Abstract
Objectives
There are few data regarding the accuracy of short frailty tools as predictors of mortality and other clinical outcomes of older patients admitted to a geriatric ward. We therefore analyzed the accuracy of Rockwood et al’s Clinical Frailty Scale and an easy and quick to perform operationalization of Fried et al’s frailty phenotype, as predictors of mortality and other clinical outcomes in our cohort of patients.
Design
Prospective analysis with a follow-up period of 6 months.
Setting and Participants
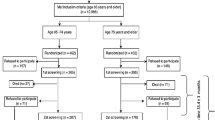
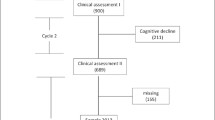
307 patients who were 65 years of age or older were included in the study. The patients were assessed in terms of the two frailty measures during their stay in a geriatric ward.
Results
The Clinical Frailty Scale and the frailty phenotype were both suitable for differentiating between patients who died due to any cause from those who survived during followup (primary outcome) (area under the ROC curves (AUC) values 0.867 (95% CI 0.807–0.926), p<0.001 and 0.754 (95% CI 0.688–0.821), p<0.001, respectively). Regarding the secondary outcomes: 1. unplanned admission to hospital and 2. a fall during follow-up, the Clinical Frailty Scale discriminated or tended to discriminate between patients to whom these criteria applied and those to whom they did not (AUC=0.569 (95% CI 0.502–0.636), p=0.046 and AUC=0.574 (95% CI 0.501–0.647), p=0.071, respectively). The frailty phenotype did not show such a differentiation when applied to secondary outcomes (AUC=0.500 (95% CI 0.432–0.568), p=0.994 and AUC=0.518 (95% CI 0.439–0.598), p=0.658, respectively).
Conclusion
Both short frailty instruments are suitable predictors of mortality in older patients who were admitted to a geriatric ward. The Clinical Frailty Scale, but not the frailty phenotype, predicted at least some of the secondary outcomes, i.e., the outcome unplanned admission to hospital during follow-up.
Similar content being viewed by others
References
Vellas B, Cestac P, Morley JE. Implementing frailty into clinical practice: we cannot wait. J Nutr Health Aging. 2012;16(7):599–600.
McMillan GJ, Hubbard RE. Frailty in older inpatients: what physicians need to know. Q J Med. 2012;105:1059–65.
Clegg A, Young J, Iliffe S, Rikkert MO, Rockwood K. Frailty in elderly people. Lancet. 2013;381(9868):752–62.
Rockwood K, Bergman H. Frailty: a report from the 3(rd) joint workshop fo the IAGG/WHO/SFGG, Athens, january 2012. Can Geriatr J. 2012;15(2):31–6.
O’Connell MDL, Tajar A, O’Neill TW, et al. Frailty is associated with impaired quality of life and falls in middle-aged and older european men. J Frailty Aging. 2013;2(2):77–83.
Abizanda P, Romero L, Sanchez-Jurado PM, Martinez-Reig M, Alfonso-Silguero SA, Rodriguez-Manas L. Age, frailty, disability, institutionalization, multimorbidity or comorbidity. Which are the main targets in older adults? J Nutr Health Aging. 2014;18(6):622–7.
Lombard K, van Steijn J, Schuur T, et al. Compliance of energy-dense, small volume oral nutritional supplements in the daily clinical paractice on a geriatric ward-an observational study. J Nutr Health Aging. 2014;18(7):649–53.
Cesari M, Landi F, Vellas B, Bernabei R, Marzetti E. Sarcopenia and physical frailty: two sides of the same coin. Front Aging Neurosci. 2014;6:192.
Morley JE, Vellas B, van Kan GA, et al. Frailty consensus: A call to action. J Am Med Dir Assoc. 2013;14(6):392–7.
Mitnitski A, Mogilner AJ, Rockwood K. Accumulation of deficits as a proxy measure of ageing. ScientificWorldJournal. 2001;1:323–36.
Jones D, Song X, Mitnitski A, Rockwood K. Evaluation of a frailty index based on a comprehensive geriatric assessment in a population based study of elderly Canadians. Aging Clin Exp Res. 2005;17:465–71.
Rockwood K, Song X, Mac Knight C, et al. A global clinical measure of fitness and frailty in elderly people. CMAJ. 2005;5(173):489–95.
Rockwood K, Rockwood MRH, Mitnitski A. Physiological redundancy in older adults in relation to the change with age in the slope of a frailty index. J Am Geriatr Soc. 2010;58:318–23.
Fried LP, Tangen CM, Walston J, et al. Frailty in older adults: Evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56A:M146–M56.
Ensrud KE, Ewing SK, Taylor BC, et al. Comparison of 2 frailty indexes for prediction of falls, disability, fractures, and death in older women. Arch Intern Med. 2008;168(4):382–9.
Ensrud KE, Ewing SK, Cawthon PM, et al. A comparison of frailty indexes for prediction of falls, disability, fractures and mortality in older men. J Am Geriatr Soc. 2009;57(3):492–8.
Moorhouse P, Rockwood K. Frailty and its quantitative clinical evaluation. J R Coll Physicians Edinb. 2012;42:333–40.
http://geriatricresearch.medicine.dal.ca/clinical_frailty_scale.html. Accessed 13 November 2014
Rockwood K, Andrew M, Mitnitski A. A comparison of two apporaches to measuring frailty in elderly people. J Gerontol A Biol Sci Med Sci. 2007;62A:738–43.
Joosten E, Demuynck M, Detroyer E, Milisen K. Prevalence of frailty and its ability to predict in hospital delirium, falls, and 6-month mortality in hospitalized older patients. BMC Geriatrics. 2014;14:1.
Pilotto A, Rengo F, Marchionni N, et al. Comparing the prognostic accuracy for allcause mortality of frailty instruments: a multicentre 1-year follow-up in hospitalized older patients. PLoS ONE. 2011;7(1):e29090.
Khandelwal D, Goel A, Kumar U, Gulatj V, Narang R, Dey AB. Frailty is associated with longer hospital stay and increased mortality in hospitalized older patients. J Nutr Health Aging. 2012;16(8):732–5.
Le Maguet P, Roquilly A, Lasocki S, et al. Prevalence and impact of frailty on mortality in elderly ICU patients: a prospective, multicenter, observational study. Intensive Care Med. 2014;40(5):674–82.
Ekerstad N, Swahn E, Janzon M, et al. Frailty is independently assoicated with short-term outcomes for elderly patients with non-ST-segment elevation myocardial infarction. Circulation. 2011;124:2397–404.
Chen C, Sia I, Ma H-M, et al. The synergistic effect of functinoal status and comorbidity burden on mortality: a 16-year survivial analysis. PLoS ONE. 2014;9(8):e106248.
Gnjidic D, Hilmer SN, Blyth FM, et al. Polypharmacy cutoff and outcomes: five or more medications were used to identify community-dwelling older men at risk of different adverse outcomes. J Clin Epidemiol. 2012;65(9):989–95.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ritt, M., Schwarz, C., Kronawitter, V. et al. Analysis of Rockwood et al’s Clinical Frailty Scale and Fried et al’s frailty phenotype as predictors of mortality and other clinical outcomes in older patients who were admitted to a geriatric ward. J Nutr Health Aging 19, 1043–1048 (2015). https://doi.org/10.1007/s12603-015-0667-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-015-0667-9