Abstract
Introduction
Immunotherapy is a new promising treatment for patients with advanced hepatocellular carcinoma (HCC), but is costly and potentially associated with considerable side effects. This study aimed to evaluate the role of machine learning (ML) models in predicting the 1-year cancer-related mortality in advanced HCC patients treated with immunotherapy.
Method
395 HCC patients who had received immunotherapy (including nivolumab, pembrolizumab or ipilimumab) between 2014 and 2019 in Hong Kong were included. The whole data sets were randomly divided into training (n = 316) and internal validation (n = 79) set. The data set, including 47 clinical variables, was used to construct six different ML models in predicting the risk of 1-year mortality. The performances of ML models were measured by the area under receiver operating characteristic curve (AUC) and their performances were compared with C-Reactive protein and Alpha Fetoprotein in ImmunoTherapY score (CRAFITY) and albumin–bilirubin (ALBI) score. The ML models were further validated with an external cohort between 2020 and 2021.
Results
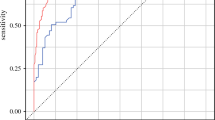
The 1-year cancer-related mortality was 51.1%. Of the six ML models, the random forest (RF) has the highest AUC of 0.92 (95% CI 0.87–0.98), which was better than logistic regression (0.82, p = 0.01) as well as the CRAFITY (0.68, p < 0.01) and ALBI score (0.84, p = 0.04). RF had the lowest false positive (2.0%) and false negative rate (5.2%), and performed better than CRAFITY score in the external validation cohort (0.91 vs 0.66, p < 0.01). High baseline AFP, bilirubin and alkaline phosphatase were three common risk factors identified by all ML models.
Conclusion
ML models could predict 1-year cancer-related mortality in HCC patients treated with immunotherapy, which may help to select patients who would benefit from this treatment.



Similar content being viewed by others
Data availability
Supporting data for this study are available from the corresponding author and the first author upon reasonable request.
Abbreviations
- AUC:
-
Area under the receiver operator characteristics curve
- CDARS:
-
Clinical Data Analysis and Reporting System
- CI:
-
Confidence interval
- LASSO:
-
Least absolute shrinkage and selection operator
- LR:
-
Logistic regression
- ML:
-
Machine learning
- NLR:
-
Negative likelihood ratio
- NPV:
-
Negative predictive value
- PLR:
-
Positive likelihood ratio
- PPV:
-
Positive predictive value
- NN:
-
Sparse neural network
- GBM:
-
Stochastic gradient boosting
- SVM:
-
Support vector machine
- XGBoost:
-
Extreme gradient boosting
- CPS:
-
Child–Pugh score
- HCC:
-
Hepatocellular carcinoma
- MAE:
-
Mean absolute error
- ICD-9:
-
The International Classification of Diseases, Ninth Revision
- TACE:
-
Trans-arterial chemoembolization
- ICI:
-
Immune checkpoint inhibitor
- TKI:
-
Tyrosine kinase inhibitor
- HBV:
-
Chronic hepatitis B infection
- DM:
-
Diabetes mellitus
- HT:
-
Hypertension
- IHD:
-
Ischemic heart disease
- AF:
-
Atrial fibrillation
- CHF:
-
Congestive heart failure
- CRF:
-
Chronic renal failure
- PPI:
-
Proton pump inhibitors
- AFP:
-
Alpha fetoprotein
- ALP:
-
Alkaline phosphatase
- ALT:
-
Alanine aminotransferase
- AST:
-
Aspartate aminotransferase
- GGT:
-
Gamma-glutamyl transferase
- PT:
-
Prothrombin time
- INR:
-
International normalized ratio (INR)
- Na:
-
Sodium
- WBC:
-
White blood cell
References
Fitzmaurice C, Abate D, Abbasi N, et al. Global, Regional, and National Cancer Incidence, Mortality, Years of life lost, years lived with disability, and disability-adjusted life-years for 29 cancer groups, 1990 to 2017: a systematic analysis for the Global Burden of Disease Study. JAMA Oncol 2019;5(12):1749–1768
Lee MJ, Chang SW, Kim JH, et al. Real-world systemic sequential therapy with sorafenib and regorafenib for advanced hepatocellular carcinoma: a multicenter retrospective study in Korea. Invest New Drugs 2021;39(1):260–268
Sangro B, Sarobe P, Hervas-Stubbs S, Melero I. Advances in immunotherapy for hepatocellular carcinoma. Nat Rev Gastroenterol Hepatol 2021. https://doi.org/10.1038/s41575-41021-00438-41570
Xie Y, Xiang Y, Sheng J, et al. Immunotherapy for hepatocellular carcinoma: current advances and future expectations. J Immunol Res 2018;2018:1–15
Nakano S, Eso Y, Okada H, Takai A, Takahashi K, Seno H. Recent advances in immunotherapy for hepatocellular carcinoma. Cancers (Basel) 2020;12(4):1–15
Ziogas IA, Evangeliou AP, Giannis D, et al. The role of immunotherapy in hepatocellular carcinoma: a systematic review and pooled analysis of 2,402 patients. Oncologist. 2021;26(6):e1036–e1049. https://doi.org/10.1002/onco.13638
Pencina MJ, Goldstein BA, D’Agostino RB. Prediction models—development, evaluation, and clinical application. N Engl J Med 2020;382(17):1583–1586
Sendak MP, Ratliff W, Sarro D, et al. Real-world integration of a sepsis deep learning technology into routine clinical care: implementation study. JMIR Med Inf 2020;8(7): e15182
Milea D, Najjar RP, Zhubo J, et al. Artificial intelligence to detect papilledema from ocular fundus photographs. N Engl J Med 2020;382(18):1687–1695
Richter AN, Khoshgoftaar TM. A review of statistical and machine learning methods for modeling cancer risk using structured clinical data. Artif Intell Med 2018;90:1–14
Lui TKL, Wong KKY, Mak LLY, Ko MKL, Tsao SKK, Leung WK. Endoscopic prediction of deeply submucosal invasive carcinoma with use of artificial intelligence. Endosc Int Open 2019;7(4):E514–E520
Leung WK, Cheung KS, Li B, Law SYK, Lui TKL. Applications of machine learning models in the prediction of gastric cancer risk in patients after Helicobacter pylori eradication. Aliment Pharmacol Ther 2021;53(8):864–872
Vanderbeck S, Bockhorst J, Komorowski R, Kleiner DE, Gawrieh S. Automatic classification of white regions in liver biopsies by supervised machine learning. Hum Pathol 2014;45(4):785–792
Byra M, Styczynski G, Szmigielski C, et al. Transfer learning with deep convolutional neural network for liver steatosis assessment in ultrasound images. Int J Comput Assist Radiol Surg 2018;13(12):1895–1903
Ma H, Xu CF, Shen Z, Yu CH, Li YM. Application of machine learning techniques for clinical predictive modeling: a cross-sectional study on nonalcoholic fatty liver disease in China. Biomed Res Int 2018;2018:4304376
Konerman MA, Zhang Y, Zhu J, Higgins PD, Lok AS, Waljee AK. Improvement of predictive models of risk of disease progression in chronic hepatitis C by incorporating longitudinal data. Hepatology 2015;61(6):1832–1841
Wei R, Wang J, Wang X, et al. Clinical prediction of HBV and HCV related hepatic fibrosis using machine learning. EBioMedicine. 2018;35:124–132
Cao Y, Hu ZD, Liu XF, Deng AM, Hu CJ. An MLP classifier for prediction of HBV-induced liver cirrhosis using routinely available clinical parameters. Dis Mark 2013;35(6):653–660
Eaton JE, Vesterhus M, McCauley BM, et al. Primary sclerosing cholangitis risk estimate tool (PREsTo) predicts outcomes of the disease: a derivation and validation study using machine learning. Hepatology 2020;71(1):214–224
Andres A, Montano-Loza A, Greiner R, et al. A novel learning algorithm to predict individual survival after liver transplantation for primary sclerosing cholangitis. PLoS One 2018;13(3): e0193523
Kim JW, Ye Q, Forgues M, et al. Cancer-associated molecular signature in the tissue samples of patients with cirrhosis. Hepatology 2004;39(2):518–527
Zou H, Yang X, Li QL, Zhou QX, Xiong L, Wen Y. A comparative study of albumin-bilirubin score with child-pugh score, model for end-stage liver disease score and indocyanine green R15 in predicting posthepatectomy liver failure for hepatocellular carcinoma patients. Dig Dis 2018;36(3):236–243
Scheiner B, Pomej K, Kirstein MM, et al. Prognosis of patients with hepatocellular carcinoma treated with immunotherapy—development and validation of the CRAFITY score. J Hepatol 2022;76(2):353–363
Mao S, Yu X, Shan Y, Fan R, Wu S, Lu C. Albumin-bilirubin (ALBI) and Monocyte to lymphocyte ratio (MLR)-based nomogram model to predict tumor recurrence of AFP-negative hepatocellular carcinoma. J Hepatocell Carcinoma 2021;8:1355–1365
Chiu SS, Lau YL, Chan KH, Wong WHS, Peiris JSM. Influenza-related hospitalizations among children in Hong Kong. N Engl J Med 2002;347(26):2097–2103
Chan EW, Lau WC, Leung WK, et al. Prevention of dabigatran-related gastrointestinal bleeding with gastroprotective agents: a population-based study. Gastroenterology 2015;149(3):586–595
Cheung KS, Seto WK, Fung J, Lai CL, Yuen MF. Epidemiology and natural history of primary biliary cholangitis in the Chinese: a territory-based study in Hong Kong between 2000 and 2015. Clin Transl Gastroenterol 2017;8(8): e116
Leung WK, Wong IOL, Cheung KS, et al. Effects of Helicobacter pylori treatment on incidence of gastric cancer in older individuals. Gastroenterology 2018;155(1):67–75
Cheung KS, Chan EW, Wong AYS, Chen LJ, Wong ICK, Leung WK. Long-term proton pump inhibitors and risk of gastric cancer development after treatment for Helicobacter pylori: a population-based study. Gut 2018;67(1):28–35
Cheung KS, Chan EW, Chen L, Seto WK, Wong ICK, Leung WK. Diabetes increases risk of gastric cancer after Helicobacter pylori eradication: a territory-wide study with propensity score analysis. Diabetes Care. 2019;42(9):1769–1775
United States, Department of Health and Human Services, Food and Drug Administration. FDA grants accelerated approval to nivolumab for HCC previously treated with sorafenib. https://www.fda.gov/drugs/resources-information-approved-drugs/fda-grants-accelerated-approval-nivolumab-hcc-previously-treated-sorafenib. Accessed 6 May 2021
United States, Department of Health and Human Services, Food and Drug Administration. FDA grants accelerated approval to pembrolizumab for hepatocellular carcinoma. https://www.fda.gov/drugs/fda-grants-accelerated-approval-pembrolizumab-hepatocellular-carcinoma. Accessed 6 May 2021
Lee JH, Shi Z, Gao Z. On LASSO for Predictive Regression. arXiv Website. https://arxiv.org/abs/1810.03140.pdf. Accessed 27 July 2020.
Kelvin PM. Machine Learning: A Probabilistic Perspective. Cambridge: MIT Press; 2012
Chen T, Guestrin C. XGBoost: a scalable tree boosting system. arXiv Website. https://arxiv.org/pdf/1603.02754.pdf. Accessed 24 Mar 2019.
Schonlau M, Zou RY. The random forest algorithm for statistical learning. Stata J 2020;20(1):3–29
Friedman JH. Stochastic gradient boosting. Comput Stat Data Anal 2002;38:367–378
Suraj S, Akshayvarun S, Venkatesh B. Training Sparse Neural Networks. arXiv Website. https://arxiv.org/abs/1611.06694.pdf. Accessed 27 July 2020.
Bruix J, Llovet JM. Prognostic prediction and treatment strategy in hepatocellular carcinoma. Hepatology 2002;35(3):519–524
Ikai I, Yamamoto Y, Yamamoto N, et al. Results of hepatic resection for hepatocellular carcinoma invading major portal and/or hepatic veins. Surg Oncol Clin N Am 2003;12(1):65–75 (ix)
Pawlik TM, Poon RT, Abdalla EK, et al. Hepatectomy for hepatocellular carcinoma with major portal or hepatic vein invasion: results of a multicenter study. Surgery 2005;137(4):403–410
Chang H, Jung W, Kim A, et al. Expression and prognostic significance of programmed death protein 1 and programmed death ligand-1, and cytotoxic T lymphocyte-associated molecule-4 in hepatocellular carcinoma. APMIS 2017;125(8):690–698
Li J, Huang L, Liu C, et al. Risk factors and clinical outcomes of extrahepatic recurrence in patients with post-hepatectomy recurrent hepatocellular carcinoma. ANZ J Surg. 2021;91(6):1174–1179. https://doi.org/10.1111/ans.16737
Chen KL, Gao J. Factors influencing the short-term and long-term survival of hepatocellular carcinoma patients with portal vein tumor thrombosis who underwent chemoembolization. World J Gastroenterol 2021;27(13):1330–1340
Xiong D, Zhang K, Xu M. Prognostic factors of nivolumab in advanced hepatocellular carcinoma: a systematic review and meta-analysis. Panminerva Med. 2021. https://doi.org/10.23736/S0031-0808.21.04282-8
Llovet JM, Bru C, Bruix J. Prognosis of hepatocellular carcinoma: the BCLC staging classification. Semin Liver Dis 1999;19(3):329–338
Yau T, Tang VY, Yao TJ, Fan ST, Lo CM, Poon RT. Development of Hong Kong Liver Cancer staging system with treatment stratification for patients with hepatocellular carcinoma. Gastroenterology 2014;146(7):1691–1700
Forner A, Reig ME, de Lope CR, Bruix J. Current strategy for staging and treatment: the BCLC update and future prospects. Semin Liver Dis 2010;30(1):61–74
Heinrich S, Sprinzl M, Schmidtmann I, et al. Validation of prognostic accuracy of MESH, HKLC, and BCLC classifications in a large German cohort of hepatocellular carcinoma patients. United European Gastroenterol J. 2020;8(4):444–452
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
WKL was involved in the study design and conception; interpretation of the data; drafting of manuscript and study supervision. KSC were involved in the data acquisition and critical review of the manuscript. TKLT was involved in the study design, conception, data analysis and drafting of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Human and animal research
This article does not contain any studies with animals performed by any of the authors.
Consent to participate
This study was approved by the ethics committees of our hospital and fully complied with the Declaration of Helsinki and the Guideline for Good Clinical Practice.
Consent for publication
Informed consent for publication was obtained from all author.
Plant reproducibility
This article does not contain any information regarding this issue.
Clinical trials registration
This article does not have clinical trial registration.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lui, T.K.L., Cheung, K.S. & Leung, W.K. Machine learning models in the prediction of 1-year mortality in patients with advanced hepatocellular cancer on immunotherapy: a proof-of-concept study. Hepatol Int 16, 879–891 (2022). https://doi.org/10.1007/s12072-022-10370-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-022-10370-3