Abstract
Background
Bariatric surgery rapidly induces improvements in type 2 diabetes (T2D) in concert with reduction in systemic markers of inflammation. The impact of bariatric surgery on local intestinal immunity is not known. We hypothesize that sleeve gastrectomy (SG) and gastric bypass (RYGB) surgeries resolve obesity-induced intestinal inflammation, thereby promoting T2D resolution.
Methods
SG and RYGB, or control surgery was performed in SD rats (n = 4–6/group). Key cytokines involved in insulin resistance (TNF-α, IFN-γ), inflammasome activation (IL-1β, IL-18), inflammation resolution (IL-10, IL-33), and Th17 cell responses (IL-17, IL-23) were measured by qPCR in mucosal scrapings of jejunum at 4 weeks post-surgery. Intestinal cytokine expressions were correlated with weight change, systemic and portal glucose, and insulin levels in response to an enteral glucose load.
Results
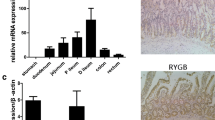
SG downregulated IL-17 and IL-23 in both proximal and distal jejunum, and IFN-γ was reduced only in distal jejunum (p < 0.05). Jejunal IL-17 and IL-23 expression correlated positively with weight changes after SG (0.93 and 0.98, respectively; p < 0.05). Changes in IFN-γ correlated strongly with insulin levels in portal and systemic circulation (0.99 and 0.95, respectively, p < 0.05). As with SG, IFN-γ, IL-17, and IL-23 were significantly reduced by RYGB. RYGB also reduced TNF-α and IL-18 and increased IL-33 levels (p < 0.05).
Conclusions
RYGB and SG reduce expression of pro-inflammatory cytokines IL-17, IL-23, and IFN-γ in the jejunum. RYGB showed attenuation of additional pro-inflammatory cytokines and enhanced expression of IL-33. Post-surgical changes in intestinal IL-17, IL-23, and IFN-γ correlate strongly with changes in weight and glucose-triggered insulin responses.






Similar content being viewed by others
References
Schauer PR, Bhatt DL, Kirwan JP, et al. Bariatric surgery versus intensive medical therapy for diabetes—5-year outcomes. N Engl J Med. 2017;376:641–51.
Wallenius V, Dirinck E, Fändriks L, et al. Glycemic control after sleeve gastrectomy and Roux-en-Y gastric bypass in obese subjects with type 2 diabetes mellitus. Obes Surg. 2017;28:1461–72.
Heshmati K, Harris DA, Aliakbarian H, et al. Comparison of early type 2 diabetes improvement after gastric bypass and sleeve gastrectomy: medication cessation at discharge predicts 1-year outcomes. SOARD.2019; S1550–7289(18)31259-0.
Yarmush ML, D'Alessandro M, Saeidi N. Regulation of energy homeostasis after gastric bypass surgery. Annu Rev Biomed Eng. 2017;19:459–84.
Murphy R, Tsai P, Jüllig M, et al. Differential changes in gut microbiota after gastric bypass and sleeve gastrectomy bariatric surgery vary according to diabetes remission. Obes Surg. 2017;27:917–25.
Osborn O, Olefsky JM. The cellular and signaling networks linking the immune system and metabolism in disease. Nat Med. 2012;18:363–74.
Delzenne NM, Cani PD. Gut microbiota and the pathogenesis of insulin resistance. Curr Diab Rep. 2011;11:154–9.
De Wit NJ, Bosch-Vermeulen H, de Groot PJ, et al. The role of the small intestine in the development of dietary fat-induced obesity and insulin resistance in C57BL/6J mice. BMC Med Genomics. 2008;1:14.
Ding S, Chi MM, Scull BP, et al. High-fat diet: bacteria interactions promote intestinal inflammation which precedes and correlates with obesity and insulin resistance in mouse. PLoS One. 2010;5:e12191.
Spagnuolo MI, Cicalese MP, Caiazzo MA, et al. Relationship between severe obesity and gut inflammation in children: what’s next? Ital J Pediatr. 2010;36:66.
Febbraio MA. Role of interleukins in obesity: implications for metabolic disease. Trends Endocrinol Metab. 2014;25:312–9.
Winer DA, Luck H, Tsai S, et al. The intestinal immune system in obesity and insulin resistance. Cell Metab. 2016;23:413–26.
Rao SR. Inflammatory markers and bariatric surgery: a meta-analysis. Inflamm Res. 2012;61:789–807.
Illán-Gómez F, Gonzálvez-Ortega M, Orea-Soler I, et al. Obesity and inflammation: change in adiponectin, C-reactive protein, tumour necrosis factor-alpha and interleukin-6 after bariatric surgery. Obes Surg. 2012;22:950–5.
Poitou C, Perret C, Mathieu F, et al. Bariatric surgery induces disruption in inflammatory signaling pathways mediated by immune cells in adipose tissue: a RNA-Seq study. PLoS One. 2015;10:e0125718.
Roberts HM, Grant MM, Hubber N, et al. Impact of bariatric surgical intervention on peripheral blood neutrophil (PBN) function in obesity. Obes Surg. 2017;6:1611–21.
Schernthaner GH, Kopp HP, Kriwanek S, et al. Effect of massive weight loss induced by bariatric surgery on serum levels of interleukin-18 and monocyte-chemoattractant-protein-1 in morbid obesity. Obes Surg. 2006;16:709–15.
Mallipedhi A, Prior SL, Barry JD, et al. Changes in inflammatory markers after sleeve gastrectomy in patients with impaired glucose homeostasis and type 2 diabetes. Surg Obes Relat Dis. 2014;10:1123–8.
Greer RL, Morgun A, Shulzhenko N. Bridging immunity and lipid metabolism by gut microbiota. J Allergy Clin Immunol. 2013;132:253–62.
Rodrigues RR, Greer RL, Dong X, et al. Antibiotic- induced alterations in gut microbiota are associated with changes in glucose metabolism in healthy mice. Front Microbiol. 2017;8:2306.
Winer DA, Winer S, Dranse HJ, et al. Immunologic impact of the intestine in metabolic disease. J Clin Invest. 2017;127:33–42.
Cani PD. Severe obesity and gut microbiota: does bariatric surgery really reset the system? Gut. 2019;68:5–6.
Bhutta HY, Deelman TE, le Roux CW, et al. Intestinal sweet-sensing pathways and metabolic changes after Roux-en-Y gastric bypass surgery. Am J Physiol Gastrointest Liver Physiol. 2014;307:G588–93.
Sumarac-Dumanovic M1, Stevanovic D, Ljubic A, et al. Increased activity of interleukin-23/interleukin-17 proinflammatory axis in obese women. Int J Obes. 2009;33(1):151–6.
Fatima N, Faisal SM, Zubair S, et al. Emerging role of interleukins IL-23/IL-17 axis and biochemical markers in the pathogenesis of type 2 diabetes: association with age and gender in human subjects. Int J Biol Macromol. 2017;105:1279–88.
Ip B, Cilfone NA, Belkina AC, et al. Th17 cytokines differentiate obesity from obesity-associated type 2 diabetes and promote TNFα production. Obesity. 2016;24:102–12.
DeFuria J, Belkina AC, Jagannathan-Bogdan M, et al. B cells promote inflammation in obesity and type 2 diabetes through regulation of T-cell function and an inflammatory cytokine profile. PNAS. 2013;110:5133–8.
Luck H, Tsai S, Chung J, et al. Regulation of obesity-related insulin resistance with gut anti-inflammatory agents. Cell Metab. 2015;21:527–42.
McLaughlin T, Ackerman SE, Shen L, et al. Role of innate and adaptive immunity in obesity-associated metabolic disease. J Clin Invest. 2017;127:5–13.
Ben-Zvi D, Meoli L, Abidi WM, et al. Time-dependent molecular responses differ between gastric bypass and dieting but are conserved across species. Cell Metab. 2018;28:1–14.
Acknowledgments
This study was supported by a Pilot and Feasibility Grant from the Boston Area Diabetes Endocrinology Research Center (P30 DK057521) and a KL2 Award from Harvard Catalyst (4KL2TR001100-04).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Table S1
(DOCX 56 kb)
Rights and permissions
About this article
Cite this article
Subramaniam, R., Aliakbarian, H., Bhutta, H.Y. et al. Sleeve Gastrectomy and Roux-en-Y Gastric Bypass Attenuate Pro-inflammatory Small Intestinal Cytokine Signatures. OBES SURG 29, 3824–3832 (2019). https://doi.org/10.1007/s11695-019-04059-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-04059-0