Abstract
Background
Gastroesophageal reflux disease (GERD) has been increasingly recognized in patients with morbid obesity. A recent global evidence-based consensus on GERD has been proposed, but its performance in patients with morbid obesity is unknown. The aim of this study was to assess the performance of the Montreal Consensus in the diagnosis of GERD in morbidly obese patients.
Methods
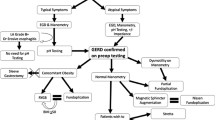
Seventy-five consecutive morbidly obese patients underwent GERD symptoms assessment, upper gastrointestinal endoscopy, and ambulatory esophageal pH monitoring “off PPI”. The performance of the Montreal Consensus was determined by comparing two diagnostic algorithms: 1. a gold standard approach in which any GERD symptom and findings from both endoscopy and pH monitoring were taken into account, and 2. the approach with the Montreal Consensus, in which troublesome GERD symptoms and endoscopic findings were considered.
Results
GERD was found present in 57 patients by applying the gold standard approach. The Montreal Consensus identified 41 of these patients, whereas the remaining 34 patients were classified as “no GERD”. Of these, 16 (47%) showed reflux esophagitis and/or abnormal pH-metry. The Montreal Consensus had an accuracy of 78.7%, sensitivity of 72% (95% CI 59–82%), specificity of 100% (95% CI 82–100%) and negative predictive value of 47% (95% CI 37–57%).
Conclusions
In morbidly obese patients, the approach with the Montreal Consensus has high specificity and suboptimal sensitivity in the diagnosis of GERD. Its intermediate negative predictive value suggests that complementary investigation might be routine in these patients, particularly in those who do not present with troublesome GERD symptoms.


Similar content being viewed by others
References
Bray GA, Bellanger T. Epidemiology, trends, and morbidities of obesity and the metabolic syndrome. Endocrine. 2006;29:109–17.
Dent J, El-Serag HB, Wallander MA, et al. Epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut. 2005;54:710–7.
Shaheen NJ, Hansen RA, Morgan DR, et al. The burden of gastrointestinal and liver diseases, 2006. Am J Gastroenterol. 2006;101:2128–38.
Sichieri R, Do NS, Coutinho W. The burden of hospitalization due to overweight and obesity in Brazil. Cad Saude Publica. 2007;23:1721–7.
Corley DA, Kubo A, Levin TR, et al. Abdominal obesity and body mass index as risk factors for Barrett’s esophagus. Gastroenterology. 2007;133:34–41.
El-Serag HB, Graham DY, Satia JA, et al. Obesity is an independent risk factor for GERD symptoms and erosive esophagitis. Am J Gastroenterol. 2005;100:1243–50.
El-Serag HB, Kvapil P, Hacken-Bitar J, et al. Abdominal obesity and the risk of Barrett’s esophagus. Am J Gastroenterol. 2005;100:2151–6.
Hampel H, Abraham NS, El-Serag HB. Meta-analysis: obesity and the risk for gastroesophageal reflux disease and its complications. Ann Intern Med. 2005;143:199–211.
Lagergren J, Bergstrom R, Lindgren A, et al. Symptomatic gastroesophageal reflux as a risk factor for esophageal adenocarcinoma. N Engl J Med. 1999;340:825–31.
Deitel M. Overweight and obesity worldwide now estimated to involve 1.7 billion people. Obes Surg. 2003;13:329–30.
Deitel M. The obesity epidemic. Obes Surg. 2006;16:377–8.
Cawley J, Prinz T, Beane S. Health insurance claims data as a means of assessing reduction in co-morbidities 6 months after bariatric surgery. Obes Surg. 2006;16:852–8.
Suter M, Dorta G, Giusti V, et al. Gastro-esophageal reflux and esophageal motility disorders in morbidly obese patients. Obes Surg. 2004;14:959–66.
Pandolfino JE, El-Serag HB, Zhang Q, et al. Obesity: a challenge to esophagogastric junction integrity. Gastroenterology. 2006;130:639–49.
Wu JC, Mui LM, Cheung CM, et al. Obesity is associated with increased transient lower esophageal sphincter relaxation. Gastroenterology. 2007;132:883–9.
Vakil N, van Zanten SV, Kahrilas P, et al. The Montreal definition and classification of gastroesophageal reflux disease: a global evidence-based consensus. Am J Gastroenterol. 2006;101:1900–20.
Fornari F, Gruber AC, Lopes AB, et al. Symptom’s questionnaire for gastroesophageal reflux disease. Arq Gastroenterol. 2004;41:263–7.
Velanovich V, Vallance SR, Gusz JR, et al. Quality of life scale for gastroesophageal reflux disease. J Am Coll Surg. 1996;183:217–24.
Hirano I, Richter JE. ACG practice guidelines: esophageal reflux testing. Am J Gastroenterol. 2007;102:668–85.
Jaffin BW, Knoepflmacher P, Greenstein R. High prevalence of asymptomatic esophageal motility disorders among morbidly obese patients. Obes Surg. 1999;9:390–5.
Ortiz V, Ponce M, Fernandez A, et al. Value of heartburn for diagnosing gastroesophageal reflux disease in severely obese patients. Obesity (Silver Spring). 2006;14:696–700.
Lundell LR, Dent J, Bennett JR, et al. Endoscopic assessment of oesophagitis: clinical and functional correlates and further validation of the Los Angeles classification. Gut. 1999;45:172–80.
Wo JM, Castell DO. Exclusion of meal periods from ambulatory 24-hour pH monitoring may improve diagnosis of esophageal acid reflux. Dig Dis Sci. 1994;39:1601–7.
Jamieson JR, Stein HJ, DeMeester TR, et al. Ambulatory 24-h esophageal pH monitoring: normal values, optimal thresholds, specificity, sensitivity, and reproducibility. Am J Gastroenterol. 1992;87:1102–11.
Wiener GJ, Richter JE, Copper JB, et al. The symptom index: a clinically important parameter of ambulatory 24-hour esophageal pH monitoring. Am J Gastroenterol. 1988;83:358–61.
Abramson JH. WINPEPI (PEPI-for-Windows): computer programs for epidemiologists. Epidemiol Perspect Innov. 2004;1:6.
Bray GA. Obesity: a time bomb to be defused. Lancet. 1998;352:160–1.
Adams KF, Schatzkin A, Harris TB, et al. Overweight, obesity, and mortality in a large prospective cohort of persons 50 to 71 years old. N Engl J Med. 2006;355:763–78.
Lagergren J, Bergstrom R, Nyren O. Association between body mass and adenocarcinoma of the esophagus and gastric cardia. Ann Intern Med. 1999;130:883–90.
Linn S, Grunau PD. New patient-oriented summary measure of net total gain in certainty for dichotomous diagnostic tests. Epidemiol Perspect Innov. 2006;3:11.
Lee YC, Lin JT, Chiu HM, et al. Intraobserver and interobserver consistency for grading esophagitis with narrow-band imaging. Gastrointest Endosc. 2007;66:230–6.
Johnson LF, DeMeester TR. Twenty-four-hour pH monitoring of the distal esophagus. A quantitative measure of gastroesophageal reflux. Am J Gastroenterol. 1974;62:325–32.
Aro P, Ronkainen J, Talley NJ, et al. Body mass index and chronic unexplained gastrointestinal symptoms: an adult endoscopic population based study. Gut. 2005;54:1377–83.
Edelstein ZR, Farrow DC, Bronner MP, et al. Central adiposity and risk of Barrett’s esophagus. Gastroenterology. 2007;133:403–11.
El-Serag HB, Ergun GA, Pandolfino J, et al. Obesity increases oesophageal acid exposure. Gut. 2007;56:749–55.
Corley DA, Kubo A, Zhao W. Abdominal obesity, ethnicity and gastro-oesophageal reflux symptoms. Gut. 2007;56:756–62.
Jansson C, Nordenstedt H, Johansson S, et al. Relation between gastroesophageal reflux symptoms and socioeconomic factors: a population-based study (the HUNT Study). Clin Gastroenterol Hepatol. 2007;5:1029–34.
Author information
Authors and Affiliations
Corresponding author
Additional information
Madalosso and Fornari contributed equally to the study.
Rights and permissions
About this article
Cite this article
Madalosso, C.A.S., Fornari, F., Callegari-Jacques, S.M. et al. Performance of the Montreal Consensus in the Diagnosis of Gastroesophageal Reflux Disease in Morbidly Obese Patients. OBES SURG 18, 668–674 (2008). https://doi.org/10.1007/s11695-008-9462-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-008-9462-6