Abstract
In this study, we investigated the ability of THP-1 monocytes and macrophages to accumulate lead (Pb) in vitro, relative to Pb concentration and length of exposure. Moreover, we also evaluated the effect of Pb accumulation on cell viability and apoptosis. THP-1 monocytes and macrophages were cultured in the presence of Pb at 1.25 μg/dL, 2.5 μg/dL, 5 μg/dL, and 10 μg/dL. Pb accumulation was examined by inductively coupled plasma and confocal microscopy. The influence of Pb on cell viability, apoptosis, and necrosis was assessed using flow cytometry. The results showed that Pb was toxic to THP-1 monocytes/macrophages even at very low environmental concentrations. Despite the use of low concentrations, both monocytes and macrophages showed dose-dependent and time-dependent decreases in viability, with a simultaneous increase in the percentage of early and late apoptotic cells. Macrophages reacted more strongly to Pb than monocytes. When exposed to the same Pb concentrations, they showed lower viability and a higher percentage of necrotic cells. The incubation time positively correlated with Pb accumulation in a dose-dependent manner. The obtained results indicate that environmental exposure to low Pb concentrations may significantly impair the function of macrophages, with the increased number of apoptotic cells potentially contributing to the development of many pathologies in the brain and whole body.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Despite numerous prevention efforts in recent years [1,2,3,4], lead (Pb) is still considered to be one of the main substances with the greatest potential concern for human health. It was classified in 2017 as a priority list 2 substance by the Agency for Toxic Substances and Disease Registry [5]. Although acute Pb poisoning is currently rare [6, 7], chronic human exposure to low Pb concentrations remains a public health concern, especially in large agglomerations and industrial areas [8,9,10].
The brain is particularly sensitive to the neurodegenerative and neuropathic effects of Pb [11, 12], with even low levels of Pb during body development resulting in cognitive disorders [13,14,15,16,17,18,19]. Later in life, Pb accelerates the progress and symptoms of age-related neurodegenerative diseases such as Alzheimer’s disease and Parkinson’s disease [20,21,22]. The immune system also seems to be one of the more sensitive targets for Pb. Although at low environmental concentrations, Pb is not able to cause overt damage to the main immune cells and does not result in deficiencies in immune cells that are determined by routine tests, it does adversely affect the regulation and function of immune cells [23]. Pb can also act as a strong pro-inflammatory factor in the brain [12] and in the whole body [11].
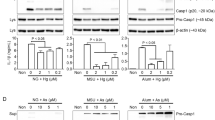
At the cellular level, Pb disrupts the energy state of cells, causing ultrastructural and functional disorders in mitochondrial metabolism by decreasing mitochondrial membrane potential, depleting adenosine triphosphate (ATP) pool, and increasing the production of reactive oxygen species [24]. Moreover, Pb influences the expression of mRNAs in the immediate early genes fos and jun [25,26,27], inhibits DNA repair, and exerts indirect genotoxic effects by acting as a co-mutagen [28]. Our previous data also shows that exposure to Pb in rats decreases the number of hippocampal neurons without severe apoptosis or necrosis [29], although a number of studies suggest that Pb does induce apoptosis in several cell types [29,30,31,32,33,34]. Excessive or disturbed apoptosis is mentioned as a major factor in the formation and propagation of autoimmune, neuropathic, and neurodegenerative diseases induced by Pb exposure [12, 35, 36].
Macrophages play a key role in the development of the aforementioned disorders induced by Pb. This very diverse group, with different functions in different organs [37], includes microglia in the central nervous system [38, 39]. Through their ability to phagocytose, they protect the organism from a wide array of xenobiotics [40, 41], so macrophages constitute a good experimental model to study Pb-induced inflammation of brain tissues [42] to provide a simplified/approximate experimental model to study the effects of Pb exposure in microglia.
In a previous study, we presented the direct effect of Pb on neurodegeneration in the brain, particularly the expression of selected proteins, the activity of enzymes, and the expression of receptors participating in neurodegeneration processes [21, 22, 43]. The aim of this present study was to evaluate Pb accumulation in THP-1 (Tohoku Hospital Pediatrics-1) macrophages after exposure to low Pb concentrations (reflecting chronic environmental exposure to this metal), and the effect of Pb accumulation on apoptosis in these cells. The Pb concentrations and exposure times used in this study have not yet been studied in terms of their effect on apoptosis. Because even small changes in apoptosis induced by environmental factors (such as Pb) might influence genetic instability [44], the results of our study may help to better understand the mechanisms of Pb toxicity.
Materials and Methods
Reagents
THP-1 cells came from the American Type Culture Collection (ATCC, Rockville, USA), while RPMI 1640 culture medium and phosphate-buffered saline (PBS) from Biomed Lublin (BIOMED-LUBIN, Poland). Antibiotics (penicillin and streptomycin) were purchased from Sigma-Aldrich (Poznan, Poland) while fetal bovine serum (FBS) from Gibco (Paisley, UK). Lead acetate (PbAc) used for the preparation of solutions came from Sigma-Aldrich (Poznan, Poland). Phorbol myristate acetate (PMA) required for the transformation of monocytes into macrophages was purchased from Sigma-Aldrich (Poznań, Poland). Annexin V/fluorescein isothiocyanate (FITC) apoptosis evaluation kit came from BD Pharmingen (USA). Nitric acid (V) (HNO3) (Suprapur, Merck, Germany) and Triton (Triton X-100, Sigma) were used for medium digestion in a microwave oven. Inductively coupled plasma (ICP) IV multi-element standard solution (Merck) was used to form a calibration curve. These solutions were made using deionized water (Direct Q UV, Millipore, approx. 18.0 MΩ). The penetration of Pb ions into the cells was examined using Leadmium™ Green AM (molecular probes). Formalin from Sigma-Aldrich (Poznań, Poland) was used to fix the cells on a microscope slide.
Cell Culture and Treatment
RPMI 1640 medium supplemented with 10% FBS, 100 IU/mL penicillin, and 10 μg/mL streptomycin at 37 °C, 5% CO2, and 95% humidity were used to culture the cells. The cells were passaged three times a week to maintain a density below 8 × 105 cells/mL. During the experiment, the cells were incubated with 100 nM PMA for 24 h to differentiate monocytes in macrophages. After three washes with warm PBS, macrophages added to the medium were incubated for 48 h with lead acetate (PbAc) at four concentrations: 1.25 μg/dL, 2.5 μg/dL, 5 μg/dL, 10 μg/dL. The control sample was cultured without the addition of irritants. After the incubation time, the cells were removed from the medium with trypsin and transferred to tubes. Centrifugation (125×g for 6 min) was used to obtain cell pellets used in the next stages of the research.
THP-1 Macrophages Experimental Model
This study used THP-1 leukemia cells (acute monocytic leukemia, FAB type M5), the most popular line in research on inflammatory response mechanisms for the last 30 years, i.e., since the isolation of this cell line [45]. THP-1 leukemia cells are also frequently used in various studies on the physiology or pathology of human monocytes and macrophages [42, 46,47,48,49,50].
PbAc solution with levels of 1.25 μg/dL, 2.5 μg/dL, 5 μg/dL, and 10 μg/dL Pb were used in in vitro cultures of THP-1 monocytes and macrophages. Our previous studies [8] indicate that the former two levels are in the range found in the whole blood and cord blood of young women living in northern Poland and their newborn children. The Pb blood level of 5 μg/dL is the threshold PbB concentration for children and pregnant women, while 10 μg/dL is the threshold PbB level for adults [51].
Flow Cytometry Measurement of Cell Viability
Flow cytometry using Annexin V-FITC staining in combination with iodide propidium (PI) was used to determine THP-1 cell viability. FITC Annexin V and PI identified live cells as negative. Early apoptotic cells were FITC Annexin V positive and PI negative. Late apoptotic/necrotic cells were FITC Annexin V positive and PI positive. A Navios (Beckman Coulter, USA) flow cytometer was used to carry out the tests.
Quantitative Evaluation of Apoptosis by Flow Cytometry
An Annex V/propidium iodide test was used to identify apoptotic and necrotic cells. FITC-conjugated Annex V protein (fluorescein isothiocyanate) was used to identify the externalizations of phosphatidylserine as an early apoptosis marker. Cell membrane damage was detected by binding PI (propidium iodide) to nuclear DNA. A Navios flow cytometer (Beckman Coulter, USA) was used to analyze the cells. Apoptosis was determined using an apoptosis detection kit according to the manufacturer’s instructions.
Lead Ion Accumulation in Cells Assessed by ICP-OES
The levels of Pb in THP-1 macrophages and culture medium were determined following 24- and 48-h exposure to the tested Pb concentrations, with the use of atomic emission spectrometry with excitation in inductively coupled plasma (ICP-OES, ICAP 7400 Duo, Thermo Scientific). A MARS 5, CEM system was used to carry out the microwave digestion of the samples. The samples were first transferred to pure polypropylene tubes, to which 1 mL of 65% HNO3 and 1 mL of non-stabilized 30% hydrogen peroxide (H2O2) were added. The samples were then transferred to Teflon vessels and placed in a microwave digestion oven. First, the samples were gradually heated to 180 °C within 15 min. Then, the temperature was maintained at 180 °C for the next 20 min. Then, the samples were transferred to pure polypropylene tubes. The products of digestion were diluted 20 times. Then, an internal standard yttrium (final concentration in the 0.5-mg/L sample) and 1 mL 1% Triton were added to a 500-μL sample. 0.075% HNO3 was used to supplement the samples to a final volume of 10 mL and stored in a refrigerator (4–8 °C) until analysis. A blank sample was prepared according to the same scheme in which 250 μL of nitric acid (V) was added instead of the test sample. Multi-elemental standard solutions were used to prepare the calibration curve. Deionized water was used to prepare all solutions (~ 18.0 MΩ). Analysis was based on the wavelengths of 220 nm and 353 nm.
Visualization of Lead Ion Accumulation in Cells Evaluated by Confocal Microscopy
Confocal microscopy was used to examine lead ion accumulation in THP-1 macrophages. Macrophages were cultured on glass slides for 48 h in a complete medium with lead acetate at the aforementioned concentrations. Following the completion of cell incubation, the slides were washed with PBS and fixed with 4% buffered formalin for 15 min at room temperature. After fixation and washing with PBS, the cells were permeabilized with 0.5% Triton X-100 solution in PBS. The penetration of Pb ions into the cells was evaluated by adding Leadmium™ Green AM dye. Cells were examined under a confocal microscope (FV1000) with an inverted IX81 microscope (Olympus, Germany). The best signal resolution from Hoechst 33258 and FITC fluorescence was obtained thanks to the use of three-channel acquisition and sequential scanning. Fluorescent images were combined with transient light images.
Statistical Analysis
Statistica 10.0 software was used to analyze the obtained results, using arithmetical mean ± SD for each of the studied parameters. The Shapiro-Wilk W test was used to determine the distribution of results for individual variables. Non-parametric tests were used for further analyses since most of the distributions were not normal. The differences between the groups studied were assessed using the non-parametric Mann-Whitney U test. Differences were deemed statistically significant when p ≤ 0.05.
Results
Lead and Cell Viability
THP-1 monocytes and macrophages were cultured for 48 h with exposure to different PbAc concentrations: 1.25 μg/dL, 2.5 μg/dL, 5 μg/dL, 10 μg/dL. The viability of both monocytes and macrophages decreased with an increase in the applied Pb concentration (Figs. 1 and 2).
The effect of Pb on the vitality of THP-1 monocytes cultured with various lead acetate solutions for 48 h. After incubation cell viability was measured by flow cytometry analysis (n = 6). **Statistically significant difference to control (p ≤ 0.005). ##Statistically significant difference to 10 μg/dL PbAc (p ≤ 0.005). ^Statistically significant difference to 1.25 μg/dL PbAc (p ≤ 0.05). Control—cells incubated in RPMI medium with 10% FBS and without Pb
The effect of lead on the viability of THP-1 macrophages cultured with various lead acetate solutions for 48 h. After incubation, cell viability was measured by flow cytometry analysis (n = 6). **Statistically significant differences in comparison with the control (p ≤ 0.005). ##Statistically significant differences in comparison with 1.25 μg/dL Pb (p ≤ 0.005). ^^Statistically significant differences in comparison with 2.5 μg/dL Pb (p ≤ 0.005), ^(p ≤ 0.05). Statistically significant differences in comparison with 5 μg/dL Pb (p ≤ 0.05). Control—cells incubated in RPMI medium with 10% FBS and without Pb
The THP-1 evaluation of monocytes showed a statistically significant decrease in the viability of cells exposed to Pb at 1.25 μg/dL, 2.5 μg/dL, and 10 μg/dL against the control. The greatest decrease was observed after the use of 10 μg/dL Pb (2.36% reduction vs. control, p ≤ 0.005). Moreover, a significant decrease in the viability of cells treated with 10 μg/dL Pb was observed in comparison with 2.5 μg/dL Pb and 5 μg/dL Pb. A statistically significant difference was also observed between the cells cultured with Pb at 1.25 μg/dL and 5 μg/dL (Fig. 1).While evaluating the viability of THP-1 macrophages, statistically significant differences were found between all studied cell groups. The greatest decrease was observed from the use of 10 μg/dL Pb (5.29% reduction vs. control, p ≤ 0.005) (Fig. 2).
The Effects of Lead on Early Apoptosis
Using the Annexin V-FITC and PI double staining method, the degree of early apoptosis in THP-1 monocytes and macrophages was quantified (Figs. 3 and 4).
The effect of lead on early apoptosis in THP-1 monocytes cultured with various lead acetate solutions for 48 h. After incubation with PbAc, cells were further incubated with Annexin V-FITC (1 ng/mL) and propidium iodide (5 ng/mL) for 30 min in the dark and analyzed by flow cytometry. Results are expressed in percentage of apoptotic cells from n = 6 separate experiments (a). Lower left quadrant shows viable cells. Lower right quadrant, early apoptotic cells. Upper left quadrant, necrotic cells. Upper right quadrant, nonviable late apoptotic cells. Diagram of representative samples (b). **Statistically significant differences in comparison with the control (p ≤ 0.005). ##Statistically significant differences in comparison with 1.25 μg/dL Pb (p ≤ 0.005), #(p ≤ 0.05). ^Statistically significant differences in comparison with 5 μg/dL Pb (p ≤ 0.05). Control—cells incubated in RPMI medium with 10% FBS and without Pb
The effect of lead on early apoptosis in THP-1 macrophages cultured with various lead acetate solutions for 48 h. After incubation with PbAc, cells were further incubated with Annexin V-FITC (1 ng/mL) and propidium iodide (5 ng/mL) for 30 min in the dark and were analyzed by flow cytometry. Results are expressed in percentage of apoptotic cells from n = 6 separate experiments (a). Lower left quadrant shows viable cells. Lower right quadrant, early apoptotic cells. Upper left quadrant, necrotic cells. Upper right quadrant, nonviable late apoptotic cells. Diagram of representative samples (b). *Statistically significant differences in comparison with the control (p ≤ 0.05). #Statistically significant differences in comparison with 1.25 μg/dL Pb (p ≤ 0.05). ^Statistically significant differences in comparison with 2.5 μg/dL Pb (p ≤ 0.05). Control—cells incubated in RPMI medium with 10% FBS and without Pb
Forty-eight hours of incubation of THP-1 monocytes with Pb in the examined concentrations caused a significant dose-dependent increase in the percentage of early apoptotic cells (FITC+, PI−) of 147% (for 1.25 μg/dL) to 275% (for 10 μg/dL) compared with that in of the control (Fig. 3). The percentage of apoptotic cells after incubation with 5 μg/dL and 10 μg/dL was significantly greater than to 1.25 μg/dL. The percentages also differed significantly between the two highest concentrations (5 μg/dL and 10 μg/dL).
THP-1 macrophages exposed for 48 h to PbAc at each of the tested concentrations showed an increase in the percentage of early apoptotic cells compared with the control (from 2.8% for 1.25 μg/dL Pb to 83% for 10 μg/dL Pb). The percentage of early apoptotic cells after incubation in 5 μg/dL Pb and 10 μg/dL Pb also significantly increased compared with that in the lowest Pb concentration. The highest Pb concentrations also showed increased early apoptosis compared with 2.5 μg/dL Pb (Fig. 4).
The Effects of Lead on Late Apoptosis/Necrosis
A 48-h incubation of THP-1 monocytes with PbAc caused a significant increase in the percentage of late apoptotic/necrotic cells (FITC +, PI +) at all tested PbAc concentrations compared with that of control, with the highest increase for 10 μg/dL Pb (99%). The difference was also statistically significant when comparing the cells exposed to the highest Pb concentrations, i.e., between 5 and 10 μg/dL Pb (Fig. 5).
The effect of lead on late apoptosis/necrosis in monocytes cultured with various acetate solutions for 48 h. After incubation with PbAc, cells were harvested by scraping then were incubated with Annexin V-FITC (1 ng/mL) and propidium iodide (5 ng/mL) for 30 min in the dark and analyzed by flow cytometry. Results are expressed in percentage of apoptotic cells from n = 6 separate experiments. **Statistically significant differences in comparison with the control (p ≤ 0.005), *(p ≤ 0.05). ##Statistically significant differences in comparison with 5 μg/dL Pb (p ≤ 0.005). Control—cells incubated in RPMI medium with 10% FBS and without Pb
THP-1 macrophages showed statistically significant differences between each of the applied Pb concentrations. The highest increase in the percentage of apoptotic cells in relation to control was observed after exposure to 10 μg/dL Pb (306% of control) (Fig. 6).
The effect of lead on late apoptosis/necrosis in macrophages cultured with various acetate solutions for 48 h. After incubation, cells were harvested by scraping, then incubated with Annexin V-FITC (1 ng/mL) and propidium iodide (5 ng/mL) for 30 min in the dark and analyzed by flow cytometry. Results are expressed in percentage of apoptotic cells from n = 6 separate experiments. **Statistically significant differences in comparison with the control (p ≤ 0.005). ##Statistically significant differences in comparison with 1.25 μg/dL Pb (p ≤ 0.005). ^^Statistically significant differences in comparison with 2.5 μg/dL Pb (p ≤ 0.005), ^(p ≤ 0.05). Statistically significant differences in comparison with 5 μg/dL Pb (p ≤ 0.05). Control—cells incubated in RPMI medium with 10% FBS and without Pb
The Concentration of Lead in THP-1 Macrophages
Our results indicate that macrophages were more sensitive to Pb than monocytes. Exposed to the same concentrations, they showed lower viability and a higher percentage of necrotic cells. Therefore, the assessment of the degree of accumulation of Pb was performed on THP-1 macrophages. We applied two incubation times: 24 and 48 h (Figs. 7, 8, and 9).
The concentration of lead in THP-1 macrophages after incubation with various acetate solutions. THP-1 macrophages were cultured with lead acetate solutions for 24 h. After incubation, cells were harvested by scraping and subjected to microwave mineralization using MARS 5 system, CEM. Ion accumulation was measured by ICP-OES. The values were expressed as an arithmetic mean (± SD) of n = 6 measurements for each concentration. *Statistically significant differences in comparison with the control (p ≤ 0.05). ##Statistically significant differences in comparison with 1.25 μg/dL Pb (p ≤ 0.005). ^Statistically significant differences in comparison with 2.5 μg/dL Pb (p ≤ 0.05). Control—cells incubated in RPMI medium with 10% FBS and without Pb
The concentration of lead in THP-1 macrophages after incubation with various acetate solutions. THP-1 macrophages were cultured with lead acetate solutions for 48 h. After incubation, cells were harvested by scraping and subjected to microwave mineralization using MARS 5 system, CEM. Ion accumulation was measured by ICP-OES. The values were expressed as an arithmetic mean (± SD) of n = 6 measurements for each concentration. *Statistically significant differences in comparison with the control (p ≤ 0.05). #Statistically significant differences in comparison with 1.25 μg/dL Pb (p ≤ 0.05). ^Statistically significant differences in comparison with 2.5 μg/dL Pb (p ≤ 0.05). %Statistically significant differences in comparison with 5 μg/dL Pb (p ≤ 0.05). Control—cells incubated in RPMI medium with 10% FBS and without Pb
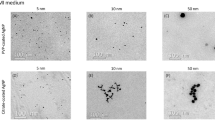
Confocal microscope images of cultured THP-1 macrophages incubated for 24 h (a) or 48 h (c) with Leadmium™ Green AM dye from control and Pb-treated cells; quantitative measurements of the fluorescence intensity after 24-h (b) and 48-h incubation (d). Quantitative measurements of the fluorescence intensity performed by an Asys UVM 340 plate reader, normalized to the number of cells on the plate. The intensity of red-green fluorescence in the cultured with Pb macrophages was significantly higher with respect to control macrophages. Experiments were repeated six times with similar results; therefore, the presented pictures may be deemed representative. The values were expressed as an arithmetic mean (± SD) of n = 6 measurements for each concentration. **Statistically significant differences in comparison with control (p ≤ 0.005). ##Statistically significant differences in comparison with 1.25 μg/dL Pb (p ≤ 0.005), #(p ≤ 0.05). ^^Statistically significant differences in comparison with 2.5 μg/dL Pb (p ≤ 0.005). &&Statistically significant differences in comparison with 5 μg/dL Pb (p ≤ 0.005). Control—cells incubated in RPMI medium with 10% FBS and without Pb
Longer exposure to Pb resulted in a higher Pb accumulation in the cells studied. Both times lead to a significant increase in the accumulation depending on the dose used. Cell evaluation after 24 h showed the highest Pb accumulation after exposure to the highest Pb level (10 μg/dL). Statistically significant differences were observed between the cells cultured with Pb at a concentration of 5 μg/dL and those exposed to 1.25 μg/dL and 2.5 μg/dL Pb, vs. control group (Figs. 7 and 9).
A 48-h incubation resulted in increased accumulation of Pb in cells exposed to 10 μg/dL Pb compared with that in the control, 1.25-μg/dL cells, and 5-μg/dL cells. The increase in the amount of Pb in cells exposed to 5 μg/dL Pb and 2.5 μg/dL Pb was significant in comparison with that in 1.25 μg/dL Pb and control cultures (Figs. 8 and 9).
Discussion
In our experiment, we investigated the influence of lead on apoptosis and necrosis in THP-1 monocytes and macrophages. We also examined the ability of macrophages to accumulate Pb, depending on the length of exposure and various levels of Pb concentrations reflecting environmental exposure in urban areas [8]. As a result of incubation with Pb, THP-1 cells, both monocytes and macrophages, showed a concentration-dependent reduction in viability and an increase in the percentage of early and late apoptotic cells.
Our results are in agreement with the results obtained by other research groups investigating various cell lines and in vivo animal models, showing Pb causing apoptosis of neurons [21, 29, 30, 43], such as in hippocampal neurons [30, 52] and mouse hippocampal neuronal cell line HT-22 [34], retinal cells [31, 53], and human leukemia cells (HL-60) [32, 33]. Only peripheral blood mononuclear cells (MNC) showed no apoptosis even at 500 μM Pb [54]. The concentrations used by other researchers were many times higher than in this study [32,33,34], yet our results showed a significant decrease in viability even after exposure to the very low concentration of 1.25 μg/dL Pb.
The demonstrated sensitivity to much lower Pb concentrations in our study may be due to the use of different research models and incubation times. Karri et al. hypothesized that the duration of exposure is a key factor influencing the occurrence of toxic or lethal Pb effect on the cells studied. They tested three exposure periods: acute (1 day), subchronic (3 days), and chronic (8 days) assays. They chose hippocampal cell line HT-22 as the research model, and 10 different Pb concentrations ranging from 10 to 100 μM Pb. A clear, time- and concentration-dependent cytotoxic effect of Pb on the examined cells was observed [34].
The mechanism of Pb entry into the target cells is still not well understood [55]. Thanks to its ability to mimic other elements, Pb most likely uses the normal function of protein transporters. By replacing physiologically essential cations (e.g., Ca2+), it can enter the cell interior through passive and active transport processes [56]. The basic mechanism of active transport, i.e., the calcium pump which uses ATP hydrolysis to transport calcium into cells, is considered specific for Ca2+ ions, but there is some evidence that several other bivalent cations can replace them, including Pb2+ ions [57, 58]. Passive transport of Pb, thanks to which Pb may pass through the cell membrane in any direction, is stimulated by bicarbonates (HCO3−) and does not depend on the external concentrations of Na+, K+, or Ca2+ [59].
An in vivo study on a rat model suggested that pH-dependent passive Pb transport in the form of monovalent permeating species of the type PbOH+ is the mechanism behind the breach of the blood-brain barrier by Pb [60], resulting in Pb accumulation in different parts of the brain tissue [61]. Under physiological conditions, macrophages formed from monocytes become long-lived cells, develop specialized functions, and are therefore more resistant to constitutive apoptosis than monocytes [62]. Our results, however, suggest that macrophages are more sensitive to Pb than monocytes, as exposure to the same concentrations resulted in a lower viability and higher percentage of necrotic cells. It is possible that Pb significantly interfered with macrophage functions and thus, the degenerated cells more readily entered the apoptotic pathway.
Pb accumulation by macrophages can have serious cytotoxic and pro-inflammatory consequences [11]. For example, it may increase lipid peroxidation in macrophages [63,64,65,66,67,68,69,70], with the accumulation of oxidized lipid leading to the formation of foam cells and the development of inflammation [37, 71,72,73].
Chronic exposure to Pb also results in elevated concentrations of total cholesterol and triglycerides [74, 75], with increased concentrations of fatty acids in blood and macrophages being an important factor in the development of atherosclerosis [76]. Baranowska-Bosiacka et al. showed that environmental Pb concentrations may also be a risk factor affecting fatty acid concentrations, inducing oxidative stress and increasing malondialdehyde (MDA) concentration in macrophages, leading to foam cell formation and development of inflammation [77].
The toxicity of Pb can also be associated with its influence on the activity of antioxidant enzymes. A study [78] evaluated the level of oxidative stress in rat brains exposed pre- and neonatal to Pb, expression of mRNAs, proteins, and activity of the most important antioxidant enzymes (copper/zinc superoxide dismutase (SOD1), manganese superoxide dismutase (SOD2), glutathione peroxidase (GPx), phospholipid hydroperoxide glutathione peroxidase (GPx4), catalase (CAT), glutathione reductase (GSR), and glutathione (GSH)). Despite the low level of Pb in the blood (10 μg/dL), a decrease in the activity of some enzymes was observed, as well as in their mRNA and protein expression, associated with an increase in MDA and CAT expression, especially in the hippocampus. The same paper also suggested that a disturbed oxidant-antioxidant balance in both neurons and glia may be a potential mechanism underlying the observed adverse effects of Pb [78].
The apoptosis of macrophages observed in our experiment may occur through the activation of many different pathways, e.g., through the Fas pathway and mitochondrial pathways. FasL is activated on the surface of cells overloaded with free cholesterol [79] and an increase in Bax levels and a release of cytochrome c result in the activation of caspase-9 and other effector caspases [80]. The accumulation of free cholesterol in the endoplasmic reticulum (ER) of cells also causes the activation of unfolded protein response (UPR) and C/EBP homologous protein (CHOP)–induced apoptosis via p38 mitogen-activated protein kinases (MAPK). Devries-Seimon et al. believe that this pathway requires the action of scavenger receptor class A (SRA) and the c-Jun NH2-terminal kinase pathway [81].
Heavy metals other than Pb can also initiate macrophage apoptosis. For example, macrophages exposed to beryllium produce an increased amount of reactive oxygen species (ROS) [82] and undergo apoptosis due to the activation of caspases [83]. Macrophages exposed to mercury die as a result of the induction of apoptosis and necrosis through different activation paths. Exposure to Hg increases the intracellular concentration of Ca2+ increases, leading to increased production of ROS which then activates p38, responsible for elevated apoptosis and necrosis of cells through its influence on caspase-3 and expression of tumor necrosis factor α (TNF-α) [84]. A study on cadmium-incubated macrophages has shown apoptosis induced via mitochondrial pathways, with a decrease in membrane potential of mitochondria and an increase in ROS production [49]. Cadmium can also activate extracellular signal-regulated kinase (ERK) [85] and JNK MAPKs [86, 87] and increases the expression of mRNA Bax while decreasing the expression of Bcl-2 (increase in Bax/Bcl-2 ratio) [87,88,89,90,91]. Olszowski et al. showed that these mechanisms can be induced by cadmium event at nanomolar concentrations [49].
Lead-induced apoptosis also seems to depend on mitochondria, as Pb is able to affect mitochondrial calcium homeostasis. Both calcium and lead depolarize mitochondrial membranes by opening permeability transition pores (PTP) [53]. Pb affects the levels of intercellular oxidants [92], adenylate energy charge value (AEC), and ATP production [24, 93, 94] and increases ROS production, all of which—through constant demand for antioxidants—lead to a depletion of resources [95]. This results in the destabilization of calcium homeostasis via disrupted electron transport, decreased ATP concentration, and membrane ion channel disruption [96], ultimately leading to cell apoptosis. Increased ROS concentration results in a disturbance of the cellular lipid bi-layer and thus disturbs the cellular transport of Ca2+. Compromised cellular membranes are indicated by a loss in mitochondrial membrane potential (MMP), resulting in disturbances in the balance of such molecules as Bcl-2 and Bax [97]. The changed Bcl-2/Bax ratio causes a release of cytochrome c and activation of caspases leading to apoptosis [98, 99]. Finally, research on the brains of rats with long-term exposure to Pb showed a significant increase in ROS, neuronal synthase of nitric oxide, and intracellular calcium levels; a decrease in membrane potential; a cytochrome c release; and changes in the Bcl-2/Bax ratio, which confirm mitochondrial-dependent Pb-induced apoptosis [100].
In conclusion, despite the use of low Pb concentrations in our experiment, both monocytes and macrophages showed both a concentration and time-dependent decrease in viability, accompanied by a simultaneous increase in the percentage of early and late apoptotic cells. Macrophages seemed to react more strongly to Pb and therefore were selected to evaluate the Pb accumulation after 24 and 48 h of incubation. Longer exposure times resulted in a stronger accumulation, with a similar dependence on concentration. The results indicate that environmental exposure to low concentrations of Pb compounds may significantly impair the function of macrophages. The resulting increase in the number of apoptotic cells may contribute to the development of many pathologies in the entire organism. Our research indicates that blood lead levels as low as 1.25 g/dL can cause apoptotic changes in monocytes and macrophages. This suggests that the safety threshold Pb levels should even lower. In addition, we should try to further curb environmental exposure to Pb, as well as continue intense research on the mechanisms of Pb toxicity.
References
Tong S, von Schirnding YE, Prapamontol T (2000) Environmental lead exposure: a public health problem of global dimensions. Bull World Health Organ 78:1068–1077
Genaidy AM, Sequeira R, Tolaymat T, Kohler J, Rinder M (2009) Evidence-based integrated environmental solutions for secondary lead smelters: pollution prevention and waste minimization technologies and practices. Sci Total Environ 407:3239–3268. https://doi.org/10.1016/j.scitotenv.2009.01.025
Gomes GMF, Mendes TF, Wada K (2011) Reduction in toxicity and generation of slag in secondary lead process. J Clean Prod 19:1096–1103. https://doi.org/10.1016/j.jclepro.2011.01.006
United Nations Environment Programme (UNEP), Leaded Petrol Phase-out: global status as at March 2017 (2017) IOP Publishing PhysicsWeb. http://wedocs.unep.org/bitstream/handle/20.500.11822/17542/MapWorldLead_March2017.pdf?sequence=1&isAllowed=y. Accessed 5 August 2019
CDC, Agency for Toxic Substances and Disease Registry (ATSDR) (2017) IOP Publishing PhysicsWeb. https://www.atsdr.cdc.gov/SPL/#2017spl. Accessed 7 August 2019
Flora G, Gupta D, Tiwari A (2012) Toxicity of lead: a review with recent updates. Interdiscip Toxicol 5:47–58. https://doi.org/10.2478/10102-012-0009-2
Vorvolakos T, Arseniou S, Samakouri M (2016) There is no safe threshold for lead exposure: a literature review. Psychiatriki 27:204–214. https://doi.org/10.22365/jpsych.2016.273.204
Baranowska-Bosiacka I, Kosińska I, Jamioł D, Gutowska I, Prokopowicz A, Rębacz-Maron E, Goschorska M, Olszowski T, Chlubek D (2016) Environmental lead (Pb) exposure versus fatty acid content in blood and milk of the mother and in the blood of newborn children. Biol Trace Elem Res 170:279–287. https://doi.org/10.1007/s12011-015-0482-5
Needleman H (2004) Lead poisoning. Annu Rev Med 55:209–222. https://doi.org/10.1146/annurev.med.55.091902.103653
Rapisarda V, Ledda C, Ferrante M, Fiore M, Cocuzza S, Bracci M, Fenga C (2016) Blood pressure and occupational exposure to noise and lead (Pb): a cross-sectional study. Toxicol Ind Health 32:1729–1736. https://doi.org/10.1177/0748233715576616
Metryka E, Chibowska K, Gutowska I, Falkowska A, Kupnicka P, Barczak K, Chlubek D, Baranowska-Bosiacka I (2018) Lead (Pb) exposure enhances expression of factors associated with inflammation. Int J Mol Sci 19:1813. https://doi.org/10.3390/ijms19061813
Chibowska K, Baranowska-Bosiacka I, Falkowska A, Gutowska I, Goschorska M, Chlubek D (2016) Effect of lead (Pb) on inflammatory processes in the brain. Int J Mol Sci 17:2140. https://doi.org/10.3390/ijms17122140
Sanders T, Liu Y, Buchner V, Tchounwou PB (2009) Neurotoxic effects and biomarkers of lead exposure: a review. Rev Environ Health 24:15–45. https://doi.org/10.1515/REVEH.2009.24.1.15
Jakubowski M (2011) Low-level environmental lead exposure and intellectual impairment in children-the current concepts of risk assessment. Int J Occup Med Environ Health 24:1–17. https://doi.org/10.2478/s13382-011-0009-z
Canfield RL, Henderson JCR, Cory-Slechta DA, Cox C, Jusko TA, Lanphear BP (2003) Intellectual impairment in children with blood lead concentrations below 10 microg per deciliter. N Engl J Med 348:1517–1526. https://doi.org/10.1056/NEJMoa022848
Lanphear BP, Hornung R, Khoury J, Yolton K, Baghurst P, Bellinger DC, Canfield RL, Dietrich KN, Bornschein R, Greene T, Rothenberg SJ, Needleman HL, Schnaas L, Wasserman G, Graziano J, Roberts R (2005) Low-level environmental lead exposure and children’s intellectual function: an international pooled analysis. Environ Health Perspect 113:894–899. https://doi.org/10.1289/ehp.7688
Bellinger D, Dietrich KN (1994) Low-levels lead exposure and cognitive function in children. Pediatr Ann 23:600–605. https://doi.org/10.3928/0090-4481-19941101-08
Bellinger D, Stiles K, Needleman HL (1992) Low-level lead exposure intelligenceand academic achievement. A long-term follow-up study. Pediatrics 90:855–861
Giddabasappa A, Hamilton WR, Chaney S, Xiao W, Johnson JE, Mukherjee S, Fox DA (2011) Low-level gestational lead exposure increases retinal progenitor cell proliferation and rod photoreceptor and bipolar cell neurogenesis in mice. Environ Health Perspect 119:71–77. https://doi.org/10.1289/ehp.1002524
Charlet L, Chapron Y, Faller P, Kirsch R, Stone AT, Baveye PC (2012) Neurodegenerative diseases and exposure to the environmental metals Mn, Pb, and Hg. Coord Chem Rev 256:2147–2163. https://doi.org/10.1016/j.ccr.2012.05.012
Gąssowska M, Baranowska-Bosiacka I, Moczydłowska J, Frontczak-Baniewicz M, Gewartowska M, Strużyńska L, Gutowska I, Chlubek D, Adamczyk A (2016) Perinatal exposure to lead (Pb) induces ultrastructural and molecular alterations in synapses of rat offspring. Toxicology 373:13–29. https://doi.org/10.1016/j.tox.2016.10.014
Baranowska-Bosiacka I, Falkowska A, Gutowska I, Gąssowska M, Kolasa-Wołosiuk A, Tarnowski M, Chibowska K, Lubkowska A, Chlubek D (2017) Glycogen metabolism in brain and neurons - astrocytes metabolic cooperation can be altered by pre- and neonatal lead (Pb) exposure. Toxicology 390:146–158. https://doi.org/10.1016/j.tox.2017.09.007
Dietert RR, Piepenbrink MS (2006) Lead and immune function. Crit Rev Toxicol 36:359–385. https://doi.org/10.1080/10408440500534297
Baranowska-Bosiacka I, Gutowska I, Marchetti C, Rutkowska M, Marchlewicz M, Kolasa A, Prokopowicz A, Wiernicki I, Piotrowska K, Baśkiewicz M, Safranow K, Wiszniewska B, Chlubek D (2011) Altered energy status of primary cerebellar granule neuronal cultures from rats exposed to lead in the pre- and neonatal period. Toxicology 280:24–32. https://doi.org/10.1016/j.tox.2010.11.004
Braga MF, Pereira EF, Mike A, Albuquerque EX (2004) Pb2+ via protein kinase C inhibits nicotinic cholinergic modulation of synaptic transmission in the hippocampus. J Pharmacol Exp Ther 311:700–710. https://doi.org/10.1124/jpet.104.070466
Murakami K, Feng G, Chen SG (1993) Inhibition of brain protein kinase C subtypes by lead. J Pharmacol Exp Ther 264:757–761
Tomsig JL, Suszkiw JB (1995) Multisite interactions between Pb2+ and protein kinase C and its role in norepinephrine release from bovine adrenal chromaffin cells. J Neurochem 64:2667–2673
Beyersman D (1994) Interactions in metal carcinogenicity. Toxicol Lett 72:333–338
Baranowska-Bosiacka I, Strużyńska L, Gutowska I, Machalinska A, Kolasa A, Kłos P, Czapski GA, Kurzawski M, Prokopowicz A, Marchlewicz M, Safranow K, Machalinski B, Wiszniewska B, Chlubek D (2013) Perinatal exposure to lead induces morphological, ultrastructural and molecular alterations in the hippocampus. Toxicology 303:187e200–187e200. https://doi.org/10.1016/j.tox.2012.10.027
Olivera A, Rosenfeldt HM, Bektas M, Wang F, Ishii I, Chun J, Milstien S, Spiegel S (2003) Sphingosine kinase type 1 induces G12/13-mediated stress fiber formation, yet promotes growth and survival independent of G protein-coupled receptors. J Biol Chem 278:46452e46460–46452e46460. https://doi.org/10.1074/jbc.M308749200
Sobieniecki A, Gutowska I, Machalińska A, Chlubek D, Baranowska-Bosiacka I (2015) Retinal degeneration following lead exposure – functional aspects. Postepy Hig Med Dosw (Online) 69:1251–1258. https://doi.org/10.5604/17322693.1180649
Yedjou CG, Milner JN, Howard CB, Tchounwou PB (2010) Basic apoptotic mechanisms of Lead toxicity in human leukemia (Hl-60) cells. Int J Environ Res Public Health 7:2008–2017. https://doi.org/10.3390/ijerph7052008
Yedjou CG, Tchounwou HM, Tchounwou PB (2015) DNA damage, cell cycle arrest, and apoptosis induction caused by lead in human leukemia cells. Int J Environ Res Public Health 13:56. https://doi.org/10.3390/ijerph13010056
Karri V, Kumar V, Ramos D, Oliveira E, Schuhmacher M (2018) Comparative in vitro toxicity evaluation of heavy metals (lead, cadmium, arsenic, and methylmercury) on HT-22 hippocampal cell line. Biol Trace Elem Res 184:226–239. https://doi.org/10.1007/s12011-017-1177-x
Elmore S (2007) Apoptosis: a review of programmed cell death. Toxicol Pathol 35:495–516. https://doi.org/10.1080/01926230701320337
Mishra KP (2009) Lead exposure and its impact on immune system: a review. Toxicol in Vitro 23:969–972. https://doi.org/10.1016/j.tiv.2009.06.014
Nazimek K, Bryniarski K (2012) The biological activity of macrophages in health an disease. Postepy Hig Med Dosw 66:507–520. https://doi.org/10.5604/17322693.1004080 (Article in Polish)
Mildner A, Schmidt H, Nitsche M, Merkler D, Hanisch UK, Mack M, Heikenwalder M, Brück W, Priller J, Prinz M (2007) Microglia in the adult brain arise from Ly-6ChiCCR2+ monocytes only under defined host conditions. Nat Neurosci 10:1544–1553. https://doi.org/10.1038/nn2015
Greter M, Merad M (2013) Regulation of microglia development and homeostasis. Glia 61:121–127. https://doi.org/10.1002/glia.22408
Kumar V (2019) Macrophages: the potent immunoregulatory innate immune cells. Macrophage Activation - Biology and Disease IOP IntechOpen. https://doi.org/10.5772/intechopen.88013. Accessed 18 May 2020
Laskin DL, Gardner CR, Laskin JD (2010) Phagocytes. In: McQueen CA (ed) Comprehensive toxicology, vol 5, 2nd edn. Elsevier Science, Amsterdam, pp 133–153. https://doi.org/10.1016/B978-0-08-046884-6.00607-2 Accessed 18 May 2020
Goschorska M, Baranowska-Bosiacka I, Gutowska I, Tarnowski M, Piotrowska K, Metryka E, Safranow K, Chlubek D (2018) Effect of acetylcholinesterase inhibitors donepezil and rivastigmine on the activity and expression of cyclooxygenases in a model of the inflammatory action of fluoride on macrophages obtained from THP-1 monocytes. Toxicology 406-407:9–20. https://doi.org/10.1016/j.tox.2018.05.007
Gąssowska M, Baranowska-Bosiacka I, Moczydłowska J, Tarnowski M, Pilutin A, Gutowska I, Strużyńska L, Chlubek D, Adamczyk A (2016) Perinatal exposure to lead (Pb) promotes tau phosphorylation in the rat brain in a GSK-3â and CDK5 dependent manner: relevance to neurological disorders. Toxicology 347-349:17–28. https://doi.org/10.1016/j.tox.2016.03.002
Wodarz D, Komarova NL (2014) Competition between genetically stable and unstable cells. In Dynamics of cancer: mathematical foundations of oncology World Scientific Singapore 57–80
Qin Z (2012) The use of THP-1 cells as a model for mimicking the function and regulation of monocytes and macrophages in the vasculature. Atherosclerosis 221:2–11. https://doi.org/10.1016/j.atherosclerosis.2011.09.003
Chanput W, Mes JJ, Wichers HJ (2014) THP-1 cell line: an in vitro cell model for immune modulation approach. Int Immunopharmacol 23:37–45. https://doi.org/10.1016/j.intimp.2014.08.002
Streit WJ, Miller KR, Lopes KO, Njie E (2008) Microglial degeneration in the aging brain - bad news for neurons? Front Biosci 13:3423–3438. https://doi.org/10.2741/2937
An C, Shi Y, Li P, Hu X, Yu G, Stetler RA, Leak RK, Gao Y, Sun BL, Zheng P, Chen J (2014) Molecular dialogues between the ischemic brain and the peripheral immune system: dualistic roles in injury and repair. Prog Neurobiol 115:6–24. https://doi.org/10.1016/j.pneurobio.2013.12.002
Olszowski T, Baranowska-Bosiacka I, Gutowska I, Piotrowska K, Mierzejewska K, Korbecki J, Kurzawski M, Tarnowski M, Chlubek D (2015) The effects of cadmium at low environmental concentrations on THP-1 macrophage apoptosis. Int J Mol Sci 16:21410–21427. https://doi.org/10.3390/ijms160921410
Korbecki J, Baranowska-Bosiacka I, Gutowska I, Piotrowska K, Chlubek D (2015) Cyclooxygenase-1 as the main source of proinflammatory factors after sodium orthovanadate treatment. Biol Trace Elem Res 163:103–111. https://doi.org/10.1007/s12011-014-0176-4
CDC (2012) Low level Lead exposure harms children: a renewed call for primary prevention. Report of the Advisory Committee on Childhood Lead Poisoning Prevention of the Centers for Disease Control and Prevention. IOP Publishing PhysicsWeb. https://www.cdc.gov/nceh/lead/acclpp/final_document_030712.pdf. Accessed 25 August 2019
Sharifi AM, Mousavi SH, Jorjani M (2010) Effect of chronic lead exposure on proapoptotic Bax and anti-apoptotic Bcl-2 protein expression in rat hippocampus in vivo. Cell Mol Neurobiol 30:769e774–769e774. https://doi.org/10.1007/s10571-010-9504-1
He L, Poblenz AT, Medrano CJ, Fox DA (2000) Lead and calcium produce rod photoreceptor cell apoptosis by opening the mitochondrial permeability transition pore. J Biol Chem 275:12175–12184. https://doi.org/10.1074/jbc.275.16.12175
de la Fuente H, Portales-Pérez D, Baranda L, Díaz-Barriga F, Saavedra-Alanís V, Layseca E, González-Amaro R (2002) Effect of arsenic, cadmium and lead on the induction of apoptosis of normal human mononuclear cells. Clin Exp Immunol 129:69–77. https://doi.org/10.1046/j.1365-2249.2002.01885.x
Bridges CC, Zalups RK (2005) Molecular and ionic mimicry and the transport of toxic metals. Toxicol Appl Pharmacol 204:274–308. https://doi.org/10.1016/j.taap.2004.09.007
Garza A, Vega R, Soto E (2006) Cellular mechanisms of lead neurotoxicity. Med Sci Monit 12:RA57–RR65
Simons TJ (1993) Lead transport and binding by human erythrocytes in vitro. J Physiol 423:307–313
Tomsig JL, Suszkiw JB (1991) Permeation of Pb2+ through calcium channels: fura-2 measurements of voltage- and dihydropyridine-sensitive Pb2+ entry in isolated bovine chromaffin cells. Biochim Biophys Acta 1069:197–200. https://doi.org/10.1016/0005-2736(91)90124-Q
Simons TJB (1986) Passive transport and binding of lead by human red blood cells. J Physiol 378:267–286
Deane R, Bradbury MWB (1990) Transport of lead-203 at the blood-brain barrier during short cerebrovascular perfusion with saline in the rat. J Neurochem 54:905–914. https://doi.org/10.1111/j.1471-4159.1990.tb02337.x
Steuerwald AJ, Blaisdell FS, Geraghty CM, Parsons PJ (2014) Regional distribution and accumulation of lead in caprine brain tissues following a long-term Oral dosing regimen. J Toxic Environ Health A 77:663–678. https://doi.org/10.1080/15287394.2014.880328
Daigneault M, Preston JA, Marriott HM, Whyte MK, Dockrell DH (2010) The identification of markers of macrophage differentiation in PMA-stimulated THP-1 cells and monocyte-derived macrophages. PLoS One 5:e8668. https://doi.org/10.1371/journal.pone.0008668
Shafiq-ur-Rehman (2013) Effect of lead on lipid peroxidation, phospholipids composition, and methylation in erythrocyte of human. Biol Trace Elem Res 154:433–439. https://doi.org/10.1007/s12011-013-9745-1
Kasperczyk S, Birkner E, Kasperczyk A, Kasperczyk J (2005) Lipids, lipid peroxidation and 7-ketocholesterol in workers exposed to lead. Hum Exp Toxicol 24:287–295. https://doi.org/10.1191/0960327105ht528oa
Kasperczyk S, Kasperczyk A, Ostalowska A, Dziwisz M, Birkner E (2004) Activity of glutathione peroxidase, glutathione reductase, and lipid peroxidation in erythrocytes in workers exposed to lead. Biol Trace Elem Res 102:61–72. https://doi.org/10.1385/bter:102:1-3:061
Kasperczyk S, Słowińska-Łożyńska L, Kasperczyk A, Wielkoszyński T, Birkner E (2015) The effect of occupational lead exposure on lipid peroxidation, protein carbonylation, and plasma viscosity. Toxicol Ind Health 31:1165–1171. https://doi.org/10.1177/0748233713491804
Abd Allah ES, Badary DM (2017) Folic acid protects against lead acetate-induced hepatotoxicity by decreasing NF-ęB, IL-1â production and lipid peroxidation mediated cell injury. Pathophysiology 24:39–44. https://doi.org/10.1016/j.pathophys.2017.02.002
Vaziri ND, Ding Y, Ni Z, Gonick HC (1997) Altered nitric oxide metabolism and increased oxygen free radical activity in lead-induced hypertension: effect of lazaroid therapy. Kidney Int 52:1042–1046
Knowles SO, Donaldson WE (1996) Dietary lead alters fatty acid composition and membrane peroxidation in chick liver microsomes. Poult Sci 75:1498–1500. https://doi.org/10.3382/ps.0751498
Gonick HC, Ding Y, Bondy SC, Ni Z, Vaziri ND (1997) Lead-induced hypertension: interplay of nitric oxide and reactive oxygen species. Hypertension 30:1487–1492. https://doi.org/10.1161/01.hyp.30.6.1487
Matsuura E, Hughes GR, Khamashta MA (2008) Oxidation of LDL and its clinical implication. Autoimmun Rev 7:558–566. https://doi.org/10.1016/j.autrev.2008.04.018
Mizuno Y, Jacob RF, Mason RP (2011) Inflammation and the development of atherosclerosis. J Atheroscler Thromb 18:351–358. https://doi.org/10.5551/jat.7591
Johnson JL, Newby AC (2009) Macrophage heterogeneity in atherosclerotic plaques. Curr Opin Lipidol 20:370–378. https://doi.org/10.1097/MOL.0b013e3283309848
Kristal-Boneh E, Coller D, Froom P, Harari G, Ribak J (1999) The association between occupational lead exposure and serum cholesterol and lipoprotein levels. Am J Public Health 89:1083–1097
Ademuyiwa O, Ugbaja RN, Idumebor F, Adebawo O (2005) Plasma lipid profiles and risk of cardiovascular disease in occupational lead exposure in Abeokuta, Nigeria. Lipids Health Dis 4:19. https://doi.org/10.1186/1476-511X-4-19
Chen C, Khismatullin DB (2015) Oxidized low-density lipoprotein contributes to atherogenesis via co-activation of macrophages and mast cells. PLoS One 10:e0123088. https://doi.org/10.1371/journal.pone.0123088
Baranowska-Bosiacka I, Olszowski T, Gutowska I, Korbecki J, Rębacz-Maron E, Barczak K, Lubkowska A, Chlubek D (2019) Fatty acid levels alterations in THP-1 macrophages cultured with lead (Pb). J Trace Elem Med Biol 52:222–231. https://doi.org/10.1016/j.jtemb.2019.01.003
Baranowska-Bosiacka I, Gutowska I, Marchlewicz M, Marchetti C, Kurzawski M, Dziedziejko V, Kolasa A, Olszewska M, Rybicka M, Safranow K, Nowacki P, Wiszniewska B, Chlubek D (2012) Disrupted pro- and antioxidative balance as a mechanism of neurotoxicity induced by perinatal exposure to lead. Brain Res 1435:56–71. https://doi.org/10.1016/j.brainres.2011.11.062
Yao PM, Tabas I (2000) Free cholesterol loading of macrophages induces apoptosis involving the fas pathway. J Biol Chem 275:23807–23813. https://doi.org/10.1074/jbc.M002087200
Yao PM, Tabas I (2001) Free cholesterol loading of macrophages is associated with widespread mitochondrial dysfunction and activation of the mitochondrial apoptosis pathway. J Biol Chem 276:42468–42476. https://doi.org/10.1074/jbc.M101419200
Devries-Seimon T, Li Y, Yao PM, Stone E, Wang Y, Davis RJ, Flavell R, Tabas I (2005) Cholesterol-induced macrophage apoptosis requires ER stress pathways and engagement of the type A scavenger receptor. J Cell Biol 171:61–73. https://doi.org/10.1083/jcb.200502078
Sawyer RT, Dobis DR, Goldstein M, Velsor L, Maier LA, Fontenpot AP, Silveira L, Newman LS, Day BJ (2005) Beryllium stimulated reactive oxygen species and macrophage apoptosis. Free Radic Biol Med 38:928–937. https://doi.org/10.1016/j.freeradbiomed.2004.12.014
Sawyer RT, Fadok VA, Kittle LA, Majer LA, Newman LS (2000) Beryllium-stimulated apoptosis in macrophage cell lines. Toxicology 149:129–142. https://doi.org/10.1016/s0300-483x(00)00237-7
Kim SH, Sharma RP (2004) Mercury-induced apoptosis and necrosis in murine macrophages: role of calcium-induced reactive oxygen species and p38 mitogen-activated protein kinase signaling. Toxicol Appl Pharmacol 196:47–57. https://doi.org/10.1016/j.taap.2003.11.020
Martin P, Poggi MC, Chambard JC, Boulukos KE, Pognonec P (2006) Low dose cadmium poisoning results in sustained ERK phosphorylation and caspase activation. Biochem Biophys Res Commun 350:803–807. https://doi.org/10.1016/j.bbrc.2006.09.126
Jiang C, Yuan Y, Hu F, Wang Q, Zhang K, Wang Y, Gu J, Liu X, Bian J, Liu Z (2014) Cadmium induces PC12 cells apoptosis via an extracellular signal-regulated kinase and c-Jun N-terminal kinase-mediated mitochondrial apoptotic pathway. Biol Trace Elem Res 158:249–258. https://doi.org/10.1007/s12011-014-9918-6
Yiran Z, Chenyang J, Jiajing W, Yan Y, Jianhong G, Jianchun B, Xuezhong L, Zongping L (2013) Oxidative stress and mitogen-activated protein kinase pathways involved in cadmium-induced BRL 3A cell apoptosis. Oxidative Med Cell Longev 2013:516051–516012. https://doi.org/10.1155/2013/516051
Mao WP, Ye JL, Guan ZB, Zhao JM, Zhang C, Zhang NN, Jiang P, Tian T (2007) Cadmium induces apoptosis in human embryonic kidney (HEK) 293 cells by caspase-dependent and - independent pathways acting on mitochondria. Toxicol in Vitro 21:343–354. https://doi.org/10.1016/j.tiv.2006.09.004
Pulido MD, Parrish AR (2003) Metal-induced apoptosis: mechanisms. Mutat Res 533:227–241. https://doi.org/10.1016/j.mrfmmm.2003.07.015
Wang Y, Wu Y, Luo K, Liu Y, Zhou M, Yan S, Shi H, Cai Y (2013) The protective effects of selenium on cadmium-induced oxidative stress and apoptosis via mitochondria pathway in mice kidney. Food Chem Toxicol 58:61–67. https://doi.org/10.1016/j.fct.2013.04.013
Ye JL, Mao WP, Wu AL, Zhang NN, Zhang C, Yu YJ, Zhou L, Wei CJ (2007) Cadmium-induced apoptosis in human normal liver L-02 cells by acting on mitochondria and regulating Ca(2+) signals. Environ Toxicol Pharmacol 24:45–54. https://doi.org/10.1016/j.etap.2007.01.007
Zamzami N, Kroemer G (2001) The mitochondrion in apoptosis: how Pandora’s box opens. Nat Rev Mol Cell Biol 2:67–71. https://doi.org/10.1038/35048073
Martinou JC, Green DR (2001) Breaking the mitochondrial barrier. Nat Rev Mol Cell Biol 2:63–67. https://doi.org/10.1038/35048069
Marchlewicz M, Baranowska-Bosiacka I, Kolasa A, Kondarewicz A, Chlubek D, Wiszniewska B (2009) Disturbances of energetic metabolism in rat epididymal epithelial cells as a consequence of chronic lead intoxication. BioMetals 22:877–888. https://doi.org/10.1007/s10534-009-9238-z
Ercal N, Treratphan P, Hammond TC, Mathews RH, Grannemann NH, Spitz DR (1996) In vivo indices of oxidative stress in lead exposed C57BL/6 mice are reduced by treatment with meso-2, 3-dimercaptosuccinic acid or N-acetyl cysteine. Free Radic Biol Med 21:157–161. https://doi.org/10.1016/0891-5849(96)00020-2
Zughaib ME, Tang XL, Sun JZ, Bolli R (1994) Myocardial reperfusion injury: fact or myth? A 1993 appraisal of a seemingly endless controversy. Ann N Y Acad Sci 723:218–228
He L, Perkins GA, Poblenz AT, Harris JB, Hung M, Ellisman MH, Fox DA (2003) Bcl-XL overexpression blocks bax-mediated mitochondrial contact sites formation and apoptosis in rod photoreceptors of lead exposed mice. Proc Natl Acad Sci U S A 100:1022–1027. https://doi.org/10.1073/pnas.0333594100
Antonsson B, Montessuit S, Lauper S, Eskes R, Martinou JC (2000) Bax oligomerization is required for channel-forming activity in liposomes and trigger cytochrome c release from mitochondria. Biochem J 345:271–278
Hengartner MO (2000) The biochemistry of apoptosis. Nature 407:770–776
Flora SJ, Saxena G, Mehta A (2007) Reversal of lead-induced neuronal apoptosis by chelation treatment in rats: role of reactive oxygen species and intracellular Ca(2+). J Pharmacol Exp Ther 322:108–116. https://doi.org/10.1124/jpet.107.121996
Funding
This study was supported by the statutory budget of the Department of Biochemistry and Medical Chemistry, Pomeranian Medical University.
Author information
Authors and Affiliations
Contributions
Emilia Metryka: literature review, analysis, interpretation of data for the work, wrote the paper and editing; Patrycja Kupnicka: analysis, interpretation of data for the work; Patrycja Kapczuk: analysis, interpretation of data for the work; Beata Aszakiewicz: literature review, analysis, interpretation of data for the work; Katarzyna Piotrowska: analysis, interpretation of data for the work; Marta Tkacz: analysis, interpretation of data for the work; Marta Goschorska: literature review; Izabela Gutowska: literature review, Dariusz Chlubek: funds collection, Irena Baranowska-Bosiacka: study design, drafted the work, and substantively revised.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethics Approval
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Metryka, E., Kupnicka, P., Kapczuk, P. et al. Lead (Pb) Accumulation in Human THP-1 Monocytes/Macrophages In Vitro and the Influence on Cell Apoptosis. Biol Trace Elem Res 199, 955–967 (2021). https://doi.org/10.1007/s12011-020-02215-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-020-02215-7