Abstract
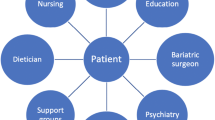
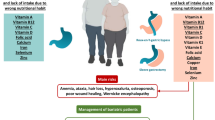
Roux-en-Y gastric bypass surgery remains the major surgical option for individuals with medically complicated obesity. The importance of preoperative evaluation to permit identification of micronutrient deficiencies is being re-evaluated. The risk of complications related to pregnancy after gastric bypass supports careful follow-up. Micronutrient deficiencies are common in postoperative gastric bypass patients, despite the suggested use of routine vitamin and mineral supplements after surgery. Copper deficiency must be considered as an origin for visual disorders after gastric bypass. Vitamin D deficiency with metabolic bone disease remains common after gastric bypass and the results suggest that the present postoperative supplements of calcium and vitamin D are inadequate. Major nutritional complications of bariatric surgery are occurring more than 20 years after surgery. There is no evidence for intestinal adaptation as there remains decreased intestinal absorption of iron up to 18 months after gastric bypass surgery. This article supports ongoing examination of nutritional complications after gastric bypass surgery and supports the notion that the daily doses of micronutrient supplements, such as vitamin D, may need to be revised.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Flegal KM, Carroll MD, Ogden CL, Curtin LR.: Prevalence and trends in obesity among US adults, 1999–2008. JAMA 2010, 303(3): 235–41.
Buchwald H, Oien DM. Metabolic/bariatric surgery Worldwide 2008.: Obes Surg 2009, 19: 1605–1611.
Makary MA, Clarke JM, Shore AD, et al.: Medication utilization and annual health care costs in patients with type 2 diabetes mellitus before and after bariatric surgery. Arch Surg 2010, 145(8): 726–31.
Sechi GP. Dietary supplements and the risk of Wernicke’s encephalopathy. Clin Pharmacol Ther 2010; 88: 164.
Schweiger C, Weiss R, Berry E, et al.: Nutritional deficiencies in bariatric surgery candidates. Obes Surg 2010, 20(2): 193–7.
Gehrer S, Kern B, Peters T, et al.: Fewer nutrient deficiencies after laparoscopic sleeve gastrectomy (LSG) than after laparoscopic Roux-Y-gastric bypass (LTYGB)—a prospective study. Obes Surg 2010, 20(4): 447–53.
Shea MK, Booth SL, Gundberg CM, et al.: Adulthood obesity is positively associated with adipose tissue concentrations of vitamin K and inversely associated with circulating indicators of vitamin K status in men and women. J Nutr 2010, 140(5): 1029–34.
Pereira S, Saboya C, Chaves G, et al.: Class III obesity and its relationship with the nutritional status of vitamin A in pre- and postoperative gastric bypass. Obes Surg 2009, 19(6): 738–44.
• Eerdekens A, Debeer A, Van Hoey G, et al.: Maternal bariatric surgery: adverse outcomes in neonates. Eur J Pediatr 2010, 169(2): 191–6. This report describes five babies with intracranial hemorrhage whose mothers had undergone bariatric surgery. The report suggests the potential for vitamin K deficiency.
Dalcanale L, Oliveira CP, Faintuch J, et al.: Long-term nutritional outcome after gastric bypass. Obes Surg 2010, 20(2): 181–7.
Toh SY, Zarshenas N, Jorgensen J.: Prevalence of nutrient deficiencies in bariatric patients. Nutrition 2009, 25(11–12): 1150–6.
Lakhani SV, Shah HN, Alexander K, Finelli FC, Kirkpatrick JR, Koch TR.: Small intestinal bacterial overgrowth and thiamine deficiency after Roux-en-Y gastric bypass surgery in obese patients. Nutrition Res 2008, 28(5): 293–298.
Rounis E, Laing CM, Davenport A.: Acute neurological presentation due to copper deficiency in a hemodialysis patient following gastric bypass surgery. Clin Nephrol 2010, 74(5): 389–92.
Spyropoulos C, Kehagias I, Panagiotopoulos S, et al.: Revisional bariatric surgery: 13-year experience from a tertiary institution. Arch Surg 2010, 145(2): 173–7.
• Naismith RT, Shepherd JB, Weihl CC, et al.: Acute and bilateral blindness due to optic neuropathy associated with copper deficiency. Arch Neurol 2009, 66(8): 1025–7. A patient 22 years after gastric bypass surgery developed bilateral blindness due to optic neuropathy. Copper deficiency was identified.
Jayakumar S, Micallef-Eynaud PD, Lyon TD, et al.: Acquired copper deficiency following prolonged jejunostomy feeds. Ann Clin Biochem 2005, 42(3), 227–231.
Genead MA, Fishman GA, Lindeman M.: Fundus white spots and acquired night blindness due to vitamin A deficiency. Doc Ophthalmol 2009, 119(3): 229–33.
• Al-Shoha A, Qui S, Palnitkar S, et al.: Osteomalacia with bone marrow fibrosis due to severe vitamin D deficiency after a gastrointestinal bypass operation for severe obesity. Endocr Pract 2009, 15(6): 528–33. This article discusses patients with bone biopsy-proven osteomalacia with marrow fibrosis; symptoms were present for 2 to 5 years after gastric bypass surgery. Significant improvement occurred after treatment with ergocalciferol (100,000 IU daily) and calcium carbonate (1 to 2.5 g daily).
Valderas JP, Velasco S, Solari S, et al.: Increase of bone resorption and the parathyroid hormone in postmenopausal women in the long-term after Roux-en-Y gastric bypass. Obes Surg 2009, 19(8): 1132–8.
Mechanick JI, Kushner RF, Sugerman HJ, Gonzalez-Campoy JM, Collazo-Clavell ML, Spitz AF, Apovian CM, Livingston EH, Brolin R, Sarwer DB, Anderson WA, Dixon J, Guven S.: American Association of Clinical Endocrinologists, the Obesity Society, and American Society for Metabolic & Bariatric Surgery medical guidelines for clinical practice for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient. Obesity 2009;17 Suppl 1:S1–70.
• Signori C, Zalesin KC, Franklin B, et al.: Effect of gastric bypass on vitamin D and secondary hyperparathyroidism. Obes Surg 2010, 20(7): 949–52. Eighty-six percent of gastric bypass patients had preoperative vitamin D deficiency, whereas at the 1-year postoperative follow-up, 70% of patients still had evidence for inadequate blood levels of vitamin D.
Sung CC, Lee HS, Diang LK, et al.: Refractory diffuse bony pain 20 years after jejunoileal bypass. South Med J 2010, 103(6): 570–3.
Ruz M, Carrasco F, Rojas P, et al.: Iron absorption and iron status are reduced after Roux-en-Y gastric bypass. Am J Clin Nutr 2009, 90(3): 527–32.
Avgerinos DV, Llaguna OH, Seigerman M, et al.: Incidence and risk factors for the development of anemia following gastric bypass surgery. World J Gastroenterol 2010, 16(15): 1867–70.
Bal B, Koch TR, Finelli FC, Sarr MG.: Management of medical and surgical disorders after divided Roux-en-Y gastric bypass surgery. Nat Rev Gastroenterol Hepatol 2010, 7(6): 320–334.
Iannelli A, Addeo P, Novellas S, et al.: Wernicke’s encephalopathy after laparoscopic Roux-en-Y gastric bypass: a misdiagnosed complication. Obes Surg 2010, 20(11): 1594–6.
Sebastian JL, V JM, Tang LW, et al.: Thiamine deficiency in a gastric bypass patient leading to acute neurologic compromise after plastic surgery. Surg Obes Relat Dis 2010, 6(1): 105–6.
• Francini-Pesenti F, Brocadello F, et al.: Wernicke’s syndrome during parenteral feeding: not an unusual complication. Nutrition 2009, 25(2): 142–6. The authors discuss the potential effects of parenteral feedings on the development of thiamine deficiency. This question of consumption may be very important in patients after gastric bypass surgery in whom parenteral nutrition is being considered for potential protein-calorie malnutrition.
• Paparrigopoulos T, Tzavelas E, Karaiskos D, et al.: Complete recovery from undertreated Wernicke-Korsakoff syndrome following aggressive thiamine treatment. In Vivo 2010, 24(2): 231–3. This is a report of improved recovery from Wernicke’s syndrome by using high-dose oral thiamine (600 mg/day) and intramuscular thiamine (300 mg/day) for 2 months.
Disclosure
No potential conflicts of interest relevant to this article were reported.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bal, B.S., Finelli, F.C. & Koch, T.R. Origins of and Recognition of Micronutrient Deficiencies After Gastric Bypass Surgery. Curr Diab Rep 11, 136–141 (2011). https://doi.org/10.1007/s11892-010-0169-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11892-010-0169-4