase-4 inhibitors, MAPK mitogen-activated protein kinase, PI3K phosphatidylinositol-3-kinase, mTOR mammalian target of rapamycin, JNK c-Jun N-terminal kinase, ERK1/2 extracellular signal-regulated kinase 1/2, ATP adenosine triphosphate, IRS insulin receptor substrates, PDX-1 pancreatic and duodenal homeobox 1, CCL C-C motif chemokine ligand, CXCL chemokine (C-X-C motif) ligand
Secondly, in addition to the acute stimulation of insulin secretion in response to a rise in blood glucose, GLP-1 slows the progressive loss of beta-cell function. By the activation of pro-survival cAMP-response element binding protein (CREB) signaling and non-receptor tyrosine kinase/c-Src and the transactivation of EGFR [83,84,85], GLP-1 induces increased expression of anti-apoptotic genes [84], attenuation of endoplasmic reticulum (ER) stress [86], prevention of oxidative stress and fatty acid-mediated toxicity [87], and subsequently exerts pro-survival and anti-apoptotic effects. Moreover, GLP-1 has been shown to alleviate glucotoxicity, lipotoxicity, excess nitric oxide (NO), and Ca2+ depletion in both primary beta-cells and cell lines to restore the insulin-secreting function of the pancreas [88,89,90,91,92].
Despite its important role in regulating insulin secretion, GLP-1 is very short-lived due to the degradation by a ubiquitous protease, dipeptidyl peptidase-4 (DPP-4), within one to two minutes under physiological conditions [93]. In order to prolong the half-life of GLP-1 and thus improve its clinical efficacy, several GLP-1 analogs (GLP-1 receptor agonists, GLP-1 RAs) have been developed. The half-life of these analogs, including exenatide, lixisenatide, liraglutide, dulaglutide, albiglutide, and semaglutide, can be extended to 2–13 h [94, 95], or up to 5 days [96]. Except the prolonged half-life, GLP-1 RAs share common mechanisms of action with the endogenous GLP-1: augmentation of hyperglycemia-induced insulin secretion, suppression of glucagon secretion at hyper- or euglycemia, and restoring the function of beta-cells [97,98,99,100]. Besides GLP-1 RAs, another widely used type of incretin-based drug is the DPP-4 inhibitor (DPP-4i). DPP4-i itself has no hypoglycemic activity. Instead, their hypoglycemic effect is mainly achieved by increasing endogenous GLP-1 concentrations [101], and their effects are more multifaceted, as described later.
3.1.2 GLP-1 RAs and cancer
At present, some preliminary and observational studies reported a link between GLP-1 RAs and cancers. Evidence showed that the GLP-1 receptors are not only expressed in normal tissues but also in malignant cells, such as endometrial cancer cells [102], breast cancer cells [94], colon cancer cells [103], and prostate cancer cells [104]. Considering its special effect on the pancreas, the relationship between GLP-1 RAs and pancreatic diseases attracted the attention of researchers. For instance, a case-control study reported that the use of GLP-1 RAs was associated with an increased risk of acute pancreatitis [105]. This raised the concern of increased risk of pancreatic cancer because recurrent acute pancreatitis turns into chronic pancreatitis and subsequently causes stenosis of the pancreatic duct and an increase in intra-ductal pressure, which leads to the development of pancreatic cancer over the years [106]. Actually, there is evidence that GLP-1 RAs are significantly associated with an increased risk of pancreatic cancer. The mechanism by which GLP-1 RAs exert their proliferative effect is still under exploration. Evidence showed that signaling pathways involved in the proliferative activity of GLP-1 are PI3-K/Akt, MAPK/ERK, and protein kinase C (PKC) pathways (Fig. 3) [107]. Another underlying mechanism is the incretin effect of GLP-1RAs. Since GLP-1RAs can elevate insulin levels both by increasing the immediate release of insulin and promoting the proliferation of beta-cells, concerns raise because of the tumorigenic effect of insulin as mentioned above.
3.1.3 DPP-4i and cancer
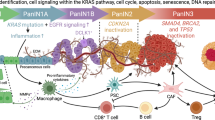
Before discussing the relationship between DPP-4i and cancer, it is necessary to introduce the pleiotropic effect of DPP-4 because the relationship between DPP-4i and cancer is the reverse of the relationship between DPP-4 and cancer. Besides its degradation effect on GLP-1, DPP-4 is also known as the T-cell antigen cluster of differentiation 26 (CD26) [108, 109]. It is a multi-functional protein widely expressed in different organs and on the surface of various cell types [110, 111]. DPP-4 is an integral membrane protein and consists of a large extracellular domain, anchored in the cell membrane by a flexible segment coupled to a trans-membrane sequence. It can exert catalytic functions with the C-terminal region of the extracellular part as well as non-enzymatic functions with the cysteine-rich region and glycosylation site-rich region [112].
When it exerts catalytic functions, DPP-4 cleaves incretin hormones related to metabolic homeostasis and a large number of cytokines, chemokines, and peptide hormones involved in the regulation of the immune system, such as GLP-1, glucose-dependent insulinotropic polypeptide (GIP), chemokine (C-X-C motif) ligand 10 (CXCL 10), CXCL 11, CXCL12, C-C motif chemokine ligand 2 (CCL2), CCL3, CCL5, CCL11, and CCL22 [113,114,115]. The catalytic effect of DPP-4 is reported to be associated with cancer progression. Evidence from hepatocellular carcinoma (HCC) showed that both gene ablation and pharmacological inhibition of DPP-4 notably prevent tumor progression by down-regulating the production of chemokine CCL2 [103]. In the investigation of HCC and breast cancer using syngeneic mouse models, Hollande and colleagues found that inhibition of DPP-4 increased the migration of eosinophils into solid tumors and reduced tumor growth. Further analysis showed that increased concentrations of the eosinophil chemoattractant CCL11, a known target for DPP4-mediated truncation, attributed to this antitumor effect (Fig. 3) [116]. Consistently, studies on melanoma and colorectal cancer also showed that DPP-4 limited the migration of T cells and natural killer (NK) cells by mediating the cleavage of chemokines CXCL10 to promote cancer progression (Fig. 3) [117, 118]. This effect can be attenuated by its inhibitor, sitagliptin, which can improve naturally occurring tumor immunity and enhance responses to T-cell-mediated immunotherapy.
Independent of its catalytic activity, DPP-4 can interact with other proteins as well as function as binding sites to affect physiological processes, such as the interaction between cells and the extracellular matrix, cell migration, and proliferation [112]. Evidence showed that DPP-4 overexpression led to increased epidermal growth factor-induced colony formation and expression of peptidylprolyl cis/trans-isomerase-1 (PIN1) and cyclin D1 in cancer cells via MEK/ERK and c-Jun N-terminal kinase (JNK) pathway, thus causing epithelial-mesenchymal transition (EMT) and tumorigenesis in breast cancer [119]. A study on endometrial carcinoma showed a positive association between DPP-4 expression and cancer cell proliferation, invasion, and tumorigenicity. Whereas, the proliferation of cancer cells was reduced when DPP-4 was knocked out or the enzyme activity was inhibited [120]. Moreover, within the immune system, DPP-4/CD26 can act as co-stimulatory molecules to amplify the immune signal, thereby leading to T-cell activation [121]. Consequently, the altered expression and/or activity of DPP-4 result in the disturbance of several pathological processes, including inflammation, viral entry, immune-mediated diseases, and tumor development [122,123,124]. When blocked by its inhibitor DPP-4i, the effect of DPP-4 on cancer will be attenuated or reversed.
3.2 Incretin-based drugs and BTC
Since its debut in 2005, the incretin-based drug has achieved great success in the management of T2DM and obesity. In the investigation of the side effects of incretin-based drugs, several observational studies showed that the use of incretin-based drugs was associated with an increased risk of some cancer types, such as pancreatic cancer [13], breast cancer [125], and thyroid cancer [12, 126]. However, as the study progressed, more and more contradictions are emerging. For example, Liu and colleagues found that liraglutide treatment accelerated human triple-negative breast cancer (TNBC) cells’ progress both in vitro and in vivo through the nicotinamide adenine dinucleotide phosphate oxidase 4/reactive oxygen species/ vascular endothelial growth factor (NOX4/ROS/VEGF) signaling pathway [125]. On the contrary, Alanteet et al. showed opposite results. In their study, liraglutide caused 48% inhibition of MCF-7 human breast cancer cell proliferation in obese adipose tissue-derived stem cells-conditioned medium, reduced the colony formation, and induced G0/G1 phase arrest [127]. Moreover, studies on other cancer types showed both pro- and anti-tumorigenic effects of incretin-based drugs. Using real-world data Wang et al. detected a differential risk association between GLP-1RAs treatment and cancers. They showed that GLP-1RAs were associated with lower risks of prostate, lung, and colon cancer, but a higher risk of thyroid cancer [128]. These results strongly indicated that complex mechanisms may involve in the interaction between incretin-based drugs and cancer.
As with other cancer types, research on incretin-based drugs and BTC began more than a decade ago. In 2007, Marzioni and colleagues found that the GLP-1receptor is expressed in cholangiocytes and will be up-regulated in the course of cholestasis. GLP-1 increases cholangiocyte growth both in vitro and in vivo through the PI3K/cAMP/PKA-Ca2+-CamKII pathway instead of the classical proliferative MAPK-ERK1/2-PKCα pathways. The proliferative effects can be blunted by GLP-1RAs [128]. Later in 2009, they found that exendin-4, a 39-amino acid GLP-1 analog, prevents cholangiocyte apoptosis both in vitro and in vivo by counteracting the activation of the mitochondrial pathway of apoptosis [129]. In 2014, Chen et al. showed that the GLP-1 receptor protein expression was upregulated in tumor tissue samples of patients with ICC and associated with lymph node metastasis [130]. These studies initially raised concerns regarding a potential association between incretin-based drugs and increased risk of BTC.
In 2016, the Liraglutide Effect and Action in Diabetes: Evaluation of Cardiovascular Outcome Results (LEADER) trial firstly reported the association of liraglutide with BTC, yielding an increased hazard of 1.62 (95%CI, 0.67–3.90) [131]. This study failed to clarify the relationship between saxagliptin and BTC because of the wide confidence interval. In 2018, an observational study conducted by Abrahami et al. attracted widespread and intense interest. Using data from the UK Clinical Practice Research Datalink (CPRD), the authors found that the use of DDP-4i was associated with a 77% increased hazard of CCA (DDP-4i HR, 1.77; 95% CI, 1.04–3.01) and the use of GLP-1 RAs was associated with an increased hazard with a wide confidence interval (GLP-1 RAs HR, 1.97; 95%CI, 0.83–4.66) [17]. However, although 154,162 patients were included in this cohort, only 105 incident BTC events occurred, of which 27 events occurred in the DPP-4i group and 7 occurred in the GLP-1 RAs group. The small number of cases prevented this study from more convincible conclusions.
However, the results of different studies are inconsistent. In 2015, the Saxagliptin Assessment of Vascular Outcomes Recorded in Patients with Diabetes Mellitus (SAVOR)–Thrombolysis in Myocardial Infarction (TIMI) 53 trial firstly reported that the use of saxagliptin was associated with a lower hazard of hepatic and biliary neoplasm (0.75; 95% CI, 0.30–1.76) [132]. In 2020, a nested case-control study (744 cases vs. 2976 controls) showed that no increased odds ratio (OR) of CCA associated with the use of either DPP-4i (OR, 0.98; 95% CI, 0.75–1.29) or GLP-1 RAs (OR, 1.09; 95% CI, 0.63–1.89) [133]. Similarly, a nationwide study using data from three Scandinavian countries in 2021 showed that neither the use of DPP-4i nor GLP-1 RAs was associated with a significantly increased risk of CCA (DPP-4i HR, 1.15; 95% CI, 0.90–1.46; GLP-1 RAs HR, 1.25; 95% CI, 0.89–1.76) [134]. Different from a study using data from the CPRD, this study had a larger sample size (n = 585,876) and more BTC cases (n = 599), of which the DPP4i group included 346,485 patients with 350 BTC events occurred and the GLP-1 RAs group included 239,391 patients with 249 BTC events occurred. More importantly, although 25% of the patients with a long-term follow-up of more than 6 years (7.0 years in the DPP4i group and 6.9 years in the GLP-1 RAs group), no elevated risk was found. This indicated that lifelong use of incretin-based drugs might be safe for BTC in patients with T2DM. To resolve the controversy between different studies, He et al. published a comprehensive meta-analysis of randomized clinical trials in 2022. A total of 76 randomized control trials (RCTs) involving 103,371 patients were included. Although the results showed that GLP-1 RAs treatment was associated with increased risks of other gallbladder or biliary diseases, there was no increased relative risk (RR) of BTC (RR, 1.43; 95% CI, 0.80–2.56). Of note, only 25 cases of BTC were observed in GLP-1 RAs groups (25/31,010) and 15 in control groups (15/30,026) [16] (Results of epidemiological studies are summarized in Table 1).
3.3 Concerns from supportive evidence: incretin-based drugs and biliary diseases
Despite the conflicting results, there is evidence to support the possible association of incretin-based drugs with an increased risk of BTC. As a complex disease, BTC is affected by many risk factors, including biliary tract diseases. Incretin-based drugs have been reported to disrupt biliary homeostasis, which has implications for the development of BTC.
Firstly, incretin-based drugs were associated with an increased risk of gallstone formation. Kellera et al. showed that GLP-1 RA exenatide significantly reduced CCK-induced gallbladder emptying compared to placebo in fasting healthy subjects [135]. The inhibition of gallbladder contractility leads to gallstone formation, which is an established risk factor for GBC. In a weight management trial of liraglutide, results showed that the use of liraglutide was associated with an increased risk of cholelithiasis [136] and consistent with results from other studies [132, 137]. The underlying mechanism for the slowed emptying of the gallbladder is that incretin-based drugs reduce smooth muscle tone in the gastrointestinal tract [138]. In addition, Rehfeld et al. showed that GLP-1 also attenuated gallbladder contractility by suppressing the secretion of cholecystokinin (CCK) after a meal in normal and diabetic subjects. The reduced CCK increased the risk of adverse gallbladder events during treatment with GLP-1-derived drugs [139]. Moreover, Smits et al. showed that liraglutide and sitagliptin induced changes in bile acids by altering the profile of the intestinal microbiome and increasing hepatic bile acid production, respectively [140]. These effects of incretin-based drugs all facilitate gallstone formation.
Secondly, incretin-based drugs are positively related to several inflammatory biliary diseases. Studies have shown that the use of GLP-1 RAs was associated with an increased risk of cholelithiasis, cholecystitis, and cholangitis [132, 141]. Consistently, in an updated meta-analysis of 76 randomized trials involving 103,371 patients, results showed that GLP-1 RAs treatment was associated with increased risks of cholelithiasis, cholecystitis, and biliary disease (including bile duct obstruction, stenosis, and stone; biliary colic, cyst, and fistula; biliary tract cancer; cholecystectomy, cholecystitis, and cholelithiasis; and cholangitis), and showed a dose-response relationship [16].
4 Conclusion
Insulin and incretin-based drugs might be important risk factors for BTC in diabetic patients. It remains a challenge to elucidate their association due to the relatively low prevalence of BTC and the intricate molecular mechanisms involved. Furthermore, the current strategy of analysis seems to be problematic and will blur the truth. At present, most available studies did not take into account the heterogeneity of BTC. The current studies mixed all BTC types together for analysis or even included HCC in BTC for evaluation. This may be the main reason for the inconsistency between the results of different studies. For instance, if incretin-based drugs are significantly associated with an increased risk of ICC but not ECC and GBC, then studies that include more ICC cases are likely to conclude that incretin-based drugs are associated with an increased risk of BTC, and at one extreme, all BTC included are ICC. In contrast, those studies that include more ECC and GBC may conclude that incretin-based drugs are not associated with an increased risk of BTC. In consideration of the heterogeneity of BTC and the complex effects of different types of insulin and incretin-based drugs, the key to clarifying their relationship is to classify these drugs and BTC specifically into different subtypes during the investigation. We suggest that experimental studies in this field should classify the incretin-based drugs by specific pharmacological mechanisms and strictly identify different types of BTC by clinicopathological and molecular features. That is, a specific drug (e.g., exenatide) is paired with a specific BTC (e.g., ICC), rather than studying the relationship between GLP-1 and BTC in general. Particularly, separate experiments should be conducted to verify whether the conclusions drawn from one drug-cancer pair can be applied to another. This strategy is also applicable to the study of incretin-based drugs and other cancers, such as liraglutide-TNBC and liraglutide-MCF-7 as mentioned above. Furthermore, by taking advantage of electronic health record databases and conducting more large-scale and in-depth studies, more promising achievements can be obtained in the future.
Data availability
Not applicable.
Code availability
Not applicable.
References
Wardell CP, Fujita M, Yamada T. et.al. Genomic characterization of biliary tract cancers identifies driver genes and predisposing mutations. J Hepatol. 2018;68(5):959–69.
Valle JW, Lamarca A, Goyal L. New horizons for precision medicine in biliary tract cancers. Cancer Discov. 2017;7(9):943–62.
Clements O, Eliahoo J, Kim JU. Risk factors for intrahepatic and extrahepatic cholangiocarcinoma: a systematic review and meta-analysis. J Hepatol. 2020;72:95–103.
Torre LA, Siegel RL, Islami F. Worldwide burden of and trends in mortality from gallbladder and other biliary tract cancers. Clin Gastroenterol Hepatol. 2018;16:427–37.
Tyson GL, El-Serag HB. Risk factors for cholangiocarcinoma. Hepatology. 2011;54:173–84.
Welzel TM, Mellemkjaer L, Gloria G, et al. Risk factors for intrahepatic cholangiocarcinoma in a low-risk population: a nationwide case-control study. Int J Cancer. 2007;120:638–41.
Shaib YH, El-Serag HB, Davila JA. et.al. Risk factors of intrahepatic cholangiocarcinoma in the United States: a case-control study. Gastroenterology. 2005;128:620–6.
Sun H, Saeedi P, Karuranga S, et al. IDF Diabetes Atlas: Global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Res Clin Pract. 2022;183:109–19.
Wu JW, Azoulay L, Majdan A. Long-term use of long-acting insulin analogs and breast cancer incidence in women with type 2 diabetes. J Clin Oncol. 2017;35(32):3647–53.
Li D, Yeung SC, Hassan MM. et.al. Antidiabetic therapies affect risk of pancreatic cancer. Gastroenterology. 2009;137:482–8.
Russo JW, Gao C, Bhasin SS, et al. Downregulation of dipeptidyl peptidase 4 accelerates progression to castration-resistant prostate cancer. Cancer Res. 2018;78(22):6354–62.
Tseng CH. Sitagliptin use and thyroid cancer risk in patients with type 2 diabetes. Oncotarget. 2016;7(17):248: 71–79.
Tseng CH. Sitagliptin and pancreatic cancer risk in patients with type 2 diabetes. Eur J Clin Invest. 2016;46(1):70–9.
Shadboorestan A, Tarighi P, Koosha M, et al. Growth promotion and increased ATP-binding cassette transporters expression by liraglutide in triple negative breast cancer cell line MDA-MB-231. Drug Res (Stuttg). 2021;71(6):307–11.
Qi X, He P, Yao H, et al. Insulin therapy and biliary tract cancer: insights from real-world data. Endocr Connect. 2022. doi:https://doi.org/10.1530/EC-21-0546.
He L, Wang J, Ping F, et al. Association of glucagon-like peptide-1 receptor agonist use with risk of gallbladder and biliary diseases: a systematic review and meta-analysis of randomized clinical trials. JAMA Intern Med. 2022;182(5):513–9.
Abrahami D, Douros A, Yin H, et al. Incretin based drugs and risk of cholangiocarcinoma among patients with type 2 diabetes: population based cohort study. BMJ. 2018. doi:https://doi.org/10.1136/bmj.k4880.
Hopkins BD, Goncalves MD, Cantley LC. Insulin-PI3 K signalling: an evolutionarily insulated metabolic driver of cancer. Nat Rev Endocrinol. 2020;16:276–83.
Hopkins BD, Pauli C, Du X, et al. Suppression of insulin feedback enhances the efficacy of PI3 K inhibitors. Nature. 2018;560:499–503.
Molinaro A, Becattini B, Mazzoli A, et al. Insulin-driven PI3K-AKT signaling in the hepatocyte is mediated by redundant PI3Kα and PI3Kβ activities and Is promoted by RAS. Cell Metab. 2019;29:1400–9.
Yoon MS. The role of mammalian target of rapamycin (mTOR) in insulin signaling. Nutrients. 2017. doi:https://doi.org/10.3390/nu9111176.
Nemazanyy I, Espeillac C, Pende M, Panasyuk G. Role of PI3 K, mTOR and Akt2 signalling in hepatic tumorigenesis via the control of PKM2 expression. Biochem Soc Trans. 2013;41:917–22.
Sarbassov DD, Ali SM, Sabatini DM. Growing roles for the mTOR pathway. Curr Opin Cell Biol. 2005;17:596–603.
Di Camillo B, Carlon A, Eduati F, et al. A rule-based model of insulin signalling pathway. BMC Syst Biol. 2016. doi:https://doi.org/10.1186/s12918-016-0281-4.
Yonezawa K, Ando A, Kaburagi Y, et al. Signal transduction pathways from insulin receptors to Ras. Analysis by mutant insulin receptors. J Biol Chem. 1994;269(6):4634–40.
Mardilovich K, Pankratz SL, Shaw LM. Expression and function of the insulin receptor substrate proteins in cancer. Cell Commun Signal. 2009. doi:https://doi.org/10.1186/1478-811X-7-14.
Belfiore A, Frasca F, Pandini G, et al. Insulin receptor isoforms and insulin receptor/insulin-like growth factor receptor hybrids in physiology and disease. Endocr Rev. 2009;30:586–623.
Kido Y, Nakae J, Accili D. The insulin receptor and its cellular targets. J Clin Endocrinol Metab. 2001;86:972–9.
Gutmann T, Schäfer IB, Poojari C, et al. Cryo-EM structure of the complete and ligand-saturated insulin receptor ectodomain. J Cell Biol. 2020. doi:https://doi.org/10.1083/jcb.201907210.
Myers MG, Wang LM, Sun XJ, et al. Role of IRS-1-GRB-2 complexes in insulin signaling. Mol Cell Biol. 1994;14:3577–87.
Nagao H, Cai W, Wewer Albrechtsen NJ, et al. Distinct signaling by insulin and IGF-1 receptors and their extra- and intracellular domains. Proc Natl Acad Sci USA. 2021. https://doi.org/10.1073/pnas.2019474118.
Zhang S, Weinheimer C, Courtois M, et al. The role of the Grb2-p38 MAPK signaling pathway in cardiac hypertrophy and fibrosis. J Clin Invest. 2003. doi:https://doi.org/10.1172/JCI16290.
Zhang W, Liu HT. MAPK signal pathways in the regulation of cell proliferation in mammalian cells. Cell Res. 2002. doi:https://doi.org/10.1038/sj.cr.7290105.
Schnelzer A, Prechtel D, Knaus U, et al. Rac1 in human breast cancer: overexpression, mutation analysis, and characterization of a new isoform, Rac1b. Oncogene. 2000;19:3013–20.
Bid HK, Roberts RD, Manchanda PK, et al. RAC1: an emerging therapeutic option for targeting cancer angiogenesis and metastasis. Mol Cancer Ther. 2013;12:1925–34.
Zou T, Mao X, Yin J, et al. Emerging roles of RAC1 in treating lung cancer patients: emerging roles of RAC1 in treating lung cancer patients. Clin Genet. 2017;91:520–8.
Yang WH, Lan HY, Huang CH, et al. RAC1 activation mediates Twist1-induced cancer cell migration. Nat Cell Biol. 2012;14:366–74.
Heid I, Lubeseder–Martellato C, Sipos B, et al. Early requirement of Rac1 in a mouse model of pancreatic cancer. Gastroenterology. 2011;141:719–30.
Emami Nejad A, Najafgholian S, Rostami A, et al. The role of hypoxia in the tumor microenvironment and development of cancer stem cell: a novel approach to developing treatment. Cancer Cell Int. 2021. doi:https://doi.org/10.1186/s12935-020-01719-5.
De Meyts P, Whittaker J. Structural biology of insulin and IGF1 receptors: implications for drug design. Nat Rev Drug Discov. 2002;1(10):769–83.
Ullrich A, Gray A, Tam AW, et al. Insulin-like growth factor I receptor primary structure: comparison with insulin receptor suggests structural determinants that define functional specificity. EMBO J. 1986;5(10):2503–12.
Le Roith D. Regulation of proliferation and apoptosis by the insulin-like growth factor I receptor. Growth Horm IGF Res. 2000;10(Suppl A):12–3.
Nakae J, Kido Y, Accili D. Distinct and overlapping functions of insulin and IGF-I receptors. Endocr Rev. 2001;22(6):818–35.
Boucher J, Tseng YH, Kahn CR. Insulin and insulin-like growth factor-1 receptors act as ligand-specific amplitude modulators of a common pathway regulating gene transcription. J Biol Chem. 2010;285(22):17235–45.
Brismar K, Fernqvist-Forbes E, Wahren J, Hall K. Effect of insulin on the hepatic production of insulin-like growth factor-binding protein-1 (IGFBP-1), IGFBP-3, and IGF-I in insulin-dependent diabetes. J Clin Endocrinol Metab. 1994;79(3):872–8.
Clayton PE, Banerjee I, Murray PG, Renehan AG. Growth hormone, the insulin-like growth factor axis, insulin and cancer risk. Nat Rev Endocrinol. 2011;7(1):11–24.
Yang YX, Hennessy S, Lewis JD. Insulin therapy and colorectal cancer risk among type 2 diabetes mellitus patients. Gastroenterology. 2004;127(4):1044–50.
Yin S, Bai H, Jing D. Insulin therapy and colorectal cancer risk among type 2 diabetes mellitus patients: a systemic review and meta-analysis. Diagn Pathol. 2014. doi:https://doi.org/10.1186/1746-1596-9-91.
Tseng CH. Human insulin therapy is associated with an increased risk of lung cancer: a population-based retrospective cohort study. Front Endocrinol (Lausanne). 2019. https://doi.org/10.3389/fendo.2019.00443.
Tseng CH. Prolonged use of human insulin increases breast cancer risk in Taiwanese women with type 2 diabetes. BMC Cancer. 2015. doi:https://doi.org/10.1186/s12885-015-1876-7.
Bodmer M, Becker C, Meier C, et al. Use of antidiabetic agents and the risk of pancreatic cancer: a case-control analysis. Am J Gastroenterol. 2012;107(4):620–6.
Liu XL, Wu H, Zhao LG, et al. Association between insulin therapy and risk of liver cancer among diabetics: a meta-analysis of epidemiological studies. Eur J Gastroenterol Hepatol. 2018;30(1):1–8.
Libby G, Donnelly LA, Donnan PT, et al. New users of metformin are at low risk of incident cancer:a cohort study among people with type 2 diabetes. Diabetes Care. 2009;32:1620–5.
Miele L, Bosetti C, Turati F, et al. Diabetes and insulin therapy, but not metformin, are related to hepatocellular cancer risk. Gastroenterol Res Pract. 2015. https://doi.org/10.1155/2015/570356.
Vicentini M, Ballotari P, Venturelli F, et al. Impact of insulin therapies on cancer incidence in type 1 and type 2 diabetes: a population-based cohort study in Reggio Emilia, Italy. Cancers (Basel). 2022. https://doi.org/10.3390/cancers14112719.
Saisana M, Griffin SM, May FEB. Insulin and the insulin receptor collaborate to promote human gastric cancer. Gastric Cancer. 2022;25(1):107–23.
Rose DP, Vona-Davis L. The cellular and molecular mechanisms by which insulin influences breast cancer risk and progression. Endocr Relat Cancer. 2012;19(6):R225–41.
Banales JM, Cardinale V, Carpino G, et al. Expert consensus document: cholangiocarcinoma: current knowledge and future perspectives consensus statement from the European Network for the Study of Cholangiocarcinoma (ENS-CCA). Nat Rev Gastroenterol Hepatol. 2016;13:261–80.
Banales JM, Marin JJG, Lamarca A, et al. Cholangiocarcinoma 2020: the next horizon in mechanisms and management. Nat Reviews Gastroenterol Hepatol. 2020;17:557–88.
Schlesinger S, Aleksandrova K, Pischon T, et al. Diabetes mellitus, insulin treatment, diabetes duration, and risk of biliary tract cancer and hepatocellular carcinoma in a European cohort. Ann Oncol. 2013;24(9):2449–55.
Moeini A, Haber PK, Sia D. Cell of origin in biliary tract cancers and clinical implications. JHEP Rep. 2021. doi:https://doi.org/10.1016/j.jhepr.2021.100226.
Nakagawa H, Hayata Y, Yamada T, et al. Peribiliary glands as the cellular origin of biliary tract cancer. Int J Mol Sci. 2018. https://doi.org/10.3390/ijms19061745.
Carpino G, Puca R, Cardinale V. Peribiliary glands as a niche of extrapancreatic precursors yielding insulin-producing cells in experimental and human diabetes. Stem Cells. 2016;34(5):1332–42.
Mu L, Zhu N, Zhang J, et al. Type 2 diabetes, insulin treatment and prognosis of breast cancer. Diabetes Metab Res Rev. 2017. doi:https://doi.org/10.1002/dmrr.2823.
Chen L, Chubak J, Boudreau DM, et al. Diabetes treatments and risks of adverse breast cancer outcomes among early-stage breast cancer patients: a SEER-medicare analysis. Cancer Res. 2017;77(21):6033–41.
Carstensen B, Witte DR, Friis S. Cancer occurrence in Danish diabetic patients: duration and insulin effects. Diabetologia. 2012;55(4):948–58.
Ghidini M, Pizzo C, Botticelli A, et al. Biliary tract cancer: current challenges and future prospects. Cancer Manag Res. 2018;11:379–88.
Kendall T, Verheij J, Gaudio E. et.al. Anatomical, histomorphological and molecular classification of cholangiocarcinoma. Liver Int. 2019;39(Suppl 1):7–18.
Roa I, de Toro G, Schalper K. Overexpression of the HER2/neu gene: a new therapeutic possibility for patients With advanced gallbladder cancer. Gastrointest Cancer Res. 2014;7(2):42–8.
Uprety D, Adjei AA. KRAS: From undruggable to a druggable cancer target. Cancer Treat Rev. 2020. https://doi.org/10.1016/j.ctrv.2020.102070.
Zhang YE. Non-Smad pathways in TGF-beta signaling. Cell Res. 2009;19:128–39.
Connolly EC, Freimuth J, Akhurst RJ. Complexities of TGF-beta targeted cancer therapy. Int J Biol Sci. 2012;8:964–78.
Graaf Cd, Donnelly D, Wootten D, et al. Glucagon-like peptide-1 and its class B G protein-coupled receptors: a long march to therapeutic successes. Pharmacol Rev. 2016;68(4):954–1013.
Lund PK. The discovery of glucagon-like peptide 1. Regul Pept. 2005;128(2):93–6.
Carlessi R, Chen Y, Rowlands J, et al. GLP-1 receptor signalling promotes beta-cell glucose metabolism via mTOR-dependent HIF-1alpha activation. Sci Rep. 2017. doi:https://doi.org/10.1038/s41598-017-02838-2.
Rowlands J, Cruzat V, Carlessi R, et al. Insulin and IGF-1 receptor autocrine loops are not required for Exendin-4 induced changes to pancreatic β-cell bioenergetic parameters and metabolism in BRIN-BD11 cells. Peptides. 2018;100:140–9.
Cornu M, Modi H, Kawamori D, et al. Glucagon-like peptide-1 increases beta-cell glucose competence and proliferation by translational induction of insulin-like growth factor-1 receptor expression. J Biol Chem. 2010;285:10538–45.
Van de S, Velde, Hogan MF, Montminy M. mTOR links incretin signaling to HIF induction in pancreatic beta cells. Proc Natl Acad Sci USA. 2011;108:16876–82.
Beguin P, Nagashima K, Nishimura M, et al. PKA-mediated phosphorylation of the human K(ATP) channel: separate roles of Kir6.2 and SUR1 subunit phosphorylation. EMBO J. 1999;1:4722–32.
Meloni AR, DeYoung MB, Lowe C, et al. GLP-1 receptor activated insulin secretion from pancreatic β-cells: mechanism and glucose dependence. Diabetes Obes Metab. 2013;15:15–27.
Kang GX, Leech CA, Chepurny OG, et al. Role of the cAMP sensor Epac as a determinant of K-ATP channel ATP sensitivity in human pancreatic beta-cells and rat INS-1 cells. J Phys Lond. 2008;586:1307–19.
Chitnis MM, Yuen JS, Protheroe AS, et al. The type 1 insulin-like growth factor receptor pathway. Clin Cancer Res. 2008;14:6364–70.
Donnelly D. The structure and function of the glucagon-like peptide-1 receptor and its ligands. Br J Pharmacol. 2012;166:27–41.
Buteau J, Foisy S, Joly E, et al. Glucagon-like peptide 1 induces pancreatic β-cell proliferation via transactivation of the epidermal growth factor receptor. Diabetes. 2003;52:124–32.
Jhala US, Canettieri G, Screaton RA, et al. cAMP promotes pancreatic beta-cell survival via CREB-mediated induction of IRS2. Genes Dev. 2003;17:1575–80.
Buteau J, El-Assaad W, Rhodes C, et al. Glucagon-like peptide-1 prevents beta cell glucolipotoxicity. Diabetologia. 2004;47:806–15.
Tsunekawa S, Yamamoto N, Tsukamoto K, et al. Protection of pancreatic β-cells by exendin-4 may involve the reduction of endoplasmic reticulum stress; in vivo and in vitro studies. J Endocrinol. 2007;193:65–74.
Shimoda M, Kanda Y, Hamamoto S, et al. The human glucagon-like peptide-1 analogue liraglutide preserves pancreatic beta cells via regulation of cell kinetics and suppression of oxidative and endoplasmic reticulum stress in a mouse model of diabetes. Diabetologia. 2011;54:1098–108.
Yusta B, Baggio LL, Estall JL, et al. GLP-1 receptor activation improves β cell function and survival following induction of endoplasmic reticulum stress. Cell Metab. 2006;4:391–406.
Biden TJ, Boslem E, Chu KY, et al. Lipotoxic endoplasmic reticulum stress, β cell failure, and type 2 diabetes mellitus. Trends Endocrinol Metab. 2014;25:389–98.
Buteau J. GLP-1 receptor signaling: effects on pancreatic β-cell proliferation and survival. Diabetes Metab. 2008;34(Suppl.):2:S73–7.
Cunha DA, Ladrière L, Ortis F, et al. Glucagon-like peptide-1 agonists protect pancreatic β-cells from lipotoxic endoplasmic reticulum stress through upregulation of BiP and JunB. Diabetes. 2009;58:2851–62.
Deacon CF, Nauck MA, Toft-Nielsen M, et al. Both subcutaneously and intravenously administered glucagon-like peptide 1 are rapidly degraded from the NH2-terminus in type 2-diabetic patients and in healthy subjects. Diabetes. 1995;44:1126–31.
Deacon CF, Pridal L, Klarskov L, et al. Glucagon-like peptide 1 undergoes differential tissue-specific metabolism in the anesthetized pig. Am J Physiol. 1996;271:E 458–E 464.
Pinkney J, Fox T, Ranganath L. Selecting. GLP-1 agonists in the management of type 2 diabetes: differential pharmacology and therapeutic benefits of liraglutide and exenatide. Ther Clin Risk Manag. 2010;6:401–11.
Chia CW, Egan JM. Incretin-based therapies in type 2 diabetes mellitus. J Clin Endocrinol Metab. 2008;93:3703–16.
Nauck MA, Quast DR, Wefers J, et al. GLP-1 receptor agonists in the treatment of type 2 diabetes - state-of-the-art. Mol Metab. 2021. doi:https://doi.org/10.1016/j.molmet.2020.101102.
Fusco J, Xiao X, Prasadan K, et al. GLP-1/Exendin-4 induces β-cell proliferation via the epidermal growth factor receptor. Sci Rep. 2017. https://doi.org/10.1038/s41598-017-09898-4.
Baggio LL, Drucker DJ. Biology of incretins: GLP-1 and GIP. Gastroenterology. 2007;132(6):2131–57.
Karaca M, Magnan C, Kargar C. Functional pancreatic beta-cell mass: involvement in type 2 diabetes and therapeutic intervention. Diabetes Metab. 2009;35(2):77–84.
Yin R, Xu Y, Wang X, et al. Role of Dipeptidyl Peptidase 4 Inhibitors in Antidiabetic Treatment. Molecules. 2022. doi:https://doi.org/10.3390/molecules27103055.
Zhang Y, Xu F, Liang H, et al. Exenatide inhibits the growth of endometrial cancer Ishikawa xenografts in nude mice. Oncol Rep. 2016;35(3):1340–8.
Ligumsky H, Wolf I, Israeli S, et al. The peptide-hormone glucagon-like peptide-1 activates cAMP and inhibits growth of breast cancer cells. Breast Cancer Res Treat. 2012;132(2):449–61.
Koehler JA, Kain T, Drucker DJ. Glucagon-like peptide-1 receptor activation inhibits growth and augments apoptosis in murine CT26 colon cancer cells. Endocrinology. 2011;152(9):3362–72.
Nomiyama T, Kawanami T, Irie S, et al. Exendin-4, a GLP-1 receptor agonist, attenuates prostate cancer growth. Diabetes. 2014;63(11):3891–905.
Singh S, Chang H, Richards TM, et al. Glucagonlike peptide 1–based therapies and risk of hospitalization for acute pancreatitis in type 2 diabetes mellitus: a population-based matched case-control study. JAMA Intern Med. 2013;173(7):534–9.
Labuzek K, Kozłowski M, Szkudłapski D, et al. Incretin-based therapies in the treatment of type 2 diabetes–more than meets the eye? Eur J Intern Med. 2013;24(3):207–12.
Kameoka J, Tanaka T, Nojima Y, et al. Direct association of adenosine deaminase with a T cell activation antigen, CD26. Science. 1993;261:466–9.
Ohnuma K, Dang NH, Morimoto C. Revisiting an old acquaintance: CD26 and its molecular mechanisms in T cell function. Trends Immunol. 2008;29:295–301.
Thul PJ, Åkesson L, Wiking M, et al. A subcellular map of the human proteome. Science. 2017. doi:https://doi.org/10.1126/science.aal3321.
Waumans Y, Baerts L, Kehoe K, et al. The dipeptidyl peptidase family, prolyl oligopeptidase, and prolyl carboxypeptidase in the immune system and inflammatory disease, including atherosclerosis. Front Immunol. 2015. doi:https://doi.org/10.3389/fimmu.2015.00387.
Deacon CF. Physiology and pharmacology of DPP-4 in glucose homeostasis and the treatment of type 2 diabetes. Front Endocrinol (Lausanne). 2019. https://doi.org/10.3389/fendo.2019.00080.
Broxmeyer HE, Hoggatt J, O’Leary HA, et al. Dipeptidylpeptidase 4 negatively regulates colony-stimulating factor activity and stress hematopoiesis. Nat Med. 2012;18:1786–96.
Proost P, Struyf S, Schols D, et al. Truncation of macrophage-derived chemokine by CD26/ dipeptidyl-peptidase IV beyond its predicted cleavage site affects chemotactic activity and CC chemokine receptor 4 interaction. J Biol Chem. 1999;274:3988–93.
Shao S, Xu Q, Yu X, et al. Dipeptidyl peptidase 4 inhibitors and their potential immune modulatory functions. Pharmacol Ther. 2020. doi:https://doi.org/10.1016/j.pharmthera.2020.107503.
Qin CJ, Zhao LH, Zhou X, et al. Inhibition of dipeptidyl peptidase IV prevents high fat diet-induced liver cancer angiogenesis by downregulating chemokine ligand 2. Cancer Lett. 2018;420:26–37.
Hollande C, Boussier J, Ziai J, et al. Inhibition of the dipeptidyl peptidase DPP4 (CD26) reveals IL-33-dependent eosinophil-mediated control of tumor growth. Nat Immunol. 2019;20:257–64.
Lam CS, Cheung AH, Wong SK, et al. Prognostic significance of CD26 in patients with colorectal cancer. PLoS ONE. 2014. doi:https://doi.org/10.1371/journal.pone.0098582.
Liang PI, Yeh BW, Li WM, et al. DPP4/CD26 overexpression in urothelial carcinoma confers an independent prognostic impact and correlates with intrinsic biological aggressiveness. Oncotarget. 2017;8(2):2995–3008.
Choi HJ, Kim JY, Lim SC, et al. Dipeptidyl peptidase 4 promotes epithelial cell transformation and breast tumourigenesis via induction of PIN1 gene expression. Br J Pharmacol. 2015;172(21):5096–109.
Yang X, Zhang X, Wu R, et al. DPPIV promotes endometrial carcinoma cell proliferation, invasion and tumorigenesis. Oncotarget. 2017;8:8679–92.
Mentlein R. Dipeptidyl-peptidase IV (CD26)–role in the inactivation of regulatory peptides. Regul Pept. 1999;85:19–24.
Yu DM, Yao TW, Chowdhury S, et al. The dipeptidyl peptidase IV family in cancer and cell biology. FEBS J. 2010;277:1126–44.
Lambeir AM, Durinx C, Scharpé S, et al. Dipeptidyl-peptidase IV from bench to bedside: an update on structural properties, functions, and clinical aspects of the enzyme DPP IV. Crit Rev Clin Lab Sci. 2003;40:209–94.
Liu ZZ, Duan XX, Yuan MC, et al. Glucagon-like peptide-1 receptor activation by liraglutide promotes breast cancer through NOX4/ROS/VEGF pathway. Life Sci. 2022. doi:https://doi.org/10.1016/j.lfs.2022.120370.
Wang J, Kim CH. Differential risk of cancer associated with glucagon-like peptide-1 receptor agonists: analysis of real-world databases. Endocr Res. 2022;47(1):18–25.
Alanteet AA, Attia HA, Shaheen S, et al. Anti-proliferative activity of glucagon-like peptide-1 receptor agonist on obesity-associated breast cancer: the impact on modulating adipokines’ expression in adipocytes and cancer cells. Dose Response. 2021. https://doi.org/10.1177/1559325821995651.
Marzioni M, Alpini G, Saccomanno S, et al. Glucagon-like peptide-1 and its receptor agonist exendin-4 modulate cholangiocyte adaptive response to cholestasis. Gastroenterology. 2007;133(1):244–55.
Marzioni M, Alpini G, Saccomanno S, et al. Exendin-4, a glucagon-like peptide 1 receptor agonist, protects cholangiocytes from apoptosis. Gut. 2009;58(7):990–7.
Chen BD, Zhao WC, Dong JD, et al. Expression of GLP-1R protein and its clinical role in intrahepatic cholangiocarcinoma tissues. Mol Biol Rep. 2014;41:4313–20.
Marso SP, Daniels GH, Brown-Frandsen K, et al. Liraglutide and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2016;375(4):311–22.
Leiter LA, Teoh H, Mosenzon O, et al. Frequency of cancer events with saxagliptin in the SAVOR-TIMI 53 trial. Diabetes Obes Metab. 2016;18(2):186–90.
Giorda CB, Picariello R, Tartaglino B, et al. Incretin-based therapy and risk of cholangiocarcinoma: a nested case-control study in a population of subjects with type 2 diabetes. Acta Diabetol. 2020;57(4):401–8.
Ueda P, Wintzell V, Melbye M, et al. Use of incretin-based drugs and risk of cholangiocarcinoma: Scandinavian cohort study. Diabetologia. 2021;64(10):2204–14.
Keller J, Trautmann ME, Haber H, et al. Effect of exenatide on cholecystokinin-induced gallbladder emptying in fasting healthy subjects. Regul Pept. 2012;179(1–3):77–83.
Pi-Sunyer X, Astrup A, Fujioka K, et al. A randomized, controlled trial of 3.0 mg of liraglutide in weight management. N Engl J Med. 2015;373(1):11–22.
Korkmaz H, Araz M, Alkan S, et al. Liraglutide-related cholelithiasis. Aging Clin Exp Res. 2015;27(5):751–3.
Tolessa T, Gutniak M, Holst JJ, et al. Glucagon-like peptide-1 retards gastric emptying and small bowel transit in the rat: effect mediated through central or enteric nervous mechanisms. Dig Dis Sci. 1998;43(10):2284–90.
Rehfeld JF, Knop FK, Asmar A, et al. Cholecystokinin secretion is suppressed by glucagon-like peptide-1: clue to the mechanism of the adverse gallbladder events of GLP-1-derived drugs. Scand J Gastroenterol. 2018;53(12):1429–32.
Smits MM, Tonneijck L, Muskiet MH, et al. Biliary effects of liraglutide and sitagliptin, a 12-week randomized placebo-controlled trial in type 2 diabetes patients. Diabetes Obes Metab. 2016;18(12):1217–25.
Faillie JL, Yu OH, Yin H, et al. Association of bile duct and gallbladder diseases with the use of incretin-based drugs in patients with type 2 diabetes mellitus. JAMA Intern Med. 2016;176(10):1474–81.
Funding
This project is funded by Hangzhou key project of medical health science and technology (ZD20220022).
Author information
Authors and Affiliations
Contributions
H.S. contributed to project conceptualization, literature search, revising, and approving the data in the manuscript; X.H.Q contributed to project conceptualization, literature search, writing of the manuscript, and generating the illustrations. All authors contributed to the critical revision and approval of the final submission of this work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sun, H., Qi, X. The role of insulin and incretin-based drugs in biliary tract cancer: epidemiological and experimental evidence. Discov Onc 13, 70 (2022). https://doi.org/10.1007/s12672-022-00536-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12672-022-00536-8