Abstract
Mesenchymal stem/stromal cells (MSCs) have the potential to form colonies in culture and reside in adult tissues. Because MSCs have been defined using cells cultured in vitro, discrepancies have arisen between studies concerning their properties. There are also differences between populations obtained using different isolation methods. This review article focuses on recent developments in the identification of novel MSC markers for the in vivo localization and prospective isolation of human MSCs. The prospective isolation method described in this study represents an important strategy for the isolation of MSCs in a short period of time, and may find applications for regenerative medicine. Purified MSCs can be tailored according to their intended clinical therapeutic applications. Lineage tracing methods define the MSC phenotype and can be used to investigate the physiological roles of MSCs in vivo. These findings may facilitate the development of effective stem cell treatments.
Similar content being viewed by others
Introduction
Stem cells derived from human somatic tissue are used in the treatment of a variety of diseases and injuries. Somatic stem cells exhibit tissue organization and contribute to homeostasis in multiple organs. The most popular cell source is bone marrow (BM) stem cells, which consist of hematopoietic stem cells (HSCs) and mesenchymal stem/stromal cells (MSCs). HSCs are present in the BM niche in a state of quiescence [1–3]. MSCs reside in the non-hematopoietic fraction and can be cultured to form fibroblast-like colonies (colony-forming unit fibroblasts: CFU-Fs) in vitro [4–7]. MSCs are found in the BM [8, 9], umbilical cord blood [10, 11], placenta [12, 13], dental pulp [14, 15], adipose tissue [16–19], and synovium [20–22]. BM-MSCs are thought to function in the maintenance of BM homeostasis, restoration of injured bone, and regulation of differentiation in HSCs [23]. The definition of MSCs depends on in vitro culture conditions, and thus varies among researchers in the stem cell field. In general, MSC refers to adherent cultured cells that can differentiate into bone, fat, and cartilage [24]. However, adherent culture conditions on plastic dishes inevitably change the expression of surface markers and the biological properties of stem cells [25, 26]. Indeed, most MSC marker information is obtained from cultured MSCs [27], which makes it difficult to identify MSC-specific markers and analyze physiological functions in vivo.
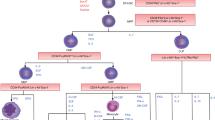
Recently, a number of studies have addressed such problems using flow cytometry and transgenic mouse (Fig. 1). Tissues are dissected or crushed to make them physically small, and the pieces of tissue are incubated for a few hours in the presence of enzymes that degrade the matrix component of tissues. It is common to use a collagenase reagent to acquire cells from tissue samples. However, obtaining different populations depends on the collagenase concentration and treatment time. In tissues containing red blood cells, the enzyme-treated cells are resuspended in water or lysis buffer to remove the red blood cells. At this stage, the cell population is heterogeneous (see enzymatic treatment in Fig. 1). In the case of the BM, whole BM cell populations may contain various mature cells, such as fat cells, macrophages, endothelial cells, blood cells, and fibroblasts. Stem cell-specific markers are needed to isolate tissue stem cells from these heterogeneous cell populations. The cells are stained with a stem cell-specific monoclonal antibody on ice (see surface marker in Fig. 1). In mouse tissue, stem cells are prospectively isolated and identified according to fluorescence generated by tissue-specific-promoter-Cre/Floxed reporter mice (see specific reporter in Fig. 1). Stem cell-specific markers can be used to obtain uniform MSCs and trace cell fate in vivo.
Prospective isolation methods for MSCs from multiple tissues. Traditional MSC isolation uses adherent cultures on the dish (left). Prospective identification of MSCs using flow cytometric identification of cell surface markers (center) and transgenic mouse expressing tissue-specific reporters allows the isolation of a pure population of multipotent MSCs (right)
MSCs are defined as self-renewing populations in multiple organs
MSCs are selected based on adherent potency in culture conditions containing fetal bovine serum. Friedenstein and others reported the existence of MSCs by CFU-F in the BM [4, 5, 28, 29]. Pittenger confirmed that MSCs have multipotency for adipocytes, chondrocytes, and osteoblasts, clonally [24]. Thereafter, a large number of studies correlated MSC phenotypic features and investigated the therapeutic potential of MSCs. Elahi et al. reported that the term “mesenchymal stem cell” yielded more than 357,000 hits in Google Scholar (Google Scholar; July 2015) [30]. Colony-forming cells have since been called “mesenchymal stem cells” or “mesenchymal stromal cells.” It appears that the term “stem cell” has become more popular than the term “stromal cell” in the last 20 years in MSCs studies. Interestingly, “stemness” has been shown to be a stricter term for MSCs involved in tissue repair (Fig. 2) [30]. Recently, “skeletal stem cells (SSCs)” has supplanted the term “tissue stem cells” as the new term for these cells [31, 32]. A web search showed that the term “skeletal stem cell(s)” yielded more than 46 hits in article titles in November 2015. SSCs self-renew and generate osteoblasts, chondrocytes, and reticular marrow stromal cells, but not adipocytes [33, 34].
Recently, many reports have demonstrated the presence of neural crest stem cells in various adult tissues, and suggested that they are present not only in embryos but also in multiple organs during adulthood [35, 36]. The neural crest is a transient embryonic tissue that originates at neural folds during vertebrate development. Neural crest cells migrate from the dorsal neural tube and migrate to various locations, where they differentiate into a vast range of cells, including neurons and glial cells of the peripheral nervous system, smooth muscle cells, bone, and cartilage cells. The characteristics of neural crest stem cells are similar to those of MSCs [37]. Cre/loxP-mediated lineage analysis also suggests that a subpopulation of adult BM-MSCs may have a developmental origin in the murine neural crest [38, 39]. Furthermore, neural crest-derived cells have been confirmed to exist in skin [40], cornea [41], and heart [42] in adult mouse. These organs may, thus, represent additional sources for the supply of MSCs. In order to avoid problems related to culture procedures, it is important to identify specific markers for MSCs to enable their rapid isolation and to define the common features of MSCs [43].
Prospective identification and isolation of human MSCs
Various surface makers have been used to isolate human MSCs (Table 1). The first isolation method used a monoclonal antibody against Stro-1 to efficiently isolate fibroblast-like cells from fresh BM [44]. The Stro-1-positive compartment includes non-hematopoietic cells, but the antibody is also reactive with red blood cells. A number of studies have examined MSC isolation using CD73-positive [45], CD49a-positive [45], CD105-positive [46], and MSCA-1-positive [47], SSEA4-positive [48, 49] populations. In 2002, a direct isolation method for MSCs was performed using an antibody against CD271 (low-affinity nerve growth factor receptor: LNGFR) [50]. LNGFR is not reactive to red blood cells and hematopoietic progenitor cells, which has made LNGFR one of the more popular markers for the isolation of human MSCs. Some studies have used the LNGFR marker in combination with MSCA-1-positive [51], CD56-positive [52, 53], CD140b-positive [54], CD146-positive/negative [55], and SSEA4-positive [56] populations. In addition, high CFU-F frequency is associated with a population double-positive for CD106 (VCAM-1) and Stro-1 antibodies [57]. These cells differentiate into bone and fat on ectopic transplantation in vivo. In 2013, our group reported that the LNGFR and THY-1 double-positive population (i.e., the LT population) have a high CFU-F frequency in the BM [8]. CFU-F can be classified into three different cell groups based on proliferation ability. Rapidly expanding MSC clones (RECs) are undifferentiated cells with proliferation and differentiation ability that are maintained during long-term subculture in vitro. RECs are highly associated with the VCAM-1hi-positive population. Aomatsu et al. recently demonstrated that the novel SCRG1/BST1 axis determines the fate of hMSCs by regulating their kinetic and differentiation potentials [58]. SCRG1/BST1 preserves self-renewal potential and the expression of stem cell markers such as LNGFR, THY-1 and VCAM-1 [58]. Cell–cell adhesion in human MSCs enhances the expression of VCAM-1 via PDGFRb [59].
Based on a study of BM-MSCs, we found that LNGFR and THY-1 markers can be used to effectively isolate these cells from other tissues. In one study, we isolated LNGFR+ THY-1+ MSCs from synovium using flow cytometry [20]. The synovium contains a higher percentage of LNGFR+ THY-1+ MSCs. We examined the colony formation and differentiation abilities of BM- and synovium-derived MSCs isolated from the same patients. Both MSC types exhibit a marked propensity to differentiate into specific lineages. BM-MSCs preferentially differentiated into bone, while in the synovium-MSC culture, we observed enhanced adipogenic and chondrogenic differentiation. In another study, we examined human dental pulp stem/progenitor cells (hDPSCs) [14]. hDPSCs are attractive candidates for regenerative therapy because they can be easily expanded to generate CFU-Fs [15, 60, 61]. We identified a dental pulp tissue-specific cell population based on the expression profiles of two cell-surface markers, LNGFR and THY-1. Prospectively isolated dental pulp-derived LNGFRLow+ THY-1High+ cells represent a highly enriched population of clonogenic cells; notably, isolated cells exhibit long-term proliferation and multilineage differentiation potential in vitro. These cells also express known mesenchymal cell markers and promote new bone formation reparative of critically sized calvarial defects in vivo. These findings suggest that LNGFRLow+ THY-1High+ dental pulp-derived cells provide an excellent source of material for bone regeneration strategies. These data suggest that the tissue from which MSCs are isolated should be tailored according to their intended clinical therapeutic application. In human MSCs, the LNGFR marker has been validated by many researchers (Table 1) [62, 63], the next step should be improved selection and characterization of human MSC populations using comprehensive analysis [64].
MSC lineage tracking in vivo
In past reports describing the use of mouse MSCs, MSCs accumulated at injury sites and released trophic factors, such as prostaglandin E2 [65], TNF-α stimulated gene/protein 6 [66–68], and soluble TNF receptor 1 [69]. It is thought that MSCs respond to inflammation and have specific roles in immune regulation, lymphopoiesis, and bone homeostasis [70, 71]. These reports used cultured MSCs; accordingly, it is unknown whether the response is similar under physiological conditions. To investigate the physiological role of MSCs in vivo, two in vivo tracing strategies can be employed (Fig. 1); one method is to transplant the purified MSCs isolated using specific surface markers [43]. We used phenotypic, morphological, and functional criteria to identify and prospectively isolate a subset of MSCs (PDGFRα+ Sca-1+ CD45− TER119−: PaS cells) from adult mouse BM [72, 73]. PaS cells mainly differentiate into fat cells in adipose tissue, hematopoiesis support cells (CAR cells) [74], and osteoblasts in the BM [73]. The other method uses lineage tracing in transgenic mice, using transcription markers such as Nestin-GFP/cre [75], Ebf2-cre [76], and LepR-cre [77]. These techniques and histologic analyses have been used to identify MSCs locally, examine cell fate, and evaluate their physiological role in vivo. The cultured MSCs are trapped in pulmonary capillaries. However, freshly isolated MSCs survive in the BM and adipose tissue [73]. In an analysis of LepR-cre and Ebf2-cre mice, the group found that MSCs participate in turnover in bone and adipose tissue in adult BM [77, 78]. Worthley and colleagues demonstrated that the expression of the bone morphogenetic protein antagonist gremlin 1 defines a population of SSCs in the BM [79]. Chan and colleagues searched for unique gene expression patterns in the transcriptome of stem/progenitor cells to identify potential regulators of mouse SSC lineage commitment [80]. Inducing SSC formation with soluble factors and subsequently regulating the SSC niche to specify its differentiation toward bone, cartilage, or stromal cells could represent a paradigm shift in the therapeutic regeneration of skeletal tissues. Additional studies are needed to clarify the physiological role of the mesenchymal (or skeletal) lineage in vivo [81].
Conclusions
Many clinical studies have been performed using MSCs. However, cultured MSCs include heterogeneous cell groups, which have an effect on therapeutic outcomes. Isolation methods should be adapted such that only true MSCs are obtained. It is extremely important to determine the physiological functions of homogeneous MSC populations directly isolated and analyzed from multiple organs.
References
Morrison SJ, Scadden DT. The bone marrow niche for haematopoietic stem cells. Nature. 2014;505:327–34.
Foudi A, Hochedlinger K, Van Buren D, Schindler JW, Jaenisch R, Carey V, et al. Analysis of histone 2B-GFP retention reveals slowly cycling hematopoietic stem cells. Nat Biotechnol. 2009;27:84–90.
Yamazaki S, Nakauchi H. Bone marrow Schwann cells induce hematopoietic stem cell hibernation. Int J Hematol. 2014;99:695–8.
Friedenstein AJ, Deriglasova UF, Kulagina NN, Panasuk AF, Rudakowa SF, Luria EA, et al. Precursors for fibroblasts in different populations of hematopoietic cells as detected by the in vitro colony assay method. Exp Hematol. 1974;2:83–92.
Piersma AH, Brockbank KG, Ploemacher RE, van Vliet E, Brakel-van Peer KM, Visser PJ. Characterization of fibroblastic stromal cells from murine bone marrow. Exp Hematol. 1985;13:237–43.
Caplan AI. Mesenchymal stem cells. J Orthop Res. 1991;9:641–50.
Kuznetsov SA, Friedenstein AJ, Robey PG. Factors required for bone marrow stromal fibroblast colony formation in vitro. Br J Haematol. 1997;97:561–70.
Mabuchi Y, Morikawa S, Harada S, Niibe K, Suzuki S, Renault-Mihara F, et al. LNGFR(+)THY-1(+)VCAM-1(hi+) Cells Reveal Functionally Distinct Subpopulations in Mesenchymal Stem Cells. Stem Cell Reports. 2013;1:152–65.
Sacchetti B, Funari A, Michienzi S, Di Cesare S, Piersanti S, Saggio I, et al. Self-renewing osteoprogenitors in bone marrow sinusoids can organize a hematopoietic microenvironment. Cell. 2007;131:324–36.
Lee OK, Kuo TK, Chen WM, Lee KD, Hsieh SL, Chen TH. Isolation of multipotent mesenchymal stem cells from umbilical cord blood. Blood. 2004;103:1669–75.
Yoshioka S, Miura Y, Iwasa M, Fujishiro A, Yao H, Miura M, et al. Isolation of mesenchymal stromal/stem cells from small-volume umbilical cord blood units that do not qualify for the banking system. Int J Hematol. 2015;102:218–29.
Battula VL, Bareiss PM, Treml S, Conrad S, Albert I, Hojak S, et al. Human placenta and bone marrow derived MSC cultured in serum-free, b-FGF-containing medium express cell surface frizzled-9 and SSEA-4 and give rise to multilineage differentiation. Differentiation. 2007;75:279–91.
Battula VL, Treml S, Abele H, Buhring HJ. Prospective isolation and characterization of mesenchymal stem cells from human placenta using a frizzled-9-specific monoclonal antibody. Differentiation. 2008;76:326–36.
Yasui T, Mabuchi Y, Toriumi H, Ebine T, Niibe K, Houlihan DD, et al. Purified Human Dental Pulp Stem Cells Promote Osteogenic Regeneration. J Dent Res (2015). doi:10.1177/0022034515610748
Gronthos S, Mankani M, Brahim J, Robey PG, Shi S. Postnatal human dental pulp stem cells (DPSCs) in vitro and in vivo. Proc Natl Acad Sci USA. 2000;97:13625–30.
Sowa Y, Imura T, Numajiri T, Takeda K, Mabuchi Y, Matsuzaki Y, et al. Adipose stromal cells contain phenotypically distinct adipogenic progenitors derived from neural crest. PLoS One. 2013;8:e84206.
Liu TM, Martina M, Hutmacher DW, Hui JH, Lee EH, Lim B. Identification of common pathways mediating differentiation of bone marrow- and adipose tissue-derived human mesenchymal stem cells into three mesenchymal lineages. Stem Cells. 2007;25:750–60.
Yanez R, Lamana ML, Garcia-Castro J, Colmenero I, Ramirez M, Bueren JA. Adipose tissue-derived mesenchymal stem cells have in vivo immunosuppressive properties applicable for the control of the graft-versus-host disease. Stem Cells. 2006;24:2582–91.
Ong WK, Tan CS, Chan KL, Goesantoso GG, Chan XH, Chan E, et al. Identification of specific cell-surface markers of adipose-derived stem cells from subcutaneous and visceral fat depots. Stem Cell Reports. 2014;2:171–9.
Ogata Y, Mabuchi Y, Yoshida M, Suto EG, Suzuki N, Muneta T, et al. Purified human synovium mesenchymal stem cells as a good resource for cartilage regeneration. PLoS One. 2015;10:e0129096.
Sakaguchi Y, Sekiya I, Yagishita K, Muneta T. Comparison of human stem cells derived from various mesenchymal tissues: superiority of synovium as a cell source. Arthritis Rheum. 2005;52:2521–9.
De Bari C, Dell’Accio F, Tylzanowski P, Luyten FP. Multipotent mesenchymal stem cells from adult human synovial membrane. Arthritis Rheum. 2001;44:1928–42.
Stappenbeck TS, Miyoshi H. The role of stromal stem cells in tissue regeneration and wound repair. Science. 2009;324:1666–9.
Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD, et al. Multilineage potential of adult human mesenchymal stem cells. Science. 1999;284:143–7.
Bianco P, Cao X, Frenette PS, Mao JJ, Robey PG, Simmons PJ, et al. The meaning, the sense and the significance: translating the science of mesenchymal stem cells into medicine. Nat Med. 2013;19:35–42.
Cai J, Miao X, Li Y, Smith C, Tsang K, Cheng L, et al. Whole-genome sequencing identifies genetic variances in culture-expanded human mesenchymal stem cells. Stem Cell Reports. 2014;3:227–33.
Bianco P, Robey PG, Simmons PJ. Mesenchymal stem cells: revisiting history, concepts, and assays. Cell Stem Cell. 2008;2:313–9.
Friedenstein AJ, Petrakova KV, Kurolesova AI, Frolova GP. Heterotopic of bone marrow. Analysis of precursor cells for osteogenic and hematopoietic tissues. Transplantation. 1968;6:230–47.
Reddi AH, Huggins CB. Formation of bone marrow in fibroblast-transformation ossicles. Proc Natl Acad Sci USA. 1975;72:2212–6.
Elahi KC, Klein G, Avci-Adali M, Sievert KD, MacNeil S, Aicher WK. Human mesenchymal stromal cells from different sources diverge in their expression of cell surface proteins and display distinct differentiation patterns. Stem Cells International (2016). doi:10.1155/2016/5646384
Kassem M, Bianco P. Skeletal stem cells in space and time. Cell. 2015;160:17–9.
Kuznetsov SA, Mankani MH, Gronthos S, Satomura K, Bianco P, Robey PG. Circulating skeletal stem cells. J Cell Biol. 2001;153:1133–40.
Bianco P, Robey PG. Skeletal stem cells. Development. 2015;142:1023–7.
Bianco P, Kuznetsov SA, Riminucci M, Gehron Robey P. Postnatal skeletal stem cells. Methods Enzymol. 2006;419:117–48.
Toma JG, Akhavan M, Fernandes KJ, Barnabe-Heider F, Sadikot A, Kaplan DR, et al. Isolation of multipotent adult stem cells from the dermis of mammalian skin. Nat Cell Biol. 2001;3:778–84.
Fernandes KJ, McKenzie IA, Mill P, Smith KM, Akhavan M, Barnabe-Heider F, et al. A dermal niche for multipotent adult skin-derived precursor cells. Nat Cell Biol. 2004;6:1082–93.
Takashima Y, Era T, Nakao K, Kondo S, Kasuga M, Smith AG, et al. Neuroepithelial cells supply an initial transient wave of MSC differentiation. Cell. 2007;129:1377–88.
Morikawa S, Mabuchi Y, Niibe K, Suzuki S, Nagoshi N, Sunabori T, et al. Development of mesenchymal stem cells partially originate from the neural crest. Biochem Biophys Res Commun. 2009;379:1114–9.
Nagoshi N, Shibata S, Kubota Y, Nakamura M, Nagai Y, Satoh E, et al. Ontogeny and multipotency of neural crest-derived stem cells in mouse bone marrow, dorsal root ganglia, and whisker pad. Cell Stem Cell. 2008;2:392–403.
Johnston AP, Naska S, Jones K, Jinno H, Kaplan DR, Miller FD. Sox2-mediated regulation of adult neural crest precursors and skin repair. Stem Cell Reports. 2013;1:38–45.
Yoshida S, Shimmura S, Nagoshi N, Fukuda K, Matsuzaki Y, Okano H, et al. Isolation of multipotent neural crest-derived stem cells from the adult mouse cornea. Stem Cells. 2006;24:2714–22.
Tomita Y, Matsumura K, Wakamatsu Y, Matsuzaki Y, Shibuya I, Kawaguchi H, et al. Cardiac neural crest cells contribute to the dormant multipotent stem cell in the mammalian heart. J Cell Biol. 2005;170:1135–46.
Mabuchi Y, Houlihan DD, Akazawa C, Okano H, Matsuzaki Y. Prospective isolation of murine and human bone marrow mesenchymal stem cells based on surface markers. Stem Cells Int. 2013;2013:507301.
Simmons PJ, Torok-Storb B. Identification of stromal cell precursors in human bone marrow by a novel monoclonal antibody, STRO-1. Blood. 1991;78:55–62.
Boiret N, Rapatel C, Veyrat-Masson R, Guillouard L, Guerin JJ, Pigeon P, et al. Characterization of non-expanded mesenchymal progenitor cells from normal adult human bone marrow. Exp Hematol. 2005;33:219–25.
Aslan H, Zilberman Y, Kandel L, Liebergall M, Oskouian RJ, Gazit D, et al. Osteogenic differentiation of non-cultured immunoisolated bone marrow-derived CD105+ cells. Stem Cells. 2006;24:1728–37.
Gronthos S, Fitter S, Diamond P, Simmons PJ, Itescu S, Zannettino AC. A novel monoclonal antibody (STRO-3) identifies an isoform of tissue non-specific alkaline phosphatase expressed by multipotent bone marrow stromal stem cells. Stem Cells Dev. 2007;16:953–63.
Gang EJ, Bosnakovski D, Figueiredo CA, Visser JW, Perlingeiro RC. SSEA-4 identifies mesenchymal stem cells from bone marrow. Blood. 2007;109:1743–51.
Trubiani O, Zalzal SF, Paganelli R, Marchisio M, Giancola R, Pizzicannella J, et al. Expression profile of the embryonic markers nanog, OCT-4, SSEA-1, SSEA-4, and frizzled-9 receptor in human periodontal ligament mesenchymal stem cells. J Cell Physiol. 2010;225:123–31.
Quirici N, Soligo D, Bossolasco P, Servida F, Lumini C, Deliliers GL. Isolation of bone marrow mesenchymal stem cells by anti-nerve growth factor receptor antibodies. Exp Hematol. 2002;30:783–91.
Sobiesiak M, Sivasubramaniyan K, Hermann C, Tan C, Orgel M, Treml S, et al. The mesenchymal stem cell antigen MSCA-1 is identical to tissue non-specific alkaline phosphatase. Stem Cells Dev. 2010;19:669–77.
Battula VL, Treml S, Bareiss PM, Gieseke F, Roelofs H, de Zwart P, et al. Isolation of functionally distinct mesenchymal stem cell subsets using antibodies against CD56, CD271, and mesenchymal stem cell antigen-1. Haematologica. 2009;94:173–84.
Mariotti E, Mirabelli P, Abate G, Schiattarella M, Martinelli P, Fortunato G, et al. Comparative characteristics of mesenchymal stem cells from human bone marrow and placenta: CD10, CD49d, and CD56 make a difference. Stem Cells Dev. 2008;17:1039–41.
Buhring HJ, Battula VL, Treml S, Schewe B, Kanz L, Vogel W. Novel markers for the prospective isolation of human MSC. Ann N Y Acad Sci. 2007;1106:262–71.
Tormin A, Li O, Brune JC, Walsh S, Schutz B, Ehinger M, et al. CD146 expression on primary non-hematopoietic bone marrow stem cells is correlated with in situ localization. Blood. 2011;117:5067–77.
Matsuoka Y, Nakatsuka R, Sumide K, Kawamura H, Takahashi M, Fujioka T, et al. Prospectively Isolated human bone marrow cell-derived MSCs support primitive human CD34-negative hematopoietic stem cells. Stem Cells. 2015;33:1554–65.
Gronthos S, Zannettino AC, Hay SJ, Shi S, Graves SE, Kortesidis A, et al. Molecular and cellular characterisation of highly purified stromal stem cells derived from human bone marrow. J Cell Sci. 2003;116:1827–35.
Aomatsu E, Takahashi N, Sawada S, Okubo N, Hasegawa T, Taira M, et al. Novel SCRG1/BST1 axis regulates self-renewal, migration, and osteogenic differentiation potential in mesenchymal stem cells. Sci Rep. 2014;4:3652.
Aomatsu E, Chosa N, Nishihira S, Sugiyama Y, Miura H, Ishisaki A. Cell-cell adhesion through N-cadherin enhances VCAM-1 expression via PDGFRbeta in a ligand-independent manner in mesenchymal stem cells. Int J Mol Med. 2014;33:565–72.
Laino G, d’Aquino R, Graziano A, Lanza V, Carinci F, Naro F, et al. A new population of human adult dental pulp stem cells: a useful source of living autologous fibrous bone tissue (LAB). J Bone Miner Res. 2005;20:1394–402.
Laino G, Carinci F, Graziano A, d’Aquino R, Lanza V, De Rosa A, et al. In vitro bone production using stem cells derived from human dental pulp. J Craniofac Surg. 2006;17:511–5.
Cuthbert RJ, Giannoudis PV, Wang XN, Nicholson L, Pawson D, Lubenko A, et al. Examining the feasibility of clinical grade CD271+ enrichment of mesenchymal stromal cells for bone regeneration. PLoS One. 2015;10:e0117855.
Alvarez-Viejo M, Menendez-Menendez Y, Otero-Hernandez J. CD271 as a marker to identify mesenchymal stem cells from diverse sources before culture. World J Stem Cells. 2015;7:470–6.
Holley RJ, Tai G, Williamson AJ, Taylor S, Cain SA, Richardson SM, et al. Comparative quantification of the surfaceome of human multipotent mesenchymal progenitor cells. Stem Cell Reports. 2015;4:473–88.
Nemeth K, Leelahavanichkul A, Yuen PS, Mayer B, Parmelee A, Doi K, et al. Bone marrow stromal cells attenuate sepsis via prostaglandin E(2)-dependent reprogramming of host macrophages to increase their interleukin-10 production. Nat Med 2009;15:42–9.
Lee RH, Pulin AA, Seo MJ, Kota DJ, Ylostalo J, Larson BL, et al. Intravenous hMSCs improve myocardial infarction in mice because cells embolized in lung are activated to secrete the anti-inflammatory protein TSG-6. Cell Stem Cell. 2009;5:54–63.
Roddy GW, Oh JY, Lee RH, Bartosh TJ, Ylostalo J, Coble K, et al. Action at a distance: systemically administered adult stem/progenitor cells (MSCs) reduce inflammatory damage to the cornea without engraftment and primarily by secretion of TNF-alpha stimulated gene/protein 6. Stem Cells. 2011;29:1572–9.
Oh JY, Roddy GW, Choi H, Lee RH, Ylostalo JH, Rosa RH Jr, et al. Anti-inflammatory protein TSG-6 reduces inflammatory damage to the cornea following chemical and mechanical injury. Proc Natl Acad Sci USA. 2010;107:16875–80.
Yagi H, Soto-Gutierrez A, Navarro-Alvarez N, Nahmias Y, Goldwasser Y, Kitagawa Y, et al. Reactive bone marrow stromal cells attenuate systemic inflammation via sTNFR1. Mol Ther. 2010;18:1857–64.
James S, Fox J, Afsari F, Lee J, Clough S, Knight C, et al. Multiparameter analysis of human bone marrow stromal cells identifies distinct immunomodulatory and differentiation-competent subtypes. Stem Cell Reports. 2015;4:1004–15.
Rodriguez R, Rosu-Myles M, Arauzo-Bravo M, Horrillo A, Pan Q, Gonzalez-Rey E, et al. Human bone marrow stromal cells lose immunosuppressive and anti-inflammatory properties upon oncogenic transformation. Stem Cell Reports. 2014;3:606–19.
Houlihan DD, Mabuchi Y, Morikawa S, Niibe K, Araki D, Suzuki S, et al. Isolation of mouse mesenchymal stem cells on the basis of expression of Sca-1 and PDGFR-alpha. Nat Protoc. 2012;7:2103–11.
Morikawa S, Mabuchi Y, Kubota Y, Nagai Y, Niibe K, Hiratsu E, et al. Prospective identification, isolation, and systemic transplantation of multipotent mesenchymal stem cells in murine bone marrow. J Exp Med. 2009;206:2483–96.
Omatsu Y, Seike M, Sugiyama T, Kume T, Nagasawa T. Foxc1 is a critical regulator of haematopoietic stem/progenitor cell niche formation. Nature. 2014;508:536–40.
Mendez-Ferrer S, Michurina TV, Ferraro F, Mazloom AR, Macarthur BD, Lira SA, et al. Mesenchymal and haematopoietic stem cells form a unique bone marrow niche. Nature. 2010;466:829–34.
Qian H, Badaloni A, Chiara F, Stjernberg J, Polisetti N, Nihlberg K, et al. Molecular characterization of prospectively isolated multipotent mesenchymal progenitors provides new insight into the cellular identity of mesenchymal stem cells in mouse bone marrow. Mol Cell Biol. 2013;33:661–77.
Zhou BO, Yue R, Murphy MM, Peyer JG, Morrison SJ. Leptin-receptor-expressing mesenchymal stromal cells represent the main source of bone formed by adult bone marrow. Cell Stem Cell. 2014;15:154–68.
Matsuzaki Y, Mabuchi Y, Okano H. Leptin receptor makes its mark on MSCs. Cell Stem Cell. 2014;15:112–4.
Worthley DL, Churchill M, Compton JT, Tailor Y, Rao M, Si Y, et al. Gremlin 1 identifies a skeletal stem cell with bone, cartilage, and reticular stromal potential. Cell. 2015;160:269–84.
Chan CK, Seo EY, Chen JY, Lo D, McArdle A, Sinha R, et al. Identification and specification of the mouse skeletal stem cell. Cell. 2015;160:285–98.
Kfoury Y, Scadden DT. Mesenchymal cell contributions to the stem cell niche. Cell Stem Cell. 2015;16:239–53.
Acknowledgments
This work was supported by Grants-in-Aid (KAKENHI, 15K06853) from the Japan Society for the Ministry of Education, Culture, Sports, Science and Technology (MEXT) (to Yo Mabuchi).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
About this article
Cite this article
Mabuchi, Y., Matsuzaki, Y. Prospective isolation of resident adult human mesenchymal stem cell population from multiple organs. Int J Hematol 103, 138–144 (2016). https://doi.org/10.1007/s12185-015-1921-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-015-1921-y