Abstract
Purpose of Review
This review aims to elucidate the limitations of diagnosing metabolic syndrome in adolescents as well as challenges and opportunities in the identification and reduction of cardiometabolic risk in this population.
Recent Findings
There are multiple criticisms of how we define and approach obesity in clinical practice and scientific research, and weight stigma further complicates the process of making and communicating weight-related diagnoses. While the goal of diagnosing and managing metabolic syndrome in adolescents would be to identify individuals at elevated future cardiometabolic risk and intervene to reduce the modifiable component of this risk, there is evidence that identifying cardiometabolic risk factor clustering may be more useful in adolescents than establishing a cutoff-based diagnosis of metabolic syndrome. It has also become clear that many heritable factors and social and structural determinants of health contribute more to weight and body mass index than do individual behavioral choices about nutrition and physical activity. Promoting cardiometabolic health equity requires that we intervene on the obesogenic environment and mitigate the compounding effects of weight stigma and systemic racism.
Summary
The existing options to diagnose and manage future cardiometabolic risk in children and adolescents are flawed and limited. While striving to improve population health through policy and societal interventions, there are opportunities to intervene at all levels of the socioecological model in order to decrease future morbidity and mortality from the chronic cardiometabolic diseases associated with central adiposity in both children and adults. More research is needed to identify the most effective interventions.
Similar content being viewed by others
Introduction
While the current use of body mass index (BMI) alone to define obesity is flawed, it is important to acknowledge the rising global prevalence of central adiposity associated with insulin resistance, dyslipidemia, and hypertension which has contributed to significant cardiovascular morbidity and mortality [1,2,3,4]. This cluster of chronic diseases, now known commonly as metabolic syndrome, was noted in adults as early as the 1940s and has been given different names with varying definitions since then [5]. In 1988, Reaven noted that insulin resistance was associated with hypertriglyceridemia, decreased high-density lipoprotein (HDL), hypertension, and an increased risk for coronary artery disease and named this cluster syndrome X [6]. In 1989, Kaplan highlighted the importance of central adiposity in addition to hypertension, diabetes, and hypertriglyceridemia in what he called the deadly quartet for cardiovascular risk [7]. In the decades since then, multiple researchers and organizations have proposed varying names and definitions for the cardiometabolic risk associated with central adiposity—with the American Association of Clinical Endocrinologists (AACE) and American College of Endocrinology (ACE) most recently proposing adiposity-based chronic disease (ABCD) in 2017 and cardiometabolic-based chronic disease (CMBCD) in 2020 [8, 9•].
This constellation of chronic diseases which was previously found mainly in adults has become increasingly common in children and adolescents, and much has been described about the pathophysiology, risk factors, clinical features and assessment, and common comorbidities of metabolic syndrome in adolescents [10,11,12,13,14]. While the goal of diagnosing and managing metabolic syndrome in adolescents would be to identify individuals at elevated future cardiometabolic risk and intervene to reduce the modifiable component of this risk, there is evidence that this diagnosis may have limited utility in this population [4]. This review aims to elucidate the limitations of diagnosing metabolic syndrome in adolescents as well as challenges and opportunities in the identification and reduction of cardiometabolic risk in this population.
Challenges in Cardiometabolic Risk Stratification
Fear of Reinforcing Weight Stigma
Weight stigma complicates the process of making and communicating weight-related diagnoses including overweight, obesity, and metabolic syndrome. Weight stigma is a well-established concept defined by Tomiyama et al. as “social rejection and devaluation that accrues to those who do not comply with prevailing social norms of adequate body weight and shape” [15]. Due to the societal prevalence of weight stigma, many individuals experience negative healthcare interactions related to weight—despite the evidence that weight stigma does not promote positive health behavior change and instead contributes to worse outcomes [15]. Given this context, even when a provider approaches a conversation about weight with appropriate empathy and sensitivity, a diagnosis of overweight or obesity can feel morally charged and reflective of judgement [15,16,17,18]. As adolescence is a vulnerable and critical period in development, the fear of reinforcing weight stigma and triggering or exacerbating poor self-image or unhealthy weight control behaviors may add to other logistical barriers in contributing to the underdiagnosis and subsequent undertreatment of pediatric and adolescent obesity [19,20,21,22,23]. A decrease in societal weight stigma would facilitate the nonjudgmental diagnosis and prevention of cardiometabolic risk associated with central adiposity, and clinicians should be leaders in mitigating weight stigma in their own practices and advocating for broader societal changes in part by accessing training and education which address this issue [24].
Limitations of Using Obesity Alone
Although BMI is easily measured and ubiquitous, there are multiple criticisms of the definition of and approach to obesity in clinical practice and scientific research [16, 25, 26]. The definition of obesity based only on BMI, which was first described by Quetelet in 1832 as the ratio of the weight in kilograms divided by the square of the height in meters and later named by Keys in 1972, has clear limitations [27, 28]. Body composition and the distribution of adiposity can vary greatly among individuals with the same BMI, and not accounting for variations by race/ethnicity and sex can make BMI thresholds particularly inaccurate in predicting future disease [29, 30]. Although diagnoses of overweight and obesity based on BMI have many limitations, a subset of such individuals, particularly those with central adiposity, are at elevated risk of developing chronic cardiometabolic diseases including diabetes, hypertension, hyperlipidemia, and atherosclerotic cardiovascular disease. Not identifying these individuals limits our ability to intervene and decrease any of this modifiable risk.
Issues with Diagnosing Metabolic Syndrome
Diagnosing metabolic syndrome is one option for identifying elevated cardiometabolic risk. While many definitions have been proposed for metabolic syndrome in children and adolescents, there is no established consensus definition [31]. In 2007, the International Diabetes Federation (IDF) published a consensus report with global diagnostic criteria which recommended against making the diagnosis before age 10 and required central obesity based on waist circumference (WC ≥ 90th percentile or adult cutoff if lower in adolescents age 10–15 and using ethnic-specific adult WC cutoffs in adolescents age 16 +) plus two of the following: hypertriglyceridemia, low HDL-C, hypertension, or evidence of impaired glucose metabolism with elevated fasting glucose or known type 2 diabetes [32].
Although the IDF urged the development of ethnic-specific normal ranges for waist circumference as part of this report, ranges which account for ethnic and national differences across adolescent populations have not been developed or broadly available, though this need has been recently re-emphasized [33,34,35]. Before metabolic syndrome could be systematically diagnosed in adolescents, multiple ranges of waist circumference would need to be published and validated, if not fully integrated into the electronic health record, in order to assess whether adolescents meet percentile-based or cutoff-based criteria. Furthermore, despite some practice guidelines recommending the measurement of waist circumference in particular patient populations, waist circumference is not routinely measured in the clinical setting, and members of the clinical team would need to be trained to measure it in a validated and reproducible way [36, 37].
Added Utility of Metabolic Syndrome Diagnosis
While the logistical barriers to diagnosing metabolic syndrome in adolescents could be surmountable, there is uncertainty around whether metabolic syndrome is a useful construct in adolescents. There is evidence that the cutoff-based diagnosis of metabolic syndrome can be highly unstable in adolescents and result in many individuals who met criteria at one point not meeting criteria at a later point despite not having lost weight; this instability can manifest over weeks or years and may be partially explained by normal changes in insulin resistance as a result of puberty [38,39,40,41]. Based on these and other factors, the American Academy of Pediatrics (AAP) in 2017 suggested shifting the focus from establishing a cutoff-based diagnosis of metabolic syndrome to using cardiometabolic risk factor clustering and associated risk factor screening to identify adolescents with overweight or obesity who are at elevated risk for developing cardiometabolic disease [4]. The lasting benefit of adult diabetes prevention programs suggests that intervening effectively to identify and address clustered risk factors in adolescence is likely to provide durable benefits over time [42].
Challenges and Opportunities in Intervening for Prevention and Management
Once recognized, the treatment of metabolic syndrome consists of treating obesity as well as the components of abnormal glucose metabolism, dyslipidemia, and hypertension if present. While the additional utility of diagnosing metabolic syndrome in adolescents is unclear, the American Heart Association (AHA) and National Heart, Lung, and Blood Institute (NHLBI) recommend prioritizing early treatment of obesity as a foundational component of reducing associated cardiometabolic risk [43, 44]. Given this, the remainder of this section will be focused on challenges and opportunities in intervening to prevent and manage obesity in adolescents.
Barriers to Intervening in Clinic
It is commonly accepted that pediatricians and other primary care clinicians are in a unique position to diagnose and treat individual adolescents in the context of their families and communities through measuring and trending BMI, counseling about lifestyle modifications through motivational interviewing, prescribing pharmacotherapy when appropriate, and referring to comprehensive multidisciplinary intervention programs when these are available [45,46,47]. However, there are many barriers to effectively diagnosing and treating overweight and obesity in pediatric primary care; these encompass staff factors including knowledge and competence, professional-parent/patient interaction factors including risk to therapeutic relationship when raising a sensitive topic in the setting of insufficient trust, organizational factors including limited time and contact opportunities, and lack of available treatment programs and resources [19, 20]. The AAP recommends referral to intensive health behavior and lifestyle treatment, ideally with 26 or more hours of contact over a 3- to 12-month period [47]. Qualitative work has shown that providers sometimes feel a sense of futility about their ability to make a difference in trying to address such a complex issue as well as frustration about limited availability of resources for referrals [48,49,50,51].
The Obesogenic Environment: a Complex Systemic Issue
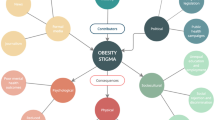
It has become clear that many heritable factors and social and structural determinants of health as part of an obesogenic environment contribute more to weight and BMI than do individual choices about nutrition and physical activity [15, 52,53,54,55,56]. Some of these factors are depicted in Fig. 1, adapted from the socioecological model [57,58,59]. As shown, the weight of an individual is influenced by variables at an individual, interpersonal (most often family), organizational (frequently school and in some cases clinic), community, and societal/policy level—most of these variables are outside of a particular adolescent or family’s control. Structural and social determinants of health (SDOH) including food insecurity, education, access and affordability of less processed food, and housing instability can influence both the risk of developing obesity as well as the ability of adolescents and their families to implement recommended lifestyle modifications related to nutrition and physical activity [60, 61, 62••]. Adolescents with excess weight are more likely to have been born to a person with overweight or obesity who may not have had access to paid parental leave or other support for breastfeeding, more likely to have been exposed to adverse childhood experiences (ACES) and chronic stress, more likely to have experienced food insecurity and/or housing instability, more likely to have grown up in a segregated neighborhood affected by a food swamp or food desert, and less likely to have access to reliable transportation and caregivers whose work environments facilitate cooperation with intensive behavioral interventions [62••, 63,64,65,66, 67••].
Adapted socioecological model of the obesogenic environment for adolescents with nonbehavioral factors (to the left) and opportunities for intervention (to the right) at the individual, interpersonal, organizational, community, and societal/policy levels. CHWs, community health workers; SDOH, social determinants of health
It is well documented that structural racism has enormously detrimental effects on the health of minoritized children and adults in the USA [68,69,70,71,72,73]. The harms of racism influence weight across the lifespan and at every level of the socioecological model [55, 56, 67••, 74,75,76,77]. While significant racial disparities in obesity and cardiometabolic disease—particularly notable for increased prevalence in Black, Latiné, and indigenous youth—long preceded the ongoing COVID-19 pandemic, these disparities have been further highlighted and exacerbated in the last few years [78,79,80,81,82,83].
Opportunities for Intervention
Clinic-Based Interventions
It is important for clinicians to approach conversations related to weight without judgement and acknowledge the complex effects of the obesogenic environment [19, 20, 24]. While more research is needed on the most effective ways to decrease implicit and explicit weight stigma among clinicians, providers can avoid stigmatizing language and imagery, learn and implement adolescents’ preferences for weight-related conversations, and provide appropriately sized medical equipment and furniture [17, 84,85,86]. Consistent nonjudgmental and person-centered anticipatory guidance and motivational interviewing about health behaviors including nutrition and physical activity are foundational to pediatric primary care and a necessary, although insufficient, part of obesity prevention [87,88,89]. The development and implementation of clear protocols for evaluation, treatment, and referrals to intensive lifestyle intervention programs, specialty clinics, and school-based and community-based interventions could promote clinician confidence and likelihood of identifying and addressing diagnoses of overweight, obesity, and elevated cardiometabolic risk [47, 90]. Since obesity in children and adolescents is strongly linked with obesity in parents, family weight management programs provide opportunity to intervene at both individual and interpersonal levels [91,92,93]. Further research is needed to determine the most effective changes to our current model of healthcare delivery.
School-Based Interventions
Given their ability to provide consistent access to children and adolescents which is less dependent on healthcare access or family transportation, schools have been a natural setting for pediatric weight management interventions [94,95,96,97]. School-based interventions which address nutrition and physical activity with some home involvement as well have proven most effective [98]. The HEALTHY study identified the complex challenges involved in conducting weight and diabetes risk interventions in schools and showed promise in decreasing adiposity [99].
Community-Partnered Interventions
Community-based interventions are another important resource. Community organizations and partnerships can help address many social determinants of health as well as provide a setting for weight-specific education and interventions [100,101,102]. It is important for social needs interventions to acknowledge and address the impact of racism to more effectively promote equity in cardiometabolic health [103]. Community health workers represent another opportunity to provide motivational interviewing about health behaviors, identify barriers related to SDOH, and make connections to both community resources and clinical care—multiple such interventions have been attempted and studied with a meta-analysis in 2018 showing a small but significant impact on BMI percentile although significant heterogeneity limited the ability to definitively identify best practices [104].
Policy Interventions
Policy interventions encompass policy that impacts healthcare delivery; impacts food availability, quality, and affordability; and impacts SDOH. Some of the barriers to clinic interventions which were previously described could be addressed by policies supporting increased access to healthcare and multidisciplinary care teams including dieticians, social workers, psychologists, and community health workers as well as subsidized referral options for intensive health behavior and lifestyle treatment programs [105,106,107,108]. Food policy opportunities include decreasing food insecurity by increasing access to food; making healthy food choices available through the Supplemental Nutrition Assistance Program (SNAP) and Special Supplemental Nutrition Program for Women, Infants and Children (WIC); promoting healthy school lunch options through the National School Lunch Program (NSLP) and School Breakfast Program (SBP), as well as regulating the advertising, affordability, and availability of ultra-processed versus nutritionally dense food [109, 110]. Finally, policy that impacts weight also includes policy addressing the myriad of factors that affect the obesogenic environment such as poverty, housing discrimination, neighborhood safety, education, and transportation among many others [55, 56, 111]. Aligned multi-sector approaches are needed to address obesity and related risk factors in adolescents; such approaches show promise when successfully implemented [112].
Conclusions/Future Directions
Although the existing options to diagnose and manage future cardiometabolic risk in children and adolescents are flawed and limited, we must intervene to decrease future morbidity and mortality from the chronic cardiometabolic diseases associated with central adiposity in both children and adults. While the ultimate goal is to improve population health through policy and societal interventions, there is an urgent need to stratify risk given limited resources and to identify and implement effective interventions at all levels of the socioecological model (see Fig. 1). Two priorities are mitigating the compounding effects of weight stigma and systemic racism to promote cardiometabolic health equity.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Chung S, Onuzuruike A, Magge S. Cardiometabolic risk in obese children. Ann N Y Acad of Sci. 2018;1411(1). https://doi.org/10.1111/nyas.13602.
Engin A. The definition and prevalence of obesity and metabolic syndrome. Adv Exp Med Biol. 2017;960. https://doi.org/10.1007/978-3-319-48382-5_1.
Weihrauch-Blüher S, Schwarz P, Klusmann J-H. Childhood obesity: increased risk for cardiometabolic disease and cancer in adulthood. Metabolism. 2019;92. https://doi.org/10.1016/j.metabol.2018.12.001.
Magge SN, Goodman E, Armstrong SC, Daniels S, Corkins M, de Ferranti S, et al. The metabolic syndrome in children and adolescents: shifting the focus to cardiometabolic risk factor clustering. Pediatrics. 2017;140(2). https://doi.org/10.1542/peds.2017-1603.
Sarafidis P, Nilsson P. The metabolic syndrome: a glance at its history. J Hypertens. 2006;24(4). https://doi.org/10.1097/01.hjh.0000217840.26971.b6.
Reaven G. Banting lecture 1988. Role of insulin resistance in human disease. Diabetes. 1988;37(12). https://doi.org/10.2337/diab.37.12.1595.
Kaplan N. The deadly quartet. Upper-body obesity, glucose intolerance, hypertriglyceridemia, and hypertension. Arch Intern Med. 1989;149(7). https://doi.org/10.1001/archinte.149.7.1514.
Mechanick J, Hurley D, Garvey W. Adiposity-based chronic disease as a new diagnostic term: the American Association of Clinical Endocrinologists and American College of Endocrinology Position Statement. Endocr Pract. 2017;23(3). https://doi.org/10.4158/EP161688.PS.
• Nieto-Martínez R, González-Rivas J, Mechanick J. Cardiometabolic risk: new chronic care models. JPEN J Parenter Enteral Nutr. 2021;45(S2). https://doi.org/10.1002/jpen.2264. (Describes a new Cardiometabolic-Based Chronic Disease (CMBCD) care model for cardiometabolic risk.)
Christian Flemming G, Bussler S, Körner A, Kiess W. Definition and early diagnosis of metabolic syndrome in children. J Pediatr Endocrinol Metab: JPEM. 2020;33(7). https://doi.org/10.1515/jpem-2019-0552.
Weihe P, Weihrauch-Blüher S. Metabolic syndrome in children and adolescents: diagnostic criteria, therapeutic options and perspectives. Curr Obes Rep. 2019;8(4). https://doi.org/10.1007/s13679-019-00357-x.
DeBoer M. Assessing and managing the metabolic syndrome in children and adolescents. Nutrients. 2019;11(8). https://doi.org/10.3390/nu11081788.
Ighbariya A, Weiss R. Insulin resistance, prediabetes, metabolic syndrome: what should every pediatrician know? J Clin Res Pediatr Endocrinol. 2017;9(Suppl 2). https://doi.org/10.4274/jcrpe.2017.S005.
Wittcopp C, Conroy R. Metabolic syndrome in children and adolescents. Pediatr Rev. 2016;37(5). https://doi.org/10.1542/pir.2014-0095.
Tomiyama A, Carr D, Granberg E, Major B, Robinson E, Sutin A, et al. How and why weight stigma drives the obesity 'epidemic' and harms health. BMC Med. 2018;16(1). https://doi.org/10.1186/s12916-018-1116-5.
Puhl R, Heuer C. Obesity stigma: important considerations for public health. Am J Public Health. 2010;100(6). https://doi.org/10.2105/AJPH.2009.159491.
Pont S, Puhl R, Cook S, Slusser W. Stigma experienced by children and adolescents with obesity. Pediatrics. 2017;140(6). https://doi.org/10.1542/peds.2017-3034.
Puhl R, Suh Y. Health consequences of weight stigma: implications for obesity prevention and treatment. Curr Obes Rep. 2015;4(2). https://doi.org/10.1007/s13679-015-0153-z.
Bradbury D, Chisholm A, Watson P, Bundy C, Bradbury N, Birtwistle S. Barriers and facilitators to health care professionals discussing child weight with parents: a meta-synthesis of qualitative studies. Br J Health Psychol. 2018;23(3). https://doi.org/10.1111/bjhp.12312.
Ray D, Sniehotta F, McColl E, Ells L. Barriers and facilitators to implementing practices for prevention of childhood obesity in primary care: a mixed methods systematic review. Obes Rev. 2022;23(4). https://doi.org/10.1111/obr.13417.
Ciciurkaite G, Moloney M, Brown R. The incomplete medicalization of obesity: physician office visits, diagnoses, and treatments, 1996–2014. Public Health Rep (Washington, DC : 1974). 2019;134(2). https://doi.org/10.1177/0033354918813102.
Camp N, Robert R, Dawes C, Kelly K. Identification of overweight and obesity in low-income minority children by pediatric providers and child characteristics associated with underrecognition. J Pediatr Health Care. 2019;33(2). https://doi.org/10.1016/j.pedhc.2018.07.007.
Tucker S, Bramante C, Conroy M, Fitch A, Gilden A, Wittleder S, et al. The most undertreated chronic disease: addressing obesity in primary care settings. Curr Obes Rep. 2021;10(3). https://doi.org/10.1007/s13679-021-00444-y.
Tanas R, Gil B, Marsella M, Nowicka P, Pezzoli V, Phelan S, et al. Addressing weight stigma and weight-based discrimination in children: preparing pediatricians to meet the challenge. J Pediatr. 2022;248. https://doi.org/10.1016/j.jpeds.2022.06.011.
Gutin I. Body mass index is just a number: conflating riskiness and unhealthiness in discourse on body size. Sociol Health illness. 2021;43(6). https://doi.org/10.1111/1467-9566.13309.
Kragelund C, Omland T. A farewell to body-mass index? Lancet (London, England). 2005;366(9497). https://doi.org/10.1016/S0140-6736(05)67642-8.
Eknoyan G. Adolphe Quetelet (1796–1874)—the average man and indices of obesity. Nephrol Dial Transplant. 2008;23(1). https://doi.org/10.1093/ndt/gfm517.
Keys A, Fidanza F, Karvonen M, Kimura N, Taylor H. Indices of relative weight and obesity. J Chronic Dis. 1972;25(6). https://doi.org/10.1016/0021-9681(72)90027-6.
Nuttall F. Body mass index: obesity, BMI, and health: a critical review. Nutr Today. 2015;50(3). https://doi.org/10.1097/NT.0000000000000092.
Stanford F, Lee M, Hur C. Race, ethnicity, sex, and obesity: is it time to personalize the scale? Mayo Clin Proc. 2019;94(2). https://doi.org/10.1016/j.mayocp.2018.10.014.
Roberts C, Hevener A, Barnard R. Metabolic syndrome and insulin resistance: underlying causes and modification by exercise training. Compr Physiol. 2013;3(1). https://doi.org/10.1002/cphy.c110062.
Zimmet P, Alberti K, Kaufman F, Tajima N, Silink M, Arslanian S, et al. The metabolic syndrome in children and adolescents—an IDF consensus report. Pediatr Diabetes. 2007;8(5). https://doi.org/10.1111/j.1399-5448.2007.00271.x.
Ross R, Neeland I, Yamashita S, Shai I, Seidell J, Magni P et al. Waist circumference as a vital sign in clinical practice: a Consensus Statement from the IAS and ICCR Working Group on Visceral Obesity. Nat Rev Endocrinol. 2020;16(3). https://doi.org/10.1038/s41574-019-0310-7.
Xi B, Zong X, Kelishadi R, Litwin M, Hong Y, Poh B, et al. International waist circumference percentile cutoffs for central obesity in children and adolescents aged 6 to 18 years. J Clin Endocrinol Metab. 2020;105(4). https://doi.org/10.1210/clinem/dgz195.
Inokuchi M, Matsuo N, Takayama J, Hasegawa T. Population-based waist circumference reference values in Japanese children (0–6 years): comparisons with Dutch, Swedish and Turkish preschool children. J Pediatr Endocrinol Metab: JPEM. 2020;34(3). https://doi.org/10.1515/jpem-2020-0418.
Garvey W, Mechanick J, Brett E, Garber A, Hurley D, Jastreboff A, et al. American Association of Clinical Endocrinologists and American College of Endocrinology Comprehensive Clinical Practice Guidelines for Medical Care of Patients with Obesity. Endocr Pract. 2016;22 Suppl 3. https://doi.org/10.4158/EP161365.GL
Lindeman C, Jones A, Klein D, Prado C, Pham A, Spence J, et al. Measurement of obesity in primary care practice: chronic conditions matter. Fami Pract. 2022;39(5). https://doi.org/10.1093/fampra/cmab170.
Goodman E, Daniels S, Meigs J, Dolan L. Instability in the diagnosis of metabolic syndrome in adolescents. Circulation. 2007;115(17). https://doi.org/10.1161/CIRCULATIONAHA.106.669994.
Ventura E, Lane C, Weigensberg M, Toledo-Corral C, Davis J, Goran M. Persistence of the metabolic syndrome over 3 annual visits in overweight Hispanic children: association with progressive risk for type 2 diabetes. J Pediatr. 2009;155(4). https://doi.org/10.1016/j.jpeds.2009.04.008.
Gustafson J, Yanoff L, Easter B, Brady S, Keil M, Roberts M,S et al. The stability of metabolic syndrome in children and adolescents. J Clin Endocrinol Metab. 2009;94(12). https://doi.org/10.1210/jc.2008-2665.
Stanley T, Chen M, Goodman E. The typology of metabolic syndrome in the transition to adulthood. J Clin Endocrinol Metab. 2014;99(3).https://doi.org/10.1210/jc.2013-3531.
Group DPPR. Long-term effects of lifestyle intervention or metformin on diabetes development and microvascular complications over 15-year follow-up: the Diabetes Prevention Program Outcomes Study. Lancet Diabetes Endocrinol. 2015;3(11). https://doi.org/10.1016/S2213-8587(15)00291-0.
Steinberger J, Daniels S. Obesity, insulin resistance, diabetes, and cardiovascular risk in children: an American Heart Association scientific statement from the Atherosclerosis, Hypertension, and Obesity in the Young Committee (Council on Cardiovascular Disease in the Young) and the Diabetes Committee (Council on Nutrition, Physical Activity, and Metabolism). Circulation. 2003;107(10). https://doi.org/10.1161/01.cir.0000060923.07573.f2.
Adolescents EPoIGfCHaRRiCa, National Heart L, and Blood Institute. Expert panel on integrated guidelines for cardiovascular health and risk reduction in children and adolescents: summary report. Pediatrics. 2011;128 Suppl 5(Suppl 5). https://doi.org/10.1542/peds.2009-2107C.
Brown C, Halvorson E, Cohen G, Lazorick S, Skelton J. Addressing childhood obesity: opportunities for prevention. Pediatr Clin North Am. 2015;62(5). https://doi.org/10.1016/j.pcl.2015.05.013.
Mihrshahi S, Gow M, Baur L. Contemporary approaches to the prevention and management of paediatric obesity: an Australian focus. Med J Aust. 2018;209(6). https://doi.org/10.5694/mja18.00140.
Hampl S, Hassink S, Skinner A, Armstrong S, Barlow S, Bolling C, et al. Clinical practice guideline for the evaluation and treatment of children and adolescents with obesity. Pediatrics. 2023. https://doi.org/10.1542/peds.2022-060640.
Barlow S, Richert M, Baker E. Putting context in the statistics: paediatricians' experiences discussing obesity during office visits. Child Care Health Dev. 2007;33(4). https://doi.org/10.1111/j.1365-2214.2006.00716.x.
Jones K, Dixon M, Dixon J. GPs, families and children's perceptions of childhood obesity. Obes Res Clin Pract. 2014;8(2). https://doi.org/10.1016/j.orcp.2013.02.001.
Turner G, Owen S, Watson P. Addressing childhood obesity at school entry: qualitative experiences of school health professionals. J Child Health Care. 2016;20(3). https://doi.org/10.1177/1367493515587061.
Liebhart J, Goodman A, Lindros J, Krafft C, Cook S, Baker A, et al. Key predictors of primary care providers' self-efficacy in caring for children with overweight or obesity. Acad Pediatr. 2022;22(7). https://doi.org/10.1016/j.acap.2022.02.017.
Lipek T, Igel U, Gausche R, Kiess W, Grande G. Obesogenic environments: environmental approaches to obesity prevention. J Pediatr Endocrinol Metab. 2015;28(5–6). https://doi.org/10.1515/jpem-2015-0127.
Sallis J, Floyd M, Rodríguez D, Saelens B. Role of built environments in physical activity, obesity, and cardiovascular disease. Circulation. 2012;125(5). https://doi.org/10.1161/CIRCULATIONAHA.110.969022.
Fall T, Mendelson M, Speliotes E. Recent advances in human genetics and epigenetics of adiposity: pathway to precision medicine? Gastroenterology. 2017;152(7). https://doi.org/10.1053/j.gastro.2017.01.054.
Lovasi G, Hutson M, Guerra M, Neckerman K. Built environments and obesity in disadvantaged populations. Epidemiologic Rev. 2009;31. https://doi.org/10.1093/epirev/mxp005.
Swinburn B, Egger G, Raza F. Dissecting obesogenic environments: the development and application of a framework for identifying and prioritizing environmental interventions for obesity. Prev Med. 1999;29(6 Pt 1). https://doi.org/10.1006/pmed.1999.0585.
Israel B, Schulz A, Parker E, Becker A. Critical issues in developing and following community-based participatory research principles. In: Minkler M, Wallerstein N, editors. Community-Based Participatory Research for Health. San Francisco: Jossey-Bass; 2008. p. 47–62.
Sallis J, Owen N, Fisher E. Ecological models of health behavior. In: Glanz K, Rimer B, Viswanath K, editors. Health behavior and health education. 4th ed. San Francisco: John Wiley & Sons; 2008. p. 465–85.
Wallerstein N, Duran B. The conceptual, historical and practice roots of community-based participatory research and related participatory traditions. In: Minkler M, Wallerstein N, editors. Community-based participatory research for health. 1st ed. San Francisco: Jossey-Bass; 2003. p. 27–52.
Javed Z, Valero-Elizondo J, Maqsood M, Mahajan S, Taha M, Patel K, et al. Social determinants of health and obesity: findings from a national study of US adults. Obesity (Silver Spring, Md). 2022;30(2). https://doi.org/10.1002/oby.23336.
Adams E, Caccavale L, Smith D, Bean M. Food insecurity, the home food environment, and parent feeding practices in the era of COVID-19. Obesity (Silver Spring, Md). 2020;28(11). https://doi.org/10.1002/oby.22996.
•• Kumanyika S. Advancing health equity efforts to reduce obesity: changing the course. Ann Rev Nutr. 2022;42. https://doi.org/10.1146/annurev-nutr-092021-050805. (Highlights how numerous inequities across the lifespan lead to disparities in obesity prevalence with a focus on Black Americans and provides recommendations for equity.)
Loring B, Robertson A. Obesity and inequities: guidance for addressing inequities in overweight and obesity. 2014. https://apps.who.int/iris/handle/10665/344619. Accessed 1/8/2023
Felitti V, Anda R, Nordenberg D, Williamson D, Spitz A, Edwards V, et al. Relationship of childhood abuse and household dysfunction to many of the leading causes of death in adults. The Adverse Childhood Experiences (ACE) Study. Am J Prev Med. 1998;14(4). https://doi.org/10.1016/s0749-3797(98)00017-8.
Hughes K, Bellis M, Hardcastle K, Sethi D, Butchart A, Mikton C, et al. The effect of multiple adverse childhood experiences on health: a systematic review and meta-analysis. Lancet Public Health. 2017;2(8). https://doi.org/10.1016/S2468-2667(17)30118-4.
Schroeder K, Schuler B, Kobulsky J, Sarwer D. The association between adverse childhood experiences and childhood obesity: a systematic review. Obes Rev. 2021;22(7). https://doi.org/10.1111/obr.13204.
•• Herbozo S, Brown K, Burke N, LaRose J. A call to reconceptualize obesity treatment in service of health equity: review of evidence and future directions. Curr Obes Rep. 2023. https://doi.org/10.1007/s13679-023-00493-5. (Describes many factors leading to disparities in obesity affecting Black and Latino adults and provides recommendations for equity.)
Bailey Z, Krieger N, Agénor M, Graves J, Linos N, Bassett M. Structural racism and health inequities in the USA: evidence and interventions. Lancet (London, England). 2017;389(10077). https://doi.org/10.1016/S0140-6736(17)30569-X.
Bailey Z, Feldman J, Bassett M. How structural racism works—racist policies as a root cause of U.S. racial health inequities. N Engl J Med. 2021;384(8). https://doi.org/10.1056/NEJMms2025396.
Jones C. The impact of racism on health. Ethn Dis. 2002;12(1).
Jones C, Jones C, Perry G, Barclay G, Jones C. Addressing the social determinants of children's health: a cliff analogy. J Health Care Poor Underserved. 2009;20(4 Suppl). https://doi.org/10.1353/hpu.0.0228.
Peek M. Racism and health: a call to action for health services research. Health Serv Res. 2021;56(4). https://doi.org/10.1111/1475-6773.13693.
Vela M, Erondu A, Smith N, Peek M, Woodruff J, Chin M. Eliminating explicit and implicit biases in health care: evidence and research needs. Ann Rev Public Health. 2022;43. https://doi.org/10.1146/annurev-publhealth-052620-103528.
Golden S. The contribution of structural racism to metabolic health disparities in the USA. Lancet Diabetes Endocrinol. 2021;9(8). https://doi.org/10.1016/S2213-8587(21)00144-3.
Browne N, Hodges E, Small L, Snethen J, Frenn M, Irving S, et al. Childhood obesity within the lens of racism. Pediatr Obes. 2022;17(5). https://doi.org/10.1111/ijpo.12878.
Grier S, Kumanyika S. The context for choice: health implications of targeted food and beverage marketing to African Americans. Am J Public Health. 2008;98(9). https://doi.org/10.2105/AJPH.2007.115626.
Kumanyika S. The sociocultural context for obesity prevention and treatment in children and adolescents: influences of ethnicity and gender. In: Freemark M (ed) Pediatric Obesity: Etiology, Pathogenesis and Treatment. Springer International Publishing; 2018. p. 695–713
Wu A, Aris I, Hivert M, Rocchio C, Cocoros N, Klompas M, et al. Association of changes in obesity prevalence with the COVID-19 pandemic in youth in Massachusetts. JAMA pediatrics. 2022;176(2). doi:https://doi.org/10.1001/jamapediatrics.2021.5095.
Dietz W. The COVID-19 lockdown increased obesity disparities; will the increases in type 2 diabetes continue? Obesity (Silver Spring, Md). 2022. https://doi.org/10.1002/oby.23662.
Bullock A, Sheff K, Moore K, Manson S. Obesity and overweight in American Indian and Alaska native children, 2006–2015. Am J Public Health. 2017;107(9). https://doi.org/10.2105/AJPH.2017.303904.
Lo C, Ash-Houchen W, Gerling H, Cheng T. Data spanning three decades illustrate racial disparities in likelihood of obesity. Ethn Health. 2020;25(5). https://doi.org/10.1080/13557858.2018.1447650.
Mannheim J, Konda S, Logan L. Racial, ethnic and socioeconomic disparities in SARS-CoV-2 infection amongst children. Paediatr Perinat Epidemiol. 2022;36(3). https://doi.org/10.1111/ppe.12865.
Belanger M, Hill M, Angelidi A, Dalamaga M, Sowers J, Mantzoros C. Covid-19 and disparities in nutrition and obesity. N Engl J Med. 2020;383(11). https://doi.org/10.1056/NEJMp2021264.
Puhl R, Himmelstein M, Armstrong S, Kingsford E. Adolescent preferences and reactions to language about body weight. Int J Obes (2005). 2017;41(7). https://doi.org/10.1038/ijo.2017.55.
Sonneville K, Mulpuri L, Khreizat I, Nichols L, Plegue M, Chang T. Youth preferences for weight-related conversations. Health Commun. 2020;35(11).https://doi.org/10.1080/10410236.2019.1631566.
Alberga A, Pickering B, Alix Hayden K, Ball G, Edwards A, Jelinski S, et al. Weight bias reduction in health professionals: a systematic review. Clin Obes. 2016;6(3). https://doi.org/10.1111/cob.12147.
Resnicow K, Davis R, Rollnick S. Motivational interviewing for pediatric obesity: conceptual issues and evidence review. J Am Diet Assoc. 2006;106(12).https://doi.org/10.1016/j.jada.2006.09.015.
Resnicow K, Harris D, Wasserman R, Schwartz R, Perez-Rosas V, Mihalcea R, et al. Advances in motivational interviewing for pediatric obesity: results of the brief motivational interviewing to reduce body mass index trial and future directions. Pediatr Clin North Am. 2016;63(3). https://doi.org/10.1016/j.pcl.2016.02.008.
Christie D, Channon S. The potential for motivational interviewing to improve outcomes in the management of diabetes and obesity in paediatric and adult populations: a clinical review. Diabetes Obes Metab. 2014;16(5). https://doi.org/10.1111/dom.12195.
Brown C, Perrin E. Obesity prevention and treatment in primary care. Acad Pediatr. 2018;18(7). https://doi.org/10.1016/j.acap.2018.05.004.
Venkataramani M, Cheng T, Yeh H, Maruthur N. Lifestyle intervention programs for adults at high-risk for type 2 diabetes: a platform to reach high-risk children? J Am Board Fam Med: JABFM. 2019;32(4). https://doi.org/10.3122/jabfm.2019.04.180317.
Weir K. Family-based behavioral treatment is key to addressing childhood obesity. Monit Psychol. 2019;50(4):30.
Wilfley D, Saelens B, Stein R, Best J, Kolko R, Schechtman K, et al. Dose, content, and mediators of family-based treatment for childhood obesity: a multisite randomized clinical trial. JAMA Pediatr. 2017;171(12). https://doi.org/10.1001/jamapediatrics.2017.2960.
Verrotti A, Penta L, Zenzeri L, Agostinelli S, De Feo P. Childhood obesity: prevention and strategies of intervention. A systematic review of school-based interventions in primary schools. J Endocrinol Invest. 2014;37(12). https://doi.org/10.1007/s40618-014-0153-y.
Yuksel H, Şahin F, Maksimovic N, Drid P, Bianco A. School-based intervention programs for preventing obesity and promoting physical activity and fitness: a systematic review. Int J Environ Res Public Health. 2020;17(1).https://doi.org/10.3390/ijerph17010347.
Ho T, Cheng L, Lau Y. School-based interventions for the treatment of childhood obesity: a systematic review, meta-analysis and meta-regression of cluster randomised controlled trials. Public Health Nutr. 2021;24(10). https://doi.org/10.1017/S1368980021001117.
Choudhry S, McClinton-Powell L, Solomon M, Davis D, Lipton R, Darukhanavala A et al. Power-up: a collaborative after-school program to prevent obesity in African American children. Prog Community Health Partnersh. 2011;5(4).
Wang Y, Cai L, Wu Y, Wilson R, Weston C, Fawole O, et al. What childhood obesity prevention programmes work? A systematic review and meta-analysis. Obes Rev. 2015;16(7). https://doi.org/10.1111/obr.12277.
Group HS, Foster G, Linder B, Baranowski T, Cooper D, Goldberg L, et al. A school-based intervention for diabetes risk reduction. N Engl J Med. 2010;363(5). https://doi.org/10.1056/NEJMoa1001933.
Burnet D, Plaut A, Wolf S, Huo D, Solomon M, Dekayie G, et al. Reach-out: a family-based diabetes prevention program for African American youth. J Natl Medi Assoc. 2011;103(3). https://doi.org/10.1016/s0027-9684(15)30290-x.
Goddu A, Roberson T, Raffel K, Chin M, Peek M. Food Rx: a community-university partnership to prescribe healthy eating on the South Side of Chicago. J Prev Interv Commun. 2015;43(2). https://doi.org/10.1080/10852352.2014.973251.
Gunter K, Peek M, Tanumihardjo J, Carbrey E, Crespo R, Johnson T, et al. Population health innovations and payment to address social needs among patients and communities with diabetes. Milbank Q. 2021;99(4). https://doi.org/10.1111/1468-0009.12522.
Cené C, Viswanathan M, Fichtenberg C, Sathe N, Kennedy S, Gottlieb L, et al. Racial health equity and social needs interventions: a review of a scoping review. JAMA Netw Open. 2023;6(1). https://doi.org/10.1001/jamanetworkopen.2022.50654.
Schroeder K, McCormick R, Perez A, Lipman T. The role and impact of community health workers in childhood obesity interventions: a systematic review and meta-analysis. Obes Rev. 2018;19(10). https://doi.org/10.1111/obr.12714.
Blanck H, Hacker K, Petersen R. Setting the stage for reimbursable pediatric healthy weight programs. Child Obes (Print). 2021;17(S1). https://doi.org/10.1089/chi.2021.29012.
Gray J, Spear F, S, Santos M, Ward W, Davis A. The status of billing and reimbursement in pediatric obesity treatment programs. J Behav Health Serv Res. 2013;40(3). https://doi.org/10.1007/s11414-012-9308-9.
Wilfley D, Staiano A, Altman M, Lindros J, Lima A, Hassink S et al. Improving access and systems of care for evidence-based childhood obesity treatment: conference key findings and next steps. Obesity (Silver Spring, Md). 2017;25(1). https://doi.org/10.1002/oby.21712.
Kyle T, Stanford F. Moving toward health policy that respects both science and people living with obesity. Nurs Clin N Am. 2021;56(4). https://doi.org/10.1016/j.cnur.2021.08.003.
Mande J, Flaherty G. Supplemental Nutrition Assistance Program as a health intervention. Curr Opin Pediatr. 2023;35(1). https://doi.org/10.1097/MOP.0000000000001192.
Popkin B, Barquera S, Corvalan C, Hofman K, Monteiro C, Ng S et al. Towards unified and impactful policies to reduce ultra-processed food consumption and promote healthier eating. Lancet Diabetes Endocrinol. 2021;9(7). https://doi.org/10.1016/S2213-8587(21)00078-4.
Fisberg M, Maximino P, Kain J, Kovalskys I. Obesogenic environment—intervention opportunities. J Pediatria. 2016;92(3 Suppl 1). https://doi.org/10.1016/j.jped.2016.02.007.
StateofChildhoodObesity. Meeting the Moment - Learning From Leaders at the Forefront of Change.2022 11–15.
Funding
Dedeepya Konuthula is supported by the University of Chicago Primary Care Investigators Training in Chronic Disease & Health Disparities (PITCH) Fellowship (Health Resources and Services Administration T32 HP42019). Deborah Burnet is supported in part by research funding through an NIH Clinical and Translation Science Award for the U Chicago Institute for Translational Research Community Cluster and through the NIDDK 2P30DK092949-11 for the Chicago Center for Diabetes Translation Research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Konuthula, D., Tan, M.M. & Burnet, D.L. Challenges and Opportunities in Diagnosis and Management of Cardiometabolic Risk in Adolescents. Curr Diab Rep 23, 185–193 (2023). https://doi.org/10.1007/s11892-023-01513-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11892-023-01513-3