Abstract
The therapeutic potential of purinergic signaling has been explored for a wide variety of diseases, including those related to the skin. In this study, we used the self-assembled skin substitutes (SASS), a highly functional reconstructed human skin model, which shares many properties with normal human skin, to study the impact of purinergic receptors agonists, such as ATP, UTP and a P2Y receptor antagonist, Reactive Blue 2 during wound healing. After treating the wounded skins, we evaluated the wound area, reepithelialization, length of migrating tongues toward the wound, quality of the skins through the cytokeratin 10 and laminin-5 expression, epidermal and dermal cell proliferation. In addition, the expression of the main ectoenzymes capable of hydrolyzing nucleotides were investigated through the wounded SASS regions: unwounded region, wound margin, intermediate region and migrating epidermal tongue. After 3 days, under the UTP treatment, the wounded SASS showed an increase in the reepithelialization and in the proliferation of keratinocytes and fibroblasts, without altering the quality of the skin. We also identified the presence of the ectoenzymes NTPDase1 and NPP1 in the reconstructed human skin model, suggesting their involvement in wound healing. Considering the need for new therapies capable of promoting healing in complex wounds, although these results are still preliminary, they suggest the involvement of extracellular nucleotides in human skin healing and the importance to understand their role in this mechanism. New experiments it will be necessary to determine the mechanisms by which the purinergic signaling is involved in the skin wound healing.
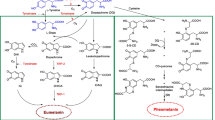
Graphical Abstract










Similar content being viewed by others
References
Abbracchio MP et al (2006) International Union of Pharmacology LVIII: update on the P2Y G protein-coupled nucleotide receptors: from molecular mechanisms and pathophysiology to therapy. Pharmacol Rev 58(3):281–341
Agorku DJ et al (2019) CD49b, CD87, and CD95 are markers for activated cancer-associated fibroblasts whereas CD39 marks quiescent normal fibroblasts in murine tumor models. Front Oncol 9:716
Anderson CM, Parkinson FE (1997) Potential signalling roles for UTP and UDP: sources, regulation and release of uracil nucleotides. Trends Pharmacol Sci 18(10):387–392
Beaudoin Cloutier C et al (2017) In vivo evaluation and imaging of a bilayered self-assembled skin substitute using a decellularized dermal matrix grafted on mice. Tissue Eng A 23(7–8):313–322
Blanpain C, Fuchs E (2006) Epidermal stem cells of the skin. Annu Rev Cell Dev Biol. https://doi.org/10.1146/annurev.cellbio.22.010305.104357
Boucher I et al (2010) The P2Y2 receptor mediates the epithelial injury response and cell migration. Am J Physiol Cell Physiol 299(2):C411–C421
Brunschweiger A, Muller C (2006) P2 receptors activated by uracil nucleotides—an update. Curr Med Chem. https://doi.org/10.2174/092986706775476052
Burnstock G (2007a) Physiology and pathophysiology of purinergic neurotransmission. Physiol Rev 87(2):659–797
Burnstock G (2007b) Purine and pyrimidine receptors. Cell Mol Life Sci CMLS 64(12):1471–1483
Burnstock G (2018) The therapeutic potential of purinergic signalling. Biochem Pharmacol. https://doi.org/10.1016/j.bcp.2017.07.016
Burnstock G, Knight GE, Greig AVH (2012a) Purinergic signaling in healthy and diseased skin. J Investig Dermatol 132(3 Pt 1):526–546
Burnstock G, Knight GE, Greig AVH (2012b) Purinergic signaling in healthy and diseased skin. J Investig Dermatol. https://doi.org/10.1038/jid.2011.344
Burrell HE et al (2003) Human keratinocytes express multiple P2Y-receptors: evidence for functional P2Y1, P2Y2, and P2Y4 receptors. J Investig Dermatol 120(3):440–447
Choudhury S, Das A (2021) Advances in generation of three-dimensional skin equivalents: pre-clinical studies to clinical therapies. Cytotherapy 23(1):1–9
Chourabi M et al (2018) ENPP1 mutation causes recessive cole disease by altering melanogenesis. J Investig Dermatol 138(2):291–300
Commandeur S et al (2009) Anin vitrothree-dimensional model of primary human cutaneous squamous cell carcinoma. Exp Dermatol. https://doi.org/10.1111/j.1600-0625.2009.00856.x
Diekmann J et al (2016) A three-dimensional skin equivalent reflecting some aspects ofin vivoaged skin. Exp Dermatol. https://doi.org/10.1111/exd.12866
Dixon CJ et al (1999) Regulation of epidermal homeostasis through P2Y2 receptors. Br J Pharmacol 127(7):1680–1686
Fausther M et al (2010) Cystic fibrosis remodels the regulation of purinergic signaling by NTPDase1 (CD39) and NTPDase3. Am J Physiol Lung Cell Mol Physiol 298(6):L804–L818
Flores-Muñoz C et al (2021) Restraint of human skin fibroblast motility, migration, and cell surface actin dynamics, by Pannexin 1 and P2X7 receptor signaling. Int J Mol Sci 22(3):7. https://doi.org/10.3390/ijms22031069
Gendaszewska-Darmach E, Kucharska M (2011) Nucleotide receptors as targets in the pharmacological enhancement of dermal wound healing. Purinergic Signal 7(2):193–206
Germain L et al (2018) Autologous bilayered self-assembled skin substitutes (SASSs) as permanent grafts: a case series of 14 severely burned patients indicating clinical effectiveness. Eur Cell Mater 36:128–141
Giuliani AL, Sarti AC, Di Virgilio F (2020) Ectonucleotidases in acute and chronic inflammation. Front Pharmacol 11:619458
Goldfine ID et al (1999) Role of PC-1 in the etiology of insulin resistance. Ann NY Acad Sci. https://doi.org/10.1111/j.1749-6632.1999.tb07797.x
Greig AVH et al (2003) Purinergic receptors are part of a functional signaling system for proliferation and differentiation of human epidermal keratinocytes. J Investig Dermatol. https://doi.org/10.1046/j.1523-1747.2003.12261.x
Gurtner GC et al (2008) Wound repair and regeneration. Nature. https://doi.org/10.1038/nature07039
Hill DS et al (2015) A novel fully humanized 3d skin equivalent to model early melanoma invasion. Mol Cancer Ther 14(11):2665–2673
Ho C-L et al (2013) Ecto-nucleoside triphosphate diphosphohydrolase 2 modulates local ATP-induced calcium signaling in human HaCaT keratinocytes. PLoS ONE 8(3):e57666
Huang Z et al (2021) From purines to purinergic signalling: molecular functions and human diseases. Signal Transduct Target Ther 6(1):162
Jean J, Soucy J, Pouliot R (2011) Effects of retinoic acid on keratinocyte proliferation and differentiation in a psoriatic skin model. Tissue Eng A. https://doi.org/10.1089/ten.tea.2010.0463
Jensen EC (2013) Quantitative analysis of histological staining and fluorescence using ImageJ. Anat Rec 296(3):378–381
Jin H et al (2014) P2Y2R activation by nucleotides promotes skin wound-healing process. Exp Dermatol. https://doi.org/10.1111/exd.12440
Jokela T et al (2017) Human keratinocytes respond to extracellular UTP by induction of hyaluronan synthase 2 expression and increased hyaluronan synthesis. J Biol Chem 292(12):4861–4872
Kauffenstein G et al (2010) NTPDase1 (CD39) controls nucleotide-dependent vasoconstriction in mouse. Cardiovasc Res 85(1):204–213
Kukulski F et al (2005) Comparative hydrolysis of P2 receptor agonists by NTPDases 1, 2, 3 and 8. Purinergic Signal 1(2):193–204
Laplante AF et al (2001) Mechanisms of wound reepithelialization: hints from a tissue-engineered reconstructed skin to long-standing questions. FASEB J 15(13):2377–2389
Larouche D et al (2016) Improved methods to produce tissue-engineered skin substitutes suitable for the permanent closure of full-thickness skin injuries. Biores Open Access 5(1):320–329
Lavoie A et al (2013) Human epithelial stem cells persist within tissue-engineered skin produced by the self-assembly approach. Tissue Eng A 19(7–8):1023–1038
Lazarowski ER, Boucher RC Harden TK (2000) Constitutive release of ATP and evidence for major contribution of ecto-nucleotide pyrophosphatase and nucleoside diphosphokinase to extracellular nucleotide concentrations. J Biol Chem 275(40):31061–31068
LeBleu VS, Neilson EG (2020) Origin and functional heterogeneity of fibroblasts. FASEB J 34(3):3519–3536
Lee S-Y (2015) Identification and pharmacological characterization of nucleotide pyrophosphatase, phosphodiesterase 1 (NPP1) inhibitors
Martin P (1997) Wound healing–aiming for perfect skin regeneration. Science 276(5309):75–81
Mizumoto N et al (2002) CD39 is the dominant Langerhans cell–associated ecto-NTPDase: modulatory roles in inflammation and immune responsiveness. Nat Med. https://doi.org/10.1038/nm0402-358
Moulin VJ (2021) Three-dimensional model of hypertrophic scar using a tissue-engineering approach. Methods Mol Biol 2299:419–434
Naasani LIS et al (2017) Extracellular nucleotide hydrolysis in dermal and limbal mesenchymal stem cells: a source of adenosine production. J Cell Biochem 118(8):2430–2442
Naasani LIS et al (2018) Comparison of human denuded amniotic membrane and porcine small intestine submucosa as scaffolds for limbal mesenchymal stem cells. Stem Cell Rev Rep. https://doi.org/10.1007/s12015-018-9819-8
Naasani LIS et al (2019) Decellularized human amniotic membrane associated with adipose derived mesenchymal stromal cells as a bioscaffold: physical, histological and molecular analysis. Biochem Eng J. https://doi.org/10.1016/j.bej.2019.107366
Nguyen BP, Gil SG, Carter WG (2000) Deposition of laminin 5 by keratinocytes regulates integrin adhesion and signaling. J Biol Chem 275(41):31896–31907
Peng X et al (2021) Mechanism of graft damage caused by NTPDase1-activated macrophages in acute antibody-mediated rejection. Transpl Proc 53(1):436–442
Pintor J et al (2004) UTP and diadenosine tetraphosphate accelerate wound healing in the rabbit cornea. Ophthalmic Physiol Opt J Br Coll Ophthalmic Opticians 24(3):186–193
Proulx S et al (2011) Stem cells of the skin and cornea: their clinical applications in regenerative medicine. Curr Opin Organ Transplant 16(1):83–89
Robson SC, Sévigny J, Zimmermann H (2006) The E-NTPDase family of ectonucleotidases: structure function relationships and pathophysiological significance. Purinergic Signal 2(2):409–430
Rodrigues M et al (2019) Wound healing: a cellular perspective. Physiol Rev. https://doi.org/10.1152/physrev.00067.2017
Santoro MM, Gaudino G (2005) Cellular and molecular facets of keratinocyte reepithelization during wound healing. Exp Cell Res 304(1):274–286
Singer AJ, Clark RA (1999) Cutaneous wound healing. N Engl J Med 341(10):738–746
Stanley JR et al (1981) Detection of basement membrane zone antigens during epidermal wound healing in pigs. J Investig Dermatol 77(2):240–243
Veith AP et al (2019) Therapeutic strategies for enhancing angiogenesis in wound healing. Adv Drug Deliv Rev 146:97–125
Vig K et al (2017) Advances in skin regeneration using tissue engineering. Int J Mol Sci. https://doi.org/10.3390/ijms18040789
von Kügelgen I, Wetter A (2000) Molecular pharmacology of P2Y-receptors. Naunyn-Schmiedeberg’s Arch Pharmacol 362(4–5):310–323
Weinmüllner R et al (2020) Organotypic human skin culture models constructed with senescent fibroblasts show hallmarks of skin aging. NPJ Aging Mech Dis 6:4
White N et al (2009) An in vivo model of melanoma: treatment with ATP. Purinergic Signal. https://doi.org/10.1007/s11302-009-9156-0
Wiendl HS, Schneider C, Ogilvie A (1998) Nucleotide metabolizing ectoenzymes are upregulated in A431 cells periodically treated with cytostatic ATP leading to partial resistance without preventing apoptosis. Biochem Biophys Acta 1404(3):282–298
Xie Y et al (2010) Development of a three-dimensional human skin equivalent wound model for investigating novel wound healing therapies. Tissue Eng Part C Methods 16(5):1111–1123
Zimmermann H (2001) Ectonucleotidases: some recent developments and a note on nomenclature. Drug Dev Res. https://doi.org/10.1002/ddr.1097
Acknowledgements
We would like to thank the members of the Research Center CHU de Québec-Université Laval for the support, specially to Julie Pelletier, Israël Martel, Guillaume Martin, Emilie Attiogbe, Lucíola Barcelos, Angela Piaceski, Syrine Arif and Sébastien Larochelle.
Funding
MRW is recipient of research productivity fellowship (PQ1D) from Conselho Nacional de Desenvolvimento Científico e Tecnológico – Brasil (CNPq); LISN is recipient of fellowship from Coordenação de Aperfeiçoamento de Pessoal de Nível Superior – Brasil (CAPES) – Finance Code 001. This study was supported by Fundação de Amparo à Pesquisa do Estado do Rio Grande do Sul—Brasil (FAPERGS/CAPES 06/2018-Programa de Internacionalização da pós-graduação no RS (19/2551-0000679-9) to MW and VM; JS, by a grant from the Natural Sciences and Engineering Research Council of Canada (NSERC; RGPIN-2016-05867 (JS) and RGPIN-2019-06500 (VM)) and Quebec Cell, Tissue and Gene Therapy Network (ThéCell) (VM).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Naasani, L.I.S., Sévigny, J., Moulin, V.J. et al. UTP increases wound healing in the self assembled skin substitute (SASS). J. Cell Commun. Signal. 17, 827–844 (2023). https://doi.org/10.1007/s12079-023-00725-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12079-023-00725-2