Abstract
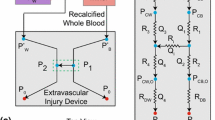
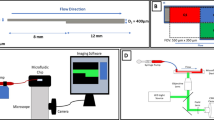
Thrombus growth at the site of vascular injury is mediated by the sequential events of platelet recruitment, activation and aggregation concomitant with the initiation of the coagulation cascade, resulting in local thrombin generation and fibrin formation. While the biorheology of a localized thrombus formation has been well studied, it is unclear whether local sites of thrombin generation propagate platelet activation within the bloodstream. In order to study the physical biology of platelet activation downstream of sites of thrombus formation, we developed a platform to measure platelet activation and microaggregate formation in the bloodstream. Our results show that thrombi formed on collagen and tissue factor promote activation and aggregation of platelets in the bloodstream in a convection-dependent manner. Pharmacological inhibition of the coagulation factors (F) X, XI or thrombin dramatically reduced the degree of distal platelet activation and microaggregate formation in the bloodstream without affecting the degree of local platelet deposition and aggregation on a surface of immobilized collagen. Herein we describe the development and an example of the utility of a platform to study platelet activation and microaggregate formation in the bloodstream (convection-limited regime) relative to the local site of thrombus formation.







Similar content being viewed by others
Abbreviations
- BSA:
-
Bovine serum albumin
- PBS:
-
Phosphate buffered saline
- DIC:
-
Differential interference contrast
- FACS:
-
Fluorescence activated cell sorting
- FX:
-
Coagulation factor X
- FXI:
-
Coagulation factor XI
- Da:
-
Dahmköhler number
References
Abulencia, J. P., N. Tien, O. J. McCarty, D. Plymire, S. A. Mousa, and K. Konstantopoulos. Comparative antiplatelet efficacy of a novel, nonpeptide GPIIb/IIIa antagonist (XV454) and abciximab (c7E3) in flow models of thrombosis. Arterioscler. Thromb. Vasc. Biol. 21:149–156, 2001.
Andrews, R. K., and M. C. Berndt. Platelet physiology and thrombosis. Thromb. Res. 114:447–453, 2004.
Baker, S. M., K. G. Phillips, and O. J. T. McCarty. Development of a label-free imaging technique for the quantification of thrombus formation. Cell. Mol. Bioeng. 5:488–492, 2012.
Baker-Groberg, S. M., F. A. Cianchetti, K. G. Phillips, and O. J. McCarty. Development of a method to quantify platelet adhesion and aggregation under static conditions. Cell. Mol. Bioeng. 7:285–290, 2014.
Chang, J. Y. Thrombin specificity. Requirement for apolar amino acids adjacent to the thrombin cleavage site of polypeptide substrate. Eur. J. Biochem. 151:217–224, 1985.
Cheng, Q., et al. A role for factor XIIa–mediated factor XI activation in thrombus formation in vivo. Blood 116:3981–3989, 2010.
Fogelson, A. L., and K. B. Neeves. Fluid mechanics of blood clot formation. Annu. Rev. Fluid Mech. 47:377–403, 2015.
Goodeve, A. C., A. Pavlova, and J. Oldenburg. Genomics of bleeding disorders. Haemoph. Off. J. World Fed. Hemoph. 20(Suppl 4):50–53, 2014.
Hathcock, J. J. Flow effects on coagulation and thrombosis. Arterioscler. Thromb. Vasc. Biol. 26:1729–1737, 2006.
Itakura, A., et al. Activated factor XI inhibits chemotaxis of polymorphonuclear leukocytes. J. Leukoc. Biol. 90:923–927, 2011.
Jones, C. M., et al. Measurement science in the circulatory system. Cell. Mol. Bioeng. 7:1–14, 2014.
Jonnalagadda, D., L. T. Izu, and S. W. Whiteheart. Platelet secretion is kinetically heterogeneous in an agonist-responsive manner. Blood 120:5209–5216, 2012.
Kravtsov, D. V., et al. Factor XI contributes to thrombin generation in the absence of factor XII. Blood 114:452–458, 2009.
Lee, A. M., G. W. Tormoen, E. Kanso, O. J. McCarty, and P. K. Newton. Modeling and simulation of procoagulant circulating tumor cells in flow. Front. Oncol. 2:108, 2012.
McCarty, O. J., J. P. Abulencia, S. A. Mousa, and K. Konstantopoulos. Evaluation of platelet antagonists in in vitro flow models of thrombosis. Methods Mol. Med. 93:21–34, 2004.
McCarty, O. J., et al. Dimensional analysis and scaling relevant to flow models of thrombus formation: communication from the SSC of the ISTH. J. Thromb. Haemost. 14:619–622, 2016.
Mousa, S. A., J. P. Abulencia, O. J. McCarty, N. A. Turner, and K. Konstantopoulos. Comparative efficacy between the glycoprotein IIb/IIIa antagonists roxifiban and orbofiban in inhibiting platelet responses in flow models of thrombosis. J. Cardiovasc. Pharmacol. 39:552–560, 2002.
Puy, C., et al. Factor XII promotes blood coagulation independent of factor XI in the presence of long-chain polyphosphates. J. Thromb. Haemost. 11:1341–1352, 2013.
Roehrig, S., et al. Discovery of the novel antithrombotic agent 5-chloro-N-({(5S)-2-oxo-3- [4-(3-oxomorpholin-4-yl)phenyl]-1,3-oxazolidin-5-yl}methyl)thiophene- 2-carboxamide (BAY 59-7939): an oral, direct factor Xa inhibitor. J. Med. Chem. 48:5900–5908, 2005.
Samuel, M., R. A. Pixley, M. A. Villanueva, R. W. Colman, and G. B. Villanueva. Human factor XII (Hageman factor) autoactivation by dextran sulfate. Circular dichroism, fluorescence, and ultraviolet difference spectroscopic studies. J. Biol. Chem. 267:19691–19697, 1992.
Tormoen, G. W., S. Rugonyi, A. Gruber, and O. J. McCarty. The role of carrier number on the procoagulant activity of tissue factor in blood and plasma. Phys. Biol. 8:066005, 2011.
White-Adams, T. C., et al. Laminin promotes coagulation and thrombus formation in a factor XII-dependent manner. J. Thromb. Haemost. 8:1295–1301, 2010.
Zilberman-Rudenko, J., et al. Coagulation factor XI promotes distal platelet activation and single platelet consumption in the bloodstream under shear flow. Arterioscler. Thromb. Vasc. Biol. 36:510–517, 2016.
Acknowledgements
We thank Cristina Puy for insightful comments and Kevin Phillips for technical assistance. This work was supported by grants from the National Institutes of Health (R01HL101972 and R01GM116184) and the Oregon Health and Science University School of Medicine MD/PhD program. O.J.T. McCarty is an American Heart Association Established Investigator (13EIA12630000). A.I. is a Bayer International Fellow and S.M.B. is a Whitaker International Fellow.
Conflict of interest
R. Vetter and C. Gerdes are employees of Bayer Pharma AG. A. Gruber, E.I. Tucker, and Oregon Health & Science University have a significant financial interest in Aronora Inc., a company that may have a commercial interest in the results of this research. This potential conflict of interest has been reviewed and managed by the Oregon Health & Science University Conflict of Interest in Research Committee. J. Zilberman-Rudenko, A. Itakura, J. Maddala, S.M. Baker-Groberg and O.J.T. McCarty declare no competing financial interests.
Ethical Standards
All human subject research was carried out in accordance with institutional guidelines approved by the Oregon Health & Science University Institutional Review Board. No animal studies were carried out by the authors for this article.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Michael R. King oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Zilberman-Rudenko, J., Itakura, A., Maddala, J. et al. Biorheology of Platelet Activation in the Bloodstream Distal to Thrombus Formation. Cel. Mol. Bioeng. 9, 496–508 (2016). https://doi.org/10.1007/s12195-016-0448-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12195-016-0448-5