Abstract
Background and Aims
Endoscopy is effective in management of bariatric surgery (BS) adverse events (AEs) but a comprehensive evaluation of long-term results is lacking. Our aim is to assess the effectiveness of a standardized algorithm for the treatment of BS-AE.
Patients and Methods
We retrospectively analyzed 1020 consecutive patients treated in our center from 2012 to 2020, collecting data on demographics, type of BS, complications, and endoscopic treatment. Clinical success (CS) was evaluated considering referral delay, healing time, surgery, and complications type. Logistic regression was performed to identify variables of CS.
Results
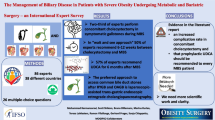
In the study period, we treated 339 fistulae (33.2%), 324 leaks (31.8%), 198 post-sleeve gastrectomy twist/stenosis (19.4%), 95 post-RYGB stenosis (9.3 %), 37 collections (3.6%), 15 LAGB migrations (1.5%), 7 weight regains (0.7%), and 2 hemorrhages (0.2%). Main endoscopic treatments were as follows: pigtail-stent positioning under endoscopic view for both leaks (CS 86.1%) and fistulas (CS 77.2%), or under EUS-guidance for collections (CS 88.2%); dilations and/or stent positioning for sleeve twist/stenosis (CS 80.6%) and bypass stenosis (CS 81.5%). After a median (IQR) follow-up of 18.5 months (4.29–38.68), complications rate was 1.9%. We found a 1% increased risk of redo-surgery every 10 days of delay to the first endoscopic treatment. Endoscopically treated patients had a more frequent regular diet compared to re-operated patients.
Conclusions
Endoscopic treatment of BS-AEs following a standardized algorithm is safe and effective. Early endoscopic treatment is associated with an increased CS rate.
Graphical abstract


Similar content being viewed by others
References
Ponce J, DeMaria EJ, Nguyen NT, et al. American Society for Metabolic and Bariatric Surgery estimation of bariatric surgery procedures in 2015 and surgeon workforce in the United States. Surg Obes Relat Dis. 2016;12(9):1637–9.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292(14):1724–37.
Altieri MS, Pryor A, Bates A, et al. Bariatric procedures in adolescents are safe in accredited centers. Surg Obes Relat Dis. 2018;14(9):1368–72.
Lainas P, Dammaro C, Gaillard M, et al. Safety and short-term outcomes of laparoscopic sleeve gastrectomy for patients over 65 years old with severe obesity. Surg Obes Relat Dis. 2018;14(7):952–9.
Jaruvongvanich V, Wongjarupong N, Vantanasiri K, et al. Midterm outcome of laparoscopic sleeve gastrectomy in Asians: a systematic review and meta-analysis. Obes Surg. 2020;30(4):1459–67.
Arterburn DE, Courcoulas AP. Bariatric surgery for obesity and metabolic conditions in adults. BMJ. 2014 Aug 27;349:g3961. https://doi.org/10.1136/bmj.g3961
Chang SH, Stoll CR, Song J, et al. The effectiveness and risks of bariatric surgery: an updated systematic review and meta-analysis, 2003-2012. JAMA Surg. 2014;149(3):275–87.
Siddique I, Alazmi W, Al-Sabah SK. Endoscopic internal drainage by double pigtail stents in the management of laparoscopic sleeve gastrectomy leaks. Surg Obes Relat Dis. 2020;16(7):831–8.
Lorenzo D, Guilbaud T, Gonzalez JM, et al. Endoscopic treatment of fistulas after sleeve gastrectomy: a comparison of internal drainage versus closure. Gastrointest Endosc. 2018;87(2):429–37.
Smith ZL, Park KH, Llano EM, et al. Outcomes of endoscopic treatment of leaks and fistulae after sleeve gastrectomy: results from a large multicenter U.S. cohort. Surg Obes Relat Dis. 2019;15(6):850–5.
Granata A, Amata M, Ligresti D, et al. Endoscopic management of post-surgical GI wall defects with the overstitch endosuturing system: a single-center experience. Surg Endosc. 2020;34(9):3805–17.
Eisendrath P, Deviere J. Major complications of bariatric surgery: endoscopy as first-line treatment. Nat Rev Gastroenterol Hepatol. 2015;12(12):701–10.
Rosenthal RJ. International Sleeve Gastrectomy Expert Panel, Diaz AA, Arvidsson D, Baker RS, Basso N, Bellanger D, Boza C, El Mourad H, France M, Gagner M, Galvao-Neto M, Higa KD, Himpens J, Hutchinson CM, Jacobs M, Jorgensen JO, Jossart G, Lakdawala M, Nguyen NT, Nocca D, Prager G, Pomp A, Ramos AC, Rosenthal RJ, Shah S, Vix M, Wittgrove A, Zundel N. International Sleeve Gastrectomy Expert Panel Consensus Statement: best practice guidelines based on experience of >12,000 cases. Surg Obes Relat Dis. 2012 Jan-Feb;8(1):8–19. https://doi.org/10.1016/j.soard.2011.10.019.
Hamed H, Said M, Elghadban H, et al. Outcome and adverse events of endoscopic bariatric stents for management of leakage after bariatric surgery. Obes Surg. 2020;30(3):982–91.
Donatelli G, Dumont J-L, Cereatti F, et al. Treatment of leaks following sleeve gastrectomy by endoscopic internal drainage (EID). Obes Surg. 2015;25(7):1293–301.
Gonzalez JM, Lorenzo D, Guilbaud T, et al. Internal endoscopic drainage as first line or second line treatment in case of postsleeve gastrectomy fistulas. Endosc Int Open. 2018;6(6):E745–50.
Cosse C, Rebibo L, Brazier F, et al. Cost-effectiveness analysis of stent type in endoscopic treatment of gastric leak after laparoscopic sleeve gastrectomy. Br J Surg. 2018;105(5):570–7.
Giuliani A, Romano L, Marchese M, et al. Gastric leak after laparoscopic sleeve gastrectomy: management with endoscopic double pigtail drainage. A systematic review. Surg Obes Relat Dis. 2019;15(8):1414–9.
Bona D, Giovannelli A, Micheletto G, et al. Treatment of persistent leaks after laparoscopic sleeve gastrectomy with the simultaneous over-the-scope clip (OTSC) and mega stent strategy. Obes Surg. 2020;30(9):3615–9.
Kuehn F, Loske G, Schiffmann L, et al. Endoscopic vacuum therapy for various defects of the upper gastrointestinal tract. Surg Endosc. 2017;31(9):3449–58.
Gjeorgjievski M, Imam Z, Cappell MS, Jamil LH, Kahaleh M. A Comprehensive Review of Endoscopic Management of Sleeve Gastrectomy Leaks. J Clin Gastroenterol. 2021 Aug 1;55(7):551–576. https://doi.org/10.1097/MCG.0000000000001451.
Baumann AJ, Mramba LK, Hawkins RB, et al. Endoscopic dilation of bariatric RNY anastomotic strictures: a systematic review and meta-analysis. Obes Surg. 2018;28(12):4053–63.
Majumder S, Buttar NS, Gostout C, et al. Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures. Endosc Int Open. 2016;4:E96–E101.
Benosman H, Rahmi G, Perrod G, et al. Endoscopic management of post-bariatric surgery fistula: a tertiary care center experience. Obes Surg. 2018 Dec;28(12):3910–5.
Chang SH, Popov VB, Thompson CC. Endoscopic balloon dilation for treatment of sleeve gastrectomy stenosis: a systematic review and meta-analysis. Gastrointest Endosc. 2020;91(5):989–1002.e4.
Christophorou D, Valats J-C, Funakoshi N, et al. Endoscopic treatment of fistula after sleeve gastrectomy: results of a multicenter retrospective study. Endoscopy. 2015;47(11):988–96.
Warren J, Bhalla V, Cresci G. Postoperative diet advancement: surgical dogma vs evidence-based medicine. Nutr Clin Pract. 2011;26(2):115–25. https://doi.org/10.1177/0884533611400231.
Watson MD, Hunter Mehaffey J, Schirmer BD, et al. Roux-en-Y gastric bypass following Nissen Fundoplication: higher risk same reward. Obes Surg. 2017;27(9):2398–403.
Weusten BLAM, Barret M, Bredenoord AJ, et al. Endoscopic management of gastrointestinal motility disorders - part 2: European Society of Gastrointestinal Endoscopy (ESGE) Guideline. Endoscopy. 2020;52(7):600–14.
Donatelli G, Dumont J-L, Pourcher G, et al. Pneumatic dilation for functional helix stenosis after sleeve gastrectomy: long-term follow-up (with videos). Surg Obes Relat Dis. 2017;13(6):943–50.
Donatelli G, Cereatti F. “Double cut technique” for endoscopic removal of eroded adjustable gastric band without previous surgical extraction of port and connection tube. Surg Obes Relat Dis. 2019;15(2):342–4.
Abu Dayyeh BK, Lautz DB, Thompson CC. Gastrojejunal stoma diameter predicts weight regain after Roux-en-Y gastric bypass. Clin Gastroenterol Hepatol. 2011;9(3):228–33.
Acknowledgements
We are thankful to all the Anesthesia Care Team of Hôpital Privé des Peupliers for the clinical support before, during, and after all endoscopic treatments.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
-Endoscopy is effective in management of bariatric surgery adverse events.
-Application of a standardized algorithm allowed a high clinical success rate.
-Early endoscopic treatment is associated with increased endoscopic clinical success.
Appendix. Adverse events standardized definition and treatment
Appendix. Adverse events standardized definition and treatment
Leak
Definition Any disruption of the staple line or dehiscence of anastomosis with spillage of fluid, with or without a concomitant collection.
Treatment Leak treatment consists in the insertion of one/multiple double pigtail stents (DPS) and simultaneous positioning of a naso-jejunal feeding tube (NJT) for the first 4 weeks. The aim is to achieve an endoscopic internal drainage (EID) safeguarding the enteral feeding. This promotes granulation tissue with progressive collapse of the abscess cavity. Whenever possible, endoscopic exploration of the abscess cavity allows to perform lavage and/or necrosectomy. The first endoscopic follow-up is scheduled after 4 weeks. Per protocol, at first follow-up, DPS are left in place whereas the NJT is removed and the patient is allowed to restart the oral diet. Second endoscopic follow-up is scheduled 3 months later to remove the DPS or, if the abscess cavity persists, to perform their replacement and continue treatment for three more months.
Success Criteria Absence of contrast agent extravasation with normal C-reactive protein and white blood cells, no need for antibiotic therapy, normal oral intake and no chronic pain.
Fistula
Definition Any communication between two epithelialized structures — i.e., gastro-bronchial, gastro-jejunal, gastro-colic, or gastro-cutaneous (all cases with surgical or radiological drainage were considered presenting an iatrogenic gastro-cutaneous fistula).
Treatment For acute fistula with percutaneous drainage still in place, EID with DPS is performed in order to reverse liquid flow into the stomach, thus allowing firstly to retract and then to remove the percutaneous drainage to avoid the development of a chronic fistula.
In case of a persistent chronic fistula, a septotomy is done during repeated endoscopic sessions. Argon plasma coagulation (APC-Forced Effect 2, Watt 60) is performed coupled with clipping at the base of the endoscopic incision in order to facilitate emptying of the associated collection within the GI lumen, similarly to Zenker diverticula treatment [29].
Success Criteria As for leaks.
Collection
Definition Any well delimited fluid or semi-solid collection, adjacent to the foregut tract and with no direct communication with it, reachable by endoscopic ultrasound (EUS).
Treatment EUS-guided 19-gauge needle puncture is first performed. Then, the entry site is enlarged with a cystotome and hydrostatic dilation. Multiple DPS or a lumen-apposing metal stent (LAMS) is deployed into the cavity. DPS are kept in place for 3 months while LAMS is exchanged after 1 month with DPS; the patient has a normal oral diet.
Success Criteria As for leaks.
Stenosis
Definition A clinically significant narrowing of the upper GI tract related to previous surgery. Depending on the type of surgical procedure, the following stenosis may occur:
-Anastomotic stricture following gastric by-pass (GBP);
-Early stricture following SG, which typically occurs as a consequence of inflammation during the first weeks after surgery being related to hematoma, edema, or erroneous calibration of the gastric tube;
-Functional stenosis (helix stricture/twist), defined as a clockwise rotation of the gastric sleeve altering the regular gastric flow.
Treatment
-Anastomotic stricture after GBP needs multiple endoscopic sessions using hydrostatic dilation up to 15 mm of diameter every 30 days, or deploying a 16×30 mm LAMS for 4 weeks.
-Early inflammatory stricture following SG (< 1 month) is treated conservatively with steroids, coupled, in a minority of cases, with NJT or gastric calibration by LAMS deployment.
-Helix stricture following SG (> 1 month) needs pneumatic dilation up to 30-35-40 mm of diameter in multiple consecutive sessions, 1 min every 3 weeks. For tight or persistent stenosis, a fully covered self-expandable metal stent (FCSEMS) or LAMS can be deployed for 21 days [30].
Success Criteria Regular oral intake without vomiting, associated with a normal swallowing study or an easy exploration with a 9.8-mm gastroscope.
Lap-Band Migration After Erosion
Definition Lap-band migration is diagnosed when erosion of more than 30% of the gastric circumference occurs.
Treatment Cutting of the silicone ring and the connection tube (if port was not removed before) with a 450-cm guide wire and a standard extracorporeal lithotripsy system, followed by its removal with a polypectomy snare [31].
Success Criteria Complete removal of the lap-band with no AE, namely leak/perforation and bleeding/sepsis.
Weight Regain
Definition Any weight increase after RYGB.
Treatment Multiple endoscopic sessions of APC (forced coagulation, 60 watt) at the level of the gastro-jejunal anastomosis are performed in order to induce fibrosis and reduce the diameter of the anastomosis [32].
Success Criteria Interruption of weight regain or recovery of weight loss.
Rights and permissions
About this article
Cite this article
Spota, A., Cereatti, F., Granieri, S. et al. Endoscopic Management of Bariatric Surgery Complications According to a Standardized Algorithm. OBES SURG 31, 4327–4337 (2021). https://doi.org/10.1007/s11695-021-05577-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-021-05577-6