Abstract
BACKGROUND
Non-verbal communication is an important aspect of the diagnostic and therapeutic process, especially with older patients. It is unknown how non-verbal communication varies with physician and patient race.
OBJECTIVE
To examine the joint influence of physician race and patient race on non-verbal communication displayed by primary care physicians during medical interviews with patients 65 years or older.
DESIGN, SETTING, AND PARTICIPANTS
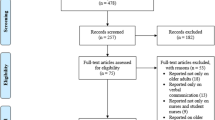
Video-recordings of visits of 209 patients 65 years old or older to 30 primary care physicians at three clinics located in the Midwest and Southwest.
MAIN MEASURES
Duration of physicians’ open body position, eye contact, smile, and non-task touch, coded using an adaption of the Nonverbal Communication in Doctor–Elderly Patient Transactions form.
KEY RESULTS
African American physicians with African American patients used more open body position, smile, and touch, compared to the average across other dyads (adjusted mean difference for open body position = 16.55, p < 0.001; smile = 2.35, p = 0.048; touch = 1.33, p < 0.001). African American physicians with white patients spent less time in open body position compared to the average across other dyads, but they also used more smile and eye gaze (adjusted mean difference for open body position = 27.25, p < 0.001; smile = 3.16, p = 0.005; eye gaze = 17.05, p < 0.001). There were no differences between white physicians’ behavior toward African American vs. white patients.
CONCLUSION
Race plays a role in physicians’ non-verbal communication with older patients. Its influence is best understood when physician race and patient race are considered jointly.
Similar content being viewed by others
References
Finset A. Nonverbal communication:–An important key to in-depth understanding of provider-patient interaction. Patient Educ Couns. 2007;66(2):127–8.
Beck RS, Daughtridge R, Sloane PD. Physician–patient communication in the primary care office: a systematic review. J Am Board Fam Pract. 2002;15(1):25–38.
DiMatteo MR, Taranta A, Friedman HS, Prince LM. Predicting patient satisfaction from physicians’ nonverbal communication skills. Med Care. 1980;18(4):376–87.
Harrigan JA, Oxman TE, Rosenthal R. Rapport expressed through nonverbal behavior. Journal of Nonverbal Behavior. 1985;9(2):95–110.
Lepper H, Martin L, DiMatteo M. A model of nonverbal exchange in physician–patient expectations for patient involvement. Journal of Nonverbal Behavior. 1995;19(4):207–22.
Mast MS. On the importance of nonverbal communication in the physician–patient interaction. Patient Educ Couns. 2007;67(3):315–8.
Duggan P, Parrott L. Physicians’ nonverbal rapport building and patients’ talk about the subjective component of illness. Hum Commun Res. 2001;27(2):299–311.
Ambady N, Laplante D, Nguyen T, Rosenthal R, Chaumeton N, Levinson W. Surgeons’ tone of voice: a clue to malpractice history. Surgery. 2002;132(1):5–9.
Griffith CH 3rd, Wilson JF, Langer S, Haist SA. House staff nonverbal communication skills and standardized patient satisfaction. J Gen Intern Med. 2003;18(3):170–4.
Harrigan JA, Rosenthal R. Physicians’ head and body positions as determinants of perceived rapport. J Appl Soc Psychol. 1983;13(6):496–509.
Irish JT. Deciphering the physician-older patient interaction. Int J Psychiatry Med. 1997;27(3):251–67.
Caris-Verhallen WM, Kerkstra A, Bensing JM. Non-verbal behaviour in nurse-elderly patient communication. J Adv Nurs. 1999;29(4):808–18.
Gorawara-Bhat R, Cook MA, Sachs GA. Nonverbal communication in doctor-elderly patient transactions (NDEPT): development of a tool. Patient Educ Couns. 2007;66(2):223–34.
Barnett S. Communication with deaf and hard-of-hearing people: a guide for medical education. Acad Med. 2002;77:694–700.
Adelman RD, Greene MG, Ory MG. Communication between older patients and their physicians. Clin Geriatr Med. 2000;16(1):1–24. vii.
Street RL, Buller DB. Patients’ characteristics affecting physician–patient nonverbal communication. Hum Commun Res. 1988;15(1):60–90.
Dovidio JF, Kawakami K, Gaertner SL. Implicit and explicit prejudice and interracial interaction. J Pers Soc Psychol. 2002;82(1):62–8.
Fazio RH, Jackson JR, Dunton BC, Williams CJ. Variability in automatic activation as an unobtrusive measure of racial attitudes: a bona fide pipeline? J Pers Soc Psychol. 1995;69(6):1013–27.
Greenwald AG, McGhee DE, Schwartz JL. Measuring individual differences in implicit cognition: the implicit association test. J Pers Soc Psychol. 1998;74(6):1464–80.
Dovidio JF, Penner LA, Albrecht TL, Norton WE, Gaertner SL, Shelton JN. Disparities and distrust: the implications of psychological processes for understanding racial disparities in health and health care. Soc Sci Med. 2008;67(3):478–86.
Burgess D, van Ryn M, Dovidio J, Saha S. Reducing racial bias among health care providers: lessons from social-cognitive psychology. J Gen Intern Med. 2007;22(6):882–7.
Green A, Carney D, Pallin D, et al. Implicit bias among physicians and its prediction of thrombolysis decisions for black and white patients. J Gen Intern Med. 2007;22(9):1231–8.
Johnson RL, Roter D, Powe NR, Cooper LA. Patient race/ethnicity and quality of patient–physician communication during medical visits. Am J Public Health. 2004;94(12):2084–90.
Cooper-Patrick L, Gallo JJ, Gonzales JJ, et al. Race, gender, and partnership in the patient–physician relationship. JAMA. 1999;282(6):583–9.
Saha S, Komaromy M, Koepsell TD, Bindman AB. Patient–physician racial concordance and the perceived quality and use of health care. Arch Intern Med. 1999;159(9):997–1004.
LaVeist TA, Carroll T. Race of physician and satisfaction with care among African-American patients. J Natl Med Assoc. 2002;94(11):937–43.
LaVeist TA, Nuru-Jeter A. Is doctor-patient race concordance associated with greater satisfaction with care? J Health Soc Behav. 2002;43(3):296–306.
Sohler NL, Fitzpatrick LK, Lindsay RG, Anastos K, Cunningham CO. Does patient-provider racial/ethnic concordance influence ratings of trust in people with HIV infection? AIDS Behav. 2007;11(6):884–96.
Gamble VN. Under the shadow of Tuskegee: African Americans and health care. Am J Public Health. 1997;87(11):1773–8.
Ridgeway C. The social construction of status value: gender and other nominal characteristics. Soc Forces. 1991;70(2):367–86.
Nunez-Smith M, Curry LA, Bigby J, Berg D, Krumholz HM, Bradley EH. Impact of race on the professional lives of physicians of African descent. Ann Intern Med. 2007;146(1):45–51.
Coombs AA, King RK. Workplace discrimination: experiences of practicing physicians. J Natl Med Assoc. 2005;97(4):467–77.
West C. When the doctor is a "lady": power status and gender in physician–patient encounters. Symbolic Interaction. 1984;7:87–106.
Stepanikova I. Patient–physician racial and ethnic concordance and perceived medical errors. Soc Sci Med. 2006;63(12):3060–6.
Hall JA, Irish JT, Roter DL, Ehrlich CM, Miller LH. Gender in medical encounters: an analysis of physician and patient communication in a primary care setting. Health Psychol. 1994;13(5):384–92.
Larsen KM, Smith CK. Assessment of nonverbal communication in the patient–physician interview. J Fam Pract. 1981;12(3):481–8.
Weinberger M, Greene JY, Mamlin JJ. The impact of clinical encounter events on patient and physician satisfaction. Soc Sci Med E. 1981;15(3):239–44.
Smith-Hanen SS. Effects of nonverbal behaviors on judged levels of counselor warmth and empathy. J Couns Psychol. 1977;24(2):87–91.
Andersen PA, Guerrero LK, Buller DB, Jorgensen PF. An empirical comparison of three theories of nonverbal immediacy exchange. Hum Commun Res. 1998;24(4):501–35.
Ruusuvuori J. Looking means listening: coordinating displays of engagement in doctor-patient interaction. Soc Sci Med. 2001;52(7):1093–1108.
Ambady N, Koo J, Rosenthal R, Winograd CH. Physical therapists’ nonverbal communication predicts geriatric patients’ health outcomes. Psychol Aging. 2002;17(3):443–52.
Bensing J. Doctor-patient communication and the quality of care. Soc Sci Med. 1991;32(11):1301–10.
Ishikawa H, Hashimoto H, Kinoshita M, Fujimori S, Shimizu T, Yano E. Evaluating medical students’ non-verbal communication during the objective structured clinical examination. Med Educ. 2006;40(12):1180–7.
Bensing J, Kerssens J, Pasch M. Patient-directed gaze as a tool for discovering and handling psychosocial problems in general practice. Journal of Nonverbal Behavior. 1995;19(4):223–42.
Bruhn JG. The doctor’s touch: tactile communication in the doctor-patient relationship. South Med J. 1978;71(12):1469–73.
Cook MA. Final Report: Assessment of Doctor-Elderly Patient Encounters, grant no. R44 AG5737-S2 Washington, DC: National Institute on Aging 2002.
Tai-Seale M, Bramson R, Drukker D, et al. Understanding primary care physicians’ propensity to assess elderly patients for depression using interaction and survey data. Med Care. 2005;43(12):1217–24.
Tai-Seale M, McGuire TG, Zhang W. Time allocation in primary care office visits. Health Serv Res. 2007;42(5):1871–94.
Tai-Seale T, Tai-Seale M, Zhang W. Weight counseling for elderly patients in primary care: how often and how much time. J Health Hum Serv Adm. Spring. 2008;30(4):420–40.
Teresi JA, Ramirez M, Ocepek-Welikson K, Cook MA. The development and psychometric analyses of ADEPT: an instrument for assessing the interactions between doctors and their elderly patients. Ann Behav Med. 2005;30(3):225–42.
Ambady N, Bernier FJ, Richeson JA. Toward a histology of social behavior: judgmental accuracy from thin slices of the behavioral stream. In: Zanna MP, ed. Advances in experimental social psychology, vol.32. San Diego, CA: Academic Press, 2000:201–71.
Murphy N. Using thin slices for behavioral coding. Journal of Nonverbal Behavior. 2005;29(4):235–46.
Bartko JJ. Measures of agreement: a single procedure. Stat Med. 1994;13(5–7):737–45.
Rabe-Hesketh S, Skrondal A, Pickles A. Generalized multilevel structural equation modeling. Psychometrika. 2004;69(2):167–190.
Adelman RD, Greene MG, Charon R. The physician-elderly patient-companion triad in the medical encounter: the development of a conceptual framework and research agenda. Gerontologist. 1987;27(6):729–34.
Ishikawa H, Roter DL, Yamazaki Y, Takayama T. Physician-elderly patient-companion communication and roles of companions in Japanese geriatric encounters. Soc Sci Med. 2005;60(10):2307–20.
Malat J, Purcell D, van Ryn M. Factors affecting whites' and blacks' attitudes toward race concordance with doctors. J Natl Med Assoc. Sep;102(9):787–793.
Malat J, van Ryn M. African-American preference for same-race healthcare providers: the role of healthcare discrimination. Ethn Dis. Autumn. 2005;15(4):740–7.
Malat J, van Ryn M, Purcell D. Blacks’ and whites’ attitudes toward race and nativity concordance with doctors. J Natl Med Assoc. 2009;101(8):800–7.
Cashdan E. Smiles, speech, and body posture: how women and men display sociometric status and power. Journal of Nonverbal Behavior. 1998;22(4):209–228.
van Wieringen JC, Harmsen JA, Bruijnzeels MA. Intercultural communication in general practice. Eur J Public Health. 2002;12(1):63–8.
Contributors
None.
Funders
This study was supported by University of South Carolina Research Opportunity Program, “Racial and Ethnic Disparities in Non-Verbal Communication Between Physicians and Elderly Patients: A Pilot Study." ($47,557)
Prior presentations
None.
Conflict of Interest
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Stepanikova, I., Zhang, Q., Wieland, D. et al. Non-Verbal Communication Between Primary Care Physicians and Older Patients: How Does Race Matter?. J GEN INTERN MED 27, 576–581 (2012). https://doi.org/10.1007/s11606-011-1934-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-011-1934-z