Abstract
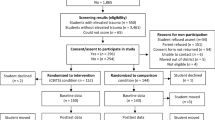
The Bounce Back program (Langley et al. in J Consult Clin Psychol 83:853, 2015) effectively reduces post-traumatic stress (PTS) symptoms and internalizing problems among Elementary students (Langley et al. in J Consult Clin Psychol 83:853, 2015; Santiago et al. in School Psychol Q 33:1–9, 2018). Some school settings may modify the program to accommodate challenges such as logistic difficulties (e.g., a busy academic schedule) and clinicians’ discomfort with parts of the protocol (i.e., the trauma narrative). Thus, research is needed to answer the question, “Can we expect to observe change if we implement a modified Bounce Back program?” Our objectives were to (1) replicate treatment outcomes, (2) examine the timing of symptom reduction to determine whether symptoms abated before and/or after the trauma narrative, and (3) test whether baseline factors predicted incremental benefits of the trauma-narrative for PTS reduction. Twenty K-5 th grade students (47.4% Hispanic/Latino, 36.8% African-American, and 63.2% White; 68% boys) attending an urban Title I Elementary school completed the Bounce Back program and reported symptoms at pre, mid therapy (immediately before the trauma narrative), and post therapy (immediately following the program). Consistent with other trials of the Bounce Back program, students in the current sample experienced significantly reduced PTS symptoms, distress, internalizing problems, and externalizing problems. Significant change in PTS and distress occurred in the first part of treatment before the trauma narrative and did not occur during the second part of treatment. The full course of treatment was needed for significant change on secondary outcomes of internalizing and externalizing problems. Distress and bereavement assessed at baseline did not predict incremental benefits of the second half of treatment. Findings yield implementation implications and directions for future research.






Similar content being viewed by others
References
Achenbach, T. M., & Rescorla, L. A. (2001). Manual for the ASEBA school-age forms & profiles. Burlington, VT: University of Vermont, Center for Children, Youth and Families.
Alegría, M., Fortuna, L. R., Lin, J. Y., Norris, L. F., Gao, S., Takeuchi, D. T., et al. (2013). Prevalence, risk, and correlates of posttraumatic stress disorder across ethnic and racial minority groups in the US. Medical Care, 51, 1114.
Alisic, E., Zalta, A. K., Van Wesel, F., Larsen, S. E., Hafstad, G. S., Hassanpour, K., et al. (2014). Rates of post-traumatic stress disorder in trauma-exposed children and adolescents: Meta-analysis. The British Journal of Psychiatry, 204, 335–340.
Baglivio, M. T., Wolff, K. T., Epps, N., & Nelson, R. (2017). Predicting adverse childhood experiences: The importance of neighborhood context in youth trauma among delinquent youth. Crime & Delinquency, 63, 166–188.
Becker, C., Darius, E., & Schaumberg, K. (2007). An analogue study of patient preferences for exposure versus alternative treatments of posttraumatic stress disorder. Behaviour Research and Therapy, 45, 2861–2873.
Becker, C. B., Zayfert, C., & Anderson, E. (2004). A survey of psychologists’ attitudes towards and utilization of exposure therapy for PTSD. Behaviour Research and Therapy, 42, 277–292.
Cohen, J. A., Mannarino, A. P., & Deblinger, E. (Eds.). (2012). Trauma-focused CBT for children and adolescents: Treatment applications. New York: Guilford Press.
Copeland, W. E., Keeler, G., Angold, A., & Costello, E. J. (2007). Traumatic events and posttraumatic stress in childhood. Archives of General Psychiatry, 64, 577–584.
Costello, E. J., Erkanli, A., Fairbank, J. A., & Angold, A. (2002). The prevalence of potentially traumatic events in childhood and adolescence. Journal of Traumatic Stress: Official Publication of the International Society for Traumatic Stress Studies, 15, 99–112.
Costello, E. J., Sampson, N. A., Kessler, R. C., & Merikangas, K. (2014). Services for adolescents with psychiatric disorders: 12-month data from the National Comorbidity Survey-Adolescent. Psychiatric Services, 65, 359–366.
Daviss, W. B., Mooney, D., Racusin, R., Ford, J. D., Fleischer, A., & McHUGO, G. J. (2000). Predicting posttraumatic stress after hospitalization for pediatric injury. Journal of the American Academy of Child & Adolescent Psychiatry, 39, 576–583.
de Arellano, M. A., Lyman, D. R., Jobe-Shields, L., George, P., Dougherty, R. H., Daniels, A. S., et al. (2014). Trauma-focused cognitive-behavioral therapy for children and adolescents: Assessing the evidence. Psychiatric Services (Washington, D.C.), 65(5), 591–602. https://doi.org/10.1176/appi.ps.201300255.
Deblinger, E., Mannarino, A. P., Cohen, J. A., Runyon, M. K., & Steer, R. A. (2011). Trauma-focused cognitive behavioral therapy for children: Impact of the trauma narrative and treatment length. Depression and Anxiety, 28, 67–75. https://doi.org/10.1002/da.20744.
Dunn, E. C., Nishimi, K., Powers, A., & Bradley, B. (2017). Is developmental timing of trauma exposure associated with depressive and post-traumatic stress disorder symptoms in adulthood? Journal of Psychiatric Research, 84, 119–127.
Elhai, J. D., Layne, C. M., Steinberg, A. S., Vrymer, M. J., Briggs, E. C., Ostrowski, S. A., et al. (2013). Psychometric properties of the UCLA PTSD Reaction Index. Part 2: Investigating factor structure findings in a national clinic-referred youth sample. Journal of Traumatic Stress, 26, 10–18.
Evans, C., Margison, F., & Barkham, M. (1998). The contribution of reliable and clinically significant change methods to evidence-based mental health. Evidence Based Mental Health, 1, 70–72.
Feeny, N. C., Zoellner, L. A., Mavissakalian, M. R., & Roy-Byrne, P. P. (2009). What would you choose? Sertraline or prolonged exposure in community and PTSD treatment seeking women. Depression and Anxiety, 26, 724–731. https://doi.org/10.1002/da.20588.
Flay, B. R., Biglan, A., Boruch, R. F., Castro, F. G., Gottfredson, D., Kellam, S., ... & Ji, P. (2005). Standards of evidence: Criteria for efficacy, effectiveness and dissemination. Prevention Science, 6(3), 151–175.
Fong, K. (2019). Neighborhood inequality in the prevalence of reported and substantiated child maltreatment. Child Abuse and Neglect, 90, 13–21.
Ford, I., Racusin, J. D., Acker, R., Bosquet, R., Ellis, C., & Schiffman, R. (2002). Traumatic Events Screening Inventory (TESI-PRR/TESI-SRR).
Goenjian, A. K., Karayan, I., Pynoos, R. S., Minassian, D., Najarian, L. M., Steinberg, A. M., et al. (1997). Outcome of psychotherapy among early adolescents after trauma. American Journal of Psychiatry, 154, 536–542.
Goenjian, A. K., Steinberg, A. M., Walling, D., Bishop, S., Karayan, I., & Pynoos, R. (2020). 25-year follow-up of treated and not-treated adolescents after the Spitak earthquake: Course and predictors of PTSD and depression. Psychological Medicine, 1–13.
Hayes, A. M., Laurenceau, J. P., Feldman, G., Strauss, J. L., & Cardaciotto, L. (2007). Change is not always linear: The study of nonlinear and discontinuous patterns of change in psychotherapy. Clinical Psychology Review, 27, 715–723.
Hembree, E. A., Foa, E. B., Dorfan, N. M., Street, G. P., Kowalski, J., & Tu, X. (2003). Do patients drop out prematurely from exposure therapy for PTSD? Journal of Traumatic Stress, 16, 555–562.
Hiller, R. M., Meiser-Stedman, R., Fearon, P., Lobo, S., McKinnon, A., Fraser, A., et al. (2016). Research review: Changes in the prevalence and symptom severity of child post-traumatic stress disorder in the year following trauma—A meta-analytic study. Journal of Child Psychology and Psychiatry, 57, 884–898.
Imel, Z. E., Laska, K., Jakupcak, M., & Simpson, T. L. (2013). Meta-analysis of dropout in treatments for posttraumatic stress disorder. Journal of Consulting and Clinical Psychology, 81, 394–404.
Jaycox, L. H., Cohen, J. A., Mannarino, A. P., Walker, D. W., Langley, A. K., Gegenheimer, K. L., et al. (2010). Children’s mental health care following Hurricane Katrina: A field trial of trauma-focused psychotherapies. Journal of Traumatic Stress: Official Publication of the International Society for Traumatic Stress Studies, 23, 223–231.
Kaplow, J. B., Rolon-Arroyo, B., Layne, C. M., Rooney, E., Oosterhoff, B., Hill, R., et al. (2019). Validation of the UCLA PTSD reaction index for DSM-5: A developmentally informed assessment tool for youth. Journal of the American Academy of Child and Adolescent Psychiatry, 59(1), 186–194.
Kataoka, S. H., Zhang, L., & Wells, K. B. (2002). Unmet need for mental health care among U.S. children: Variation by ethnicity and insurance status. The American Journal of Psychiatry, 159, 1548–1555.
Langley, A. K., Gonzalez, A., Sugar, C. A., Solis, D., & Jaycox, L. (2015). Bounce back: Effectiveness of an elementary school-based intervention for multicultural children exposed to traumatic events. Journal of Consulting and Clinical Psychology, 83, 853.
Langley, A. K., Nadeem, E., Kataoka, S. H., Stein, B. D., & Jaycox, L. H. (2010). Evidence-based mental health programs in schools: Barriers and facilitators of successful implementation. School Mental Health, 2, 105–113.
Layne, C. M., Saltzman, W. R., Poppleton, L., Burlingame, G. M., Pašalić, A., Duraković, E., et al. (2008). Effectiveness of a school-based group psychotherapy program for war-exposed adolescents: A randomized controlled trial. Journal of the American Academy of Child and Adolescent Psychiatry, 47, 1048–1062.
Lyon, A. R., & Bruns, E. J. (2019). From evidence to impact: Joining our best school mental health practices with our best implementation strategies. School Mental Health, 11, 106–114.
McLaughlin, K. A., Green, J. G., Gruber, M. J., Sampson, N. A., Zaslavsky, A., & Kessler, R. C. (2012). Childhood adversities and first onset of psychiatric disorders in a national sample of adolescents. Archives of General Psychiatry, 69, 1151–1160.
McLaughlin, K. A., Koenen, K. C., Hill, E., Petukhova, M., Sampson, N. A., Zaslavsky, A., et al. (2013). Trauma exposure and posttraumatic stress disorder in a US national sample of adolescents. Journal of the American Academy of Child and Adolescent Psychiatry, 52, 815–830. https://doi.org/10.1016/j.jaac.2013.05.011.
McLean, C. P., Yeh, R., Rosenfield, D., & Foa, E. B. (2015). Changes in negative cognitions mediate PTSD symptom reductions during client-centered therapy and prolonged exposure for adolescents. Behaviour Research and Therapy, 68, 64–69.
Nixon, R. D. V., Sterk, J., & Pearce, A. (2012). A randomized trial of cognitive behavior therapy and cognitive therapy for children with posttraumatic stress disorder following single-incident trauma. Journal of Abnormal Child Psychology, 40, 327–337.
Olatunji, B. O., Deacon, B. J., & Abramowitz, J. S. (2009). The cruelest cure? Ethical issues in the implementation of exposure-based treatments. Cognitive and Behavioral Practice, 16, 172–180.
Onken, L. S., Carroll, K. M., Shoham, V., Cuthbert, B. N., & Riddle, M. (2014). Reenvisioning clinical science: Unifying the discipline to improve the public health. Clinical Psychological Science, 2, 22–34. https://doi.org/10.1177/2167702613497932.
Ribbe, D. (1996). Psychometric review of Traumatic Event Screening Instrument for Children (TESI-C). In B. H. Stamm (Ed.), Measurement of stress, trauma, and adap- tation (pp. 144–151). Lutherville, MD: Sidran Pres.
Resick, P. A., Galovski, T. E., Uhlmansiek, M. O., Scher, C. D., Clum, G. A., & Young-Xu, Y. (2008). A randomized clinical trial to dismantle components of cognitive processing therapy for posttraumatic stress disorder in female victims of interpersonal violence. Journal of Consulting and Clinical Psychology, 76, 243–258.
Roberts, A. L., Gilman, S. E., Breslau, J., Breslau, N., & Koenen, K. C. (2011). Race/ethnic differences in exposure to traumatic events, development of post-traumatic stress disorder, and treatment-seeking for post-traumatic stress disorder in the United States. Psychological Medicine, 41, 71–83. https://doi.org/10.1017/S0033291710000401.
Rolfsnes, E. S., & Idsoe, T. (2011). School-based intervention programs for PTSD symptoms: A review and meta-analysis. Journal of Traumatic Stress, 24, 155–165.
Rubel, J., Lutz, W., & Schulte, D. (2015). Patterns of change in different phases of outpatient psychotherapy: A stage-sequential pattern analysis of change in session reports. Clinical Psychology & Psychotherapy, 22, 1–14.
Salloum, A., & Overstreet, S. (2012). Grief and trauma intervention for children after disaster: Exploring coping skills versus trauma narration. Behaviour Research and Therapy, 50, 169–179. https://doi.org/10.1016/j.brat.2012.01.001.
Salloum, A., Wang, W., Robst, J., Murphy, T. K., Scheeringa, M. S., Cohen, J. A., et al. (2016). Stepped care versus standard trauma-focused cognitive behavioral therapy for young children. Journal of Child Psychology and Psychiatry, 57, 614–622.
Sanchez, A. L., Cornacchio, D., Poznanski, B., Golik, A. M., Chou, T., & Comer, J. S. (2018). The effectiveness of school-based mental health services for elementary-aged children: A meta-analysis. Journal of the American Academy of Child and Adolescent Psychiatry, 57, 153–165.
Santiago, C. D., Raviv, T., Ros, A. M., Brewer, S. K., Distel, L. M. L., Torres, S. A., et al. (2018). Implementing the Bounce Back trauma intervention in urban elementary schools: A real world replication trial. School Psychology Quarterly, 33, 1–9.
Schwartz, A. C., Bradley, R. L., Sexton, M., Sherry, A., & Ressler, K. J. (2005). Posttraumatic stress disorder among African Americans in an inner city mental health clinic. Psychiatric Services, 56, 212–215. https://doi.org/10.1176/appi.ps.56.2.212.
Steinberg, A. M., Brymer, M., Decker, K., & Pynoos, R. S. (2004). The University of California at Los Angeles post-traumatic stress disorder reaction index. Current Psychiatry Reports, 6, 96–100.
Steinberg, A. M., Brymer, M. J., Kim, S., Ghosh, C., Ostrowski, S. A., Gulley, K., et al. (2013). Psychometric properties of the UCLA PTSD Reaction Index: Part I. Journal of Traumatic Stress, 26, 1–9.
Stirman, S. W., Calloway, M. A., Toder, M. K., Miller, M. C. J., DeVito, M. A. K., Meisel, M. S. N., et al. (2013). Modifications to cognitive therapy by community mental health providers: Implications for effectiveness and sustainability. Psychiatric Services, 64, 1–6.
Tarrier, N., Liversidge, T., & Gregg, L. (2006). The acceptability and preference for the psychological treatment of PTSD. Behaviour Research and Therapy, 44, 1643–1656.
van Minnen, A., Hendriks, L., & Olff, M. (2010). When do trauma experts choose exposure therapy for PTSD patients? A controlled study of therapist and patient factors. Behaviour Research and Therapy, 48, 312–320.
Wamser-Nanney, R., Scheeringa, M. S., & Weems, C. F. (2016). Early treatment response in children and adolescents receiving CBT for trauma. Journal of Pediatric Psychology, 41, 128–137.
Weisz, J. R., Chorpita, B. F., Frye, A., Ng, M. Y., Lau, N., Bearman, S. K., et al. (2011). Youth Top Problems: using idiographic, consumer-guided assessment to identify treatment needs and to track change during psychotherapy. Journal of consulting and clinical psychology, 79, 369–380.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
We would also like to acknowledge the contributions of our research assistants at West Chester University of Pennsylvania and University of Delaware, our collaborators within the Red Clay Consolidated School District, and, most importantly, our participants whose perseverance inspires us. A Delaware Department of Education Grant to the Red Clay Consolidated School District funded this work.
Rights and permissions
About this article
Cite this article
Grassetti, S.N., Haut, B., Beveridge, R.M. et al. When Do Posttraumatic Stress and Related Problems Abate During School-Based Group Therapy for Elementary Students?. School Mental Health 12, 689–702 (2020). https://doi.org/10.1007/s12310-020-09377-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12310-020-09377-8