Abstract
Propose
To evaluate the safety and efficacy of endovascular brachytherapy (EVBT) with iodine-125 (125I) seed strand implantation combined with stent placement and transarterial chemoembolization (TACE) to treat hepatocellular carcinoma (HCC) with main portal vein tumor thrombus (MPVTT).
Methods
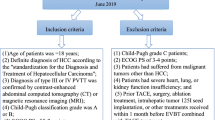
Data of 276 consecutive HCC patients with MPVTT treated by stent placement and TACE were analyzed retrospectively. 125I seed strands were implanted in 182 patients (group A). The remaining 94 patients, who did not receive EVBT, served as control (group B). The overall survival, free of disease progression survival, stent patency period and procedure-related complications were compared between the two groups.
Results
During a mean 9.9 ± 9.7 month (range 1.3–62.2 months) follow-up, the median survival time was 9.3 ± 0.9 months (95 % CI 7.6–11.0 months) in group A compared to 4.9 ± 0.5 months (95 % CI 4.0–5.8 months) in group B (p < 0.001). Median free of disease progression survival time in group A and B was 1.8 ± 0.1 months (95 % CI 1.6–2.0 months) and 1.5 ± 0.1 months (95 % CI 1.3–1.7 months), respectively (p < 0.001). Median stent patency period was 9.2 ± 1.1 months (95 % CI 7.0–11.4 months) in group A and 4.8 ± 0.5 months (95 % CI 3.9–5.7 months) in group B, respectively (p < 0.001).
Conclusion
These findings suggested that EVBT combined with stent placement and TACE might be a safe and effective palliative treatment option for HCC with main portal vein tumor thrombus.




Similar content being viewed by others
Abbreviations
- EVBT:
-
Endovascular brachytherapy
- 125I:
-
Iodine-125
- TACE:
-
Transarterial chemoembolization
- HCC:
-
Hepatocellular carcinoma
- MPV:
-
Main portal vein
- MPVTT:
-
Main portal vein tumor thrombus
- CT:
-
Computed tomography
- AFP:
-
Alpha-fetoprotein
References
Yang JD, Roberts LR. Hepatocellular carcinoma: a global view. Nat Rev Gastroenterol Hepatol 2010;7:448–458
Cheung TK, Lai CL, Wong BCY, et al. Clinical features, biochemical parameters, and virological profiles of patients with hepatocellular carcinoma in Hong Kong. Aliment Pharmacol Ther 2006;24:573–583
Minagawa M, Makuuchi M. Treatment of hepatocellular carcinoma accompanied by portal vein tumor thrombus. World J Gastroenterol 2006;12:7561–7567
Katagiri S, Yamamoto M. Multidisciplinary treatments for hepatocellular carcinoma with major portal vein tumor thrombus. Surg Today 2014;44:219–226
Bruix J, Sherman M. AASLD practice guideline: management of hepatocellular carcinoma: an update. Hepatology 2011;53:1020–1022
Lau WY, Lai EC. Hepatocellular carcinoma: current management and recent advances. Hepatobiliary Pancreat Dis Int 2008;7:237–257
Llovet JM, Ricci S, Mazzaferro V, et al. Sorafenib in advanced he-patocellular carcinoma. N Engl J Med 2008;359:378–390
Shao YY, Huang CC, Po-Chin L, et al. Hepatic arterial infusion of chemotherapy for advanced hepatocellular carcinoma. Asia Pac J Clin Oncol 2010;6:80–88
Lee DS, Seong J. Radiotherapeutic options for hepatocellular carcinoma with portal vein tumor thrombosis. Liver Cancer 2014;3:18–30
Lau WY, Sangro B, Pier-Jer Chen PJ, et al. Treatment for hepatocellular carcinoma with portal vein tumor thrombosis: the emerging role for radioembolization using yttrium-90. Oncology 2013;84:311–318
Xue TC, Xie Xiao-Ying, Zhang Lan, et al. Transarterial chemoembolization for hepatocellular carcinoma with portal vein tumor thrombus: a meta-analysis. BMC Gastroenterol 2013;13:60–68
Zhang XB, Wang JH, Yan ZP, et al. Hepatocellular carcinoma invading the main portal vein: treatment with transcatheter arterial chemoembolization and portal vein stenting. Cardiovasc Intervent Radiol 2009;32:52–61
Zhang W, Yan Z, Luo J, et al. Iodine-125 seeds strand for treatment of tumor thrombus in inferior vena cava: an experimental study in a rabbit model. Cardiovasc Intervent Radiol 2013;36:1371–1382
Luo J, Yan Z, Liu Q, et al. Endovascular placement of iodine-125 seed strand and stent combined with chemoembolization for treatment of hepatocellular carcinoma with tumor thrombus in main portal vein. J Vasc Interv Radiol 2011;22:479–489
Llovet JM, Bru C, Bruix J. Prognosis of hepatocellular carcinoma: The BCLC staging classification. Semin Liver Dis 1999;19:329–338
Lencioni R, Llovet JM. Modified RECIST (mRECIST) assessment for hepatocellular carcinoma. Semin Liver Dis 2010;30:52–60
National Cancer Institute. Common terminology criteria for adverse events, version 3.0. http://ctep.cancer.gov/reporting/ctc.html. Published 9 August 2006. Accessed 18 June 2009
Nath R, Anderson LL, Luxton G, et al. Dosimetry of interstitial brachytherapy sources: recommendations of AAPM radiation therapy committee task group No. 43. Med Phys 1995;22:209–234
Chen Y, Wang XL, Yan ZP, et al. The use of 125I seed strands for intraluminal brachytherapy of malignant obstructive jaundice. Cancer Biother Radiopharm 2012;27:317–323
Jeong SW, Jang JY, Shim KY, et al. Practical effect of sorafenib monotherapy on advanced hepatocellular carcinoma and portal vein tumor thrombosis. Gut Liver 2013;7:696–703
Liu L, Zhang C, Zhao Y, et al. Transarterial chemoembolization for the treatment of advanced hepatocellular carcinoma with portal vein tumor thrombosis: prognostic factors in a single-center study of 188 patients. Biomed Res Int 2014;2014:194278
Zhu K, Chen J, Lai L, et al. Hepatocellular carcinoma with portal vein tumor thrombus: treatment with transarterial chemoembolization combined with sorafenib—a retrospective controlled study. Radiology 2014;272:284–293
Hu H, Duan Z, Long X, et al. Sorafenib combined with transarterial chemoembolization versus transarterial chemoembolization alone for advanced-stage hepatocellular carcinoma: a propensity score matching study. PLoS ONE 2014;9:e96620
Jelic S, Sotiropoulos GC. ESMO Guidelines Working Group. Hepatocellular carcinoma: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 2010;21(suppl 5):v59–v64
Sidawy AN, Weiswasser JM, Waksman R. Peripheral vascular brachytherapy. J Vasc Surg 2002;35:1041–1047
Sindelar WF, Kinsella TJ. Normal tissue tolerance to intraoperative radiotherapy. Surg Oncol Clin N Am 2003;12:925–942
Acknowledgements
This work was supported by the project of Advanced and Appropriate Technique Generalization from Shanghai Health and Family Planning Committee (2013SY060).
Author contribution
Study concept and design by JJL and ZPY; acquisition of data by ZHZ and WZ; analysis and interpretation of data by JJL, JHW and QXL; obtained funding by JJL and ZPY.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Jian-Jun Luo, Zi-Han Zhang, Qing-Xin Liu, Jian-Hua Wang and Zhi-Ping Yan declare that they have no conflict of interest.
Ethical standards
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (Zhongshan Hospital, Fudan University, China) and the Helsinki Declaration of 1975, as revised in 2008 (5). Informed consent was obtained from all patients for being included in the study.
Additional information
Jian-Jun Luo, Zi-Han Zhang and Qing-Xin Liu have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Luo, JJ., Zhang, ZH., Liu, QX. et al. Endovascular brachytherapy combined with stent placement and TACE for treatment of HCC with main portal vein tumor thrombus. Hepatol Int 10, 185–195 (2016). https://doi.org/10.1007/s12072-015-9663-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-015-9663-8