Abstract
Purpose
Neutrophil/lymphocyte ratio (NLR) and platelet/lymphocyte ratio (PLR) were immune response-related indicators. Preoperative NLR and PLR had been considered to be related to the prognosis of various cancers. The objective of this study was to evaluate the prognostic significance of NLR and PLR in patients with gallbladder carcinoma (GBC).
Methods
From 2001 to 2013, 145 patients with GBC were recruited in this retrospective study. Cutoff values of NLR and PLR were determined by receiver operating characteristic curves (ROC). The correlation of clinical data, including tumor differentiation, nevin stage, TNM stage, operation margin, operation mode, NLR, PLR, hemoglobin, C reactive protein (CRP), carcinoembryonic antigen (CEA), and carbohydrate antigen 199 (CA199) with median survival period of patients was analyzed by univariate survival analysis. The multivariate prognosis analysis was performed to select the independent prognostic factors.
Results
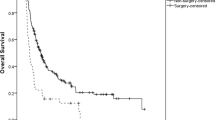
The cutoff values of NLR and PLR were 1.94 and 113.34, respectively. Compared with low NLR and low PLR group, the 5-year survival rates in high NLR and high PLR group were reduced (P < 0.05). The degree of tumor differentiation, nevin stage, TNM stage, operation mode, NLR, PLR, CA199, total bilirubin, CRP and CEA were associated with the median survival period of patients (P < 0.01). The multivariate prognosis analysis showed that NLR, nevin stage, operation mode and hemoglobin were independent prognostic factors (P < 0.05).
Conclusion
Preoperative NLR and PLR were closely related to prognosis of patients with GBC and might be useful for the evaluation of prognosis of patients with GBC.




Similar content being viewed by others
References
Liu Y, He X, Wang J, Li J, Li K, Liu F et al. Establishment of liver metastasis model of human gallbladder cancer and isolation of the subpopulation with high metastatic potential. Zhonghua yi xue za zhi. 2006;86:2117–21.
Butte JM, Matsuo K, Gönen M, D'Angelica MI, Waugh E, Allen PJ et al. Gallbladder cancer: differences in presentation, surgical treatment, and survival in patients treated at centers in three countries. J Am Coll Surg. 2011;212:50–61.
Haq N, Khan BA, Imran M, Akram A, Jamal AB, Bangash F. Frequency of gall bladder carcinoma in patients with acute and chronic cholecystitis. J Ayub Med Coll Abbottabad. 2014;26:191.
Miller G, Jarnagin W. Gallbladder carcinoma. Eur J Surg Oncol (EJSO). 2008;34:306–12.
Bartlett DL, Fong Y, Fortner JG, Brennan MF, Blumgart LH. Long-term results after resection for gallbladder cancer. Implications for staging and management. Ann Surg. 1996;224:639.
Wu XS, Shi LB, Li ML, Ding Q, Weng H, Wu WG, Cao Y, et al. Evaluation of two inflammation-based prognostic scores in patients with resectable gallbladder carcinoma. Ann Surg Oncol. 2014;21:449–57.
Kinoshita A, Onoda H, Imai N, Iwaku A, Oishi M, Tanaka K et al. The Glasgow Prognostic Score, an inflammation based prognostic score, predicts survival in patients with hepatocellular carcinoma. BMC cancer. 2013;13:52.
Azab B, Bhatt VR, Phookan J, Murukutla S, Kohn N, Terjanian T et al. Usefulness of the neutrophil-to-lymphocyte ratio in predicting short-and long-term mortality in breast cancer patients. Ann Surg Oncol. 2012;19:217–24.
Duan H, Zhang X, Wang F-X, Cai M-Y, Ma G-W, Yang H et al. Prognostic role of neutrophil-lymphocyte ratio in operable esophageal squamous cell carcinoma. World J Gastroenterol. 2015;21:5591.
Gao F, Li X, Geng M, Ye X, Liu H, Liu Y et al. Pretreatment neutrophil-lymphocyte ratio: an independent predictor of survival in patients with hepatocellular carcinoma. Medicine. 2015;94:e639.
Fan W, Zhang Y, Wang Y, Yao X, Yang J, Li J. Neutrophil-to-lymphocyte and platelet-to-lymphocyte ratios as predictors of survival and metastasis for recurrent hepatocellular carcinoma after transarterial chemoembolization. PLoS One. 2015;10.
Nevin JE, Moran TJ, Kay S, King R. Carcinoma of the gallbladder. Staging, treatment, and prognosis. Cancer. 1976;37:141–8.
Edge SB, Compton CC. The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncology. 2010;17:1471–4.
Gregory AD, Houghton AM. Tumor-associated neutrophils: new targets for cancer therapy. Cancer Res. 2011;71:2411–6.
Demers M, Krause DS, Schatzberg D, Martinod K, Voorhees JR, Fuchs TA, et al. Cancers predispose neutrophils to release extracellular DNA traps that contribute to cancer-associated thrombosis. Proc Natl Acad Sci. 2012;109:13076–81.
Dunn GP, Old LJ, Schreiber RD. The immunobiology of cancer immunosurveillance and immunoediting. Immunity. 2004;21:137–48.
Fogar P, Sperti C, Basso D, Sanzari MC, Greco E, Davoli C, et al. Decreased total lymphocyte counts in pancreatic cancer: an index of adverse outcome. Pancreas. 2006;32:22–8.
Adamek M, Kawczyk-Krupka A, Mostowy A, Czuba Z, Krol W, Kasperczyk S, Jakobisiak M, et al. Topical ALA-PDT modifies neutrophils’ chemiluminescence, lymphocytes’ interleukin-1beta secretion and serum level of transforming growth factor beta1 in patients with nonmelanoma skin malignancies: a clinical study. Photodiagnosis Photodyn Ther. 2005;2:65–72.
Templeton AJ, McNamara MG, Šeruga B, Vera-Badillo FE, Aneja P, Ocaña A et al. Prognostic role of neutrophil-to-lymphocyte ratio in solid tumors: a systematic review and meta-analysis. J Natl Cancer Inst. 2014;106:dju124.
Gay LJ, Felding-Habermann B. Contribution of platelets to tumour metastasis. Nat Rev Cancer. 2011;11:123–34.
Takagi S, Sato S, Oh-hara T, Takami M, Koike S, Mishima Y, et al. Platelets promote tumor growth and metastasis via direct interaction between Aggrus/podoplanin and CLEC-2. PLoS One. 2013;8:e73609.
Cho MS, Bottsford-Miller J, Vasquez HG, Stone R, Zand B, Kroll MH, et al. Platelets increase the proliferation of ovarian cancer cells. Blood. 2012;120:4869–72.
Asher V, Lee J, Innamaa A, Bali A. Preoperative platelet lymphocyte ratio as an independent prognostic marker in ovarian cancer. Clin Transl Oncol. 2011;13:499–503.
Templeton AJ, Ace O, McNamara MG, Al-Mubarak M, Vera-Badillo FE, Hermanns T et al. Prognostic role of platelet to lymphocyte ratio in solid tumors: a systematic review and meta-analysis. Cancer Epidemiol Biomark Prev. 2014 (cebp. 0146).
Roxburgh CS, McMillan DC. Role of systemic inflammatory response in predicting survival in patients with primary operable cancer. Future Oncol. 2010;6:149–63.
Koike Y, Miki C, Okugawa Y, Yokoe T, Toiyama Y, Tanaka K, et al. Preoperative C-reactive protein as a prognostic and therapeutic marker for colorectal cancer. J Surg Oncol. 2008;98:540–4.
Jagdev S, Gregory W, Vasudev N, Harnden P, Sim S, Thompson D, et al. Improving the accuracy of pre-operative survival prediction in renal cell carcinoma with C-reactive protein. Br J Cancer. 2010;103:1649–56.
Yokoyama Y, Ebata T, Igami T, Sugawara G, Ando M, Nagino M. Predictive power of prothrombin time and serum total bilirubin for postoperative mortality after major hepatectomy with extrahepatic bile duct resection. Surgery. 2014;155:504–11.
Nomura S, Watanabe M, Komine O, Shioya T, Toyoda T, Bou H, et al. Serum total bilirubin elevation is a predictor of the clinicopathological severity of acute appendicitis. Surg Today. 2014;44:1104–8.
Conflict of interest
All authors declare that they have no conflict of interests to state.
Ethical standards
This study was approved by hospital medical ethics committee of the Qingdao Municipal Hospital.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, Y., Jiang, C., Li, J. et al. Prognostic significance of preoperative neutrophil/lymphocyte ratio and platelet/lymphocyte ratio in patients with gallbladder carcinoma. Clin Transl Oncol 17, 810–818 (2015). https://doi.org/10.1007/s12094-015-1310-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-015-1310-2