Abstract
Hematopoietic stem cells are a remarkable resource currently used for the life saving treatment, hematopoietic stem cell transplantation. Today, hematopoietic stem cells are primarily obtained from mobilized peripheral blood following treatment of the donor with the cytokine G-CSF, and in some settings, chemotherapy and/or the CXCR4 antagonist plerixafor. The collection of hematopoietic stem cells is contingent on adequate and timely mobilization of these cells into the peripheral blood. The use of healthy donors, particularly when unrelated to the patient, requires mobilization strategies be safe for the donor. While current mobilization strategies are largely successful, adequate mobilization fails to occur in a significant portion of donors. Understanding the mechanisms involved in the egress of stem cells from the bone marrow provides opportunities to further improve the process of collecting hematopoietic stem cells. Here, the role extracellular components of the blood and bone marrow in the mobilization process are discussed.
Similar content being viewed by others
Introduction
Hematopoietic stem cell transplantation (HSCT) is a life saving therapeutic modality used to treat a range of malignant and genetic conditions, the most common being hematological malignancies. While historically bone marrow was collected for HSCT, today, hematopoietic stem cells (HSC) are most commonly harvested from the peripheral blood following mobilization with G-CSF, although bone marrow is still preferred in some settings [1]. Less commonly, and often as a result of the lack of a suitable donor, cord blood may be used [2].
HSC and their progenitors (HSPC) are retained within the bone marrow in specific niches where proliferation and survival are closely regulated (reviewed in [3, 4]). Considerable information regarding the nature of the HSC niche has been obtained over the last two decades, but the precise makeup remains undefined. HSC exit the bone marrow and travel through the circulation only rarely under resting conditions; however, a range of physiological and pharmacological factors can increase the number of circulating HSPC [5–8]. G-CSF is by far the most commonly used agent for the mobilization of HSPC for transplantation. In the autologous setting, various chemotherapy regimens are used in conjunction with G-CSF and increasingly the CXCR4 antagonist plerixafor (reviewed in [9]). In addition, numerous agents from various chemical classes, including other cytokines, such as GM-CSF, SCF, Groβ, IL8, and sulphated glycans, such as fucoidan, hormones, such as parathyroid hormone, and neurotransmitters, such as norepinephrine, are known to mobilize HSPC [10–13]. Although the mechanisms involved are not identical [14], key features appear to be common. Discussion in this review has been limited to mobilizing agents currently used clinically.
CXCL12
CXCL12 is the best-characterized factor involved in the retention of HSC in the bone marrow. It is a member of the CXC chemokine family that binds two receptors, CXCR4 and CXCR7 (reviewed in [15]). Of these, CXCR4 plays the predominant role in HSC biology [16]. HSC are highly responsive to CXCL12 which is arguably the most potent naturally occurring chemoattractant for these cells [17], inducing directed (chemotaxis) but not random (chemokinesis) movement [18]. CXCL12 enhances HSPC adhesion to both cellular (e.g., VCAM-1) and matrix components (e.g., fibronectin) via activation of integrins [19]. HSC proliferation is also regulated by CXCL12 in a manner that is affected by the micro-environment [20, 21]. CXCL12 is produced by a number of micro-environmental cells, including CXCL12-abundant reticular (CAR) cells [22], nestin+ cells [23], cells of the osteoid lineage [24], arteriolar pericytes [25], and endothelial cells [26]. Once produced, CXCL12 may be bound to matrix components, including fibronectin [27], collagen IV [28], and heparan sulfate [29] expressed within the niche [30, 31] potentially refining the activity of this chemokine. Therefore, CXCL12 has the potential to facilitate the retention of HSC in multiple niches within the bone marrow.
The role of CXCL12 in controlling HSPC interactions with the bone marrow niche was first reported by Lapidot et al. [32], and then definitely demonstrated by Foudi and co-workers [33] using mice chimeric for CXCR4−/− HSC. These mice have dramatically increased numbers of circulating HSC. Pharmacological disruption of CXCL12 binding to its receptor rapidly mobilizes HSC into the circulation in mice and humans [34–36]. This finding has resulted in the introduction of pharmacological antagonists of CXCR4 being developed for HSPC mobilization, with the lead compound plerixafor (AMD3100) now used in clinical practice in combination with other standard mobilization protocols, most commonly G-CSF.
Disruption of CXCL12 binding to CXCR4 is a common feature of mobilization strategies, occurring in G-CSF, Flt-3L, SCF, LECT2, plerixafor, and chemotherapy-driven mechanisms [36–38]. The importance of the loss of CXCL12/CXCR4 interactions in G-CSF-mediated mobilization is highlighted by the complete absence of G-CSF induced mobilization in CXCR4−/− bone marrow chimeric mice [37]. CXCL12 protein concentrations and mRNA expression within the bone marrow are dramatically reduced during mobilization by G-CSF or chemotherapy [36, 39, 40]. This profound reduction in bone marrow appears to result in the reversal of the CXCL12 gradient between the blood and bone marrow providing a potential gradient to facilitate the egress of HSC [39]. However, in humans, the expression of the essential amino-terminal region of CXCR4 on HSPC is cleaved by proteases rendering the cells at least temporarily unresponsive to CXCL12 [36]. Although demonstrated in mice, evidence to show increased plasma CXCL12 levels during mobilization with G-CSF or plerixafor in humans is lacking [41]. Interestingly, the chemotactic activity of plasma from autologous stem cell donors is increased at the time of leukapheresis following chemotherapy and G-CSF [42]. While this activity was CXCR4-dependent, CXCL12 plasma concentrations pre- and post-mobilization were not examined. The previous studies failed to detect an increase in total plasma CXCL12 in similarly patients [41]. Furthermore, the CXCL12 in the plasma was largely degraded into inactive forms [42]. Despite lacking chemotactic activity, some of the truncated forms induced HSPC mobilization when injected retro-orbitally in mice. It has been proposed that this relates to competition for proteoglycan binding. While reduced CXCL12 activity in the bone marrow is clearly important for HSPC mobilization, whether increased plasma concentrations play requires further confirmation in humans.
Proteases
During cytokine and chemotherapy-induced HSC mobilization, the dramatic reduction in CXCL12 protein concentration in the bone marrow is thought to be mediated, at least in part, by proteolytic degradation of the chemokine. A number of active proteases, including neutrophil elastase, cathepsin G, matrix metalloproteinase (MMP)-9, MMP14, and plasmin, are increased in the bone marrow following G-CSF or chemotherapy administration, largely secondary to the dramatic increase in maturing myeloid cells [43–45]. Furthermore, endogenous protease inhibitors, such as serpin A1 and serpin A3, are significantly reduced in the bone marrow following G-CSF administration [46] resulting in a highly proteolytic environment. In addition to cleaving and inactivating CXCL12 [36], bone marrow proteases also cleave other molecules thought to be involved in HSC retention in the bone marrow. Perhaps, the most prominent of these are adhesion molecules important for the retention of HSC, including CD44 and VCAM-1, and the cytokine receptor c-kit (Table 1) [45, 47, 48].
However, despite the clear evidence of increased protease activity during mobilization and the ability of these enzymes to cleave chemokine and adhesive targets, the identity of the proteases involved in HSC mobilization remains to be defined. Conflicting data regarding the role individual proteases has been obtained. Perhaps, the most notable surrounds the role of MMP-9 in G-CSF induced mobilization with different groups obtaining opposing results using MMP-9 null mice [49–51], while a study in rhesus monkeys showed a partial inhibition of IL-8-induced mobilization using antibodies directed against MMP-9 [52]. Perhaps, unexpectedly, the CXCL12 degradation product produced by MMP-9 was not detected in the plasma of mobilized patients, while those of neutrophil elastase, cathepsin G, and CD26 were abundant [42]. The use of serine protease deficient mice failed to demonstrate any effect on G-CSF-induced HSC mobilization, even in the presence of a broad-spectrum matrix metalloproteinase inhibitor [51]. Of note, cleavage of VCAM-1 was completely inhibited in this study, suggesting that loss of VCAM-1 function is sufficient [53] but not essential for HSC mobilization. In contrast, CXCL12 was still degraded in the absence of cathepsin G and neutrophil elastase. Considering the large number of proteases capable of cleaving and inactivating CXCL12 (Table 1), this is, perhaps, not surprising.
Of the remaining potential proteases, CD26 is a high priority candidate. Mice lacking CD26 [54] and those treated with CD26 inhibitors, such as Diprotin A [55], demonstrated reduced progenitor cell mobilization, although definitive studies on transplantable HSC remain to be published. Furthermore, CD26 deficient mice still significantly mobilized progenitors in response to G-CSF, suggesting that other factors are involved in the process. It is possible that the above-discussed serine and metalloproteinases are responsible for the CD26-independent mobilization.
Other candidate proteases include carboxypeptidase M and carboxypeptidase N. Carboxypeptidase N, which cleaves the carboxy-terminal lysine from CXCL12, has been shown to be largely responsible for the reduced activity of this chemokine in the peripheral blood [56], but there is no evidence to suggest that this liver produced enzyme is regulated by G-CSF or other mobilizing agents. In contrast, carboxypeptidase M, which similarly cleaves the carboxy-terminal lysine of CXCL12, is located on the cell surface of hematopoietic cells. Furthermore, it is upregulated by G-CSF [57] placing it in the right location and with appropriate regulation, making it a candidate for involvement in HSC mobilization. Whether carboxypeptidase M plays a significant role in the process remains to be demonstrated.
While plasmin does not directly cleave CXCL12, it can degrade a number of factors with potential roles in HSPC mobilization, including extracellular matrix proteins [58] and components of the complement cascade [59], as well as activate MMPs [60], which can, in turn, cleave CXCL12. Deletion of plasminogen impairs mobilization [44] and this appears to be at least partially dependent on reduced MMP-9 activation [61]. Increasing the activity of the fibrinolytic pathway enhanced G-CSF-mediated HSPC mobilization, although increasing MMP-9 concentrations failed to replicate this effect leaving the underlying mechanism uncertain [62]. Plasmin is also thought to cleave membrane bound uPAR [44], releasing soluble fragments into the circulation [63]. These soluble uPAR-derived peptides are chemotactic for HSPC, and antagonize the response of HSPC cells to CXCL12 [63]. When injected into mice, uPAR-derived peptides induced progenitor cell mobilization [64]. Whether plasmin and the fibrinolytic pathway play a role in G-CSF-induced mobilization remains to be determined. Interestingly, fibrinolysis was also activated when plerixafor was the mobilizing agent [65].
It has also been proposed that the coagulation pathway, in particular thrombin, may play a role in HSPC mobilization. Although thrombin can induce HSPC mobilization in mice [66], whether it is involved in G-CSF, chemotherapy or plerixafor-mediated mobilization is not clear with G-CSF making small but significant increases in some pro-thrombotic features while reducing others [67].
S1P
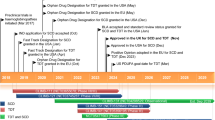
Sphingosine 1-phosphate (S1P) is a bioactive lipid produced by two enzymes, sphingosine kinase 1 and 2. There are five G-protein coupled receptors for S1P, S1P1–S1P5, of which S1P1 plays the dominant role on HSC [86, 87]. S1P is a chemoattractant for many hematopoietic cell types, including HSC, and exists in a gradient between the bone marrow, where concentrations are kept low by degradative enzymes, such as sphingosine lyase [88], and the peripheral blood [89]. The concentration of S1P in resting plasma is sufficient for it to provide a suitable chemo-attractive gradient to facilitate HSC egress. While mechanisms for increasing plasma S1P during mobilization have been demonstrated in mice and primates [90, 91], S1P plasma concentrations are not significantly changed in humans during CXCR4 antagonist or G-CSF-induced mobilization [41]. Regardless of whether plasma S1P is modulated during mobilization, this lipid is ideally position to provide a gradient that could be used to actively direct HSC out of the marrow into the peripheral circulation (Fig. 1).
Schematic diagram showing the role of S1P in CXCR4 antagonist-mediated mobilization. Under resting conditions, CXCL12 strongly attracts and retains HSPC in the bone marrow, while the effect of S1P in the blood is relatively weak. A CXCR4 antagonist blocks the ability of HSPC to detect CXCL12, the attraction to the bone marrow is lost/reduced and HSPC now responds to the S1P present in the blood, facilitating entry into the circulation. The need for increased S1P in the blood and the involvement of S1P in G-CSF-mediated mobilization are not clear
HSC mobilization by CXCR4 antagonists is diminished in settings where the S1P gradient is compromised by raising bone marrow S1P concentrations or reducing plasma S1P concentrations [41, 90, 91]. Furthermore, internalization of the receptor S1P1 rendering HSPC insensitive to exogenous S1P, also inhibits mobilization by CXCR4 antagonists. Together, this provides a strong case for the involvement of S1P in HSC mobilization by CXCR4 antagonists. Whether exaggeration of the S1P gradient using an S1P mimetic, such as SEW2871, during plerixafor-induced mobilization is clinically feasible with currently available agents is unlikely. While one study demonstrated a further increase in the mobilization of progenitors and transplantable HSC [41] another showed at best an insignificant trend only for phenotypic HSC [92]. The disparity between these studies could be due to differences in the route of drug administration with intravenous injection being used in the first, while an intra-peritoneal route was used in the latter study. FTY720 and most new generation S1P1 agonists induce bradycardia [93] that may not be tolerated when administered acutely by the intravenous route. Furthermore, an S1P1 antagonist, W146, was found to enhance plerixafor-mediated mobilization of progenitors and phenotypic HSC. A mechanism to explain this observation was not provided by the authors.
The involvement of S1P in G-CSF-mediated mobilization is less clear. Inhibition of the S1P receptor S1P1 by FTY-720 was unable to modulate G-CSF-induced mobilization in two studies [41, 94], while another found an inhibitory effect using this same antagonist [91]. Furthermore, this same study showed reduced mobilization in sphingosine kinase 1 and S1P1-deficient mice, which have reduced plasma S1P concentrations and HSPC unable to respond to S1P, respectively. Further work is required to determine the role of S1P in G-CSF-mediated HSPC mobilization.
SNS neurotransmitters
Various stresses are known to increase the number of circulating HSPC [95, 96]. While G-CSF directly acts on myeloid progenitor cells to expand granulocyte numbers resulting in a proteolytic environment, the other key cellular feature of mobilization, the reduction in osteoblasts cannot be a direct consequence of G-CSF as these cells lack the G-CSF receptor [13]. The mediators of this effect are thought to be adrenergic neurotransmitters released from the sympathetic nervous system. At present, the focus is on norepinephrine (aka noradrenalin), which is synthesized and released by sympathetic neurones. G-CSF receptors are expressed on peripheral sympathetic neurons [13, 97], suggesting that these cells can respond directly to G-CSF. Perhaps, surprisingly, G-CSF does not induce the release of norepinephrine, but rather inhibits reuptake resulting in higher concentrations remaining in the tissues [98]. A role for norepinephrine in HSPC mobilization is supported by experiments showing mobilization in mice injected with norepinephrine [65, 99]. Norepinephrine acts on niche cells, including osteoblasts, nestin+ mesenchymal cells, and endothelial cells via binding adrenergic receptors. This results in reduced synthesis of niche retention factors, including CXCL12, SCF and VCAM1, by osteoblasts and mesenchymal cells [13, 23, 100]. However, in endothelial cells, norepinephrine increases CXCL12 production [65, 101]. Norepinephrine also likely acts on bone marrow macrophages as they express the appropriate receptors and are known to respond to adrenergic stimulation [102]. In addition to effects on micro-environmental elements, norepinephrine has been reported to have chemotactic effects on HSPC [99]. However, humans treated with either noradrenalin reuptake inhibitors or β-receptor blockers mobilize with equivalent efficiency as untreated donors [103]. This suggests that there could be differences between the human and murine systems, or alternatively that the long-term administration of these agents for chronic conditions may result in adaptive changes that counter the effect. Whether norepinephrine or related compounds play a role in the mobilization of human HSPC awaits further investigation.
Recently, another neurotransmitter has been implicated in HSPC mobilization. Mice lacking neuropeptide Y have impaired mobilization in response to various mediators, including G-CSF, plerixafor and the chemotherapeutic agent 5 fluoro-uracil. Receptors for neuropeptide Y are expressed by a number of bone marrow micro-environmental cells, including stromal cells, osteoblasts, and endothelial cells [104, 105]. Intravenous injection of neuropeptide Y in mice rapidly (less than 1 h) mobilized HSC and was associated with a small but significant reduction in CXCL12 concentrations in the bone marrow and reciprocal increase in the peripheral blood. Reduced gene expression of osteoblast, but not nestin+ MSC-derived HSC retention factors was also observed in neuropeptide Y treated mice. Mice lacking the neuropeptide Y receptor, Y1, in osteoblasts failed to mobilize in response to exogenous neuropeptide Y. However, in vitro treatment of culture-induced osteoblasts with neuropeptide Y could required 3 days rather than the less than 60 min observed in vivo to reduce the expression of retention factors, suggesting that other factors may be involved. Perhaps, surprisingly, an antibody to MMP9 blocked the effects of neuropeptide Y on the expression of bone marrow retention factors. Since MMP9 is unlikely to directly modulate gene expression, it appears that the change in gene expression depends on altered osteoblast behaviour secondary to MMP9-mediated changes to the micro-environment. Since MMP9 can degrade many micro-environmental factors, the mechanism remains unclear. The source of neuropeptide Y has not been firmly established. Although it is produced by sympathetic neurones [106], other bone marrow cells, including myeloid cells and bone marrow-derived macrophages, [107] also synthesize neuropeptide Y.
Compliment cascade
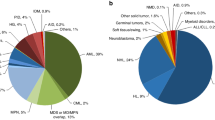
The complement cascade is part of the innate immune system, facilitating the clearance of microbes and damaged cells by antibodies and phagocytic cells (see [108] for an overview). Consisting of a number of small proteins that are sequentially recruited, it can be activated in response to antibody-binding antigen on a surface, recognition of sugars present on microbes, or binding of C3 convertase, generated from spontaneously hydrolysed C3, to a cell that lacks mammalian protective proteins (Fig. 2). The complement system can be activated in the bone marrow in response to damage by for example radiation or cytotoxic agents, or by mobilizing agents, such as G-CSF [109–111]. How the complement system regulates mobilization is complex and not entirely clear. C5-deficient mice have impaired G-CSF and plerixafor-induced mobilization [111, 112], suggesting that the stable active form of C5, desArgC5a, plays a positive role in HSC mobilization. Indeed, the concentration of desArgC5a in plasma weakly correlates with mobilized CD34+ counts in donors [113]. However, desArgC5a does not directly interact with HSC as these cells lack the receptor but instead activates mature granulocytes [112]. In this model, G-CSF- or plerixaphor-activated granulocytes migrate into bone marrow sinusoids where released proteases cleave and activate additional C5. Increased desArgC5a, which is a chemoattractant for granulocytes, encourages the egress of additional granulocytes from the extravascular compartment into sinusoids, theoretically clearing the way for the HSPC.
Potential effects of the complement, fibrinolysis, and coagulation pathways in HSPC mobilization. Increased C3 activation is seen in the bone marrow during G-CSF mobilization. Several potential explanations for this have been provided (activation of the classical, lectin, or alternative pathways or cleavage of C3 by plasmin). Activation further downstream by C5 convertase activity could be provided by C5 convertase from the complement pathway, or by plasmin, thrombin, or neutrophil elastase. Plasmin also has the potential to inhibit the complement cascade by degrading and inactivating C3b and C5b. Note that for clarity, not all components of all pathways have been shown
Downstream components of the complement cascade, C5b-C9, also known as the membrane attack complex (MAC) lyse red blood cells [90, 91]. Since red blood cells contain high concentrations of S1P [114], this is thought to elevate plasma S1P concentrations, augmenting the egress-promoting gradient between the blood and marrow. Although increased S1P has been shown in mice [90], this has not been demonstrated in humans despite reduced RBC numbers [41], although it is possible that the timing of sampling may not have optimal as the window where S1P is elevated is narrow in mice.
In contrast to C5, which is activated in the plasma, C3 is activated by cleavage in the bone marrow during G-CSF-induced mobilization [111]. Activated C3 (C3a) interacts directly with HSC, increasing chemotactic responses to CXCL12 [115] and antagonising G-CSF-mediated mobilization [116]. Consistently, C3-deficient mice mobilize HSPC very efficiently when administered G-CSF. This contrasts with the poor mobilization seen in C5-deficient mice and demonstrates opposing effects of different components of the complement cascade.
The mechanism by which the complement cascade is activated during G-CSF or plerixafor-mediated mobilization is not certain. Some immunoglobulin-deficient mice (Rag2, SCID, Jh) are poor mobilizers [111], but others are not (Rag1, IL7Ra) [13]. Exogenous immunoglobulins can enhance mobilization and this is associated with the activation of C3 and to a lesser extent C5, but an essential role for immunoglobulins has not yet been shown [111]. It has recently been reported that there is crosstalk between the complement cascade and the fibrinolysis and coagulation cascades to further enhance HSPC mobilization [117]. The activation of these cascades would be consistent with the drop in platelet counts seen during G-CSF-induced mobilization [41]. The primary mechanism was suggested to be via the provision of C5 convertase activity by thrombin and plasmin. Thrombin can also activate MMP2, promoting degradation of matrix components [118]; however, plasmin has been reported to inhibit the complement cascade at several levels leading to reduced red blood cell lysis [59]. It also remains possible that neutrophil elastase released from an expanded granulocyte pool could contribute to complement activation during mobilization by activating C5 [119].
Summary
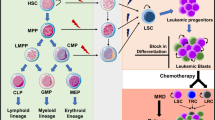
A number of extracellular components play key roles in the retention and mobilization of hematopoietic stem cells (an overview summary is provided in Fig. 3). Of these, CXCL12 is clearly the most important, but other molecules, such as S1P, proteases, and members of the complement, coagulation, and fibrinolysis pathways, appear to have roles that are remain to be fully elucidated. Manipulation of the concentrations of these molecules or targeting their cellular receptors has the potential to improve stem cell mobilization strategies in the future.
Schematic diagram for G-CSF induced mobilization of HSPC. The upper panel shows resting bone marrow and the lower panel bone marrow following G-CSF treatment. G-CSF directly results in expansion of granulocytes and a proteolytic micro-environment. G-CSF also induces the release of norepinephrine from the sympathetic nervous system. Norepinephrine contributes to the suppression the production of retentive factors (e.g., CXCL12) by micro-environmental cells, while proteases cleave proteins already present in the micro-environment, including VCAM1, CXCL12, and extracellular matric components. This permits HSPC to escape from the bone marrow. In addition activation, the complement cascade may result in formation of the membrane attack complex and red blood cell lysis. The released S1P may then provide a chemotactic gradient for HSPC, attracting them into the periphery. Further study is required to confirm the roles of S1P and the complement cascade
References
Byrne M, Savani BN, Mohty M, Nagler A. Peripheral blood stem cell versus bone marrow transplantation: a perspective from the Acute Leukemia Working Party of the European Society for Blood and Marrow Transplantation. Exp Hematol. 2016;44:567–73.
Broxmeyer HE. Enhancing the efficacy of engraftment of cord blood for hematopoietic cell transplantation. Transfus Apher Sci. 2016;54:364–72.
Calvi LM, Link DC. The hematopoietic stem cell niche in homeostasis and disease. Blood. 2015;126:2443–51.
Boulais PE, Frenette PS. Making sense of hematopoietic stem cell niches. Blood. 2015;125:2621–9.
De Lisio M, Parise G. Exercise and hematopoietic stem and progenitor cells: protection, quantity, and function. Exerc Sport Sci Rev. 2013;41:116–22.
Borlongan CV. Bone marrow stem cell mobilization in stroke: a ‘bonehead’ may be good after all! Leukemia. 2011;25:1674–86.
Wojakowski W, Landmesser U, Bachowski R, Jadczyk T, Tendera M. Mobilization of stem and progenitor cells in cardiovascular diseases. Leukemia. 2012;26:23–33.
To LB, Levesque JP, Herbert KE, Winkler IG, Bendall LJ, Hiwase DK, et al. Mobilisation strategies for normal and malignant cells. Pathology. 2011;43:547–65.
Hsu YM, Cushing MM. Autologous stem cell mobilization and collection. Hematol Oncol Clin North Am. 2016;30:573–89.
Suarez-Alvarez B, Lopez-Vazquez A, Lopez-Larrea C. Mobilization and homing of hematopoietic stem cells. Adv Exp Med Biol. 2012;741:152–70.
Laterveer L, Lindley IJ, Hamilton MS, Willemze R, Fibbe WE. Interleukin-8 induces rapid mobilization of hematopoietic stem cells with radioprotective capacity and long-term myelolymphoid repopulating ability. Blood. 1995;85:2269–75.
Sweeney EA, Priestley GV, Nakamoto B, Collins RG, Beaudet AL, Papayannopoulou T. Mobilization of stem/progenitor cells by sulfated polysaccharides does not require selectin presence. Proc Natl Acad Sci USA. 2000;97:6544–9.
Katayama Y, Battista M, Kao WM, Hidalgo A, Peired AJ, Thomas SA, et al. Signals from the sympathetic nervous system regulate hematopoietic stem cell egress from bone marrow. Cell. 2006;124:407–21.
Winkler IG, Pettit AR, Raggatt LJ, Jacobsen RN, Forristal CE, Barbier V, et al. Hematopoietic stem cell mobilizing agents G-CSF, cyclophosphamide or AMD3100 have distinct mechanisms of action on bone marrow HSC niches and bone formation. Leukemia. 2012;26:1594–601.
Nagasawa T. CXC chemokine ligand 12 (CXCL12) and its receptor CXCR4. J Mol Med (Berl). 2014;92:433–9.
Asri A, Sabour J, Atashi A, Soleimani M. Homing in hematopoietic stem cells: focus on regulatory role of CXCR7 on SDF1a/CXCR4 axis. Excli j. 2016;15:134–43.
Wright D, Bowman E, Wagers A, Butcher E, Weissman I. Hematopoietic stem cells are uniquely selective in their migratory response to chemokines. J Exp Med. 2002;195:1145–54.
Kim CH, Broxmeyer HE. In vitro behavior of hematopoietic progenitor cells under the influence of chemoattractants: stromal cell-derived factor-1, steel factor, and the bone marrow environment. Blood. 1998;91:100–10.
Peled A, Kollet O, Ponomaryov T, Petit I, Franitza S, Grabovsky V, et al. The chemokine SDF-1 activates the integrins LFA-1, VLA-4, and VLA-5 on immature human CD34(+) cells: role in transendothelial/stromal migration and engraftment of NOD/SCID mice. Blood. 2000;95:3289–96.
Cashman J, Clark-Lewis I, Eaves A, Eaves C. Stromal-derived factor 1 inhibits the cycling of very primitive human hematopoietic cells in vitro and in NOD/SCID mice. Blood. 2002;99:792–9.
Lataillade J, Clay D, Bourin P, Herodin F, Dupuy C, Jasmin C, et al. Stromal cell-derived factor 1 regulates primitive hematopoiesis by suppressing apoptosis and by promoting G(0)/G(1) transition in CD34(+) cells: evidence for an autocrine/paracrine mechanism. Blood. 2002;99:1117–29.
Sugiyama T, Kohara H, Noda M, Nagasawa T. Maintenance of the hematopoietic stem cell pool by CXCL12-CXCR4 chemokine signaling in bone marrow stromal cell niches. Immunity. 2006;25:977–88.
Mendez-Ferrer S, Michurina TV, Ferraro F, Mazloom AR, Macarthur BD, Lira SA, et al. Mesenchymal and haematopoietic stem cells form a unique bone marrow niche. Nature. 2010;466:829–34.
Ponomaryov T, Peled A, Petit I, Taichman R, Habler L, Sandbank J, et al. Induction of the chemokine stromal-derived factor-1 following DNA damage improves human stem cell function. J Clin Invest. 2000;106:1331–9.
Kunisaki Y, Bruns I, Scheiermann C, Ahmed J, Pinho S, Zhang D, et al. Arteriolar niches maintain haematopoietic stem cell quiescence. Nature. 2013;502:637–43.
Imai K, Kobayashi M, Wang J, Shinobu N, Yoshida H, Hamada J, et al. Selective secretion of chemoattractants for haemopoietic progenitor cells by bone marrow endothelial cells: a possible role in homing of haemopoietic progenitor cells to bone marrow. Br J Haematol. 1999;106:905–11.
Pelletier AJ, van der Laan LJ, Hildbrand P, Siani MA, Thompson DA, Dawson PE, et al. Presentation of chemokine SDF-1 alpha by fibronectin mediates directed migration of T cells. Blood. 2000;96:2682–90.
Yang BG, Tanaka T, Jang MH, Bai Z, Hayasaka H, Miyasaka M. Binding of lymphoid chemokines to collagen IV that accumulates in the basal lamina of high endothelial venules: its implications in lymphocyte trafficking. J Immunol. 2007;179:4376–82.
Murphy JW, Cho Y, Sachpatzidis A, Fan C, Hodsdon ME, Lolis E. Structural and functional basis of CXCL12 (stromal cell-derived factor-1 alpha) binding to heparin. J Biol Chem. 2007;282:10018–27.
Nilsson SK, Debatis ME, Dooner MS, Madri JA, Quesenberry PJ, Becker PS. Immunofluorescence characterization of key extracellular matrix proteins in murine bone marrow in situ. J Histochem Cytochem. 1998;46:371–7.
Malara A, Currao M, Gruppi C, Celesti G, Viarengo G, Buracchi C, et al. Megakaryocytes contribute to the bone marrow-matrix environment by expressing fibronectin, type IV collagen, and laminin. Stem Cells. 2014;32:926–37.
Peled A, Petit I, Kollet O, Magid M, Ponomaryov T, Byk T, et al. Dependence of human stem cell engraftment and repopulation of NOD/SCID mice on CXCR4. Science. 1999;283:845–8.
Foudi A, Jarrier P, Zhang Y, Wittner M, Geay J, Lecluse Y, et al. Reduced retention of radioprotective hematopoietic cells within the bone marrow microenvironment in CXCR4-/- chimeric mice. Blood. 2006;107:2243–51.
Liles W, Broxmeyer H, Rodger E, Wood B, Hubel K, Cooper S, et al. Mobilization of hematopoietic progenitor cells in healthy volunteers by AMD3100, a CXCR4 antagonist. Blood. 2003;102:2728–30.
Broxmeyer H, Orschell C, Clapp D, Hangoc G, Cooper S, Plett P, et al. Rapid mobilization of murine and human hematopoietic stem and progenitor cells with AMD3100, a CXCR4 antagonist. J Exp Med. 2005;201:1307–18.
Levesque J, Hendy J, Takamatsu Y, Simmons P, Bendall L. Disruption of the CXCR4/CXCL12 chemotactic interaction during hematopoietic stem cell mobilization induced by GCSF or cyclophosphamide. J Clin Invest. 2003;111:187–96.
Christopher MJ, Liu F, Hilton MJ, Long F, Link DC. Suppression of CXCL12 production by bone marrow osteoblasts is a common and critical pathway for cytokine-induced mobilization. Blood. 2009;114:1331–9.
Lu XJ, Chen Q, Rong YJ, Yang GJ, Li CH, Xu NY, et al. LECT2 drives haematopoietic stem cell expansion and mobilization via regulating the macrophages and osteolineage cells. Nat Commun. 2016;7:12719.
Petit I, Szyper-Kravitz M, Nagler A, Lahav M, Peled A, Habler L, et al. G-CSF induces stem cell mobilization by decreasing bone marrow SDF-1 and up-regulating CXCR4. Nat Immunol. 2002;3:687–94.
Semerad CL, Christopher MJ, Liu F, Short B, Simmons PJ, Winkler I, et al. G-CSF potently inhibits osteoblast activity and CXCL12 mRNA expression in the bone marrow. Blood. 2005;106:3020–7.
Juarez JG, Harun N, Thien M, Welschinger R, Baraz R, Dela Pena A, et al. Sphingosine-1-phosphate facilitates trafficking of hematopoietic stem cells and their mobilization by CXCR4 antagonists in mice. Blood. 2012;119:707–16.
Richter R, Jochheim-Richter A, Ciuculescu F, Kollar K, Seifried E, Forssmann U, et al. Identification and characterization of circulating variants of CXCL12 from human plasma: effects on chemotaxis and mobilization of hematopoietic stem and progenitor cells. Stem Cells Dev. 2014;23:1959–74.
Levesque JP, Hendy J, Takamatsu Y, Williams B, Winkler IG, Simmons PJ. Mobilization by either cyclophosphamide or granulocyte colony-stimulating factor transforms the bone marrow into a highly proteolytic environment. Exp Hematol. 2002;30:440–9.
Tjwa M, Sidenius N, Moura R, Jansen S, Theunissen K, Andolfo A, et al. Membrane-anchored uPAR regulates the proliferation, marrow pool size, engraftment, and mobilization of mouse hematopoietic stem/progenitor cells. J Clin Invest. 2009;119:1008–18.
Vagima Y, Avigdor A, Goichberg P, Shivtiel S, Tesio M, Kalinkovich A, et al. MT1-MMP and RECK are involved in human CD34 + progenitor cell retention, egress, and mobilization. J Clin Invest. 2009;119:492–503.
Winkler IG, Hendy J, Coughlin P, Horvath A, Levesque JP. Serine protease inhibitors serpina1 and serpina3 are down-regulated in bone marrow during hematopoietic progenitor mobilization. J Exp Med. 2005;201:1077–88.
Levesque J, Takamatsu Y, Nilsson S, Haylock D, Simmons P. Vascular cell adhesion molecule-1 (CD106) is cleaved by neutrophil proteases in the bone marrow following hematopoietic progenitor cell mobilization by granulocyte colony-stimulating factor. Blood. 2001;98:1289–97.
Papayannopoulou T, Craddock C, Nakamoto B, Priestley GV, Wolf NS. The VLA4/VCAM-1 adhesion pathway defines contrasting mechanisms of lodgement of transplanted murine hemopoietic progenitors between bone marrow and spleen. Proc Natl Acad Sci USA. 1995;92:9647–51.
Heissig B, Hattori K, Dias S, Friedrich M, Ferris B, Hackett N, et al. Recruitment of stem and progenitor cells from the bone marrow niche requires MMP-9 mediated release of kit-ligand. Cell. 2002;109:625–37.
Papayannopoulou T, Priestley GV, Bonig H, Nakamoto B. The role of G-protein signaling in hematopoietic stem/progenitor cell mobilization. Blood. 2003;101:4739–47.
Levesque JP, Liu F, Simmons PJ, Betsuyaku T, Senior RM, Pham C, et al. Characterization of hematopoietic progenitor mobilization in protease-deficient mice. Blood. 2004;104:65–72.
Pruijt JF, Fibbe WE, Laterveer L, Pieters RA, Lindley IJ, Paemen L, et al. Prevention of interleukin-8-induced mobilization of hematopoietic progenitor cells in rhesus monkeys by inhibitory antibodies against the metalloproteinase gelatinase B (MMP-9). Proc Natl Acad Sci U S A. 1999;96:10863–8.
Craddock CF, Nakamoto B, Andrews RG, Priestley GV, Papayannopoulou T. Antibodies to VLA4 integrin mobilize long-term repopulating cells and augment cytokine-induced mobilization in primates and mice. Blood. 1997;90:4779–88.
Christopherson KW, Cooper S, Hangoc G, Broxmeyer HE. CD26 is essential for normal G-CSF-induced progenitor cell mobilization as determined by CD26−/− mice. Exp Hematol. 2003;31:1126–34.
Christopherson KW 2nd, Cooper S, Broxmeyer HE. Cell surface peptidase CD26/DPPIV mediates G-CSF mobilization of mouse progenitor cells. Blood. 2003;101:4680–6.
Davis DA, Singer KE, De La Luz Sierra M, Narazaki M, Yang F, Fales HM, et al. Identification of carboxypeptidase N as an enzyme responsible for C-terminal cleavage of stromal cell-derived factor-1alpha in the circulation. Blood. 2005;105:4561–8.
Marquez-Curtis L, Jalili A, Deiteren K, Shirvaikar N, Lambeir AM, Janowska-Wieczorek A. Carboxypeptidase M expressed by human bone marrow cells cleaves the C-terminal lysine of stromal cell-derived factor-1alpha: another player in hematopoietic stem/progenitor cell mobilization? Stem Cells. 2008;26:1211–20.
Bonnefoy A, Legrand C. Proteolysis of subendothelial adhesive glycoproteins (fibronectin, thrombospondin, and von Willebrand factor) by plasmin, leukocyte cathepsin G, and elastase. Thromb Res. 2000;98:323–32.
Barthel D, Schindler S, Zipfel PF. Plasminogen is a complement inhibitor. J Biol Chem. 2012;287:18831–42.
Baramova EN, Bajou K, Remacle A, L’Hoir C, Krell HW, Weidle UH, et al. Involvement of PA/plasmin system in the processing of pro-MMP-9 and in the second step of pro-MMP-2 activation. FEBS Lett. 1997;405:157–62.
Gong Y, Fan Y, Hoover-Plow J. Plasminogen regulates stromal cell-derived factor-1/CXCR4-mediated hematopoietic stem cell mobilization by activation of matrix metalloproteinase-9. Arterioscler Thromb Vasc Biol. 2011;31:2035–43.
Tjwa M, Janssens S, Carmeliet P. Plasmin therapy enhances mobilization of HPCs after G-CSF. Blood. 2008;112:4048–50.
Selleri C, Montuori N, Ricci P, Visconte V, Carriero MV, Sidenius N, et al. Involvement of the urokinase-type plasminogen activator receptor in hematopoietic stem cell mobilization. Blood. 2005;105:2198–205.
Selleri C, Montuori N, Ricci P, Visconte V, Baiano A, Carriero MV, et al. In vivo activity of the cleaved form of soluble urokinase receptor: a new hematopoietic stem/progenitor cell mobilizer. Cancer Res. 2006;66:10885–90.
Dar A, Schajnovitz A, Lapid K, Kalinkovich A, Itkin T, Ludin A, et al. Rapid mobilization of hematopoietic progenitors by AMD3100 and catecholamines is mediated by CXCR4-dependent SDF-1 release from bone marrow stromal cells. Leukemia. 2011;25:1286–96.
Gur-Cohen S, Itkin T, Chakrabarty S, Graf C, Kollet O, Ludin A, et al. PAR1 signaling regulates the retention and recruitment of EPCR-expressing bone marrow hematopoietic stem cells. Nat Med. 2015;21:1307–17.
LeBlanc R, Roy J, Demers C, Vu L, Cantin G. A prospective study of G-CSF effects on hemostasis in allogeneic blood stem cell donors. Bone Marrow Transplant. 1999;23:991–6.
Kollet O, Dar A, Shivtiel S, Kalinkovich A, Lapid K, Sztainberg Y, et al. Osteoclasts degrade endosteal components and promote mobilization of hematopoietic progenitor cells. Nat Med. 2006;12:657–64.
Proost P, Struyf S, Schols D, Durinx C, Wuyts A, Lenaerts JP, et al. Processing by CD26/dipeptidyl-peptidase IV reduces the chemotactic and anti-HIV-1 activity of stromal-cell-derived factor-1alpha. FEBS Lett. 1998;432:73–6.
McQuibban G, Butler G, Gong J, Bendall L, Power C, Clark-Lewis I, et al. Matrix metalloproteinase activity inactivates the CXC chemokine stromal cell-derived factor-1. J Biol Chem. 2001;276:43503–8.
Levesque J, Hendy J, Winkler I, Takamatsu Y, Simmons P. Granulocyte colony-stimulating factor induces the release in the bone marrow of proteases that cleave c-KIT receptor (CD117) from the surface of hematopoietic progenitor cells. Exp Hematol. 2003;31:109–17.
Cruz AC, Frank BT, Edwards ST, Dazin PF, Peschon JJ, Fang KC. Tumor necrosis factor-alpha-converting enzyme controls surface expression of c-Kit and survival of embryonic stem cell-derived mast cells. J Biol Chem. 2004;279:5612–20.
Garton KJ, Gough PJ, Philalay J, Wille PT, Blobel CP, Whitehead RH, et al. Stimulated shedding of vascular cell adhesion molecule 1 (VCAM-1) is mediated by tumor necrosis factor-alpha-converting enzyme (ADAM 17). J Biol Chem. 2003;278:37459–64.
Chetty C, Vanamala SK, Gondi CS, Dinh DH, Gujrati M, Rao JS. MMP-9 induces CD44 cleavage and CD44 mediated cell migration in glioblastoma xenograft cells. Cell Signal. 2012;24:549–59.
Mori H, Tomari T, Koshikawa N, Kajita M, Itoh Y, Sato H, et al. CD44 directs membrane-type 1 matrix metalloproteinase to lamellipodia by associating with its hemopexin-like domain. EMBO J. 2002;21:3949–59.
Kryczka J, Stasiak M, Dziki L, Mik M, Dziki A, Cierniewski C. Matrix metalloproteinase-2 cleavage of the beta1 integrin ectodomain facilitates colon cancer cell motility. J Biol Chem. 2012;287:36556–66.
Bermpohl F, Loster K, Reutter W, Baum O. Rat dipeptidyl peptidase IV (DPP IV) exhibits endopeptidase activity with specificity for denatured fibrillar collagens. FEBS Lett. 1998;428:152–6.
Bossard MJ, Tomaszek TA, Thompson SK, Amegadzie BY, Hanning CR, Jones C, et al. Proteolytic activity of human osteoclast cathepsin K. Expression, purification, activation, and substrate identification. J Biol Chem. 1996;271:12517–24.
Christiansen VJ, Jackson KW, Lee KN, McKee PA. Effect of fibroblast activation protein and alpha2-antiplasmin cleaving enzyme on collagen types I, III, and IV. Arch Biochem Biophys. 2007;457:177–86.
Shapiro SD. Matrix metalloproteinase degradation of extracellular matrix: biological consequences. Curr Opin Cell Biol. 1998;10:602–8.
Ohuchi E, Imai K, Fujii Y, Sato H, Seiki M, Okada Y. Membrane type 1 matrix metalloproteinase digests interstitial collagens and other extracellular matrix macromolecules. J Biol Chem. 1997;272:2446–51.
Knauper V, Cowell S, Smith B, Lopez-Otin C, O’Shea M, Morris H, et al. The role of the C-terminal domain of human collagenase-3 (MMP-13) in the activation of procollagenase-3, substrate specificity, and tissue inhibitor of metalloproteinase interaction. J Biol Chem. 1997;272:7608–16.
Latijnhouwers MA, Bergers M, Veenhuis RT, Beekman B, Ankersmit-Ter Horst MF, Schalkwijk J. Tenascin-C degradation in chronic wounds is dependent on serine proteinase activity. Arch Dermatol Res. 1998;290:490–6.
Didangelos A, Yin X, Mandal K, Saje A, Smith A, Xu Q, et al. Extracellular matrix composition and remodeling in human abdominal aortic aneurysms: a proteomics approach. Mol Cell Proteomics. 2011;10(M111):008128.
Gueders MM, Hirst SJ, Quesada-Calvo F, Paulissen G, Hacha J, Gilles C, et al. Matrix metalloproteinase-19 deficiency promotes tenascin-C accumulation and allergen-induced airway inflammation. Am J Respir Cell Mol Biol. 2010;43:286–95.
Rivera J, Proia R, Olivera A. The alliance of sphingosine-1-phosphate and its receptors in immunity. Nat Rev Immunol. 2008;8:753–63.
Rosen H, Gonzalez-Cabrera PJ, Sanna MG, Brown S. Sphingosine 1-phosphate receptor signaling. Annu Rev Biochem. 2009;78:743–68.
Rosen H, Goetzl EJ. Sphingosine 1-phosphate and its receptors: an autocrine and paracrine network. Nat Rev Immunol. 2005;5:560–70.
Bendall LJ, Basnett J. Role of sphingosine 1-phosphate in trafficking and mobilization of hematopoietic stem cells. Curr Opin Hematol. 2013;20:281–8.
Ratajczak MZ, Lee H, Wysoczynski M, Wan W, Marlicz W, Laughlin MJ, et al. Novel insight into stem cell mobilization-plasma sphingosine-1-phosphate is a major chemoattractant that directs the egress of hematopoietic stem progenitor cells from the bone marrow and its level in peripheral blood increases during mobilization due to activation of complement cascade/membrane attack complex. Leukemia. 2010;24:976–85.
Golan K, Vagima Y, Ludin A, Itkin T, Cohen-Gur S, Kalinkovich A, et al. S1P promotes murine progenitor cell egress and mobilization via S1P1-mediated ROS signaling and SDF-1 release. Blood. 2012;119:2478–88.
Liu J, Zhao J, Lee JF, Gartung A, Jawadi H, Zhang W, et al. 3-amino-4-(3-hexylphenylamino)-4-oxobutyl phosphonic acid (W146), a Selective Antagonist of Sphingosine-1-phospahte Receptor Subtype 1, Enhances AMD3100-stimulated Mobilization of Hematopoietic Stem Progenitor Cells in Animals. J Biochem Pharmacol Res. 2013;1:197–203.
Guerrero M, Urbano M, Roberts E. Sphingosine 1-phosphate receptor 1 agonists: a patent review (2013–2015). Expert Opin Ther Pat. 2016;26:455–70.
Massberg S, Schaerli P, Knezevic-Maramica I, Köllnberger M, Tubo N, Moseman E, et al. Immunosurveillance by hematopoietic progenitor cells trafficking through blood, lymph, and peripheral tissues. Cell. 2007;131:994–1008.
Barrett AJ, Longhurst P, Sneath P, Watson JG. Mobilization of CFU-C by exercise and ACTH induced stress in man. Exp Hematol. 1978;6:590–4.
Shah S, Ulm J, Sifri ZC, Mohr AM, Livingston DH. Mobilization of bone marrow cells to the site of injury is necessary for wound healing. J Trauma. 2009;67:315–21 (discussion 21-2).
Schneider A, Kruger C, Steigleder T, Weber D, Pitzer C, Laage R, et al. The hematopoietic factor G-CSF is a neuronal ligand that counteracts programmed cell death and drives neurogenesis. J Clin Invest. 2005;115:2083–98.
Lucas D, Bruns I, Battista M, Mendez-Ferrer S, Magnon C, Kunisaki Y, et al. Norepinephrine reuptake inhibition promotes mobilization in mice: potential impact to rescue low stem cell yields. Blood. 2012;119:3962–5.
Spiegel A, Shivtiel S, Kalinkovich A, Ludin A, Netzer N, Goichberg P, et al. Catecholaminergic neurotransmitters regulate migration and repopulation of immature human CD34+ cells through Wnt signaling. Nat Immunol. 2007;8:1123–31.
Mendez-Ferrer S, Battista M, Frenette PS. Cooperation of beta(2)- and beta(3)-adrenergic receptors in hematopoietic progenitor cell mobilization. Ann N Y Acad Sci. 2010;1192:139–44.
Wu B, Wang L, Yang X, Mao M, Ye C, Liu P, et al. Norepinephrine inhibits mesenchymal stem cell chemotaxis migration by increasing stromal cell-derived factor-1 secretion by vascular endothelial cells via NE/abrd3/JNK pathway. Exp Cell Res. 2016;. doi:10.1016/j.yexcr.2016.09.007.
Xiang M, Yuan Y, Fan L, Li Y, Li A, Yin L, et al. Role of macrophages in mobilization of hematopoietic progenitor cells from bone marrow after hemorrhagic shock. Shock. 2012;37:518–23.
Bonig H, Papayannopoulou T. Hematopoietic stem cell mobilization: updated conceptual renditions. Leukemia. 2013;27:24–31.
Movafagh S, Hobson JP, Spiegel S, Kleinman HK, Zukowska Z. Neuropeptide Y induces migration, proliferation, and tube formation of endothelial cells bimodally via Y1, Y2, and Y5 receptors. Faseb j. 2006;20:1924–6.
Lundberg P, Allison SJ, Lee NJ, Baldock PA, Brouard N, Rost S, et al. Greater bone formation of Y2 knockout mice is associated with increased osteoprogenitor numbers and altered Y1 receptor expression. J Biol Chem. 2007;282:19082–91.
Zukowska-Grojec Z, Neuropeptide Y. A novel sympathetic stress hormone and more. Ann N Y Acad Sci. 1995;771:219–33.
Singer K, Morris DL, Oatmen KE, Wang T, DelProposto J, Mergian T, et al. Neuropeptide Y is produced by adipose tissue macrophages and regulates obesity-induced inflammation. PLoS One. 2013;8:e57929.
Travers P, Walport M, Janeway CJ. Innate Immunity: The first lines of defense. In: Murphy K, editor. Immunobiology: the immune system in health and disease. London and New York: Garland Science; 2012. p. 37–72.
Surace L, Lysenko V, Fontana AO, Cecconi V, Janssen H, Bicvic A, et al. Complement is a central mediator of radiotherapy-induced tumor-specific immunity and clinical response. Immunity. 2015;42:767–77.
Michlmayr A, Bachleitner-Hofmann T, Baumann S, Marchetti-Deschmann M, Rech-Weichselbraun I, Burghuber C, et al. Modulation of plasma complement by the initial dose of epirubicin/docetaxel therapy in breast cancer and its predictive value. Br J Cancer. 2010;103:1201–8.
Reca R, Cramer D, Yan J, Laughlin MJ, Janowska-Wieczorek A, Ratajczak J, et al. A novel role of complement in mobilization: immunodeficient mice are poor granulocyte-colony stimulating factor mobilizers because they lack complement-activating immunoglobulins. Stem Cells. 2007;25:3093–100.
Lee HM, Wysoczynski M, Liu R, Shin DM, Kucia M, Botto M, et al. Mobilization studies in complement-deficient mice reveal that optimal AMD3100 mobilization of hematopoietic stem cells depends on complement cascade activation by AMD3100-stimulated granulocytes. Leukemia. 2009;24:573–82.
Jalili A, Shirvaikar N, Marquez-Curtis L, Qiu Y, Korol C, Lee H, et al. Fifth complement cascade protein (C5) cleavage fragments disrupt the SDF-1/CXCR4 axis: further evidence that innate immunity orchestrates the mobilization of hematopoietic stem/progenitor cells. Exp Hematol. 2010;38:321–32.
Hanel P, Andreani P, Graler MH. Erythrocytes store and release sphingosine 1-phosphate in blood. FASEB J. 2007;21:1202–9.
Reca R, Mastellos D, Majka M, Marquez L, Ratajczak J, Franchini S, et al. Functional receptor for C3a anaphylatoxin is expressed by normal hematopoietic stem/progenitor cells, and C3a enhances their homing-related responses to SDF-1. Blood. 2003;101:3784–93.
Ratajczak J, Reca R, Kucia M, Majka M, Allendorf DJ, Baran JT, et al. Mobilization studies in mice deficient in either C3 or C3a receptor (C3aR) reveal a novel role for complement in retention of hematopoietic stem/progenitor cells in bone marrow. Blood. 2004;103:2071–8.
Borkowska S, Suszynska M, Mierzejewska K, Ismail A, Budkowska M, Salata D, et al. Novel evidence that crosstalk between the complement, coagulation and fibrinolysis proteolytic cascades is involved in mobilization of hematopoietic stem/progenitor cells (HSPCs). Leukemia. 2014;28:2148–54.
Koo BH, Park MY, Jeon OH, Kim DS. Regulatory mechanism of matrix metalloprotease-2 enzymatic activity by factor Xa and thrombin. J Biol Chem. 2009;284:23375–85.
Vogt W. Cleavage of the fifth component of complement and generation of a functionally active C5b6-like complex by human leukocyte elastase. Immunobiology. 2000;201:470–7.
Acknowledgements
Funding was provided by National Health and Medical Research Council (Grant No. 1042305).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author has no conflicts to declare.
About this article
Cite this article
Bendall, L. Extracellular molecules in hematopoietic stem cell mobilisation. Int J Hematol 105, 118–128 (2017). https://doi.org/10.1007/s12185-016-2123-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-016-2123-y