Abstract
Introduction
Given the relatively short life expectancy of patients with hepatocellular carcinoma (HCC), quality of life (QOL) plays a significant role in treatment selection. This analysis aimed to compare time to deterioration (TTD) in QOL with transarterial radioembolization (TARE) and atezolizumab–bevacizumab, as well as sorafenib, in advanced and unresectable HCC.
Methods
Patient-level data from SARAH (TARE using SIR-Spheres® Y-90 resin microspheres [SIR-Spheres] versus sorafenib) and aggregate data from IMbrave150 (atezolizumab–bevacizumab versus sorafenib) randomized controlled trials were used to conduct an anchored matching-adjusted indirect comparison (MAIC). Patients with a Child–Pugh score B in SARAH were excluded to align with exclusion criteria in IMbrave150. To identify potential effect modifiers for adjustment, the literature was searched and multivariate Cox proportional hazards models were implemented using SARAH data. Patients from SARAH were then weighted to balance with baseline characteristics from IMbrave150. Median TTD in QOL and hazard ratios (HRs) were calculated.
Results
Four potential effect modifiers were identified and used for adjustment: cause of disease (viral/non-viral), macrovascular invasion, Eastern Cooperative Oncology Group performance score, and alpha-fetoprotein level. The MAIC included 217 patients from SARAH (TARE = 94; sorafenib = 123). Median TTD in QOL was 11.23 and 8.64 months for atezolizumab–bevacizumab and TARE, respectively (HR = 1.06; 95% confidence interval [CI] 0.75–1.50; p = 0.725). A sensitivity analysis was conducted adjusting for cause of disease defined as hepatitis B/hepatitis C/non-viral: median TTD in QOL was higher for TARE compared with atezolizumab–bevacizumab (19.88 vs 11.23 months; HR = 0.66; 95% CI 0.36–1.19; p = 0.163). Sorafenib resulted in the shortest TTD in QOL, with statistically significant differences in both base case and sensitivity analyses.
Conclusion
TARE using SIR-Spheres may achieve similar TTD in QOL compared with atezolizumab–bevacizumab, as the analyses found no statistically significant differences between these two interventions. Both TARE using SIR-Spheres and atezolizumab–bevacizumab seem to be more efficacious than sorafenib in maintaining QOL.
Plain Language Summary
For patients with hepatocellular carcinoma, as well as physicians treating hepatocellular carcinoma, the quality of life that different treatments can offer represents an increasingly important aspect to consider when choosing treatments. Transarterial radioembolization and atezolizumab–bevacizumab are two potential treatments for advanced and unresectable hepatocellular carcinoma, but no clinical trials have directly compared the outcomes of these two therapeutic options. With the data available (patient-level data from a clinical trial of transarterial radioembolization using SIR-Spheres® Y-90 resin microspheres [SIR-Spheres] versus sorafenib and data from a trial of atezolizumab–bevacizumab versus sorafenib from the literature), this study indirectly compared the time to deterioration of quality of life (i.e., how long quality of life is maintained) after treatment with transarterial radioembolization and atezolizumab–bevacizumab. The study showed that quality of life may be preserved over a similar time period with transarterial radioembolization using SIR-Spheres and atezolizumab–bevacizumab; also, both transarterial radioembolization using SIR-Spheres and atezolizumab–bevacizumab seem to maintain patients’ quality of life over a longer period of time compared with sorafenib. These results are expected to enrich the existing evidence on which patients and physicians can base their decisions, allowing them to choose the most appropriate treatment by assessing the treatments’ characteristics as a whole.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Why carry out this study? |
When life expectancy is short, quality of life (QOL) is crucial for treatment selection. Hepatocellular carcinoma (HCC) patients have a short life expectancy, hence the importance of a holistic approach to treatment selection. |
The SARAH and IMbrave150 trials investigated transarterial radioembolization (TARE) and atezolizumab–bevacizumab, versus sorafenib, in HCC, but no clinical trials have directly compared these two treatments. This study aimed to understand the relative QOL outcomes of these treatments. |
What was learned from the study? |
This study indirectly compared the time to deterioration in QOL after treatment with TARE and atezolizumab–bevacizumab, and the results indicated that QOL may be maintained over a similar time period with TARE and atezolizumab–bevacizumab. Also, both TARE and atezolizumab–bevacizumab may maintain patients’ QOL over a longer period compared with sorafenib. |
These results can potentially optimize decision-making by both patients with HCC and physicians, when understanding treatments’ characteristics as a whole is of the uttermost importance. These results should, therefore, be considered in conjunction with other clinical outcomes such as survival and adverse event profile. |
Introduction
The World Health Organization defines health as “a state of complete physical, mental and social well-being, not merely the absence of disease and infirmity” [1]. This definition encourages moving away from the sole focus of evaluation based on traditional outcomes such as survival and morbidity, and the move towards a holistic approach including additional measures such as of quality of life (QOL) [2].
Quality of life is therefore an important outcome to consider, particularly in patients with a short life expectancy, as maximizing their QOL could offer a substantial benefit to their remaining time alive. Quality of life measures allow us to evaluate the impact of treatments on patients’ lives and enable informed decision-making by both patients and clinicians [3]. This can improve patient experience, but also support optimum treatment selection for patients in an environment where there may be several treatment options available and more still in development. Interestingly, several patient preference studies in oncology have also demonstrated how important QOL is for patients with cancer, with some being willing to trade time alive for treatments with less negative impacts on their QOL [3,4,5,6,7,8,9,10]. Taking this into consideration a comparative analysis of time to deterioration (TTD) in QOL for different treatments for patients with advanced and unresectable hepatocellular carcinoma (HCC) would provide valuable information which can be used in treatment selection decisions.
HCC is a cancer composed of malignant hepatocytes that develop in the parenchymal tissue of the liver, and is the predominant histology of primary liver cancer, accounting for approximately 80% of all cases [11]. It is the sixth most common malignancy worldwide, with an estimated 905,677 new cases diagnosed in 2020 [12]. Although in some cases treatments can be curative, in Western countries a large proportion of patients (approximately 50%) are diagnosed with later stage disease (Barcelona Clinic Liver Cancer [BCLC] stages C and D) that is not amenable to potentially curative therapy [13]. Treatment selection in HCC varies according to disease stage: patients with BCLC stage 0/A disease are preferentially treated with potentially curative therapies (resection, ablation, or liver transplant) that can be associated with long-term survival; on the other hand, patients with unresectable HCC (stages BCLC B and C) have historically been restricted to systemic therapy with sorafenib (Bayer AG, Leverkusen, Germany), or locoregional therapy with transarterial radioembolization (TARE, also known as selective internal radiation therapy) or transarterial chemoembolization (TACE) [13].
SIR-Spheres® Y-90 resin microspheres (SIR-Spheres; Sirtex Medical Inc, Woburn, Massachusetts, USA) are a form of TARE consisting of resin microspheres containing radioactive yttrium-90. They deliver radiation directly to tumors through the hepatic artery, thereby limiting damage to normal liver cells. Positioning of TARE within the treatment algorithm is based on results from two phase III randomized controlled trials (RCTs), SARAH and SIRveNIB, comparing TARE using SIR-Spheres with sorafenib which show that SIR-Spheres results in comparable outcomes between the two arms (i.e., overall survival [OS] and progression-free survival [PFS]), while minimizing the impact of adverse events [14, 15]. The results of these RCTs were further supported by the conclusions of a meta-analysis that demonstrated that TARE with SIR-Spheres as initial therapy is noninferior to sorafenib in terms of OS, while offering a better safety profile [16]. Additionally, a recent analysis of the QOL data collected within the SARAH RCT found that TARE was associated with significantly better preservation of QOL and significantly delayed TTD in QOL relative to sorafenib in patients with locally advanced, unresectable HCC (and including in patients with macroscopic vascular invasion) [17].
The first-line systemic treatment landscape for HCC has changed substantially based on results from the IMbrave150 trial where atezolizumab–bevacizumab (F. Hoffmann-La Roche Ltd., Basel, Switzerland) demonstrated superiority over sorafenib for the first time in terms of OS and QOL [18]. However, no head-to-head comparisons of TARE with atezolizumab–bevacizumab have been undertaken and, to the authors’ knowledge, there are no data available to patients and clinicians on the comparative impact of these treatments on patients’ QOL. The current study therefore addresses this gap by undertaking an indirect analysis of TTD in QOL of TARE versus atezolizumab–bevacizumab, using data of sorafenib as the common comparator across trials, and aims to generate results that allow better decision-making by both patients with HCC and physicians.
Methods
Data Sources and Analysis Process
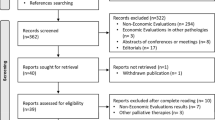
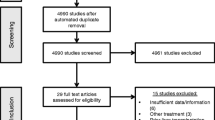
Individual patient-level data (IPD) from SARAH and published, aggregate data from IMbrave150 RCTs were used. Using sorafenib as the common comparator (Fig. 1), an anchored matching-adjusted indirect comparison (MAIC) was conducted to compare TARE using SIR-Spheres with atezolizumab–bevacizumab by matching trial characteristics and adjusting for between-trial differences in the distribution of variables that influence the outcome of interest. This methodology has been widely used in the absence of head-to-head clinical trials and is accepted by health technology assessment (HTA) agencies such as the National Institute for Health and Care Excellence (NICE) [19,20,21,22,23]. The MAIC was performed following NICE Decision Support Unit guidelines for population-adjusted indirect comparisons [23]. The analysis process flowchart is depicted in Fig. 2. All the analyses were conducted in R (version 4.0.3) [24]. Protocol and ethical approval for the SARAH study was granted by the Comité de Protection des Personnes Ile de France XI. In the IMbrave150 study, protocol approval was obtained from the institutional review board or ethics committee at each site. Both studies were done in accordance with the provisions of the International Council for Harmonisation of Technical Requirements for Pharmaceuticals for Human Use Guidelines for Good Clinical Practice and the Declaration of Helsinki. All patients in both studies provided written informed consent.
Comparison of Data Sources
Initially, SARAH and IMbrave150 RCT designs were compared to evaluate whether there were important differences preventing a reliable analysis (Supplementary Material, Supplementary Table 1) [14, 18]. Important similarities across trials include (i) sorafenib was the comparator arm in both studies, with the same treatment schedule; (ii) randomization was conducted using the Eastern Cooperative Oncology Group Performance Status (ECOG PS) and the presence of macroscopic vascular invasion as stratification factors; (iii) both studies were open label; (iv) OS, PFS and EORTC QLQ-C30 were collected as either primary or secondary outcomes; (v) both studies had the following key inclusion criteria: ECOG PS 0 or 1, and patients had at least one untreated lesion as per RECIST v1.1; (vi) IMbrave150 included patients without prior systemic therapy for HCC, while previous systemic treatment was an exclusion criterion in SARAH.
The following key differences were identified: (i) SARAH was conducted in French treatment centers only, whereas IMbrave150 was a multi-country study with treatment centers in Asia-Pacific, Europe, and the USA; (ii) IMbrave150 allowed the participation of patients with metastatic HCC, whereas significant extrahepatic disease (except lung tumors less than 1 cm and lymph nodes less than 2 cm) was an exclusion criterion in SARAH; (iii) SARAH included patients with Child–Pugh class A or B (score of 7 or lower), whereas IMbrave150 only allowed class A patients. The availability of IPD from SARAH enabled the removal of patients with Child–Pugh class B from SARAH, but the other two key differences between the trials represented unavoidable limitations for this analysis. Patients’ baseline characteristics in SARAH and IMbrave150 were then compared [14, 18].
A side-by-side comparison showed that some baseline characteristics were balanced across treatment arms and trials, while others differed substantially (Table 1). The following baseline characteristics were considered to be balanced: age, sex (despite the proportion of males being slightly higher in SARAH), and ECOG PS. Baseline characteristics that varied substantially across trials include Child–Pugh class (16% of patients in SARAH were categorized as Child–Pugh class B at study initiation, while these patients were excluded from IMbrave150), BCLC stage, etiology (approximately 30% of patients in SARAH had HCC caused by either hepatitis B or C virus, with approximately 70% patients in IMbrave150), and the proportion of patients with macrovascular invasion.
Using IPD from SARAH (i.e., unmatched and unadjusted), the TTD in QOL was calculated using the Global Health Score (GHS) from the EORTC QLQ-C30 questionnaire. This was calculated for the intention-to-treat (ITT) population and in line with the definition of TTD in QOL in the IMbrave150 study protocol, where TTD was defined as a decrease from baseline of 10 points or more on the GHS for two consecutive assessments or when there was a decrease of 10 points or more in one assessment followed by death within 3 weeks (see Supplementary Material for further details) [18]. For the comparison of survival curves, published TTD in QOL data from IMbrave150 were digitized with the DigitizeIt software and, using the algorithm developed by Guyot et al., patient-level data were reconstructed [18, 25]. Also, a linear mixed model (LMM) was implemented to shed light on the values of the GHS for each treatment arm before and after deterioration in QOL: fixed effects included treatment arm, deterioration in QOL (GHS measurement before/at the time of, or after deterioration) and an interaction term for treatment arm and deterioration in QOL; a random intercept was included for patient.
Matching
On the basis of the comparison of study design characteristics, as well as the inclusion and exclusion criteria of SARAH and IMbrave150 trials, patients with Child–Pugh score B were removed from the SARAH IPD to align with the population in IMbrave150.
Covariate Selection for Population Adjustment
NICE guidelines state researchers must demonstrate that population adjustment is likely to produce less biased estimates than standard indirect comparisons [23]. This requires (a) showing that there are grounds for believing one or more of the available covariates are effect modifiers, and (b) showing that there is sufficient imbalance in those effect modifiers to result in a material bias [23]. Also, NICE states that for anchored MAICs all effect modifiers should be adjusted for, while purely prognostic variables should not be accounted for to avoid standard error due to overmatching [23]. For this purpose, the covariate selection was conducted in two steps: (1) identification of covariates of potential interest: the literature was reviewed to identify potential effect modifiers of TTD in QOL; and (2) identification of effect modifiers: Cox regression models were implemented, using IPD from SARAH, to evaluate whether the covariates of potential interest identified in the literature could be confirmed as effect modifiers within the SARAH data set. The analyses identified ECOG PS and alpha-fetoprotein level as potential effect modifiers and were selected for the MAIC despite the close alignment in these covariates across trials. Cause of disease (defined as viral vs non-viral) and macrovascular invasion were also included in the MAIC, as they were identified as effect modifiers in the literature (although not in the SARAH data set) and there was some level of imbalance across trials. Further details on covariate selection are provided in the Supplementary Material. In a sensitivity analysis, viral cause of disease was defined as either hepatitis B, hepatitis C, or non-viral, providing further granularity to this covariate in line with the literature, despite the risk of reducing the effective sample size substantially.
Population Adjustment and Indirect Comparison
Prior to population adjustment, patients with incomplete data were removed to generate the final data set. The baseline characteristics of matched patients in SARAH were reweighted via the method of moments [23, 26]. Reweighted data from SARAH were used to indirectly compare TTD in QOL with TARE and atezolizumab–bevacizumab. The scale of the outcome for the indirect comparison was log hazard ratio (HR), as per NICE methods [23]. Kaplan–Meier curves and median TTD in QOL were estimated, as well as the HR (and 95% confidence interval [CI]) for TARE versus atezolizumab–bevacizumab.
Results
Of 459 patients in the SARAH ITT population 305 had GHS measurements at more than one time point, one being the measurement at baseline (135 and 170 in the TARE and sorafenib arms, respectively). These were the patients included in the unmatched and unadjusted analysis. Time-to-deterioration in QOL was 6.93 months for TARE, compared with 4.30 months for sorafenib, with a HR of 0.69 (95% CI 0.54–0.88; p = 0.003; Table 2; Fig. 3). The LMM showed higher values for TARE (p = 0.061), a significant reduction of − 15 points in GHS after deterioration (p < 0.001), and no interaction between treatment arm and whether the measurement happened before or after deterioration (p = 0.110; Supplementary Material, Supplementary Table 3).
Out of these 305 patients, cause of disease was missing for 31 and alpha-fetoprotein level was missing for 24. Of the remaining patients, 33 had a Child–Pugh score B and were therefore removed. The final data set for the MAIC therefore consisted of 217 patients: 94 and 123 in the TARE and sorafenib arms, respectively. A flowchart detailing patient numbers at various analysis steps is available in Supplementary Fig. 1.
Base Case Analysis
The application of the population adjustment algorithm resulted in balanced covariates across SARAH and IMbrave150 (Table 3). The effective sample size, however, decreased to 90. No individual had a weight of zero (minimum = 0.21; maximum = 4.99). The survival estimates and Kaplan–Meier curves of all four treatment arms in SARAH and IMbrave150, are reported in Table 4 and Fig. 4, respectively. There were statistically significant differences among the Kaplan–Meier curves (p < 0.001). The atezolizumab–bevacizumab combination resulted in the longest median TTD in QOL (11.23 months; 95% CI 6.15–NE), followed by TARE (8.64 months; 95% CI 7.16–19.02), although the difference between these was not statistically significant (i.e., 95% CIs overlapped). The HR for TARE, compared with atezolizumab–bevacizumab, was 1.06 (95% CI 0.75–1.50; p [weighted Cox model] = 0.725). The sorafenib treatment arms from both SARAH and IMbrave150 had a significantly lower median TTD in QOL.
Sensitivity Analysis
The application of the population adjustment algorithm also resulted in balanced covariates across SARAH and IMbrave150 (Table 3). The effective sample size further decreased to 36 patients as a result of the additional granularity of cause of disease. No individual had a weight of zero (minimum = 0.22; maximum = 16.65). The survival estimates and Kaplan–Meier curves of all four treatment arms in SARAH and IMbrave150 are reported in Table 4 and Fig. 5, respectively. There were statistically significant differences among the Kaplan–Meier curves (p < 0.0001). The TARE arm resulted in the longest median TTD in QOL (19.88 months; 95% CI 9.59–24.30), followed by the atezolizumab–bevacizumab combination (11.23 months; 95% CI 6.15–NE), although the difference between these was not statistically significant (i.e., 95% CIs overlapped). The HR for TARE, compared with atezolizumab–bevacizumab, was 0.66 (95% CI 0.36–1.19; p [weighted Cox model] = 0.163). The sorafenib treatment arms from both SARAH and IMbrave150 had a lower median TTD in QOL, although the uncertainty in SARAH was large and the 95% CI overlapped with those of TARE and atezolizumab–bevacizumab.
Discussion
This analysis provides physicians with meaningful insights into the time frames in which QOL is maintained and deteriorates when treating patients with advanced HCC with TARE, atezolizumab–bevacizumab, and sorafenib. The MAIC found no statistically significant differences in TTD in QOL in between TARE using SIR-Spheres and atezolizumab–bevacizumab. The base case analysis showed the longest TTD in QOL for atezolizumab–bevacizumab (median of 11.23 months), followed by TARE (median of 8.64 months), although the difference between these was not statistically significant. The results showed that sorafenib had a statistically significantly shorter TTD in QOL, compared with TARE (median of 5.52 and 3.58 months in the matching-adjusted SARAH population and IMbrave150, respectively). The sensitivity analysis resulted in longest TTD in QOL for TARE (median of 19.88 months), followed by atezolizumab–bevacizumab, although the difference between these was again statistically not significant. Sorafenib had a shorter TTD, with a statistically significant difference in the case of the IMbrave150 arm.
Even though survival is usually the most important treatment attribute for both patients and physicians, studies have demonstrated that other attributes such as adverse event profile or mode of administration (e.g., intravenous versus a one-off procedure) can play a significant role, with patients willing to make substantial trade-offs between survival and the risk of adverse events [7,8,9,10]. For this reason, the results from this MAIC demonstrate that TARE using SIR-Spheres can be a reliable treatment option when treatment attributes such as adverse event profiles, with the subsequent impact on QOL, are key to patients and physicians making therapeutic decisions [27,28,29]. This is particularly relevant when considering the results of the SARAH RCT, where despite the lack of statistically significant differences in efficacy, it has been shown that TARE using SIR-Spheres offer a longer time without deterioration of QOL compared with sorafenib, and could therefore be a preferred treatment for patients and physicians [17]. The NEMESIS meta-analysis further reinforced this idea concluding that TARE with SIR-Spheres as initial therapy for advanced HCC is non-inferior to sorafenib in terms of OS, while offering a better safety profile [16]. Furthermore, the IMbrave150 RCT also showed, as the SARAH and SIRveNIB RCTs did, that there are patient subgroups for which no statistically significant differences exist in treatment efficacy and therefore treatment selection may not be straightforward [14, 15, 18]. All this supports the conclusion that patients and physicians should carefully consider and select a particular treatment for advanced and unresectable HCC by gauging patients’ and treatments’ characteristics in a holistic manner.
This analysis has some strengths that underline its value. The SARAH and SIRveNIB are the only RCTs showing a head-to-head comparison of TARE with a systemic treatment in HCC; EORTC QLQ-C30, however, was only measured in SARAH. Therefore, this analysis represents, to the authors’ knowledge, the only possible approach that can reliably compare QOL outcomes of a TARE (i.e., SIR-Spheres) with atezolizumab–bevacizumab using IPD. A typical limitation of MAIC studies is the impact of unobserved or unmeasured confounders [20, 21, 23, 30]. Although it is likely that not all potentially relevant confounders were included in the reweighting model used for this MAIC, the literature was thoroughly searched and patient-level data from SARAH were analyzed in depth to identify the key potential effect modifiers. Justifying the effect modifier status of variables included in the weighting model is considered essential in the eyes of HTA agencies such as NICE, and therefore the effort to identify the key potential effect modifiers represents an important strength of the analysis presented here [23, 31]. Also, because disease etiology (defined as hepatitis C) was identified as an effect modifier in the literature, a sensitivity analysis explored the results considering etiology as either hepatitis B, hepatitis C, or other cause. The effective sample size in this case was lower than in the base case and the results are therefore more uncertain; however, the generated results provide clinicians and patients with a full picture on which decisions can be based. Finally, the results from this study were in line with the results from the analysis by Pereira et al., endorsing the appropriateness of these analyses. Pereira et al. reported a significant difference in TTD in QOL between TARE using SIR-Spheres (median 3.9 months; 95% CI 3.7–4.3) and sorafenib (median 2.6 months; 95% CI 2.0–3.0) [17]. The lower median values reported by Pereira et al., compared with the results from this study, are not surprising because of the differences in the definitions of TTD in QOL used.
This study also had some limitations and therefore the results presented here should be interpreted taking these into consideration. Although the potential for bias was considerably reduced after matching, there were unavoidable differences between clinical trial designs [14, 18]. A key difference is the timing of QOL measurements between SARAH and IMbrave150: in SARAH, the EORTC QLQ-C30 questionnaire was completed by patients at months 1, 3, and every 3 months thereafter, whereas in IMbrave150 patients were asked to complete the questionnaires on cycle 1, at every three-weekly cycle until treatment discontinuation or disease progression, and every 3 months (for 1 year) thereafter. The longer measurement intervals in SARAH (at least before patients in IMbrave150 progress or discontinue treatment) may have confounded the results, in some cases potentially capturing QOL deterioration later than when it actually happened (although it is also possible that instances captured as deterioration in SARAH would not have been captured as such in IMbrave150). This is an unavoidable limitation associated with the design of both SARAH and IMbrave150 trials, but one that should be considered when interpreting the results. Also, the number of patients from SARAH excluded from the analysis was high because of the lack of responses to QOL questionnaires (completion rates of 77.5% and 80.4% in the TARE and sorafenib groups, respectively); compliance in IMbrave150 seemed to be substantially higher (at least 93% from baseline until cycle 17 and at least 80% thereafter), although this was defined as completion of at least one question, which could potentially misrepresent the actual responses collected on the GHS scale [17, 18]. In terms of patients’ baseline characteristics, a higher proportion of patients presented with macrovascular invasion in SARAH compared with IMbrave150, which indicated that patients in SARAH may have had a poorer prognosis [32]. In both trials, the proportion of BCLC C patients was higher than the proportion of BCLC B patients, and the latter was higher than the proportion of BCLC A patients. The spread of BCLC C and BCLC B patients was somewhat different between SARAH and IMbrave150 trials, with a higher proportion of BCLC C patients in IMbrave150 (including patients with macrovascular invasion and extrahepatic metastases) compared with SARAH. Despite these differences not being enormous, patients in IMbrave150 may have had a more advanced disease.
When interpreting the results of these analyses, focus should be placed on the way TTD in QOL was defined [18]. Even though many clinical trials now include QOL as one of the key outcomes, its analysis is still not standardized, thereby hindering the comparability of results across trials and the literature [33, 34]. Time to deterioration in QOL analyses rely, among other factors, on the threshold used to determine clinical relevance, with a change of 10 or more points on the GHS (in a single measurement) being one of the most common thresholds [33,34,35,36,37,38,39,40]. Although to a lesser extent, other thresholds have also been evaluated [41, 42]. Apart from the threshold, the consideration or not of competing risks (e.g., death, progression, or toxicity) or the requirement for confirmation of deterioration in QOL is likely to play an important role, and different results could be expected depending on the approach chosen [33, 43]. For the MAIC to be relevant, TTD in QOL in SARAH had to match the definition in IMbrave150; however, the IMbrave150 protocol was not clear, for instance, on how data were handled when no TTD in QOL event occurred but death was captured at a time later than the last QOL measurement. In these cases, this MAIC conservatively assumed the last date of QOL measurement to be the date of the event, even without a decrease of 10 or more points from baseline. The lack of knowledge of how these data were handled in IMbrave150 represents a limitation in this analysis, and the TTD in QOL estimates presented for TARE may be conservative compared with what the estimates would be if the data were in fact managed differently in IMbrave150. Conversely, because IMbrave150 had a conservative approach to define TTD in QOL, all the estimates presented here cannot be directly compared with other data for TTD in QOL presented in the literature unless the outcome definitions match. All this, along with the different timing of QOL measurements, means the results from these analyses are not as robust as the conclusions from a purposely conducted clinical trial would be. This analysis and the facts stated here, however, could ideally guide future clinical trial design to improve the comparability of clinical trial data and advance the understanding of QOL outcomes in disease areas where this is crucial.
Finally, as demonstrated by Lo et al. [10], treatments’ characteristics should be assessed in a holistic manner when making a decision of the best approach to treatment, and for that reason the results from these analyses should be considered in conjunction with indirect comparisons evaluating other outcomes (e.g., OS, PFS, response rates, or adverse events). This is particularly relevant given the differences observed between the SARAH and IMbrave150 RCTs. Median OS was 9.9 months for both TARE and sorafenib in the per protocol populations in SARAH; in IMbrave150, however, median OS was not reached for atezolizumab–bevacizumab (with 67.2% of patients alive at 12 months) and was 13.2 months for sorafenib. With regard to the safety profile, 41% and 63% of patients receiving TARE and sorafenib had grade ≥ 3 adverse events in SARAH, whereas this proportion was 61% in both treatment arms in IMbrave150. These unmatched and unadjusted results indicate clinically relevant differences in efficacy and safety may exist between these treatments and, for that reason, indirect comparisons adjusting for between-trial differences are needed for a fair comparison. Because of the interesting clues that the current analyses have provided, future research will include indirect comparisons of other outcomes so that a full picture is provided to relevant stakeholders.
Conclusions
TARE using SIR-Spheres may achieve similar TTD in QOL compared with atezolizumab–bevacizumab, as the analyses found no statistically significant differences between these two interventions. The MAIC also showed that both TARE using SIR-Spheres and atezolizumab–bevacizumab seem to be more efficacious than sorafenib in maintaining QOL. These results are relevant for patients and clinicians, as preference studies show the role of QOL in treatment selection and therefore the treatment strategy can be adapted to maximize the benefit for patients.
References
IH Conference. Constitution of the World Health Organization 1946. Bull World Health Organ. 2002;80(12):983–4.
Salvador-Carulla L, Lucas R, Ayuso-Mateos JL, Miret M. Use of the terms “wellbeing” and “quality of life” in health sciences: a conceptual framework. Eur J Psychiatry. 2014;28:50–65. http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S0213-61632014000100005&nrm=iso.
Aning JJ, Wassersug RJ, Goldenberg SL. Patient preference and the impact of decision-making aids on prostate cancer treatment choices and post-intervention regret. Curr Oncol. 2012;19(Suppl 3):S37–44. https://doi.org/10.3747/co.19.1287.
Pauwels K, Huys I, Casteels M, Denier Y, Vandebroek M, Simoens S. What does society value about cancer medicines? A discrete choice experiment in the Belgian population. Appl Health Econ Health Policy. 2019;17(6):895–902. https://doi.org/10.1007/s40258-019-00504-4.
Schmidt K, Damm K, Vogel A, et al. Therapy preferences of patients with lung and colon cancer: a discrete choice experiment. Patient Prefer Adherence. 2017;11:1647–56. https://doi.org/10.2147/PPA.S138863.
Ciruelos EM, Díaz MN, Isla MD, et al. Patient preference for oral chemotherapy in the treatment of metastatic breast and lung cancer. Eur J Cancer Care (Engl). 2019;28(6): e13164. https://doi.org/10.1111/ecc.13164.
Bridges JFP, Mohamed AF, Finnern HW, Woehl A, Hauber AB. Patients’ preferences for treatment outcomes for advanced non-small cell lung cancer: a conjoint analysis. Lung Cancer. 2012;77(1):224–31. https://doi.org/10.1016/j.lungcan.2012.01.016.
Uemura H, Matsubara N, Kimura G, et al. Patient preferences for treatment of castration-resistant prostate cancer in Japan: a discrete-choice experiment. BMC Urol. 2016;16(1):63. https://doi.org/10.1186/s12894-016-0182-2.
Srinivas S, Mohamed AF, Appukkuttan S, et al. Patient and caregiver benefit-risk preferences for nonmetastatic castration-resistant prostate cancer treatment. Cancer Med. 2020;9(18):6586–96. https://doi.org/10.1002/cam4.3321.
Lo SH, Sharma R, Costentin CE, et al. Patient preferences for advanced hepatocellular carcinoma treatment: a multicountry stated preference study. Future Oncol. 2021;17:4275–87. https://doi.org/10.2217/fon-2021-0697.
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68(6):394–424. https://doi.org/10.3322/caac.21492.
The Global Cancer Observatory (International Agency for Research on Cancer—World Health Organization). All cancers. 2020. https://gco.iarc.fr/today/data/factsheets/cancers/39-All-cancers-fact-sheet.pdf. Accessed July 13, 2021.
EASL Clinical Practice Guidelines. Management of hepatocellular carcinoma. J Hepatol. 2018;69(1):182–236. https://doi.org/10.1016/j.jhep.2018.03.019.
Vilgrain V, Pereira H, Assenat E, et al. Efficacy and safety of selective internal radiotherapy with yttrium-90 resin microspheres compared with sorafenib in locally advanced and inoperable hepatocellular carcinoma (SARAH): an open-label randomised controlled phase 3 trial. Lancet Oncol. 2017;18(12):1624–36. https://doi.org/10.1016/S1470-2045(17)30683-6.
Chow PKH, Gandhi M, Tan S-B, et al. SIRveNIB: selective internal radiation therapy versus sorafenib in Asia-Pacific patients with hepatocellular carcinoma. J Clin Oncol. 2018;36(19):1913–21. https://doi.org/10.1200/JCO.2017.76.0892.
Venerito M, Pech M, Canbay A, et al. NEMESIS: noninferiority, individual-patient metaanalysis of selective internal radiation therapy with (90)Y resin microspheres versus sorafenib in advanced hepatocellular carcinoma. J Nucl Med. 2020;61(12):1736–42. https://doi.org/10.2967/jnumed.120.242933.
Pereira H, Bouattour M, Dioguardi Burgio M, et al. Health-related quality of life in locally advanced hepatocellular carcinoma treated by either radioembolisation or sorafenib (SARAH trial). Eur J Cancer. 2021;154:46–56. https://doi.org/10.1016/j.ejca.2021.05.032.
Finn RS, Qin S, Ikeda M, et al. Atezolizumab plus bevacizumab in unresectable hepatocellular carcinoma. N Engl J Med. 2020;382(20):1894–905. https://doi.org/10.1056/NEJMoa1915745.
Chowdhury S, Oudard S, Uemura H, et al. Matching-adjusted indirect comparison of health-related quality of life and adverse events of apalutamide versus enzalutamide in non-metastatic castration-resistant prostate cancer. Adv Ther. 2020;37(1):512–26. https://doi.org/10.1007/s12325-019-01157-4.
Chowdhury S, Oudard S, Uemura H, et al. Matching-adjusted indirect comparison of the efficacy of apalutamide and enzalutamide with ADT in the treatment of non-metastatic castration-resistant prostate cancer. Adv Ther. 2020;37(1):501–11. https://doi.org/10.1007/s12325-019-01156-5.
Kelley RK, Mollon P, Blanc J-F, et al. Comparative efficacy of cabozantinib and regorafenib for advanced hepatocellular carcinoma. Adv Ther. 2020;37(6):2678–95. https://doi.org/10.1007/s12325-020-01378-y.
Song J, Ma Q, Gao W, et al. Matching-adjusted indirect comparison of blinatumomab vs. inotuzumab ozogamicin for adults with relapsed/refractory acute lymphoblastic leukemia. Adv Ther. 2019;36(4):950–61. https://doi.org/10.1007/s12325-019-0873-7.
Phillippo DM, Ades AE, Dias S, Palmer S, Abrams KR, Welton NJ. NICE DSU technical support document 18: methods for population-adjusted indirect comparisons in submissions to NICE; 2016. http://www.nicedsu.org.uk/Populationadjusted-ICs-TSD(3026862).htm. Accessed Apr 22, 2021
R Core Team. R: a language and environment for statistical computing. 2020. https://www.r-project.org/. Access Dec 1, 2020
Guyot P, Ades AE, Ouwens MJNM, Welton NJ. Enhanced secondary analysis of survival data: reconstructing the data from published Kaplan–Meier survival curves. BMC Med Res Methodol. 2012;12(1):9. https://doi.org/10.1186/1471-2288-12-9.
Signorovitch JE, Wu EQ, Yu AP, et al. Comparative effectiveness without head-to-head trials: a method for matching-adjusted indirect comparisons applied to psoriasis treatment with adalimumab or etanercept. Pharmacoeconomics. 2010;28(10):935–45. https://doi.org/10.2165/11538370-000000000-00000.
Di Maio M, Leighl NB, Gallo C, et al. Quality of life analysis of TORCH, a randomized trial testing first-line erlotinib followed by second-line cisplatin/gemcitabine chemotherapy in advanced non-small-cell lung cancer. J Thorac Oncol. 2012;7(12):1830–44. https://doi.org/10.1097/JTO.0b013e318275b327.
Patil S, Figlin RA, Hutson TE, et al. Q-TWiST analysis to estimate overall benefit for patients with metastatic renal cell carcinoma treated in a phase III trial of sunitinib vs interferon-α. Br J Cancer. 2012;106(10):1587–90. https://doi.org/10.1038/bjc.2012.149.
Gelber RD, Goldhirsch A. A new endpoint for the assessment of adjuvant therapy in postmenopausal women with operable breast cancer. J Clin Oncol. 1986;4(12):1772–9. https://doi.org/10.1200/JCO.1986.4.12.1772.
Tremblay G, Chandiwana D, Dolph M, Hearnden J, Forsythe A, Monaco M. Matching-adjusted indirect treatment comparison of ribociclib and palbociclib in HR+, HER2- advanced breast cancer. Cancer Manag Res. 2018;10:1319–27. https://doi.org/10.2147/CMAR.S163478.
National Institute for Health and Care Excellence. Guide to the methods of technology appraisal. 2013. https://www.nice.org.uk/process/pmg9/chapter/foreword. Accessed April 22, 2021.
Costentin CE, Ferrone CR, Arellano RS, Ganguli S, Hong TS, Zhu AX. Hepatocellular carcinoma with macrovascular invasion: defining the optimal treatment strategy. Liver Cancer. 2017;6(4):360–74. https://doi.org/10.1159/000481315.
Anota A, Hamidou Z, Paget-Bailly S, et al. Time to health-related quality of life score deterioration as a modality of longitudinal analysis for health-related quality of life studies in oncology: do we need RECIST for quality of life to achieve standardization? Qual Life Res. 2015;24(1):5–18. https://doi.org/10.1007/s11136-013-0583-6.
Skaltsa K, Casamayor M, Ivanescu C. PRM26—time to deterioration (TTD) in health related quality of life (HRQOL) in NSCLC patients: a review of definitions. Value Health. 2018;21:S360. https://doi.org/10.1016/j.jval.2018.09.2150.
Weisel K, Ludwig H, Rieth A, Lebioda A, Goldschmidt H. Health-related quality of life of carfilzomib- and daratumumab-based therapies in patients with relapsed/refractory multiple myeloma, based on German benefit assessment data. Qual Life Res. 2020;29(1):69–79. https://doi.org/10.1007/s11136-019-02307-5.
Hemstock M, Amadi A, Kupas K, et al. Indirect treatment comparison of nivolumab versus placebo for the adjuvant treatment of melanoma. Eur J Cancer. 2020;132:176–86. https://doi.org/10.1016/j.ejca.2020.03.011.
Ludwig H, Pönisch W, Knop S, et al. Quality of life in patients with relapsed/refractory multiple myeloma during ixazomib-thalidomide-dexamethasone induction and ixazomib maintenance therapy and comparison to the general population. Leuk Lymphoma. 2020;61(2):377–86. https://doi.org/10.1080/10428194.2019.1666381.
Lenz H-J, Argiles G, Yoshino T, et al. Health-related quality of life in the phase III LUME-colon 1 study: comparison and interpretation of results from EORTC QLQ-C30 analyses. Clin Colorectal Cancer. 2019;18(4):269-279.e5. https://doi.org/10.1016/j.clcc.2019.08.005.
Al-Batran S-E, Van Cutsem E, Oh SC, et al. Quality-of-life and performance status results from the phase III RAINBOW study of ramucirumab plus paclitaxel versus placebo plus paclitaxel in patients with previously treated gastric or gastroesophageal junction adenocarcinoma. Ann Oncol. 2016;27(4):673–9. https://doi.org/10.1093/annonc/mdv625.
Harrington KJ, Ferris RL, Blumenschein G Jr, et al. Nivolumab versus standard, single-agent therapy of investigator’s choice in recurrent or metastatic squamous cell carcinoma of the head and neck (CheckMate 141): health-related quality-of-life results from a randomised, phase 3 trial. Lancet Oncol. 2017;18(8):1104–15. https://doi.org/10.1016/S1470-2045(17)30421-7.
Cocks K, King MT, Velikova G, et al. Evidence-based guidelines for interpreting change scores for the European Organisation for the Research and Treatment of Cancer Quality of Life Questionnaire Core 30. Eur J Cancer. 2012;48(11):1713–21. https://doi.org/10.1016/j.ejca.2012.02.059.
Hamidou Z, Dabakuyo TS, Mercier M, et al. Time to deterioration in quality of life score as a modality of longitudinal analysis in patients with breast cancer. Oncologist. 2011;16(10):1458–68. https://doi.org/10.1634/theoncologist.2011-0085.
Anota A, Boulin M, Dabakuyo-Yonli S, et al. An explorative study to assess the association between health-related quality of life and the recommended phase II dose in a phase I trial: idarubicin-loaded beads for chemoembolisation of hepatocellular carcinoma. BMJ Open. 2016;6(6):e010696. https://doi.org/10.1136/bmjopen-2015-010696.
Bruix J, Cheng A-L, Meinhardt G, Nakajima K, De Sanctis Y, Llovet J. Prognostic factors and predictors of sorafenib benefit in patients with hepatocellular carcinoma: analysis of two phase III studies. J Hepatol. 2017;67(5):999–1008. https://doi.org/10.1016/j.jhep.2017.06.026.
Fayers P, Aaronson N, Bjordal K, Groenvold M, Curran D, Bottomley A. The EORTC QLQ-C30 Scoring Manual, 3rd ed.; 2001. http://www.eortc.be/qol/files/scmanualqlq-c30.pdf. Accessed Apr 22, 2021
Acknowledgements
Funding
This study was funded by Sirtex Medical United Kingdom Ltd (London, UK). The journal’s Rapid Service and Open Access fees were purchased using funding provided by the study sponsor.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work, and have given their approval for this version to be published.
Author Contributions
All authors (Ion Agirrezabal, Victoria K Brennan, Fabien Colaone, Suki Shergill, Helena Pereira, Gilles Chatellier, and Valérie Vilgrain) conceptualized and designed the study; Ion Agirrezabal collected, cleaned, and analyzed the data; all authors interpreted the data; Ion Agirrezabal and Victoria K Brennan drafted the manuscript; all authors revised the manuscript, approved its final version and provided consent for publication. No authors meeting the authorship criteria have been omitted.
Disclosures
Ion Agirrezabal, Victoria K Brennan, Fabien Colaone, and Suki Shergill were full-time employees of Sirtex at the time of manuscript preparation; Fabien Colaone is a full-time employee of Varian at the time of manuscript submission. Helena Pereira and Gilles Chatellier have no competing interests. Valérie Vilgrain reports personal fees from Sirtex during the period the study was conducted.
Compliance with Ethics Guidelines
Individual patient-level data from SARAH and published, aggregate data from IMbrave150 RCTs were used for this analysis. Protocol and ethical approval for the SARAH study was granted by the Comité de Protection des Personnes Ile de France XI. In the IMbrave150 study protocol approval was obtained from the institutional review board or ethics committee at each site. Both studies were done in accordance with the provisions of the International Council for Harmonisation of Technical Requirements for Pharmaceuticals for Human Use Guidelines for Good Clinical Practice and the Declaration of Helsinki. All patients in both studies provided written informed consent.
Data Availability
The data sets analyzed during the current study are not publicly available due to confidentiality reasons.
Author information
Authors and Affiliations
Corresponding author
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Agirrezabal, I., Brennan, V.K., Colaone, F. et al. Transarterial Radioembolization Versus Atezolizumab–Bevacizumab in Unresectable Hepatocellular Carcinoma: A Matching-Adjusted Indirect Comparison of Time to Deterioration in Quality of Life. Adv Ther 39, 2035–2051 (2022). https://doi.org/10.1007/s12325-022-02099-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-022-02099-0