Abstract
Introduction
Repeat hepatectomy (RH) is considered a valuable option for management of recurrent colorectal liver metastases (R-CLM). Here, the outcome of RH for R-CLM was compared to that of patients who underwent single hepatectomy (SH) after subdividing the later according to re-recurrence status.
Methods
Between 2001 and 2013, patients who received hepatectomy for CLM and R-CLM were included in study. Patients with non-resectable R-CLM were excluded.
Results
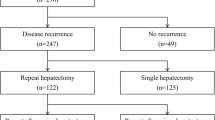
One hundred sixteen patients were included: 86 patients in SH group and 30 patients in RH group. Repeat hepatectomy group had more synchronous CLM (76.7 versus 50 %, p = 0.011). From the 86 patients who underwent SH, 69 patients did not have R-CLM. Survival analysis was done from the time of first hepatectomy for the no R-CLM group and the time of RH for the RH group. The 3- and 5-year survival rates for the no R-CLM group were 66.4 and 48.8%, respectively, and for the RH group were 56 and 44.8% respectively (p = 0.841). Multivariate analysis showed that larger size of R-CLM is an independent risk factor for survival after RH.
Conclusion
Repeat hepatectomy for R-CLM shows a comparable OS to non-recurrent CLM after single hepatectomy, despite the RH group had higher incidence of synchronous CLM.


Similar content being viewed by others
Abbreviations
- CLM:
-
Colorectal liver metastases
- RH:
-
Repeat hepatectomy
- R-CLM:
-
Recurrent colorectal liver metastasis
- SH:
-
Single hepatectomy
- RFA:
-
Radiofrequency ablation
- CEUS:
-
Contrast enhanced ultrasonography
- CT:
-
Computed tomography
- MRI:
-
Magnetic resonance imaging
- CEA:
-
Carcino-embryonic antigen
- OS:
-
Overall survival
- PFS:
-
Progression-free survival
References
Fong Y, Fortner J, Sun RL, Brennan MF and Blumgart LH. Clinical score for predicting recurrence after hepatic resection for metastatic colorectal cancer: analysis of 1001 consecutive cases. Ann Surg 1999; 230:309–318.
Abdalla EK, Vauthey JN, Ellis LM, et al. Recurrence and outcomes following hepatic resection, radiofrequency ablation, and combined resection/ablation for colorectal liver metastases. Ann Surg 2004; 239:818–825.
Scheele J, Stang R, Altendorf-Hofmann A, Paul M. Resection of colorectal liver metastases. World J Surg 1995; 19:59 –71.
Wei AC, Greig PD, Grant D, Taylor B, Langer B, Gallinger S. Survival after hepatic resection for colorectal metastases: A 10-year experience. Ann Surg Oncol, 2006; 13:668–676.
Sa Cunha A, Laurent C, Rault A, Couderc P, Rullier E, Saric J. A second liver resection due to recurrent colorectal liver metastases. Arch Surg 2007; 142:1144–1149.
Suzuki S, Sakaguchi T, Yokoi Y, et al. Impact of repeat hepatectomy on recurrent colorectal liver metastases. Surgery 2001; 129:421–428.
Adam R, Bismuth H, Castaing D, et al. Repeat hepatectomy for colorectal liver metastases. Ann Surg 1997; 225:51–60.
Nishio H, Hamady ZZ, Malik HZ, Fenwick S, Rajendra Prasad K, Toogood GJ, Lodge JP. Outcome following repeat liver resection for colorectal liver metastases. Eur J Surg Oncol 2007; 33:729–734.
Neeff HP, Drognitz O, Holzner P, Klock A, Bronsert P, Hopt UT, Makowiec F. Outcome after repeat resection of liver metastases from colorectal cancer. Int J Colorectal Dis 2013; 28:1135–1141.
Shaw IM, Rees M, Welsh FK, Bygrave S, John TG. Repeat hepatic resection for recurrent colorectal liver metastases is associated with favourable long-term survival. Br J Surg 2006; 93:457–464.
Wicherts DA, de Haas RJ, Salloum C, et al. Repeat hepatectomy for recurrent colorectal metastases. Br J Surg 2013; 100:808–818.
De Carlis L., Di Sandro S., Giacomoni A, et al. Colorectal liver metastases: Hepatic pedicle clamping during hepatectomy reduces the incidence of tumor recurrence in selected patients. Case-matched analysis. Eur J Surg Oncol 2013; 39:726–733.
D’Angelica M, Brennan MF, Fortner JG, Cohen AM, Blumgart LH, Fong Y. Ninety-six five year survivors after liver resection for metastatic colorectal cancer. J Am Coll Surg 1997; 185:554–559.
Choti MA, Sitzmann JV, Tiburi MF, et al. Trends in long-term survival following liver resection for hepatic colorectal metastases. Ann Surg 2002; 235:759–766.
Jonsson K, Grondahl G, Salo M, Tingstedt B, Andersson R. Repeated Liver Resection for Colorectal Liver Metastases: a Comparison with Primary Liver Resections concerning Perioperative and Long-Term Outcome. Gastroenterol Res Pract 2012; 2012:568214.
Takahashi S, Inoue K, Konishi M, Nakagouri T, Kinoshita T. Prognostic factors for poor survival after repeat hepatectomy in patients with colorectal liver metastases. Surgery 2003; 133:627–634.
Luo LX, Yu ZY, Huang JW, Wu H. Selecting patients for a second hepatectomy for colorectal metastases: An systemic review and meta-analysis. Eur J Surg Oncol 2014; 40:1036–1048.
Tsai MS, Su YH, Ho MC, Liang JT, Chen TP, Lai HS, Lee PH. Clinicopathological features and prognosis in resectable synchronous and Metachronous colorectal liver metastasis. Ann Surg Oncol 2007; 14:786–794.
Ghiringhelli F, Hennequin A, Drouillard A, Lepage C, Faivre J, Bouvier AM. Epidemiology and prognosis of synchronous and metachronous colon cancer metastasis: a French population-based study. Dig Liver Dis 2014; 46: 854–858.
Adam R, De Gramont A, Figueras J, et al. The oncosurgery approach to managing liver metastases from colorectal cancer: a multidisciplinary international consensus. The Oncologist 2012; 17:1225–1239.
Clavien PA, Petrowsky H, DeOliveira ML, Graf R. Strategies for safer liver surgery and partial liver transplantation. N Engl J Med 2007; 356:1545–1559.
Misiakos EP, Karidis NP, Kouraklis G. Current treatment for colorectal liver metastases. World J Gastroenterol 2011; 17:4067– 4075.
Charnsangavej C, Clary B, Fong Y, Grothey A, Pawlik TM, Choti MA. Selection of patients for resection of hepatic colorectal metastases: expert consensus statement. Ann Surg Oncol 2006; 13:1261–1268.
Pessaux P, Lermite E, Brehant O, Tuech JJ, Lorimier G, Arnaud JP. Repeat hepatectomy for recurrent colorectal liver metastases. J Surg Oncol 2006; 93:1–7.
Petrowsky H, Gonen M, JarnaginW, et al. Second liver resections are safe and effective treatment for recurrent hepatic metastases from colorectal cancer: a bi-institutional analysis. Ann Surg 2002; 235:863–871.
de Jong MC, Pulitano C, Ribero D, et al. Rates and patterns of recurrence following curative intent surgery for colorectal liver metastasis: an international multi-institutional analysis of 1669 patients. Ann Surg 2009; 250:440–448.
Kokudo N., Miki Y, Sugai S, et al. Genetic and histological assessment of surgical margins in resected liver metastases from colorectal carcinoma: minimum surgical margins for successful resection. Arch Surg 2002; 137:833–840.
Lalmahomed ZS, Ayez N, van der Pool AE, Verheij J, IJzermans JN, Verhoef C. Anatomical versus nonanatomical resection of colorectal liver metastases: is there a difference in surgical and oncological outcome? World J Surg 2011; 35:656–661.
Gold JS, Are C, Kornprat P, et al. Increased use of parenchymal-sparing surgery for bilateral liver metastases from colorectal cancer is associated with improved mortality without change in oncologic outcome: trends in treatment over time in 440 patients. Ann Surg 2008; 247:109–117
Kokudo N, Tada K, Seki M et al. Anatomical major resection versus nonanatomical limited resection for liver metastases from colorectal carcinoma. Am J Surg 2001; 181:153–159.
Conflict of interest
No conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ali, M.A., Di Sandro, S., Lauterio, A. et al. Repeat Hepatectomy for Recurrent Colorectal Liver Metastases: Is it Worth the Challenge?. J Gastrointest Surg 19, 2192–2198 (2015). https://doi.org/10.1007/s11605-015-2939-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-015-2939-4