Abstract
Objectives
The aim of this study was to determine the prevalence and related predictors of dizziness in a sample of community-dwelling people 65 years of age and older living in a metropolitan area in Germany.
Design
Prospective cohort study.
Setting
Interdisciplinary Centre of Gerontology at the University of Erlangen-Nuremberg, Germany.
Participants
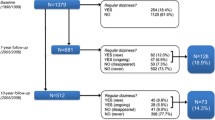
6000 people aged 65 years and older recruited and randomized from the registration office, 1801 were fully evaluated at baseline and were re-evaluated in a prospective follow-up two years later. A full data set was obtained for 620 participants, of which 297 (47.9%) were females. Mean age was 73.45 ± 6.05. 200 participants (32.4%) were 65–69 years, 315 (51%) were 70–79 years, 92 (14.9%) 80–89 years and 11 (1.8%) 90 years and older.
Measurements
Demographic, medical, functional and psychological factors were measured by a standardised questionnaire in 2004. In a follow-up survey participants were reevaluated in a prospective design two years later (2006), including a dizziness questionnaire, containing frequency, duration, space of dizziness and releasing positions and activities.
Results
At the second measurement 181 persons (29.2%) reported dizziness in the last 6 months. Dizziness was age dependent, with a prevalence of 27% in participants aged 70 years and younger, up to 54% in the group of 90 years and older. 96 (68.2%) persons reported daily or weekly dizziness. 46 (27.9%) participants reported multiple sensations of dizziness. In 108 (59.7) persons dizziness was released by multiple positions or activities. The main predictors of dizziness were age, female gender, cardiovascular disease, osteoporosis, depression, sleep disorder, disturbance of memory, shortsightedness (defined by glasses), incontinence, 3 and more medical conditions, 4 and more medications, poor health status, falls and mobility problems. We found similar risk factors for dizziness and falls.
Conclusion
Dizziness is a very common symptom in older community dwelling persons. Comorbidity, poor health status and mobility problems are strong medical predictors; age and female gender and decline in mobility are important predictors as well. Our study suggests, that dizziness in older age is often caused by multifactorial medical and functional conditions. Gait disorders and mobility problems also seem to play an important role in dizziness among older people. Therefore, interventions in dizziness should be developed in a multifactorial way. We suggest, that the interventions to be tested first, should be those that have been previously successful in older persons with gait disorders and falls.
Similar content being viewed by others
References
Boult C, Murphy J, Sloane P, Mor V, Drone C. The relation of dizziness to functional decline. J Am Geriatr Soc 1991; 39:858–861.
Colledge NR, Wilson JA, MacIntyre CC, MacLennan WJ. The prevalence and characteristics of dizziness in an elderly community. Age Ageing 1994; 23:17–20.
Ensrud KE, Nevitt MC, Yunis C, Hulley SB, Grimm RH, Cummings SR. Postural hypotension and postural dizziness in elderly women. Arch Intern Med 1992;152:1058–1064.
Sloane P, Blazer D, George LK. Dizziness in a community elderly population. J Am Geriatr Soc 1989; 37:101–108.
Tilvis RJ, Hakula SM, Valvanne J, Erkinjuntti T. Postural hypotension and dizziness in a gen-eral aged population: a four-year follow-up of the Helsinki Aging Study. J Am Geriatr Soc 1996; 44:809–814.
Ensrud KE, Nevitt MC, Yunis C, Cauley JA, Seeley DG, Fox KM, et al. Correlates of impaired function in older women. J Am Geriatr Soc 1994;42:481–489.
Grimby A, Rosenhall U. Health-related quality of life and dizziness in old age. Gerontology 1995; 41:286–298.
Grimley EJ. Transient neurological dysfunction and risk of stroke in an elderly English population: the different significance of vertigo and nonrotatory dizziness. Age Ageing 1990; 19:43–49.
Sixt E, Landahl S. Postural disturbances in a 75-year old population: I. Prevalence and functional consequences. Age Ageing 1987; 16:393–398.
Kroenke K, Lucas CA, Rosenberg ML, Scherokman B, Herbers JE, Wehrle PA, et al. Causes of persistent dizziness. A prospective study of 100 patients in ambulatory care. Ann Intern Med 1992; 117:898–904.
Davis LE. Dizziness in elderly men. J Am Geriatr Soc 1994; 42:1184–1188.
Katsarkas A. Dizziness in aging: a retrospective study of 1194 cases. Otolaryngol Head Neck Surg 1994; 110:296–301.
Lawson J, Fitzgerald J, Birchall J, Aldren CP, Kenny RA. Diagnosis of geriatric patients with severe dizziness. J Am Geriatr Soc 1999;47:12–17.
McIntosh S, DaCosta D, Kenny RA. Outcome of an integrated approach to the investigation of dizziness, falls and syncope in elderly patients referred to a “syncope” clinic. Age Ageing 1993;22:53–58
Colledge NR, Barr-Hamilton RM, Lewis SJ, Sellar RJ, Wilson JA. Evaluation of investigations to diagnose the cause of dizziness in elderly people: a community based controlled study. BMJ 1996; 313: 788–792.
Sloane PD, Hartman M, Mitchell CM. Psychological factors associated with chronic dizziness in patients aged 60 and older. J Am Geriatr Soc 1994; 42:847–852.
Goring H, Baldwin R, Marriott A, Pratt H, Roberts C (2004) Validation of short screening tests for depression and cognitive impairment in older medically ill inpatients. Int J Geriatr Psychiatry 19: 465–471.
Drachman DA. Dizziness. In: Feldmann E, ed. Current Diagnosis in Neurology. St. Louis: Mosby-Year Book; 1994:264–270.
Drachman DA. A 69-year-old man with chronic dizziness. JAMA 1998; 280:2111–2118.
Tinetti ME, Williams C, Gill T. Dizziness among older adults: a possible geriatric syndrome. Ann Intern Med 2000; 132:337–344.
Frishman WH, Azer V, Sica D. Drug treatment of orthostatic hypotension and vasovagal syncope. Heart Dis 2003; 5(1):49–64.
Drachman DA, Hart CW. An approach to the dizzy patient. Neurology 1972; 22:323–334.
Gassmann KG, Rupprecht R, Freiberger E. Predictors for occasional and recurrent falls in older community dwelling people. Submitted to Z Gerontol Geriatr.
Montero-Odasso M, Schapira M, Duque G, Soriano ER, Kaplan R, Camera LA. Gait disorders are associated with non-cardiovascular falls in elderly people: a preliminary study. BMC Geriatr 2005; 5:15.
Stalenhoef PA, Diederiks JP, Knottnerus JA, Kester AD, Crebolder HF. A risk model for the prediction of recurrent falls in community-dwelling elderly: a prospective cohort study. J Clin Epidemiol 2002; 55:1088–1094.
Author information
Authors and Affiliations
Additional information
FOR THE IZG STUDY GROUP
Members of the IZG Study Group: Participating centres and investigators (alphabetical by centre): Carl-Korth-Institute, Erlangen: Lang, E.; Chair for Health Management, FAU Erlangen-Nuremberg: Schöffski, O.; Chair of Internal Medicine V and Institute of Biomedicine of Aging, FAU Erlangen-Nuremberg: Mühlberg, W., Sieber, C.; Clinic for Geriatric Medicine, Waldkrankenhaus St. Marien, Erlangen: Gaßmann, K.-G.; Clinic for Neurology, FAU Erlangen-Nuremberg: Kolominsky-Rabas, P.; Clinic for Psychiatry and Psychotherapy, FAU Erlangen-Nuremberg: Gräßel, E., Kornhuber, J.; Department of Management, FAU Erlangen-Nuremberg: Esslinger, A.S.; Institute of History and Ethics in Medicine, FAU Erlangen-Nuremberg: Wittern-Sterzel, R.; Institute of Psychogerontology, FAU Erlan-gen-Nuremberg: Ackermann, A., Engel, S., Kaiser, H.-J., Lang, F.R., Oswald, W.D., Rupprecht, R., Schüssel, K.; Institute of Sport Sciences, FAU Erlangen-Nuremberg: Freiberger, E., Pfeifer, K., Rütten, A; Members without affiliation: Schneider, H., Stosberg, M.
Rights and permissions
About this article
Cite this article
Gassmann, K.G., Rupprecht, R. Dizziness in an older community dwelling population: A multifactorial syndrome. J Nutr Health Aging 13, 278–282 (2009). https://doi.org/10.1007/s12603-009-0073-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-009-0073-2