Abstract
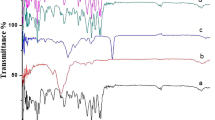
Isradipine (ISDP) is an effective calcium channel blocker used in the treatment of hypertension. It undergoes extensive first pass metabolism and bioavailability through the oral route is only about 15 to 24%. Hence we attempted to develop a matrix type controlled transdermal drug delivery system for ISDP. Formulations A1, A2, A3 were composed of Eudragit RL100 and hydroxypropyl methyl cellulose (HPMC) in 1:3, 1:1, 3:1 ratios; A4, A5, A6 were composed of Eudragit RS100 and HPMC in 1:3, 1:1, 3:1 ratios. All six formulations carried 5 mg of ISDP/patch area, 5% v/w of D-limonene, 15 % v/w of propylene glycol in methanol:dichloromethane (1:1). The physicochemical compatibility of the drug and the polymers was studied by infrared spectroscopy and differential scanning calorimetry. The results suggested no physicochemical incompatibility between the drug and the polymers. The prepared transdermal drug delivery system were evaluated for physicochemical characteristics, mainly in vitro release and ex vivo permeation. The ex vivo permeation studies were carried out across excised rat skin using Franz diffusion cell. All the formulations exhibited satisfactory physicochemical characteristics. Cumulative amount of the drug released in 36 h from the six formulations were 1695.32, 1527.89, 1455.54, 1485.65, 1282.81 and 916.88 μg/cm2 respectively. Corresponding values for the cumulative amounts of drug permeated across the rat skin for the above matrix films were 1456.29, 1284.70, 1182.99, 1212.72, 1046.05, and 782.60 μg/cm2 respectively. By fitting the data into zero order, first order and Higuchi models, it was concluded that drug release from matrix films followed Higuchi model and the mechanism of drug release was diffusion mediated. Based on the physical evaluation, in vitro drug release and ex vivo permeation characteristics, it was concluded that for potential therapeutic use, monolithic drug matrix films A1, may be suitable for the development of a transdermal drug delivery system of ISDP.
Similar content being viewed by others
References
Al-Saidan, S. M., Krishnaiah, Y. S. R., Chandrasekhar, D. V., Lalla, J. K., Rama, B., Jayaram, B., and Bhaskar, P., Formulation of an HPMC gel drug reservoir system with ethanol-water as a solvent system and limonene as a penetration enhancer for enhancing in vitro transdermal delivery of nicorandil. Skin Pharmacol. Physiol., 17, 310–320 (2004).
Arora, P. and Mukherjee, B., Design, development, physicochemical and in vitro and in vivo evaluation of transdermal patches containing diclofenac diethylammonium salt. J. Pharm. Sci., 91, 2076–2089 (2002).
Barry, B. W., Penetration enhancers: Dermatological formulations. Marcel Dekker, New York, pp. 160–172, (1983).
Barry, B. W., Novel mechanisms and devices to enable successful transdermal drug delivery. Eur. J. Pharm. Sci., 14, 101–114 (2001).
Bodmeier, R. and Paeratakul, O., Drug release from laminated polymeric films prepared from aqueous latexes. J. Pharm. Sci., 79, 32–36 (1990).
Costa, P. and Lobo, J. M. S., Modeling and comparison of dissolution profiles. Eur. J. Pharm. Sci., 13, 123–133 (2001).
El-Kattan, A. F., Asbill, C. S., Kim, N., and Michniak, B. B., The effects of terpene enhancers on the percutaneous permeation of drugs with different lipophilicities. Int. J. Pharm., 215, 229–240 (2001).
Gao, S. and Singh, J., In vitro percutaneous absorption enhancement of a lipophilic drug tamoxifen by terpenes. J. Control. Release, 51, 193–199 (1998).
Gupta, R. and Mukherjee, B., Development and in vitro evaluation of diltiazem hydrochloride transdermal patches based on povidone-ethyl cellulose matrices. Drug Dev. Ind. Pharm., 29, 1–7 (2003).
Hayton, W. L. and Chen, T., Correction of perfusate concentration for sample removal. J. Pharm. Sci., 71, 820–821 (1982).
Ho, H. O., Huang, F. C., Sokolaski, T. D., and Sheu, M. T., The influence of cosolvents on the in-vitro percutaneous penetration of diclofenac sodium from a gel system. J. Pharm. Pharmacol., 46, 636–642 (1994).
Krishnaiah, Y. S. R., Bhaskar, P., and Satyanarayana, V., In vitro percutaneous permeability enhancement of nimodipine by limonene across the excised rat abdominal skin. Pharmazie, 59, 942–947 (2004).
Kusum Devi, V., Saisivum, S., Maria, G. R., and Deepti, P. U., Design and evaluation of matrix diffusion controlled transdermal patches of verapamil hydrochloride. Drug Dev. Ind. Pharm., 29, 495–503 (2003).
Mamatha, T., Venkateswara, Rao, J., Mukkanti, K., and Ramesh, G., Transdermal drug delivery system for atomoxetine hydrochloride-in vitro and ex vivo evaluation. Curr. Trends Biotechnol. Pharm., 3, 188–196 (2009).
Moffat, A. C., David, O., and Brian, W., Clarke’s Analysis of Drugs and Poisons. Third Edition, Pharmaceutical Press, Great Britain, (2005).
Monti, D., Chetoni, P., Burgalassi, S., Najarro, M., Saettone, M. F., and Boldrini, E., Effect of different terpenecontaining essential oils on permeation of estradiol through hairless mouse skin. Int. J. Pharm., 237, 209–214 (2002).
Moser, K., Kriwet, K., Naik, A., Kalia, Y. N., and Guy, R. H., Passive skin penetration enhancement and its quantification in vitro. Eur. J. Pharm. Biopharm., 52, 103–112 (2001).
Mutalic, S. and Udupa, N., Glibenclamide transdermal patches: physicochemical, pharmacodynamic, and pharmacokinetic evaluations. J. Pharm. Sci., 93, 1577–1594 (2004).
Nair, V. B. and Panchagnula, R., The effect of pretreatment with terpenes on transdermal iontophoretic delivery of arginine vasopressin. Farmaco, 59, 575–581 (2004).
Nishihata, T., Kamada, A., Sakai, K., Takahashi, K., Matsumoto, K., Shinozaki, K., Tabata, Y., Keigami, M., Miyagi, T., and Tatsumi, N., Percutaneous absorption of diclofenac in rats and humans: aqueous gel formulation. Int. J. Pharm., 46, 1–7 (1988).
Okabe, H., Takayama, K., Ogura, A., and Nagai, T., Effect of limonene and related compounds on the percutaneous absorption of indomethacin. Drug Des. Deliv., 4, 313–321 (1989).
Okabe, H., Obata, Y., Takayama, K., and Nagai, T., Percutaneous absorption enhancing effect and skin irritation of monocyclic monoterpenes. Drug Des. Deliv., 6, 229–238 (1990).
Ota, Y., Hamada, A., Nakano, M., and Saito, H., Evaluation of percutaneous absorption of midazolam by terpenes. Drug Metab. Pharmacokinet., 18, 261–266 (2003).
Parsaee, S., Sarbolouki, M. N., and Parnianpour, M., In vitro release of diclofenac diethylammonium from lipid-based formulations. Int. J. Pharm., 241, 185–190 (2002).
Rao, P. R. and Diwan, P. V., Formulation and in vitro evaluation of polymeric films of diltiazem hydrochloride and indomethacin for transdermal administration. Drug Dev. Ind. Pharm., 24, 327–336 (1998).
Santoyo, S., Arellano, A., Ygartua, P., and Martin, C., Penetration enhancer effects on the in vitro percutaneous absorption of piroxicam through rat skin. Int. J. Pharm., 117, 219–224 (1995).
Suwanpiodokkul, N., Thongnopnua, P., and Umprayan, K., Transdermal delivery of zidovidine (AZT): The effects of vehicles, enhancers, and polymer membranes on permeation across cadaver pig skin. AAPS PharmSciTech, 5, e48 (2004).
Sweetman, S. C., The Complete Drug Reference. Martindale 34th edi, Pharmaceutical Press, London, pp. 942, (2005).
Tokudome, Y. and Sugibayashi, K., The synergic effects of various electrolytes and electroporation on the in vitro skin permeation of calcein. J. Control. Release, 92, 93–101 (2003).
Wade, A. and Weller, P. J., Handbook of Pharmaceutical Excipients. American Pharmaceutical Publishing Association, Washington: DC, pp. 252–255, 401–406 (2000).
Williams, A. C. and Barry, B. W., Terpenes and lipid-protein-partitioning theory of skin penetration enhancement. Pharm. Res., 8, 17–24 (1991).
Zhao, K. and Singh, J., In vitro percutaneous absorption enhancement of propranolol hydrochloride through porcine epidermis by terpenes/ethanol. J. Control. Release, 62, 359–366 (1999).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tirunagari, M., Jangala, V.R., Khagga, M. et al. Transdermal therapeutic system of isradipine: Effect of hydrophilic and hydrophobic matrix on In Vitro and Ex vivo characteristics. Arch. Pharm. Res. 33, 1025–1033 (2010). https://doi.org/10.1007/s12272-010-0708-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12272-010-0708-1