Abstract
Background
An in-depth understanding of risk factors for revision TKA is needed to minimize the burden of revision surgery. Previous studies indicate that hospital and community characteristics may influence outcomes after TKA, but a detailed investigation in a diverse population is warranted to identify opportunities for quality improvement.
Questions/purposes
We asked: (1) What is the frequency of revision TKA within 10 years of primary arthroplasty? (2) Which patient demographic factors are associated with revision within 10 years of TKA? (3) Which community and institutional characteristics are associated with revision within 10 years of TKA?
Methods
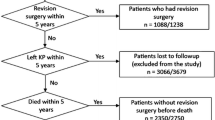
We identified 301,955 patients who underwent primary TKAs in New York or California from 1997 to 2005 from statewide databases. Identifier codes were used to determine whether they underwent revision TKA. Patient, community, and hospital characteristics were analyzed using multivariable regression modeling to determine predictors for revision.
Results
The frequency of revision was 4.0% at 5 years after the index arthroplasty and 8.9% at 9-years. Patients between 50 and 75 years old had a lower risk of revision than patients younger than 50 years (hazard ratio [HR], 0.47; 95% CI, 0.44, 0.50). Black patients were at increased risk for needing revision surgery (HR, 1.39; 95% CI, 1.29, 1.49) after adjustment for insurance type, poverty level, and education. Women (HR, 0.82; 95% CI, 0.79, 0.86) and Medicare recipients (HR, 0.82; 95% CI, 0.79, 0.86) were less likely to undergo revision surgery, whereas those from the most educated (HR, 1.09; 95% CI, 1.02, 1.16) and the poorest communities (HR, 1.08; 95% CI, 1.01, 1.15) had modest increases in risk of revision. Mid-volume hospitals (200–400 annual cases) had a reduction of early revision (HR, 0.91; 95% CI, 0.83, 0.99) compared with those performing less than 200 cases annually, whereas higher-volume hospitals (greater than 400 cases) showed little effect compared with low-volume hospitals.
Conclusions
Patient, community, and institutional characteristics affect the risk for revision within 10 years of index TKA. These data can be used to develop process improvement and implant surveillance strategies among high-risk patients.
Level of Evidence
Level III, therapeutic study. See the Instructions for Authors for a complete description of levels of evidence.


Similar content being viewed by others
References
Bang H, Chiu YL, Memtsoudis SG, Mandl LA, Della Valle AG, Mushlin AI, Marx RG, Mazumdar M. Total hip and total knee arthroplasties: trends and disparities revisited. Am J Orthop (Belle Mead NJ). 2010;39:E95–102.
Berend ME, Davis PJ, Ritter MA, Keating EM, Faris PM, Meding JB, Malinzak RA. “Thicker” polyethylene bearings are associated with higher failure rates in primary total knee arthroplasty. J Arthroplasty. 2010;25(6 suppl):17–20.
Borkhoff CM, Hawker GA, Kreder HJ, Glazier RH, Mahomed NN, Wright JG. The effect of patients’ sex on physicians’ recommendations for total knee arthroplasty. CMAJ. 2008;178:681–687.
Bozic KJ, Kinder J, Meneghini RM, Zurakowski D, Rosenberg AG, Galante JO. Implant survivorship and complication rates after total knee arthroplasty with a third-generation cemented system: 5 to 8 years followup. Clin Orthop Relat Res. 2005;430:117–124.
Bozic KJ, Kurtz SM, Lau E, Ong K, Chiu V, Vail TP, Rubash HE, Berry DJ. The epidemiology of revision total knee arthroplasty in the United States. Clin Orthop Relat Res. 2010;468:45–51.
Collins TC, Daley J, Henderson WH, Khuri SF. Risk factors for prolonged length of stay after major elective surgery. Ann Surg. 1999;230:251–259.
Cram P, Vaughan-Sarrazin MS, Rosenthal GE. Hospital characteristics and patient populations served by physician owned and non physician owned orthopedic specialty hospitals. BMC Health Serv Res. 2007;7:155.
Curtin B, Malkani A, Lau E, Kurtz S, Ong K. Revision after total knee arthroplasty and unicompartmental knee arthroplasty in the Medicare population. J Arthroplasty. 2012;27:1480–1486.
Duffy GP, Trousdale RT, Stuart MJ. Total knee arthroplasty in patients 55 years old or younger: 10- to 17-year results. Clin Orthop Relat Res. 1998;356:22–27.
Elixhauser A, Steiner C, Harris DR, Coffey RM. Comorbidity measures for use with administrative data. Med Care. 1998;36:8–27.
FitzGerald JD, Soohoo NF, Losina E, Katz JN. Potential impact on patient residence to hospital travel distance and access to care under a policy of preferential referral to high-volume knee replacement hospitals. Arthritis Care Res (Hoboken). 2012;64:890–897.
Francis ML, Scaife SL, Zahnd WE, Cook EF, Schneeweiss S. Joint replacement surgeries among medicare beneficiaries in rural compared with urban areas. Arthritis Rheum. 2009;60:3554–3562.
Heck DA, Melfi CA, Mamlin LA, Katz BP, Arthur DS, Dittus RS, Freund DA. Revision rates after knee replacement in the United States. Med Care. 1998;36:661–669.
Ibrahim SA, Siminoff LA, Burant CJ, Kwoh CK. Variation in perceptions of treatment and self-care practices in elderly with osteoarthritis: a comparison between African American and white patients. Arthritis Rheum. 2001;45:340–345.
Katz JN, Barrett J, Mahomed NN, Baron JA, Wright RJ, Losina E. Association between hospital and surgeon procedure volume and the outcomes of total knee replacement. J Bone Joint Surg Am. 2004;86:1909–1916.
Katz JN, Mahomed NN, Baron JA, Barrett JA, Fossel AH, Creel AH, Wright J, Wright EA, Losina E. Association of hospital and surgeon procedure volume with patient-centered outcomes of total knee replacement in a population-based cohort of patients age 65 years and older. Arthritis Rheum. 2007;56:568–574.
Katz JN, Wright EA, Baron JA, Corbett KL, Nti AA, Malchau H, Wright J, Losina E. Predictive value of Medicare claims data for identifying revision of index hip replacement was modest. J Clin Epidemiol. 2011;64:543–546.
Khatod M, Inacio M, Paxton EW, Bini SA, Namba RS, Burchette RJ, Fithian DC. Knee replacement: epidemiology, outcomes, and trends in Southern California: 17,080 replacements from 1995 through 2004. Acta Orthop. 2008;79:812–819.
Krieger N. Overcoming the absence of socioeconomic data in medical records: validation and application of a census-based methodology. Am J Public Health. 1992;82:703–710.
Kurtz S, Mowat F, Ong K, Chan N, Lau E, Halpern M. Prevalence of primary and revision total hip and knee arthroplasty in the United States from 1990 through 2002. J Bone Joint Surg Am. 2005;87:1487–1497.
Labek G, Thaler M, Janda W, Agreiter M, Stockl B. Revision rates after total joint replacement: cumulative results from worldwide joint register datasets. J Bone Joint Surg Br. 2011;93:293–297.
Mahomed NN, Barrett J, Katz JN, Baron JA, Wright J, Losina E. Epidemiology of total knee replacement in the United States Medicare population. J Bone Joint Surg Am. 2005;87:1222–1228.
Manley M, Ong K, Lau E, Kurtz SM. Total knee arthroplasty survivorship in the United States Medicare population: effect of hospital and surgeon procedure volume. J Arthroplasty. 2009;24:1061–1067.
Mulhall KJ, Ghomrawi HM, Scully S, Callaghan JJ, Saleh KJ. Current etiologies and modes of failure in total knee arthroplasty revision. Clin Orthop Relat Res. 2006;446:45–50.
Oduwole KO, Molony DC, Walls RJ, Bashir SP, Mulhall KJ. Increasing financial burden of revision total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2010;18:945–948.
Pabinger C, Berghold A, Boehler N, Labek G. Revision rates after knee replacement: cumulative results from worldwide clinical studies versus joint registers. Osteoarthritis Cartilage. 2013;21:263–268.
Psaty BM, Cheadle A, Koepsell TD, Diehr P, Wickizer T, Curry S, VonKorff M, Perrin EB, Pearson DC, Wagner EH. Race- and ethnicity-specific characteristics of participants lost to follow-up in a telephone cohort. Am J Epidemiol. 1994;140:161–171.
Rand JA, Ilstrup DM. Survivorship analysis of total knee arthroplasty: cumulative rates of survival of 9200 total knee arthroplasties. J Bone Joint Surg Am. 1991;73:397–409.
Ritter MA, Worland R, Saliski J, Helphenstine JV, Edmondson KL, Keating EM, Faris PM, Meding JB. Flat-on-flat, nonconstrained, compression molded polyethylene total knee replacement. Clin Orthop Relat Res. 1995;321:79–85.
Robertsson O, Knutson K, Lewold S, Lidgren L. The Swedish Knee Arthroplasty Register 1975-1997: an update with special emphasis on 41,223 knees operated on in 1988-1997. Acta Orthop Scand. 2001;72:503–513.
Santaguida PL, Hawker GA, Hudak PL, Glazier R, Mahomed NN, Kreder HJ, Coyte PC, Wright JG. Patient characteristics affecting the prognosis of total hip and knee joint arthroplasty: a systematic review. Can J Surg. 2008;51:428–436.
Skinner J, Weinstein JN, Sporer SM, Wennberg JE. Racial, ethnic, and geographic disparities in rates of knee arthroplasty among Medicare patients. N Engl J Med. 2003;349:1350–1359.
Skinner J, Zhou W, Weinstein J. The influence of income and race on total knee arthroplasty in the United States. J Bone Joint Surg Am. 2006;88:2159–2166.
SooHoo NF, Lieberman JR, Ko CY, Zingmond DS. Factors predicting complication rates following total knee replacement. J Bone Joint Surg Am. 2006;88:480–485.
Tejwani NC, Takemoto RC, Nayak G, Pahk B, Egol KA. Who is lost to followup?: a study of patients with distal radius fractures. Clin Orthop Relat Res. 2010;468:599–604.
Worland RL, Johnson GV, Alemparte J, Jessup DE, Keenan J, Norambuena N. Ten to fourteen year survival and functional analysis of the AGC total knee replacement system. Knee. 2002;9:133–137.
Young NL, Cheah D, Waddell JP, Wright JG. Patient characteristics that affect the outcome of total hip arthroplasty: a review. Can J Surg. 1998;41:188–195.
Acknowledgments
We thank Timothy Wright PhD, Hospital for Special Surgery, New York, NY, for guidance in the development of the research questions and scientific approach, and Huong Do MA, Hospital for Special Surgery, New York, NY, for assistance with preparation of the data for further analysis.
Author information
Authors and Affiliations
Corresponding author
Additional information
One of the authors (CJD) certifies that he has received, during the study period, funding from the National Institute of Arthritis and Musculoskeletal and Skin Diseases (Bethesda, MD, USA) (Grant T32-AR07281). One of the authors (SL) certifies that he has received, during the study period, funding from the National Institute of Arthritis and Musculoskeletal and Skin Diseases (Grant R03 AR05063) and the Agency for Healthcare Research and Quality (Rockville, MD, USA) (Grant U18-HS16075). Each author certifies that he or she, or a member of his or her immediate family, has no commercial associations (eg, consultancies, stock ownership, equity interest, patent/licensing arrangements, etc) that might pose a conflict of interest in connection with the submitted article.
All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research editors and board members are on file with the publication and can be viewed on request.
Each author certifies that his or her institution approved or waived approval for the human protocol for this investigation and that all investigations were conducted in conformity with ethical principles of research.
This work was performed at Hospital for Special Surgery, New York, NY, USA.
About this article
Cite this article
Dy, C.J., Marx, R.G., Bozic, K.J. et al. Risk Factors for Revision Within 10 Years of Total Knee Arthroplasty. Clin Orthop Relat Res 472, 1198–1207 (2014). https://doi.org/10.1007/s11999-013-3416-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-013-3416-6