Abstract
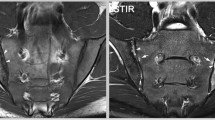
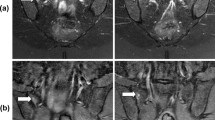
The introduction of MRI in spondyloarthritis (SpA) constitutes a major advance and is increasingly being implemented in clinical practice in cases in which clinical suspicion of SpA is high yet pelvic radiography is equivocal. Recent studies and development of consensus by international experts support the routine use of specific MRI sequences and scanning protocols for the evaluation of the sacroiliac joints in diagnostic work-up. There is also agreement that the finding of bone marrow edema in the sacroiliac joints carries a high probability of SpA, and emerging data indicate that the finding of erosion may also be diagnostically helpful, even in preradiographic SpA. Recent studies suggest that the diagnostic role of MRI may be further enhanced through the study of additional MRI sequences and prospective studies using systematic methodologies aimed at further scrutiny of structural lesions and the contribution of spinal imaging. Interest in MRI for SpA is poised for substantial growth.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
• Rudwaleit M, Haibel H, Baraliakos X, Listing J, et al. The early disease stage in axial Spondylarthritis. Results from the German Spondyloarthritis Inception Cohort. Arthritis Rheum 2009; 60:717–727. This prospective study shows that SpA patients with preradiographic disease experience similar severity of symptoms to those with established AS.
• Barkham N, Keen HI, Coates LC, et al. Clinical and imaging efficacy of infliximab in HLA-B27–positive patients with magnetic resonance imaging–determined early sacroiliitis. Arthritis Rheum 2009; 60: 946–954. This randomized controlled trial in very early SpA diagnosed by MRI demonstrated exceptional clinical responses to infliximab.
• Hildrun H, Rudwaleit M, Listing J, et al. Efficacy of adalimumab in the treatment of axial spondylarthritis without radiographically defined sacroiliitis. Arthritis Rheum 2008; 58: 1981–1991. This randomized controlled trial of adalimumab showed that ASAS20 responses are even higher in preradiographic SpA than previously demonstrated in pivotal phase 3 trials of anti-TNF agents.
•• Rudwaleit M, van der Heijde D, Landewé R, et al. The development of assessment of SpondyloArthritis international Society (ASAS) Classification Criteria for axial spondyloarthritis (Part II): validation and final selection. Ann Rheum Dis 2009; 68: 777–783. This final study report describes the final selection of items and validation of the new ASAS axial SpA criteria. A notable inclusion is the addition of MRI as an imaging criterion for patients who do not have radiographic sacroiliitis.
Rudwaleit M, Jurik AG, Hermann KG, Landewé R, et al. Defining active sacroiliitis on magnetic resonance imaging (MRI) for classification of axial spondyloarthritis—a consensual approach by the ASAS/OMERACT MRI Group. Ann Rheum Dis. 2009;68:1520–7.
Weber U, Maksymowych WP. How does imaging help the clinician in the evaluation and management of spondyloarthritis? Skeletal Radiol. 2008;37:487–90.
Christian EA, Feist E, Burovaa E, et al. Magnetic resonance imaging of active sacroiliitis: do we really need gadolinium? Eur J Rad. 2009;71:232–6.
Muche B, Bollow M, Francois RJ, Sieper J, Hamm B, Braun J. Anatomic structures involved in early- and late-stage sacroiliitis in spondylarthritis. A detailed analysis by contrast-enhanced magnetic resonance imaging. Arthritis Rheum. 2003;48:1374–84.
Puhakka KB, Melsen F, Jurik AG, Boel LW, Vesterby A, Egund N. MR imaging of the normal sacroiliac joint with correlation to histology. Skelet Radiol. 2004;33:15–28.
Madsen KB, Egund N, Jurik AG. Grading of inflammatory disease activity in the sacroiliac joints with magnetic resonance imaging: comparison between short tau inversion recovery and gadolinium contrast-enhanced sequences. J Rheumatol. 2010;37:393–400.
Baraliakos X, Hermann KG, Landewe R, et al. Assessment of acute spinal inflammation in patients with ankylosing spondylitis by magnetic resonance imaging: a comparison between contrast enhanced T1 and short tau inversion recovery (STIR) sequences. Ann Rheum Dis. 2005;64:1141–4.
Madsen KB, Jurik AG. Magnetic resonance imaging grading system for active and chronic spondylarthritis changes in the sacroiliac joint. Arthritis Care Res. 2010;62:11–8.
Weber U, Maksymowych WP, Jurik AG, et al. Validation of whole-body against conventional magnetic resonance imaging for scoring acute inflammatory lesions in the sacroiliac joints of patients with spondyloarthritis. Arthritis Rheum. 2009;61:893–9.
Weber U, Hodler J, Jurik AG, et al. Assessment of active spinal inflammatory changes in patients with axial spondyloarthritis: validation of whole body MRI against conventional MRI. Ann Rheum Dis. 2010;69:648–53.
Bollow M, Hermann KG, Biedermann T, Sieper J, Schontube M, Braun J. Very early spondyloarthritis: where the inflammation in the sacroiliac joints starts. Ann Rheum Dis. 2005;64:1644–6.
Lambert RGW, Salonen D, Rahman P, et al. Adalimumab significantly reduces both spinal and sacroiliac joint inflammation in patients with ankylosing spondylitis. Arthritis Rheum. 2007;56:4005–14.
Maksymowych W, Dhillon SS, Chiowchanwisawakit P, et al. Development and validation of web-based training modules for systematic evaluation of active inflammatory lesions in the spine and sacroiliac joints in spondyloarthritis. J Rheumatol. 2009;36 Suppl 84:48–57.
Algin O, Gokalp G, Ocakoglu G. Evaluation of bone cortex and cartilage of spondyloarthropathic sacroiliac joint. Acad Radiol. 2010;17:1292–8.
Wick MC, Weiss RJ, Jaschke W, Klauser A. Erosions are the most relevant magnetic resonance imaging features in quantification of sacroiliac joints in ankylosing spondylitis. J Rheumatol. 2010;37:622–7.
Weber U, Pedersen SJ, Hodler J, Ostergaard M, Lambert RGW, Maksymowych WP. Does fat infiltration in the sacroiliac joint contribute to the diagnostic utility of MRI in ankylosing spondylitis? Arthritis Rheum. 2009;60 Suppl 10:54. abstract.
Braun J, Bollow M, Eggens U, Koenig H, Distler A, Sieper J. Use of dynamic magnetic resonance imaging with fast imaging in the detection of early and advanced sacroiliitis in spondyloarthropathy patients. Arthritis Rheum. 1994;37:1039–45.
Hanly JG, Mitchell MJ, Barnes DC, MacMillan L. Early recognition of sacroiliitis by magnetic resonance imaging and single photon emission computed tomography. J Rheumatol. 1994;21:2088–95.
Bollow M, Braun J, Hamm B, et al. Early sacroiliitis in patients with spondyloarthropathy: evaluation with dynamic gadolinium-enhanced MR imaging. Radiology. 1995;194:529–36.
Blum U, Buitrago-Tellez C, Mundinger A, et al. Magnetic resonance imaging (MRI) for detection of active sacroiliitis-a prospective study comparing conventional radiography, scintigraphy, and contrast enhanced MRI. J Rheumatol. 1996;23:2107–15.
Puhakka KB, Jurik AG, Egund N, et al. Imaging of sacroiliitis in early seronegative spondyloarthropathy. Assessment of abnormalities by MRI in comparison with radiography and CT. Acta Radiol. 2003;44:218–29.
Rudwaleit M, van der Heijde D, Khan MA, Braun J, Sieper J. How to diagnose axial spondyloarthritis early. Ann Rheum Dis. 2004;63:535–43.
•• Weber U, Lambert RG, Ostergaard M, Hodler J, Pedersen SJ, Maksymowych WP. The diagnostic utility of MRI in spondyloarthritis: an international multicentre evaluation of 187 subjects. Arthritis Rheum 2010; 62: 3048–3058. This international, multicenter evaluation represents the first study using a standardized methodology and MRI sequences used in clinical practice to assess the diagnostic utility of MRI.
• Weber U, Lambert RGW, Pedersen SJ, Hodler J, Østergaard M, Maksymowych WP. Assessment of structural lesions in sacroiliac joints enhances diagnostic utility of MRI in early spondyloarthritis. Arthritis Care Res 2010; 62: 1763–1771. This report highlights the importance of rheumatologist training to recognize abnormalities on the T1W sequence. It shows that rheumatologist evaluation of MRI scans is heavily biased toward interpretation of STIR images.
Maksymowych WP, Inman RD, Salonen D, et al. Spondyloarthritis Research Consortium of Canada magnetic resonance imaging index for assessment of sacroiliac joint inflammation in ankylosing spondylitis. Arthritis Rheum (Arthritis Care Res). 2005;53:703–9.
• Lambert RGW, Pedersen SJ, Maksymowych WP, Chiowchanwisawakit P, Østergaard M. Active inflammatory lesions detected by magnetic resonance imaging in the spine of patients with spondyloarthritis—definitions, assessment system, and reference image set. J Rheumatol 2009; 36 suppl 84: 3–17. This report elaborates on the standardized definitions for active inflammatory lesions in the spine developed by the Canada-Denmark MRI International Working Group.
• Østergaard M, Maksymowych WP, Pedersen SJ, Chiowchanwisawakit P, Lambert RGW. Structural lesions detected by magnetic resonance imaging in the spine of patients with spondyloarthritis—definitions, assessment system, and reference image set. J Rheumatol 2009; 36 suppl 84: 18–34. This report elaborates on the standardized definitions for structural lesions in the spine developed by the Canada-Denmark MRI International Working Group.
• Pedersen SJ, Østergaard M, Chiowchanwisawakit P, Lambert RGW, Maksymowych WP. Validation of definitions for active inflammatory lesions detected by magnetic resonance imaging in the spine of patients with spondyloarthritis. J Rheumatol 2009; 36(suppl 84): 35–38. This report outlines the validation of definitions for active lesions of the spine, which constitutes an essential preliminary step prior to their implementation in clinical practice and research.
• Chiowchanwisawakit P, Østergaard M, Pedersen SJ, Lambert RGW, Conner-Spady B, Maksymowych WP. Validation of definitions for structural lesions detected by magnetic resonance imaging in the spine of patients with spondyloarthritis. J Rheumatol 2009; 36(suppl 84): 39–47. This report outlines the validation of definitions for structural lesions of the spine, which constitutes an essential preliminary step prior to their implementation in clinical practice and research.
• Weber U, Hodler J, Kubik RA, et al. Sensitivity and specificity of spinal inflammatory lesions assessed by whole-body magnetic resonance imaging in patients with ankylosing spondylitis or recent-onset inflammatory back pain. Arthritis Rheum 2009; 61: 900–908. This report using WBMRI shows that a vertebral corner inflammatory lesion may be seen in about one third of healthy controls, and that diagnostic utility of these lesions is optimal when at least two are present, especially in the thoracic spine.
Bennett AN, Rehman A, Hensor EM, Marzo-Ortega H, Emery P, McGonagle D. The fatty Romanus lesion: a non-inflammatory spinal MRI lesion specific for axial spondyloarthropathy. Ann Rheum Dis. 2010;69:891–4.
•• Rennie WJ, Dhillon SS, Conner-Spady B, Maksymowych WP, Lambert RGW. MRI assessment of spinal inflammation in ankylosing spondylitis: standard clinical protocols may omit inflammatory lesions in thoracic vertebrae. Arthritis Rheum 2009; 61: 1187–1193. This report has major clinical practice implications in that it highlights the importance of using appropriate MRI scanning protocols that ensure adequate visualization of the lateral segments of the spine, where inflammatory lesions are frequently observed and are highly specific for SpA.
Acknowledgment
Dr. Maksymowych is a scientist of the Alberta Heritage Foundation for Medical Research.
Disclosure
Dr. Weber has received support from the Walter L. and Johanna Wolf Foundation and the Foundation for Scientific Research at the University of Zurich. He also received payment for contribution to the imaging section of a comprehensive educational slide kit on all clinical aspects of spondyloarthritis (SPARKLE initiative) sponsored by Abbott Laboratories International.
Dr. Maksymowych reported no potential conflicts of interest relevant to this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maksymowych, W.P., Weber, U. Diagnostic Utility of MRI in Early Spondyloarthritis. Curr Rheumatol Rep 13, 402–408 (2011). https://doi.org/10.1007/s11926-011-0190-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11926-011-0190-x