Abstract
Purpose
Cardiopulmonary bypass (CPB) induces a significant inflammatory response that may increase the risk for delirium. We hypothesized that exposure to CPB during coronary artery bypass grafting (CABG) surgery would correlate with an increased risk of delirium.
Methods
We reviewed clinical data from two databases at our medical centre - the Cardiac Surgery Perioperative Outcomes Database and the Society of Thoracic Surgeons Database. Patients undergoing elective CABG surgery (on-pump and off-pump) from November 1, 2009 to September 30, 2015 were included in the study. Delirium was defined as any postoperative positive Confusion Assessment Method for the Intensive Care Unit exam during the intensive care unit stay. We performed logistic regression to isolate the association between CPB exposure and delirium adjusted for predetermined risk factors and potential confounders.
Results
During the study period, 2,280 patients underwent elective CABG surgery, with 384 patients (16.9%) exposed to CPB. Delirium was diagnosed in 451 patients (19.8%). Exposure to CPB showed a significant independent association with delirium. Patients exposed to CPB for 142 min (90th percentile of CPB duration) vs those exposed for 54 min (10th percentile) had an adjusted relative risk (RR) of delirium of 2.18 (95% confidence interval [CI], 1.39 to 3.07; P = 0.002) vs a RR of 1.51 (95% CI, 0.92 to 2.29; P = 0.10), respectively.
Conclusions
The use and duration of cardiopulmonary bypass were associated with an increased risk of delirium in patients undergoing CABG surgery.
Trial registration
www.clinicaltrials.gov, NCT02548975. Registered 4 September 2015.
Résumé
Objectif
La circulation extracorporelle (CEC) cause une réaction inflammatoire significative qui pourrait augmenter le risque de délirium. Nous avons émis l’hypothèse que l’exposition à la CEC pendant une chirurgie de pontage aortocoronarien (PAC) serait corrélée à un risque accru de délirium.
Méthode
Nous avons passé en revue les données cliniques tirées de deux bases de données dans notre centre médical, soit la Base de données sur les résultats périopératoires de chirurgie cardiaque et la Base de données de la Société des chirurgiens thoraciques. Les patients subissant une chirurgie de PAC non urgente (avec ou sans CEC) entre le 1er novembre 2009 et le 30 septembre 2015 ont été inclus dans l’étude. Le délirium a été défini en tant que tout examen postopératoire positif selon la Méthode d’évaluation de la confusion en unité de soins intensifs (Confusion Assessment Method for the Intensive Care Unit – CAMICU) pendant le séjour à l’unité de soins intensifs. Nous avons réalisé une régression logistique afin d’isoler l’association entre l’exposition à une CEC et le délirium puis ajusté les résultats afin de tenir compte des facteurs de risque et des facteurs parasite potentiels.
Résultats
Pendant la période d’étude, 2280 patients ont subi une chirurgie de PAC non urgente, parmi lesquels 384 (16,9 %) patients ont été exposés à une CEC. Le délirium a été diagnostiqué chez 451 patients (19,8 %). Une association indépendante significative a été démontrée entre l’exposition à la CEC et le délirium. Les patients exposés à la CEC pendant 142 min (90ème percentile de durée de CEC) vs ceux exposés pendant 54 min (10ème percentile) ont affiché un risque relatif (RR) ajusté de délirium de 2,18 (intervalle de confiance [IC] 95 %, 1,39 à 3,07; P = 0,002) vs un RR de 1,51 (IC 95 %, 0,92 à 2,29; P = 0,10), respectivement.
Conclusion
L’utilisation et la durée de la circulation extracorporelle ont été associées à un risque accru de délirium chez les patients subissant une chirurgie de PAC.
Enregistrement de l’étude
www.clinicaltrials.gov, NCT02548975. Enregistrée le 4 septembre 2015.
Similar content being viewed by others
Up to 50% of patients older than 60 yrs experience postoperative delirium following cardiac surgery.1 Delirium is associated with many adverse hospital outcomes, including increased mortality and nosocomial complications, poor one-year functional recovery, and even postoperative cognitive decline (POCD).2-4 Studies investigating medications and other interventions to reduce the incidence of delirium have been conducted5; however, so far the results have not truly influenced clinical practice. A theory behind the development of delirium is that systemic inflammation causes disruption of the blood-brain barrier leading to a neuroinflammatory process in which neurons are susceptible to injury and dysfunction.6 Therefore, a condition or exposure that produces an inflammatory response, such as cardiopulmonary bypass (CPB), may increase the risk for delirium.
Several biomarkers implicated in the neuroinflammatory pathway have been investigated in POCD and also delirium after cardiac surgery.6-8 Studies have shown increases in biomarker levels, such as S100β for disruption of the blood-brain barrier and neuron-specific enolase for neuronal injury, to be indicative of cerebral damage in patients undergoing on-pump cardiac surgery compared with off-pump cases9-11 that may lead to a lower prevalence of delirium.12 These findings suggest a greater inflammatory response with exposure to CPB.
Previous studies have supported a link between delirium and POCD, suggesting that the cognitive disturbance seen in each condition may be related.13,14 Investigators have evaluated whether or not differences in POCD exist between patients exposed vs those not exposed to CPB during cardiac surgery. The results are inconclusive, with some suggesting greater POCD in CPB patients15 and others finding no difference.16,17 Studies investigating an association between CPB and delirium are lacking; hence, this is the main objective of our study.
Accordingly, we completed this study to test the hypothesis that exposure to CPB during coronary artery bypass grafting surgery would be associated with an increased incidence of postoperative delirium.
Methods
The Society of Thoracic Surgeons National Adult Cardiac Database (STS-NCD) was established in 1989 to compile perioperative data on patients undergoing cardiac surgery. Data are collected quarterly from Vanderbilt University Medical Center (VUMC) and entered into the STS-NCD. The Cardiac Surgery Perioperative Outcomes Database (POD) at VUMC is an Institutional Review Board (IRB) approved data registry of cardiac surgical patients. The POD links and stores patient information from the VUMC electronic medical record. Extensive information is recorded in the POD, including laboratory values, medical conditions, patient history, and some perioperative information, such as medications administered and surgical times. Both databases contain prospectively collected data on cardiac surgery patients at VUMC which are stored and managed using REDCap (Research Electronic Data Capture) tools.18
Data from the STS database at VUMC and the POD were linked using electronic medical record numbers and date of surgery to create a unique identifier. The data quality was verified by independent investigators (J.B.O. and F.T.B.), with frequent crosschecks for completeness and consistency of the datasets. The STS database for VUMC also undergoes both internal and external audits, with internal audits occurring quarterly to crosscheck data for accuracy. This paper has been structured according to the STrengthening the Reporting of OBservational studies in Epidemiology (STROBE) criteria for cohort studies.19 The VUMC IRB reviewed and approved the study on September 14, 2015 under protocol #151362.
Study design
This was a historical cohort study of patients undergoing either elective on-pump coronary artery bypass grafting (CABG) or off-pump coronary artery bypass grafting (OPCAB) cardiac surgery at VUMC from November 1, 2009 to September 30, 2015.
Variables
On-pump coronary artery bypass grafting surgeries were defined by the use of CPB at any time during coronary artery bypass grafting. Off-pump coronary artery bypass grafting surgeries were defined as surgeries in which CPB was not used during coronary artery bypass grafting. Only elective procedures were included in the study, and patients undergoing combined CABG and valve operations were excluded.
Primary outcome
Delirium was defined as any postoperative positive Confusion Assessment Method for the Intensive Care Unit (CAM-ICU) exam during the ICU stay. At our institution, ICU standard practice directs bedside nurses to perform a CAM-ICU exam twice per 12-hr shift. Delirium is a major emphasis within our institution, and nurses are extensively trained to complete an accurate CAM-ICU exam at bedside. Completing a CAM-ICU exam twice per 12-hr shift is considered standard of care within the ICU, and this frequency was initiated at our institution in 2007. Duration of delirium was defined as total number of days with CAM-ICU positive recorded in the patient’s chart (if a patient was positive for either one or both of the daily assessments, this was still considered a day of delirium). Delirium was not assessed after patients were transferred to the floor.
Secondary outcomes
In-hospital, 30-day, 60-day, 90-day, and one-year mortality data were obtained from the POD. Acute kidney injury (AKI) was defined using Kidney Disease: Improving Global Outcomes (KDIGO) stage 1, 2, or 3 serum creatinine (SCr) criteria.20 The development of postoperative atrial fibrillation (AF) was defined as a report of newly diagnosed AF in the patient’s medical record after surgery. Hospital length of stay (LOS) was reported in days. Postoperative stroke was defined as any confirmed neurological deficit of abrupt onset caused by a disturbance in blood supply to the brain that did not resolve within 24 hours per STS-NCD guidelines.
Statistical analysis
All patient demographic and clinical data were summarized using counts and percentiles, means and standard deviations, or medians [interquartile range (IQR)] by group (CABG/OPCAB). The Pearson Chi square and Deuchler-Wilcoxon tests were used to make unadjusted comparisons between groups. Logistic regression was performed to determine the adjusted association between exposure to CPB and the risk of delirium, KDIGO stage 1, KDIGO stage 2, AF, and one-year mortality, adjusting for the following pre-specified risk factors and potential confounders: history of cerebrovascular disease, age, race, body mass index (BMI), current tobacco use, chronic lung disease, history of diabetes, dyslipidemia, end-stage renal disease, hypertension, congestive heart failure, myocardial infarction, peripheral arterial disease, cerebrovascular disease, previous cardiac surgery, preoperative hematocrit, SCr, and glomerular filtration rate.
The effects of CPB were summarized using an adjusted relative risk (RR) with 95% confidence interval (CI). The adjusted RR was computed from the adjusted odds ratio using the method of Zhang and Yu,21 where the baseline risk was taken as the marginal risk among OPCAB patients. Goodness-of-fit for logistic regression analyses was examined using the C-statistic. Linear regression was used to quantify the association between CPB exposure and log-transformed LOS while adjusting for the same set of risk factors and confounders. Continuous covariates, including CPB duration and age, were modelled using restricted cubic splines with four evenly spaced knots. Given the nested relationship between CPB exposure (CABG group) and CPB duration, a multiple degree-of-freedom for likelihood ratio test22 was performed to test for overall associations with the outcomes. The effect of CPB duration vs OPCAB was further summarized by computing the adjusted RR at a sequence of percentiles of CPB duration (10th = 54 min, 25th = 73 min, 50th = 91 min, 75th = 113 min, and 90th percentile = 142 min), with pointwise Wald-type 95% CI. Normal quantile-quantile (Q-Q) plots were used to examine the residuals of linear regression analyses. The normal Q-Q plots for all the models did not show obvious deviations from the assumption of the normal distribution of the outcomes. The remaining binary outcomes of postoperative stroke, death in hospital, death within 30 days, 60 days, and 90 days were rare and thus were not analyzed using regression analysis. The statistical significance threshold (P < 0.05) was selected to preserve a 5% testwise type I error rate. We did not attempt to control the familywise type I error probability.
Results
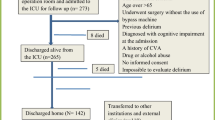
The final dataset included 5,659 cardiac surgery cases that met our inclusion criteria. Emergency cases (designated by American Society of Anesthesiologists physical status classification) and valve surgery cases were excluded, leaving 2,280 cases for the study (Fig. 1).
There were 386 (16.9%) patients exposed vs 1,894 (83.9%) patients not exposed to CPB. Delirium was diagnosed in 451 patients (19.8%) during their ICU stay. Median [IQR] age in the cohort was 63 [55 -70] yr, and female patients comprised 22.9% (Table 1). The demographics, including age, sex, and BMI, were similar between the groups. The CABG group had more comorbidities than the OPCAB group, including history of myocardial infarction, history of congestive heart failure, and current tobacco use. Other comorbidities and baseline laboratory values were similar across both groups.
Outcomes
The unadjusted univariate analyses are outlined in Table 2. After adjusting for risk factors and potential confounders, the estimated effect of CPB was unfavourable for each outcome (Table 3). After adjusting for potential confounders, there was strong evidence that use and duration of CPB were associated with an increased risk of postoperative delirium (P = 0.002). There was also an association between CPB use and hospital LOS (P = 0.047), though its strength is uncertain without adjusting for an interaction with CPB time itself or other potential covariates. After adjustment, there was no evidence of an association between CPB and other outcomes.
Extended CPB duration was associated with an increased risk of delirium and potentially prolonged hospital stay. When compared with OPCAB procedures, the risk of delirium was more than twofold greater (RR, 2.18; 95% CI, 1.39 to 3.07; P = 0.002) among patients who were exposed to CPB for 142 min (90th percentile of CPB duration). This compares with the adjusted RR of only 1.51 (95% CI, 0.92 to 2.29; P = 0.10) for those on CPB for 54 min (10th percentile) (Fig. 2). Hospital LOS was prolonged by 12% (95% CI, 0 to 25; P = 0.05) and 3% (95% CI, −7 to 14; P = 0.59) for patients on CPB for 142 and 54 min, respectively (Fig. 3).
Independent Association between CPB duration and risk of Delirium. The figure illustrates the adjusted relative risk of delirium as a function of CPB time for on-pump vs off-pump CABG cases (P = 0.002) with pointwise 95% confidence band. The rug plot along the horizontal axis shows the distribution of CPB times in this cohort. CPB = cardiopulmonary bypass
Independent Association between CPB duration and relative hospital length of stay. The figure illustrates the relative hospital length of stay as a function of CPB time for on-pump vs off-pump CABG cases (P = 0.047) with pointwise 95% confidence band. The rug plot along the horizontal axis shows the distribution of CPB times in this cohort. CPB = cardiopulmonary bypass
Discussion
In our study, CPB exposure and duration were significantly associated with the incidence of delirium following cardiac surgery. As duration of CPB increased, hospital LOS also increased, though we could not rule out an interaction with delirium itself (or other covariates). Other secondary outcomes, including mortality, postoperative AF, and AKI stages 1 and 2, showed increasing odds with prolonged CPB duration, although these findings were not statistically significant.
The overall incidence of delirium was 19.8%, which corresponds to previous studies.23,24 Studies of the potential effect of CPB on postoperative delirium are lacking, but several studies have investigated an association between CPB exposure and POCD, which may be linked to postoperative delirium.13,15-17 In a study conducted by Baba et al. in elderly patients with severe systemic atherosclerosis, results showed reduced POCD in OPCAB vs CABG patients when neuropsychological dysfunction was measured one week postoperatively.15 In a meta-analysis of eight randomized trials, no difference was found between OPCAB and CABG patients when evaluating for POCD.16 Results of a pilot study investigating postoperative delirium and POCD showed that patients undergoing valve surgery with or without CABG had higher rates of both delirium and POCD than patients undergoing CABG alone.25 This study did not directly analyze the effects of CPB duration with either outcome, although the valve surgery with or without CABG group had significantly longer mean (SD) runs on CPB compared with the CABG alone group [173 (53) min vs 139 (37) min; P = 0.01].25 Results of another study which aimed to construct a predictive model for delirium in cardiac surgery patients showed increased odds for delirium with increased duration (per 30 min) of surgery (OR, 1.3; 95% CI, 1.1 to 1.5; P < 0.001). In our study, the odds of delirium increased as CPB duration increased, suggesting that prolonged CPB duration may contribute to an increased risk of delirium postoperatively.
Acute kidney injury occurs in up to 30% of cardiac surgery patients.26 A link between on-pump coronary artery grafting cardiac surgery and AKI has been investigated, but previous studies have shown marginal benefit with OPCAB in preventing this insult.27-29 Our study is consistent with these findings as there was no significant difference between the CABG and OPCAB groups at any stage of AKI. Thus, our results do not suggest an advantage to avoiding the use of CPB and/or limiting the duration of exposure to CPB for the outcome of AKI in patients undergoing CABG surgery.
The development of AF after cardiac surgery is fairly common and the incidence may be as high as 50%.30-32 Considering the significant amount of systemic inflammation generated during on-pump cardiac surgery, the use of CPB may be a risk factor for developing AF following cardiac surgery.33 This theory is supported by Davoodi et al. in their study which showed a higher prevalence of postoperative AF in patients exposed vs not exposed to CPB.34 In our study, the odds of postoperative AF steadily increased with longer bypass run; however, this finding was not statistically significant and does not support an association between CPB and AF.
In our cohort, the incidence of stroke among patients undergoing OPCAB was similar to that of CABG patients. A meta-analysis of randomized trials comparing on-pump with off-pump CABG surgery showed a 20.7% reduction in the incidence of stroke in off-pump patients.35 Nevertheless, a Cochrane review of 86 randomized trials did not show a difference in stroke rates when comparing on-pump with off-pump patients.36 With such a low incidence of stroke in this patient population, finding a statistically significant difference may be difficult. Our results do not advocate a true benefit to OPCAB for a reduction in the rate of postoperative stroke.
Limitations
The cohort’s large population strengthens our study. The databases used in the study (VUMC POD and VUMC STS) contain prospectively collected data. Even so, limitations should be considered before interpreting our results.
Our study was completed at a single tertiary medical centre, and the generalizability of our findings should be considered. There is also an institutional bias towards OPCAB over CABG at VUMC. Another consideration is selection bias for or against on-pump surgery based on surgeon preference or known patient comorbidities. Other surgical techniques were not accounted for in this study, including the use of single or partial aortic cross-clamp, how the proximal anastomoses were implanted, the location and type of cannulae used for on-pump CABG, and other variances between surgeons. The analyses were completed with adjustments for several confounders and risk factors; however, residual confounding could be present as this was a non-randomized study. Known risk factors for delirium, such as dementia, decreased functional status, and psychiatric illness, were not incorporated into the model.37 Hemodynamic data were not available for inclusion in our analysis, which may differ when comparing OPCAB with CABG patients. Deviations from optimal intraoperative blood pressure could also be linked to delirium.38 Nurses in the ICU recorded delirium using the CAM-ICU method. Although use of the CAM-ICU by nurses was previously validated,39 the consistency by which delirium was measured may not have been similar across all patients. Also, delirium is a waxing and waning condition, and delirious episodes could have been missed in some patients at the times delirium was measured. Sedation protocols were not standardized for the patients included in the study, and the amount of opiates, benzodiazepines, and other sedatives varied in the study population; consequently, these data were not available for inclusion as covariates in the study.
Conclusions
In this large historical study of prospectively collected data, we found an association between CPB use and postoperative delirium in cardiac surgery patients. Given these findings, medical centres should consider avoiding the use of CPB when appropriate. Future studies that randomize patients to either an on-pump or an off-pump group for CABG may further elucidate associations between CPB use and adverse outcomes following cardiac surgery.
References
Rudolph JL, Jones RN, Levkoff SE, et al. Derivation and validation of a preoperative prediction rule for delirium after cardiac surgery. Circulation 2009; 119: 229-36.
Saczynski JS, Marcantonio ER, Quach L, et al. Cognitive trajectories after postoperative delirium. N Engl J Med 2012; 367: 30-9.
Inouye SK. Delirium in older persons. N Engl J Med 2006; 354: 1157-65.
Chaput AJ, Bryson GL. Postoperative delirium: risk factors and management: continuing professional development. Can J Anesth 2012; 59: 304-20.
Mariscalco G, Cottini M, Zanobini M, et al. Preoperative statin therapy is not associated with a decrease in the incidence of delirium after cardiac operations. Ann Thorac Surg 2012; 93: 1439-47.
Rudolph JL, Ramlawi B, Kuchel GA, et al. Chemokines are associated with delirium after cardiac surgery. J Gerontol Series A Biol Sci Med Sci 2008; 63: 184-9.
Ramlawi B, Rudolph JL, Mieno S, et al. Serologic markers of brain injury and cognitive function after cardiopulmonary bypass. Ann Surg 2006; 244: 593-601.
Khan BA, Zawahiri M, Campbell NL, Boustani MA. Biomarkers for delirium–a review. J Am Geriatr Soc 2011; 59(Suppl 2): S256-61.
Yuan SM. S100 and S100beta: biomarkers of cerebral damage in cardiac surgery with or without the use of cardiopulmonary bypass. Rev Bras Cir Cardiovasc 2914; 29: 630-41.
Zheng L, Fan QM, Wei ZY. Serum S-100beta and NSE levels after off-pump versus on-pump coronary artery bypass graft surgery. BMC Cardiovasc Disord 2015; 15: 70.
Bonacchi M, Prifti E, Maiani M, Bartolozzi F, Di Eusanio M, Leacche M. Does off-pump coronary revascularization reduce the release of the cerebral markers, S-100beta and NSE? Heart Lung Circ 2006; 15: 314-9.
Bucerius J, Gummert JF, Borger MA, et al. Predictors of delirium after cardiac surgery delirium: effect of beating-heart (off-pump) surgery. J Thorac Cardiovasc Surg 2004; 127: 57-64.
Rudolph JL, Marcantonio ER, Culley DJ, et al. Delirium is associated with early postoperative cognitive dysfunction. Anaesthesia 2008; 63: 941-7.
Liang CK, Chu CL, Chou MY, et al. Interrelationship of postoperative delirium and cognitive impairment and their impact on the functional status in older patients undergoing orthopaedic surgery: a prospective cohort study. PLoS One 2014; 9: e110339.
Baba T, Goto T, Maekawa K, Ito A, Yoshitake A, Koshiji T. Early neuropsychological dysfunction in elderly high-risk patients after on-pump and off-pump coronary bypass surgery. J Anesth 2007; 21: 452-8.
Marasco SF, Sharwood LN, Abramson MJ. No improvement in neurocognitive outcomes after off-pump versus on-pump coronary revascularisation: a meta-analysis. Eur J Cardiothorac Surg 2008; 33: 961-70.
Fink HA, Hemmy LS, MacDonald R, et al. Intermediate- and long-term cognitive outcomes after cardiovascular procedures in older adults: a systematic review. Ann Intern Med 2015; 163: 107-17.
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 2009; 42: 377-81.
von Elm E, Altman DG, Egger M, et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol 2008; 61: 344-9.
Khwaja A. KDIGO clinical practice guidelines for acute kidney injury. Nephron Clin Pract 2012; 120: c179-84.
Zhang J, Yu KF. What’s the relative risk? A method of correcting the odds ratio in cohort studies of common outcomes. JAMA 1998; 280: 1690-1.
Harrell FE Jr. Regression Modeling Strategies - With Applications to Linear Models, Logistic Regression, and Survival Analysis. New York: Springer-Verlag New York Inc.; 2010.
Tse L, Schwarz SK, Bowering JB, Moore RL, Barr AM. Incidence of and risk factors for delirium after cardiac surgery at a quaternary care center: a retrospective cohort study. J Cardiothorac Vasc Anesth 2015; 29: 1472-9.
Andrejaitiene J, Benetis R, Sirvinskas E. Postoperative delirium following cardiac surgery: the incidence, risk factors and outcome. J Cardiothorac Surg 2015; 10(Suppl 1): A298.
Hudetz JA, Iqbal Z, Gandhi SD, Patterson KM, Byrne AJ, Pagel PS. Postoperative delirium and short-term cognitive dysfunction occur more frequently in patients undergoing valve surgery with or without coronary artery bypass graft surgery compared with coronary artery bypass graft surgery alone: results of a pilot study. J Cardiothorac Vasc Anesth 2011; 25: 811-6.
Lagny MG, Jouret F, Koch JN, et al. Incidence and outcomes of acute kidney injury after cardiac surgery using either criteria of the RIFLE classification. BMC Nephrol 2015; 16: 76.
Nigwekar SU, Kandula P, Hix JK, Thakar CV. Off-pump coronary artery bypass surgery and acute kidney injury: a meta-analysis of randomized and observational studies. Am J Kidney Dis 2009; 54: 413-23.
Seabra VF, Alobaidi S, Balk EM, Poon AH, Jaber BL. Off-pump coronary artery bypass surgery and acute kidney injury: a meta-analysis of randomized controlled trials. Clin J Am Soc Nephrol 2010; 5: 1734-44.
Cheungpasitporn W, Thongprayoon C, Kittanamongkolchai W, et al. Comparison of renal outcomes in off-pump versus on-pump coronary artery bypass grafting: a systematic review and meta-analysis of randomized controlled trials. Nephrology (Carlton) 2015. DOI:10.1111/nep.12506.
Hogue CW Jr, Hyder ML. Atrial fibrillation after cardiac operation: risks, mechanisms, and treatment. Ann Thorac Surg 2000; 69: 300-6.
Narducci ML, Pelargonio G, Rio T, et al. Predictors of postoperative atrial fibrillation in patients with coronary artery disease undergoing cardiopulmonary bypass: a possible role for myocardial ischemia and atrial inflammation. J Cardiothorac Vasc Anesth 2014; 28: 512-9.
Mathew JP, Parks R, Savino JS, et al. Atrial fibrillation following coronary artery bypass graft surgery: predictors, outcomes, and resource utilization. MultiCenter Study of Perioperative Ischemia Research Group. JAMA 1996; 276: 300-6.
Lamm G, Auer J, Weber T, Berent R, Ng C, Eber B. Postoperative white blood cell count predicts atrial fibrillation after cardiac surgery. J Cardiothorac Vasc Anesth 2006; 20: 51-6.
Davoodi S, Karimi A, Ahmadi SH, et al. Early outcome of off-pump versus on-pump coronary revascularization. Pan Afr Med J 2014; 17: 309.
Sa MP, Ferraz PE, Escobar RR, et al. Off-pump versus on-pump coronary artery bypass surgery: meta-analysis and meta-regression of 13,524 patients from randomized trials. Rev Bras Cir Cardiovasc 2012; 27: 631-41.
Moller CH, Penninga L, Wetterslev J, Steinbruchel DA, Gluud C. Off-pump versus on-pump coronary artery bypass grafting for ischaemic heart disease. Cochrane Database Syst Rev 2012; 3: CD007224.
Bin Abd Razak HR, Yung WY. Postoperative delirium in patients undergoing total joint arthroplasty: a systematic review. J Arthroplasty 2015; 30: 1414-7.
Hori D, Max L, Laflam A, et al. Blood pressure deviations from optimal mean arterial pressure during cardiac surgery measured with a novel monitor of cerebral blood flow and risk for perioperative delirium: a pilot study. J Cardiothorac Vasc Anesth 2016; 30: 606-12.
Ely EW, Margolin R, Francis J, et al. Evaluation of delirium in critically ill patients: validation of the Confusion Assessment Method for the Intensive Care Unit (CAM-ICU). Crit Care Med 2001; 29: 1370-9.
Acknowledgement
The authors thank Leslie Busbee (Department of Cardiac Surgery, Vanderbilt University Medical Center) for assistance with data retrieval.
Conflicts of interest
None declared.
Editorial responsibility
This submission was handled by Dr. Hilary P. Grocott, Editor-in-Chief, Canadian Journal of Anesthesia.
Author contributions
Jason B. O’Neal, Frederic T. Billings, and Andrew D. Shaw contributed substantially to all aspects of this manuscript, including conception and design; acquisition, analysis, and interpretation of data; and drafting the article. Ashish S. Shah and Xulei Liu contributed substantially to the conception and design of the manuscript. Jesse M. Ehrenfeld and Jonathan P. Wanderer contributed substantially to the acquisition of data. Xulei Liu and Matthew S. Shotwell contributed to the analysis of data. Ashish S. Shah, Yafen Liang, Jesse M. Ehrenfeld, Jonathan P. Wanderer, Xulei Liu, and Matthew S. Shotwell contributed substantially to the interpretation of data.
Funding
This work was supported by the National Institutes of Health under award numbers T32GM108554 (J.B.O.), K23GM102676 (F.T.B.), and R01GM112871 (F.T.B.). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. Research reported in this publication was also supported by Vanderbilt Institute for Clinical and Translational Research grant support (UL1 TR000445 from NCATS/NIH).
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
O’Neal, J.B., Billings, F.T., Liu, X. et al. Risk factors for delirium after cardiac surgery: a historical cohort study outlining the influence of cardiopulmonary bypass. Can J Anesth/J Can Anesth 64, 1129–1137 (2017). https://doi.org/10.1007/s12630-017-0938-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12630-017-0938-5