Abstract
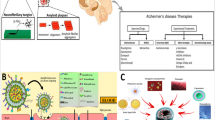
Based on the findings in recent years, we summarize the therapeutic potential of vorinostat (VOR), the first approved histone deacetylase (HDAC) inhibitor, in disorders of brain, and strategies to improve drug efficacy and reduce side effects. Scientific evidences provide a strong case for the therapeutic utility of VOR in various disorders affecting brain, including stroke, Alzheimer’s disease, frontotemporal dementia, Parkinson's disease, Huntington's disease, amyotrophic lateral sclerosis, spinal muscular atrophy, X‐linked adrenoleukodystrophy, epilepsy, Niemann-Pick type C disease, and neuropsychiatric disorders. Further elucidation of the neuroprotective and neurorestorative properties of VOR using proper clinical study designs could provide momentum towards its clinical application. To improve the therapeutic prospect, concerns on systemic toxicity and off-target actions need to be addressed along with the improvement in formulation and delivery aspects, especially with respect to solubility, permeability, and pharmacokinetic properties. Newer approaches in this regard include poly(ethylene glycol)-b-poly(dl-lactic acid) micelles, VOR-pluronic F127 micelles, encapsulation of iron complexes of VOR into PEGylated liposomes, human serum albumin bound VOR nanomedicine, magnetically guided layer-by-layer assembled nanocarriers, as well as convection-enhanced delivery. Even though targeting specific class or isoform of HDAC is projected as advantageous over pan-HDAC inhibitor like VOR, in terms of adverse effects and efficacy, till clinical validation, the idea is debated. As the VOR treatment-related adverse changes are mostly found reversible, further optimization of the therapeutic strategies with respect to dose, dosage regimen, and formulations of VOR could propel its clinical prospects.


Similar content being viewed by others
Abbreviations
- ABCD1:
-
ATP‐binding cassette subfamily D member 1
- BBB:
-
Blood–brain barrier
- BDNF:
-
Brain-derived neurotrophic factor
- cAMP:
-
Cyclic adenosine monophosphate
- CREB:
-
CAMP response element binding protein
- CRTC1:
-
CREB-regulated transcription coactivator 1
- CBP:
-
CREB binding protein
- CNS:
-
Central nervous system
- CTCL:
-
Cutaneous T-cell lymphoma
- DMSO:
-
Dimethyl sulfoxide
- GBM:
-
Glioblastoma multiforme
- GDNF:
-
Glial cell-derived neurotrophic factor
- HATs:
-
Histone acetyltransferases
- HDACs:
-
Histone deacetylases
- Hsp:
-
Heat shock protein
- iPSC:
-
Induced pluripotent stem cells
- NPC:
-
Niemann-Pick Type C
- NR2B:
-
N-Methyl-D-aspartate receptor 2 subunit B
- PTCL:
-
Peripheral T-cell lymphoma
- SAHA:
-
Suberoylanilide hydroxamic acid
- SMA:
-
Spinal muscular atrophy
- SMN:
-
Survival motor neuron
- VLCFA:
-
Very long‐chain fatty acids
- VOR:
-
Vorinostat
References
Abel, T., & Zukin, R. S. (2008). Epigenetic targets of HDAC inhibition in neurodegenerative and psychiatric disorders. Current Opinion in Pharmacology, 8(1), 57–64
Alarcón, J. M., Malleret, G., Touzani, K., Vronskaya, S., Ishii, S., Kandel, E. R., & Barco, A. (2004). Chromatin acetylation, memory, and LTP are impaired in CBP+/− mice: a model for the cognitive deficit in Rubinstein-Taybi syndrome and its amelioration. Neuron, 42(6), 947–959
Almeida, S., Gao, F., Coppola, G., & Gao, F.-B. (2016). Suberoylanilide hydroxamic acid increases progranulin production in iPSC-derived cortical neurons of frontotemporal dementia patients. Neurobiology of Aging, 42, 35–40
Alquezar, C., Esteras, N., de la Encarnación, A., Moreno, F., de Munain, A. L., & Martín-Requero, Á. (2015). Increasing progranulin levels and blockade of the ERK1/2 pathway: Upstream and downstream strategies for the treatment of progranulin deficient frontotemporal dementia. European Neuropsychopharmacology, 25(3), 386–403
Athira, K. V., Bandopadhyay, S., Samudrala, P. K., Naidu, V., Lahkar, M., & Chakravarty, S. (2020). An overview of the heterogeneity of major depressive disorder: Current knowledge and future prospective. Current Neuropharmacology, 18(3), 168–187
Athira, K., Madhana, R. M., Lahkar, M., Sinha, S., & Naidu, V. (2018). Antidepressant activity of vorinostat is associated with amelioration of oxidative stress and inflammation in a corticosterone-induced chronic stress model in mice. Behavioural Brain Research, 344, 73–84
Athira, K., Wahul, A. B., Soren, K., Das, T., Dey, S., Samudrala, P. K., Kumar, A., Lahkar, M., & Chakravarty, S. (2021). Differential modulation of GR signaling and HDACs in the development of resilient/vulnerable phenotype and antidepressant-like response of vorinostat. Psychoneuroendocrinology, 124, 105083
Atluri, V. S. R., Pilakka-Kanthikeel, S., Samikkannu, T., Sagar, V., Kurapati, K. R. V., Saxena, S. K., Yndart, A., Raymond, A., Ding, H., & Hernandez, O. (2014). Vorinostat positively regulates synaptic plasticity genes expression and spine density in HIV infected neurons: Role of nicotine in progression of HIV-associated neurocognitive disorder. Molecular Brain, 7(1), 37
Benito, E., Urbanke, H., Ramachandran, B., Barth, J., Halder, R., Awasthi, A., Jain, G., Capece, V., Burkhardt, S., & Navarro-Sala, M. (2015). HDAC inhibitor–dependent transcriptome and memory reinstatement in cognitive decline models. The Journal of Clinical Investigation, 125(9), 3572–3584
Berger, J., & Gärtner, J. (2006). X-linked adrenoleukodystrophy: Clinical, biochemical and pathogenetic aspects. Biochimica et Biophysica Acta B, 1763(12), 1721–1732
Berton, O., McClung, C. A., DiLeone, R. J., Krishnan, V., Renthal, W., Russo, S. J., Graham, D., Tsankova, N. M., Bolanos, C. A., & Rios, M. (2006). Essential role of BDNF in the mesolimbic dopamine pathway in social defeat stress. Science, 311(5762), 864–868
Broide, R. S., Redwine, J. M., Aftahi, N., Young, W., Bloom, F. E., & Winrow, C. J. (2007). Distribution of histone deacetylases 1–11 in the rat brain. Journal of Molecular Neuroscience, 31(1), 47–58
Buchwald, M., Krämer, O. H., & Heinzel, T. (2009). HDACi–targets beyond chromatin. Cancer Letters, 280(2), 160–167
Cenik, B., Sephton, C. F., Dewey, C. M., Xian, X., Wei, S., Yu, K., Niu, W., Coppola, G., Coughlin, S. E., & Lee, S. E. (2011). Suberoylanilide hydroxamic acid (vorinostat) up-regulates progranulin transcription rational therapeutic approach to frontotemporal dementia. Journal of Biological Chemistry, 286(18), 16101–16108
Chakravarty, S., Bhat, U. A., Reddy, R. G., Gupta, P., & Kumar, A. (2014a). Histone deacetylase inhibitors and psychiatric disorders. Epigenetics in Psychiatry, 2, 515–544
Chakravarty, S., Pathak, S. S., Maitra, S., Khandelwal, N., Chandra, K. B., & Kumar, A. (2014b). Epigenetic regulatory mechanisms in stress-induced behavior. International Review of Neurobiology., 115, 117–154
Chandran, P., Kavalakatt, A., Malarvizhi, G. L., Vasanthakumari, D. R. V. N., Retnakumari, A. P., Sidharthan, N., Pavithran, K., Nair, S., & Koyakutty, M. (2014). Epigenetics targeted protein-vorinostat nanomedicine inducing apoptosis in heterogeneous population of primary acute myeloid leukemia cells including refractory and relapsed cases. Nanomedicine: Nanotechnology, Biology and Medicine, 10(4), 721–732
Chen, S., Wu, H., Ossola, B., Schendzielorz, N., Wilson, B. C., Chu, C.-H., Chen, S., Wang, Q., Zhang, D., & Qian, L. (2012). Suberoylanilide hydroxamic acid, a histone deacetylase inhibitor, protects dopaminergic neurons from neurotoxin-induced damage. British Journal of Pharmacology, 165(2), 494–505
Choudhary, C., Kumar, C., Gnad, F., Nielsen, M. L., Rehman, M., Walther, T. C., Olsen, J. V., & Mann, M. (2009). Lysine acetylation targets protein complexes and co-regulates major cellular functions. Science, 325(5942), 834–840
Covington, H. E., Maze, I., LaPlant, Q. C., Vialou, V. F., Ohnishi, Y. N., Berton, O., Fass, D. M., Renthal, W., Rush, A. J., & Wu, E. Y. (2009). Antidepressant actions of histone deacetylase inhibitors. Journal of Neuroscience, 29(37), 11451–11460
Cuadrado-Tejedor, M., Garcia-Barroso, C., Sanzhez-Arias, J., Mederos, S., Rabal, O., Ugarte, A., Franco, R., Pascual-Lucas, M., Segura, V., & Perea, G. (2015). Concomitant histone deacetylase and phosphodiesterase 5 inhibition synergistically prevents the disruption in synaptic plasticity and it reverses cognitive impairment in a mouse model of Alzheimer’s disease. Clinical Epigenetics, 7(1), 108
De Ruijter, A. J., Van Gennip, A. H., Caron, H. N., Stephan, K., & Van Kuilenburg, A. B. (2003). Histone deacetylases (HDACs): Characterization of the classical HDAC family. Biochemical Journal, 370(3), 737–749
De Souza, C. (2015). P Chatterji B: HDAC inhibitors as novel anti-cancer therapeutics. Recent Patents on Anti-cancer Drug Discovery, 10(2), 145–162
De Souza, C., Lindstrom, A. R., Ma, Z., & Chatterji, B. P. (2020). Nanomaterials as potential transporters of HDAC inhibitors. Medicine in Drug Discovery, 6, 100040
Di, X.-J., Han, D.-Y., Wang, Y.-J., Chance, M. R., & Mu, T.-W. (2013). SAHA enhances proteostasis of epilepsy-associated α1 (A322D) β2γ2 GABAA receptors. Chemistry & Biology, 20(12), 1456–1468
Didonna, A., & Opal, P. (2015). The promise and perils of HDAC inhibitors in neurodegeneration. Annals of Clinical and Translational Neurology, 2(1), 79–101
Dokmanovic, M., Clarke, C., & Marks, P. A. (2007). Histone deacetylase inhibitors: Overview and perspectives. Molecular Cancer Research, 5(10), 981–989
Drummond, D. C., Noble, C. O., Kirpotin, D. B., Guo, Z., Scott, G. K., & Benz, C. C. (2005). Clinical development of histone deacetylase inhibitors as anticancer agents. Annual Review of Pharmacology and Toxicology, 45, 495–528
Durisic, N., Keramidas, A., Dixon, C. L., & Lynch, J. W. (2018). SAHA (vorinostat) corrects inhibitory synaptic deficits caused by missense epilepsy mutations to the GABAA receptor γ2 subunit. Frontiers in Molecular Neuroscience, 11, 89
Eckschlager, T., Plch, J., Stiborova, M., & Hrabeta, J. (2017). Histone deacetylase inhibitors as anticancer drugs. International Journal of Molecular Sciences, 18(7), 1414
Eyüpoglu, I. Y., Hahnen, E., Buslei, R., Siebzehnrübl, F. A., Savaskan, N. E., Lüders, M., Tränkle, C., Wick, W., Weller, M., & Fahlbusch, R. (2005). Suberoylanilide hydroxamic acid (SAHA) has potent anti-glioma properties in vitro, ex vivo and in vivo. Journal of Neurochemistry, 93(4), 992–999
Faraco, G., Pancani, T., Formentini, L., Mascagni, P., Fossati, G., Leoni, F., Moroni, F., & Chiarugi, A. (2006). Pharmacological inhibition of histone deacetylases by suberoylanilide hydroxamic acid specifically alters gene expression and reduces ischemic injury in the mouse brain. Molecular Pharmacology, 70(6), 1876–1884
Faria Freitas, M., Cuendet, M., & Bertrand, P. (2018). HDAC inhibitors: a 2013–2017 patent survey. Expert Opinion on Therapeutic Patents, 28(5), 365–381
Finnin, M. S., Donigian, J. R., Cohen, A., Richon, V. M., Rifkind, R. A., Marks, P. A., Breslow, R., & Pavletich, N. P. (1999). Structures of a histone deacetylase homologue bound to the TSA and SAHA inhibitors. Nature, 401(6749), 188–193
Fujita, Y., Morinobu, S., Takei, S., Fuchikami, M., Matsumoto, T., Yamamoto, S., & Yamawaki, S. (2012). Vorinostat, a histone deacetylase inhibitor, facilitates fear extinction and enhances expression of the hippocampal NR2B-containing NMDA receptor gene. Journal of Psychiatric Research, 46(5), 635–643
Galanis, E., Jaeckle, K. A., Maurer, M. J., Reid, J. M., Ames, M. M., Hardwick, J. S., Reilly, J. F., Loboda, A., Nebozhyn, M., & Fantin, V. R. (2009). Phase II trial of vorinostat in recurrent glioblastoma multiforme: A north central cancer treatment group study. Journal of Clinical Oncology, 27(12), 2052
Gangisetty, O. & Murugan, S. (2016). Epigenetic modifications in neurological diseases: natural products as epigenetic modulators a treatment strategy. In The benefits of natural products for neurodegenerative diseases. (pp. 1–25). Springer.
Gao, L., Cueto, M. A., Asselbergs, F., & Atadja, P. (2002). Cloning and functional characterization of HDAC11, a novel member of the human histone deacetylase family. Journal of Biological Chemistry, 277(28), 25748–25755
Ge, Z., Da, Y., Xue, Z., Zhang, K., Zhuang, H., Peng, M., Li, Y., Li, W., Simard, A., & Hao, J. (2013). Vorinostat, a histone deacetylase inhibitor, suppresses dendritic cell function and ameliorates experimental autoimmune encephalomyelitis. Experimental Neurology, 241, 56–66
Gill, S. S. (2019). Method of treating a CNS disorder using a water-soluble histone deacetylase inhibitor. Google Patents.
Golden, S. A., Christoffel, D. J., Heshmati, M., Hodes, G. E., Magida, J., Davis, K., Cahill, M. E., Dias, C., Ribeiro, E., & Ables, J. L. (2013). Epigenetic regulation of RAC1 induces synaptic remodeling in stress disorders and depression. Nature Medicine, 19(3), 337
Grayson, D. R., Kundakovic, M., & Sharma, R. P. (2010). Is there a future for histone deacetylase inhibitors in the pharmacotherapy of psychiatric disorders? Molecular Pharmacology, 77(2), 126–135
Gryder, B. E., Sodji, Q. H., & Oyelere, A. K. (2012). Targeted cancer therapy: giving histone deacetylase inhibitors all they need to succeed. Future Medicinal Chemistry, 4(4), 505–524
Guan, J.-S., Haggarty, S. J., Giacometti, E., Dannenberg, J.-H., Joseph, N., Gao, J., Nieland, T. J., Zhou, Y., Wang, X., & Mazitschek, R. (2009). HDAC2 negatively regulates memory formation and synaptic plasticity. Nature, 459(7243), 55
Haberland, M., Montgomery, R. L., & Olson, E. N. (2009). The many roles of histone deacetylases in development and physiology: Implications for disease and therapy. Nature Reviews Genetics, 10(1), 32
Hahnen, E., Eyüpoglu, I. Y., Brichta, L., Haastert, K., Tränkle, C., Siebzehnrübl, F. A., Riessland, M., Hölker, I., Claus, P., & Romstöck, J. (2006). In vitro and ex vivo evaluation of second-generation histone deacetylase inhibitors for the treatment of spinal muscular atrophy. Journal of Neurochemistry, 98(1), 193–202
Hanson, J. E., La, H., Plise, E., Chen, Y.-H., Ding, X., Hanania, T., Sabath, E. V., Alexandrov, V., Brunner, D., & Leahy, E. (2013a). SAHA enhances synaptic function and plasticity in vitro but has limited brain availability in vivo and does not impact cognition. PLoS ONE, 8(7), e69964
Hanson, J. E., La, H., Plise, E., Chen, Y.-H., Ding, X., Hanania, T., Sabath, E. V., Alexandrov, V., Brunner, D., & Leahy, E. (2013b). SAHA enhances synaptic function and plasticity in vitro but has limited brain availability in vivo and does not impact cognition. PLoS ONE, 8(7), e69968
Hauke, J., Riessland, M., Lunke, S., Eyüpoglu, I. Y., Blümcke, I., El-Osta, A., Wirth, B., & Hahnen, E. (2009). Survival motor neuron gene 2 silencing by DNA methylation correlates with spinal muscular atrophy disease severity and can be bypassed by histone deacetylase inhibition. Human Molecular Genetics, 18(2), 304–317
Hockly, E., Richon, V. M., Woodman, B., Smith, D. L., Zhou, X., Rosa, E., Sathasivam, K., Ghazi-Noori, S., Mahal, A., & Lowden, P. A. (2003). Suberoylanilide hydroxamic acid, a histone deacetylase inhibitor, ameliorates motor deficits in a mouse model of Huntington’s disease. Proceedings of the National Academy of Sciences, 100(4), 2041–2046
Hoodin, F., LaLonde, L., Errickson, J., Votruba, K., Kentor, R., Gatza, E., Reddy, P., & Choi, S. W. (2019). Cognitive function and quality of life in vorinostat-treated patients after matched unrelated donor myeloablative conditioning hematopoietic cell transplantation. Biology of Blood and Marrow Transplantation, 25(2), 343–353
Jakovcevski, M., & Akbarian, S. (2012). Epigenetic mechanisms in neurological disease. Nature Medicine, 18(8), 1194
Jayant, R. D., Atluri, V. S., Agudelo, M., Sagar, V., Kaushik, A., & Nair, M. (2015). Sustained-release nanoART formulation for the treatment of neuroAIDS. International Journal of Nanomedicine, 10, 1077
Jhelum, P., Karisetty, B., Kumar, A., & Chakravarty, S. (2017). Implications of epigenetic mechanisms and their targets in cerebral ischemia models. Current Neuropharmacology, 15(6), 815–830
Jochems, J., Boulden, J., Lee, B. G., Blendy, J. A., Jarpe, M., Mazitschek, R., Van Duzer, J. H., Jones, S., & Berton, O. (2014). Antidepressant-like properties of novel HDAC6-selective inhibitors with improved brain bioavailability. Neuropsychopharmacology, 39(2), 389
Johnstone, R. W., & Licht, J. D. (2003). Histone deacetylase inhibitors in cancer therapy: Is transcription the primary target? Cancer Cell, 4(1), 13–18
Kazantsev, A. G., & Thompson, L. M. (2008). Therapeutic application of histone deacetylase inhibitors for central nervous system disorders. Nature Reviews Drug Discovery, 7(10), 854–868
Kelly, W. K., O’Connor, O. A., Krug, M. L., Chiao, J. H., Heaney, M., Curley, T., MacGregore-Cortelli, B., Tong, W., Secrist, J. P., & Schwartz, L. (2005). Phase I study of an oral histone deacetylase inhibitor, suberoylanilide hydroxamic acid, in patients with advanced cancer. Journal of Clinical Oncology, 23(17), 3923
Kelly, W. K., Richon, V. M., O’Connor, O., Curley, T., MacGregor-Curtelli, B., Tong, W., Klang, M., Schwartz, L., Richardson, S., & Rosa, E. (2003). Phase I clinical trial of histone deacetylase inhibitor: Suberoylanilide hydroxamic acid administered intravenously. Clinical Cancer Research, 9(10), 3578–3588
Kidd, S. K., & Schneider, J. S. (2010). Protection of dopaminergic cells from MPP+-mediated toxicity by histone deacetylase inhibition. Brain Research, 1354, 172–178
Kilgore, M., Miller, C. A., Fass, D. M., Hennig, K. M., Haggarty, S. J., Sweatt, J. D., & Rumbaugh, G. (2010). Inhibitors of class 1 histone deacetylases reverse contextual memory deficits in a mouse model of Alzheimer’s disease. Neuropsychopharmacology, 35(4), 870–880
Kontopoulos, E., Parvin, J. D., & Feany, M. B. (2006). α-synuclein acts in the nucleus to inhibit histone acetylation and promote neurotoxicity. Human Molecular Genetics, 15(20), 3012–3023
Kretsovali, A., Hadjimichael, C., & Charmpilas, N. (2012). Histone deacetylase inhibitors in cell pluripotency, differentiation, and reprogramming. Stem Cells International, 2012, 1–10
Kuta, R., Larochelle, N., Fernandez, M., Pal, A., Minotti, S., Tibshirani, M., Louis, K. S., Gentil, B. J., Nalbantoglu, J. N., & Hermann, A. (2020). Depending on the stress, histone deacetylase inhibitors act as heat shock protein co-inducers in motor neurons and potentiate arimoclomol, exerting neuroprotection through multiple mechanisms in ALS models. Cell Stress and Chaperones, 1, 1–19
Kv, A., Madhana, R. M., Bais, A. K., Singh, V. B., Malik, A., Sinha, S., Lahkar, M., Kumar, P., & Samudrala, P. K. (2020). Cognitive improvement by vorinostat through modulation of endoplasmic reticulum stress in a corticosterone-induced chronic stress model in mice. ACS Chemical Neuroscience, 11(17), 2649–2657
Lai, J.-I., Leman, L. J., Ku, S., Vickers, C. J., Olsen, C. A., Montero, A., Ghadiri, M. R., & Gottesfeld, J. M. (2017). Cyclic tetrapeptide HDAC inhibitors as potential therapeutics for spinal muscular atrophy: Screening with iPSC-derived neuronal cells. Bioorganic & Medicinal Chemistry Letters, 27(15), 3289–3293
Lee, P., Murphy, B., Miller, R., Menon, V., Banik, N. L., Giglio, P., Lindhorst, S. M., & Varma, A. K. (2015). Mechanisms and clinical significance of histone deacetylase inhibitors: epigenetic glioblastoma therapy. Anticancer Research, 35(2), 615–625
Li, S., Lu, X., Shao, Q., Chen, Z., Huang, Q., Jiao, Z., Huang, X., Yue, M., Peng, J., & Zhou, X. (2019). Early histone deacetylase inhibition mitigates ischemia/reperfusion brain injury by reducing microglia activation and modulating their phenotype. Frontiers in Neurology, 10, 893
Lindemann, R., Newbold, A., Whitecross, K., Cluse, L., Frew, A., Ellis, L., Williams, S., Wiegmans, A., Dear, A., & Scott, C. (2007). Analysis of the apoptotic and therapeutic activities of histone deacetylase inhibitors by using a mouse model of B cell lymphoma. Proceedings of the National Academy of Sciences, 104(19), 8071–8076
Mai, A., Rotili, D., Valente, S., & Kazantsev, A. G. (2009). Histone deacetylase inhibitors and neurodegenerative disorders: Holding the promise. Current Pharmaceutical Design, 15(34), 3940–3957
Mann, B. S., Johnson, J. R., Cohen, M. H., Justice, R., & Pazdur, R. (2007). FDA approval summary: Vorinostat for treatment of advanced primary cutaneous T-cell lymphoma. The Oncologist, 12(10), 1247–1252
Marks, P. A., & Breslow, R. (2007). Dimethyl sulfoxide to vorinostat: Development of this histone deacetylase inhibitor as an anticancer drug. Nature Biotechnology, 25(1), 84–90
Marks, P. A., & Dokmanovic, M. (2005). Histone deacetylase inhibitors: discovery and development as anticancer agents. Expert opinion on investigational drugs, 14(12), 1497–1511
McLaughlin, F., & La Thangue, N. B. (2004). Histone deacetylase inhibitors open new doors in cancer therapy. Biochemical Pharmacology, 68(6), 1139–1144
Meng, J., Li, Y., Camarillo, C., Yao, Y., Zhang, Y., Xu, C., & Jiang, L. (2014). The anti-tumor histone deacetylase inhibitor SAHA and the natural flavonoid curcumin exhibit synergistic neuroprotection against amyloid-beta toxicity. PLoS ONE, 9(1), e85570
Meng, J., Li, Y., Zhang, M., Li, W., Zhou, L., Wang, Q., Lin, L., Jiang, L., & Zhu, W. (2019). A combination of curcumin, vorinostat and silibinin reverses Aβ-induced nerve cell toxicity via activation of AKT-MDM2-p53 pathway. PeerJ, 7, e6716
Meylan, E. M., Halfon, O., Magistretti, P. J., & Cardinaux, J.-R. (2016). The HDAC inhibitor SAHA improves depressive-like behavior of CRTC1-deficient mice: possible relevance for treatment-resistant depression. Neuropharmacology, 107, 111–121
Mielcarek, M., Benn, C. L., Franklin, S. A., Smith, D. L., Woodman, B., Marks, P. A., & Bates, G. P. (2011). SAHA decreases HDAC 2 and 4 levels in vivo and improves molecular phenotypes in the R6/2 mouse model of Huntington’s disease. PLoS ONE, 6(11), e203
Mitsiades, C. S., Mitsiades, N. S., McMullan, C. J., Poulaki, V., Shringarpure, R., Hideshima, T., Akiyama, M., Chauhan, D., Munshi, N., & Gu, X. (2004). Transcriptional signature of histone deacetylase inhibition in multiple myeloma: Biological and clinical implications. Proceedings of the National Academy of Sciences, 101(2), 540–545
Mohamed, E. A., Hashim, I. I. A., Yusif, R. M., Suddek, G. M., Shaaban, A. A. A., & Badria, F. A. E. (2017). Enhanced in vitro cytotoxicity and anti-tumor activity of vorinostat-loaded pluronic micelles with prolonged release and reduced hepatic and renal toxicities. European Journal of Pharmaceutical Sciences, 96, 232–242
Mohamed, E. A., Zhao, Y., Meshali, M. M., Remsberg, C. M., Borg, T. M., Foda, A. M. M., Takemoto, J. K., Sayre, C. L., Martinez, S. E., & Davies, N. M. (2012). Vorinostat with sustained exposure and high solubility in poly (ethylene glycol)-b-poly (dl-lactic acid) micelle nanocarriers: Characterization and effects on pharmacokinetics in rat serum and urine. Journal of Pharmaceutical Sciences, 101(10), 3787–3798
Morris, M. J., & Monteggia, L. M. (2013). Unique functional roles for class I and class II histone deacetylases in central nervous system development and function. International Journal of Developmental Neuroscience, 31(6), 370–381
Mueller, S., Yang, X., Sottero, T. L., Gragg, A., Prasad, G., Polley, M.-Y., Weiss, W. A., Matthay, K. K., Davidoff, A. M., & DuBois, S. G. (2011). Cooperation of the HDAC inhibitor vorinostat and radiation in metastatic neuroblastoma: Efficacy and underlying mechanisms. Cancer Letters, 306(2), 223–229
Munkacsi, A. B., Hammond, N., Schneider, R. T., Senanayake, D. S., Higaki, K., Lagutin, K., Bloor, S. J., Ory, D. S., Maue, R. A., & Chen, F. W. (2017). Normalization of hepatic homeostasis in the Npc1nmf164 mouse model of Niemann-Pick type C disease treated with the histone deacetylase inhibitor vorinostat. Journal of Biological Chemistry, 292(11), 4395–4410
Musolino, P. L., Gong, Y., Snyder, J. M., Jimenez, S., Lok, J., Lo, E. H., Moser, A. B., Grabowski, E. F., Frosch, M. P., & Eichler, F. S. (2015). Brain endothelial dysfunction in cerebral adrenoleukodystrophy. Brain, 138(11), 3206–3220
Nuutinen, T., Suuronen, T., Kauppinen, A., & Salminen, A. (2010). Valproic acid stimulates clusterin expression in human astrocytes: Implications for Alzheimer’s disease. Neuroscience Letters, 475(2), 64–68
Olsen, E., Kim, Y., Kuzel, T., Pacheco, T., Foss, F., Parker, S., Wang, J., Frankel, S., Lis, J., & Duvic, M. (2006). Vorinostat (suberoylanilide hydroxamic acid, SAHA) is clinically active in advanced cutaneous T-cell lymphoma (CTCL): Results of a phase IIb trial. Journal of Clinical Oncology, 24(18 suppl), 7500–7500
Palmieri, D., Lockman, P. R., Thomas, F. C., Hua, E., Herring, J., Hargrave, E., Johnson, M., Flores, N., Qian, Y., & Vega-Valle, E. (2009). Vorinostat inhibits brain metastatic colonization in a model of triple-negative breast cancer and induces DNA double-strand breaks. Clinical Cancer Research, 15(19), 6148–6157
Peixoto, P., & Lansiaux, A. (2006). Histone-deacetylases inhibitors: from TSA to SAHA. Bulletin du Cancer, 93(1), 27–36
Pipalia, N. H., Subramanian, K., Mao, S., Ralph, H., Hutt, D. M., Scott, S. M., Balch, W. E., & Maxfield, F. R. (2017). Histone deacetylase inhibitors correct the cholesterol storage defect in most Niemann-Pick C1 mutant cells. Journal of Lipid Research, 58(4), 695–708
Price, S., & Dyke, H. J. (2007). Histone deacetylase inhibitors: An analysis of recent patenting activity. Expert Opinion on Therapeutic Patents, 17(7), 745–765
Rauniyar, N., Subramanian, K., Lavallée-Adam, M., Martínez-Bartolomé, S., Balch, W. E., & Yates, J. R. (2015). Quantitative proteomics of human fibroblasts with I1061T mutation in Niemann-Pick C1 (NPC1) protein provides insights into the disease pathogenesis. Molecular & Cellular Proteomics, 14(7), 1734–1749
Reddy, R. G., Surineni, G., Bhattacharya, D., Marvadi, S. K., Sagar, A., Kalle, A. M., Kumar, A., Kantevari, S., & Chakravarty, S. (2019). Crafting carbazole-based vorinostat and tubastatin-A-like histone deacetylase (HDAC) inhibitors with potent in vitro and in vivo neuroactive functions. ACS Omega, 4(17), 17279–17294
Richon, V., Webb, Y., Merger, R., Sheppard, T., Jursic, B., Ngo, L., Civoli, F., Breslow, R., Rifkind, R., & Marks, P. (1996). Second generation hybrid polar compounds are potent inducers of transformed cell differentiation. Proceedings of the National Academy of Sciences, 93(12), 5705–5708
Riessland, M., Ackermann, B., Förster, A., Jakubik, M., Hauke, J., Garbes, L., Fritzsche, I., Mende, Y., Blumcke, I., & Hahnen, E. (2010). SAHA ameliorates the SMA phenotype in two mouse models for spinal muscular atrophy. Human Molecular Genetics, 19(8), 1492–1506
Rooney, A. G., Carson, A., & Grant, R. (2011). Depression in cerebral glioma patients: A systematic review of observational studies. Journal of the National Cancer Institute, 103(1), 61–76
Schroeder, F. A., Lewis, M. C., Fass, D. M., Wagner, F. F., Zhang, Y.-L., Hennig, K. M., Gale, J., Zhao, W.-N., Reis, S., & Barker, D. D. (2013). A selective HDAC 1/2 inhibitor modulates chromatin and gene expression in brain and alters mouse behavior in two mood-related tests. PLoS ONE, 8(8), e71323
Seo, Y. J., Kang, Y., Muench, L., Reid, A., Caesar, S., Jean, L., Wagner, F., Holson, E., Haggarty, S. J., & Weiss, P. (2014). Image-guided synthesis reveals potent blood-brain barrier permeable histone deacetylase inhibitors. ACS Chemical Neuroscience, 5(7), 588–596
Shahbazian, M. D., & Grunstein, M. (2007). Functions of site-specific histone acetylation and deacetylation. Annual Review of Biochemistry, 76, 75–100
She, A., Kurtser, I., Reis, S. A., Hennig, K., Lai, J., Lang, A., Zhao, W.-N., Mazitschek, R., Dickerson, B. C., & Herz, J. (2017). Selectivity and kinetic requirements of HDAC inhibitors as progranulin enhancers for treating frontotemporal dementia. Cell Chemical Biology, 24(7), 892–906
Shim, H., Wei, L., Holder, C. A., Guo, Y., Hu, X. P., Miller, A. H., & Olson, J. J. (2014). Use of high-resolution volumetric MR spectroscopic imaging in assessing treatment response of glioblastoma to an HDAC inhibitor. American Journal of Roentgenology, 203(2), W158–W165
Sukumari-Ramesh, S., Alleyne, C. H., & Dhandapani, K. M. (2016). The histone deacetylase inhibitor suberoylanilide hydroxamic acid (SAHA) confers acute neuroprotection after intracerebral hemorrhage in mice. Translational Stroke Research, 7(2), 141–148
Suraweera, A., O’Byrne, K. J., & Richard, D. J. (2018). Combination therapy with histone deacetylase inhibitors (HDACi) for the treatment of cancer: achieving the full therapeutic potential of HDACi. Frontiers in Oncology, 8, 92
Tanaka, M., Levy, J., Terada, M., Breslow, R., Rifkind, R. A., & Marks, P. A. (1975). Induction of erythroid differentiation in murine virus infected eythroleukemia cells by highly polar compounds. Proceedings of the National Academy of Sciences, 72(3), 1003–1006
Tsankova, N. M., Berton, O., Renthal, W., Kumar, A., Neve, R. L., & Nestler, E. J. (2006). Sustained hippocampal chromatin regulation in a mouse model of depression and antidepressant action. Nature Neuroscience, 9(4), 519
Uchida, S., Hara, K., Kobayashi, A., Otsuki, K., Yamagata, H., Hobara, T., Suzuki, T., Miyata, N., & Watanabe, Y. (2011). Epigenetic status of Gdnf in the ventral striatum determines susceptibility and adaptation to daily stressful events. Neuron, 69(2), 359–372
Ugur, H. C., Ramakrishna, N., Bello, L., Menon, L. G., Kim, S.-K., Black, P. M., & Carroll, R. S. (2007). Continuous intracranial administration of suberoylanilide hydroxamic acid (SAHA) inhibits tumor growth in an orthotopic glioma model. Journal of Neuro-Oncology, 83(3), 267–275
VanderMolen, K. M., McCulloch, W., Pearce, C. J., & Oberlies, N. H. (2011). Romidepsin (Istodax, NSC 630176, FR901228, FK228, depsipeptide): A natural product recently approved for cutaneous T-cell lymphoma. The Journal of Antibiotics, 64(8), 525
Wang, Y., Tu, S., Steffen, D., & Xiong, M. P. (2014). Iron complexation to histone deacetylase inhibitors SAHA and LAQ824 in PEGylated liposomes can considerably improve pharmacokinetics in rats. Journal of Pharmacy & Pharmaceutical Sciences, 17(4), 583
Wash, P. L., Hoffman, T. Z., Wiley, B. M., Bonnefous, C., Smith, N. D., Sertic, M. S., Lawrence, C. M., Symons, K. T., Nguyen, P.-M., & Lustig, K. D. (2008). α-Mercaptoketone based histone deacetylase inhibitors. Bioorganic & Medicinal Chemistry Letters, 18(24), 6482–6485
Wei, L., Hong, S., Yoon, Y., Hwang, S. N., Park, J. C., Zhang, Z., Olson, J. J., Hu, X. P., & Shim, H. (2012). Early prediction of response to Vorinostat in an orthotopic rat glioma model. NMR in Biomedicine, 25(9), 1104–1111
Xu, J., Shi, J., Zhang, J., & Zhang, Y. (2018). Vorinostat: a histone deacetylases (HDAC) inhibitor ameliorates traumatic brain injury by inducing iNOS/Nrf2/ARE pathway. Folia Neuropathologica, 56, 179–186
Yang, C., Rahimpour, S., Lu, J., Pacak, K., Ikejiri, B., Brady, R. O., & Zhuang, Z. (2013). Histone deacetylase inhibitors increase glucocerebrosidase activity in Gaucher disease by modulation of molecular chaperones. Proceedings of the National Academy of Sciences, 110(3), 966–971
Yin, D., Ong, J. M., Hu, J., Desmond, J. C., Kawamata, N., Konda, B. M., Black, K. L., & Koeffler, H. P. (2007). Suberoylanilide hydroxamic acid, a histone deacetylase inhibitor: Effects on gene expression and growth of glioma cells in vitro and in vivo. Clinical Cancer Research, 13(3), 1045–1052
Yu, Q., Feng, N., Hu, Y., Luo, F., Zhao, W., Zhao, W., Liu, Z., Li, M., Xu, L., & Wu, L. (2019). Suberoylanilide hydroxamic acid (SAHA) alleviates the learning and memory impairment in rat offspring caused by maternal sevoflurane exposure during late gestation. The Journal of Toxicological Sciences, 44(3), 177–189
Zagni, C., Floresta, G., Monciino, G., & Rescifina, A. (2017). The search for potent, small-molecule HDACIs in cancer treatment: A decade after vorinostat. Medicinal Research Reviews, 37(6), 1373–1428
Ziemka-Nalecz, M., Jaworska, J., Sypecka, J., & Zalewska, T. (2018). Histone deacetylase inhibitors: A therapeutic key in neurological disorders? Journal of Neuropathology & Experimental Neurology, 77(10), 855–870
Zierfuss, B., Weinhofer, I., Kühl, J. S., Köhler, W., Bley, A., Zauner, K., Binder, J., Martinović, K., Seiser, C., & Hertzberg, C. (2020). Vorinostat in the acute neuroinflammatory form of X-linked adrenoleukodystrophy. Annals of Clinical and Translational Neurology, 7, 639–652
Funding
The work was jointly supported by CSIR-Indian Institute of Chemical Technology, Hyderabad, and Amrita Vishwa Vidyapeetham, Kochi. IICT communication number generated by KIM division, CSIR-IICT [IICT/Pubs./2020/244], for this manuscript is duly acknowledged.
Author information
Authors and Affiliations
Contributions
AKV and PS involved in conceptualization, data curation, formal analysis, funding acquisition, and writing–reviewing and editing. SC participated in formal analysis, funding acquisition, supervision, and writing—review and editing.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Athira, K.V., Sadanandan, P. & Chakravarty, S. Repurposing Vorinostat for the Treatment of Disorders Affecting Brain. Neuromol Med 23, 449–465 (2021). https://doi.org/10.1007/s12017-021-08660-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12017-021-08660-4