Abstract
Objectives
Administration of oral nutritional supplements (ONS) is an effective strategy to treat and avoid malnutrition, a persisting issue in nursing homes. However, little is known about compliance in the NH population. This study aimed to analyse the effects of compliance of NH residents with a low-volume, nutrientand energy-dense ONS on nutritional status and to identify residents’ characteristics associated with compliance.
Design & Setting
Randomized, controlled trial in nursing homes.
Participants & Intervention
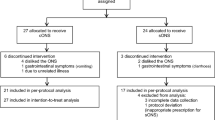
87 nursing home residents (87±6y, 91% female) with malnutrition or at risk of malnutrition were randomly allocated to an intervention group (IG) receiving 2×125 ml ONS (2.4 kcal/ml)/d for 12 weeks, or the control group (CG) with usual care.
Measurements
ONS intake was recorded daily and compliance calculated. Low and high compliance were defined as ≤30% and ≥80% of provided ONS actually consumed, respectively. Body weight (BW), BMI, upper-arm (UAC) and calf-circumference (CC) and MNA-SF were assessed at baseline and after 12 weeks. Associations between compliance and changes of nutritional parameters and residents’ characteristics were analysed.
Results
Compliance was high in 35.7% and low in 28.6% of the IG (n=42). BW change was significantly higher in subjects with high compliance (median +3.0 (interquartile range +2.1;+3.8) kg, n=15) than in those with low compliance (−0.2 (−2.2;+1.6) kg, n=12) and CG (−0.1 (−1.2; +0.6) kg, n=35; p<0.001), and significantly correlated with compliance in IG (r=0.691; p<0.001). Significant differences and correlations were also identified for BMI, UAC and MNA-SF. High compliance was more often observed in residents with malnutrition (66.7 vs. 27.3%) and chewing difficulties (77.8 vs. 24.2%) than in those without these conditions. Low compliance was more prevalent in residents who were immobile (45.0 vs. 13.6%), depressed (33.3 vs. 6.7%) or had gastrointestinal complaints (50.0 vs. 17.9%) (all p<0.05).
Conclusions
A high compliance of nursing home residents with a low volume, nutrient- and energy dense ONS was related to a significantly improved nutritional status in comparison to low compliance and therefore enhanced the effectiveness of ONS. A higher compliance may be achieved by consideration of different residents’ characteristics.
Similar content being viewed by others
References
Milne AC, Potter J, Vivanti A, Avenell A: Protein and energy supplementation in elderly people at risk from malnutrition. Cochrane Database Syst Rev 2009(2):CD003288.
Volkert D, Berner YN, Berry E, Cederholm T, Coti BP, Milne A, Palmblad J, Schneider S, Sobotka L, Stanga Z et al: ESPEN Guidelines on Enteral Nutrition: Geriatrics. Clin Nutr 2006, 25(2):330–360.
Donini LM, Scardella P, Piombo L, Neri B, Asprino R, Proietti AR, Carcaterra S, Cava E, Cataldi S, Cucinotta D et al: Malnutrition in elderly: social and economic determinants. J Nutr Health Aging 2013, 17(1):9–15.
Kaiser MJ, Bauer JM, Ramsch C, Uter W, Guigoz Y, Cederholm T, Thomas DR, Anthony PS, Charlton KE, Maggio M et al: Frequency of malnutrition in older adults: a multinational perspective using the mini nutritional assessment. J Am Geriatr Soc 2010, 58(9):1734–1738.
Stange I, Poeschl K, Stehle P, Sieber CC, Volkert D: Screening for malnutrition in nursing home residents: comparison of different risk markers and their association to functional impairment. J Nutr Health Aging 2013, 17(4):357–363.
Thomas DR, Ashmen W, Morley JE, Evans WJ: Nutritional management in longterm care: development of a clinical guideline. Council for Nutritional Strategies in Long-Term Care. J Gerontol A Biol Sci Med Sci 2000, 55(12):M725–734.
Schrader E, Baumgartel C, Gueldenzoph H, Stehle P, Uter W, Sieber CC, Volkert D: Nutritional Status According to Mini Nutritional Assessment is Related to Functional Status in Geriatric Patients — Independent of Health Status. J Nutr Health Aging 2014, 18(3):257–263.
Kiesswetter E, Pohlhausen S, Uhlig K, Diekmann R, Lesser S, Heseker H, Stehle P, Sieber CC, Volkert D: Malnutrition is related to functional impairment in older adults receiving home care. J Nutr Health Aging 2013, 17(4):345–350.
Arvanitakis M, Coppens P, Doughan L, van Gossum A: Nutrition in care homes and home care: recommendations — a summary based on the report approved by the Council of Europe. Clin Nutr 2009, 28(5):492–496.
Allen V, Methven L, Gosney M: The influence of nutritional supplement drinks on providing adequate calorie and protein intake in older adults with dementia. J Nutr Health Aging 2013, 17(9):752–755.
Bonnefoy M, Cornu C, Normand S, Boutitie F, Bugnard F, Rahmani A, Lacour JR, Laville M: The effects of exercise and protein-energy supplements on body composition and muscle function in frail elderly individuals: a long-term controlled randomised study. Br J Nutr 2003, 89(5):731–739.
Fiatarone MA, O’Neill EF, Ryan ND, Clements KM, Solares GR, et al.: Exercise training and nutritional supplementation for physical frailty in very elderly people. N Engl J Med 1994, 330:1769–1775.
Freeman R, Ralph AF, Cawood AL, Stratton RJ: A survey of compliance and use of ready-made liquid oral nutritional supplements in elderly malnourished care home residents. Aging Clin Exp Res 2011, 23:159.
Kayser-Jones J, Schell ES, Porter C, Barbaccia JC, Steinbach C, Bird WF, Redford M, Pengilly K: A prospective study of the use of liquid oral dietary supplements in nursing homes. J Am Geriatr Soc 1998, 46:1378–1386.
Manders M, De Groot LC, Hoefnagels WH, Dhonukshe-Rutten RA, Wouters- Wesseling W, Mulders AJ, Van Staveren WA, de Groot CP, Blauw YH, van Hoeckel-Prust L et al: The effect of a nutrient dense drink on mental and physical function in institutionalized elderly people. J Nutr Health Aging 2009, 13(9):760–767.
Turic A, Gordon KL, Craig LD, Ataya DG, Voss AC: Nutrition supplementation enables elderly residents of long-term-care facilities to meet or exceed RDAs without displacing energy or nutrient intakes from meals. J Am Diet Assoc 1998, 98:1457–1459.
Wouters-Wesseling W, Wouters AE, Kleijer CN, Bindels JG, de Groot CP, van Staveren WA: Study of the effect of a liquid nutrition supplement on the nutritional status of psycho-geriatric nursing home patients. Eur J Clin Nutr 2002, 56(3):245–251.
Hubbard GP, Elia M, Holdoway A, Stratton RJ: A systematic review of compliance to oral nutritional supplements. Clin Nutr 2012, 31(3):293–312.
Nieuwenhuizen WF, Weenen H, Rigby P, Hetherington MM: Older adults and patients in need of nutritional support: review of current treatment options and factors influencing nutritional intake. Clin Nutr 2010, 29(2):160–169.
Lad H, Gott M, Gariballa S: Elderly patients compliance and elderly patients and health professional's, views, and attitudes towards prescribed sip- feed supplements. J Nutr Health Aging 2005, 9(5):310–314.
Barton AD, Beigg CL, Macdonald IA, Allison SP: A recipe for improving food intakes in elderly hospitalized patients. Clin Nutr 2000, 19(6):451–454.
Hubbard GP, Holdoway A, Stratton RJ: A pilot study investigating compliance and efficacy of a novel, low volume, energy dense (2.4kcal/ml) multi-nutrient supplement in malnourished community patients Clinical Nutrition Supplements 2009, 4:41.
Cowan DT, Roberts JD, Fitzpatrick JM, While AE, Baldwin J: Nutritional status of older people in long term care settings: current status and future directions. Int J Nurs Stud 2004, 41(3):225–237.
Beck AM, Damkjaer K, Tetens I: Lack of compliance of staff in an intervention study with focus on nutrition, exercise and oral care among old (65+ yrs) Danish nursing home residents. Aging Clin Exp Res 2009, 21(2):143–149.
Bruce D, Laurance I, McGuiness M, Ridley M, Goldswain P: Nutritional supplements after hip fracture: poor compliance limits effectiveness. Clin Nutr 2003, 22(5):497–500.
Stange I, Bartram M, Liao Y, Poeschl K, Kolpatzik S, Uter W, Sieber CC, Stehle P, Volkert D: Effects of a low volume, nutrient- and energy-dense oral nutritional supplement on nutritional and functional status: a randomized, controlled trial in nursing home residents. J Am Med Dir Assoc 2013, 14:628.e621–e628.
Mahoney FI, Barthel DW: Functional evaluation: The Barthel index. Maryland State MedJ 1965, 14(2):61–65.
Folstein MF, Folstein SE, McHugh PR: “Mini Mental State”: A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 1975, 12:189–198.
Yesavage JA, Brink TL, Rose TL, Lum O, Huang V, Adey M, Leirer VO: Development and validation of a geriatric depression screening scale: a preliminary report. J Psychiatr Res 1982, 17(1):37–49.
Simmons SF, Patel AV: Nursing home staff delivery of oral liquid nutritional supplements to residents at risk for unintentional weight loss. J Am Geriatr Soc 2006, 54(9):1372–1376.
Taylor JS, DeMers SM, Vig EK, Borson S: The disappearing subject: exclusion of people with cognitive impairment and dementia from geriatrics research. J Am Geriatr Soc 2012, 60(3):413–419.
Smoliner C, Norman K, Wagner KH, Hartig W, Lochs H, Pirlich M: Malnutrition and depression in the institutionalised elderly. Br J Nutr 2009, 102(11):1663–1667.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jobse, I., Liao, Y., Bartram, M. et al. Compliance of nursing home residents with a nutrient- and energy-dense oral nutritional supplement determines effects on nutritional status. J Nutr Health Aging 19, 356–364 (2015). https://doi.org/10.1007/s12603-014-0544-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-014-0544-y