Abstract
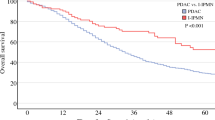
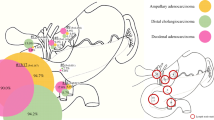
Intraductal papillary mucinous neoplasms (IPMNs) show varying degrees of dysplasia throughout the neoplasm that can range from adenoma to invasive carcinoma, with dysplastic changes of borderline neoplasms and carcinoma in situ in between. An understanding of the natural history, and especially the required time to transform into either carcinoma in situ or an invasive adenocarcinoma, is critically important for management policy. This topic serves as the rationale for the present analysis. At the beginning of February 2007, using the key word “IPMN” in PubMed, we initially selected 119 publications using the principal criteria as defined by the WHO classification. We identified 20 appropriate original reports and one consensus paper. Neither randomized control trials (RCT) or systematic reviews of RCTs (level 1 evidence) nor cohort studies or reviews of cohort studies (level 2 evidence) have been published. Only one report fit the criteria for level 3 evidence (case control study). Nineteen papers satisfied criteria for level 4 (cases series) and two for level 5 (expert opinion publication). After additional review and analysis, we considered only six reports to be “cornerstone papers” of merit for the final review. Clues to the natural history of IPMNs can be gained by using several methods to examine the articles: (a) to verify different prognoses between main and side branch duct subtypes; (b) to compare the average age of patients with benign vs. malignant IPMNs; (c) to summarize the findings of nonoperative, observational studies based on follow up by clinical, biochemical, and imaging techniques without operative resection; (d) to determine the prognostic importance of the status of the resection margin; and (e) to follow patients clinically after surgical resection. Although important aspects of the natural history of IPMN are still unknown, the following conclusions can be drawn: (1) Branch-duct IPMNs are less aggressive than main-duct IPMNs. (2) Malignancy is more common in older patients. (3) Malignancy (invasive or carcinoma in situ) is found in about 70% of resected main-duct IPMNs. (4) After resection of noninvasive IPMNs (branch- and main-duct varieties), recurrence is rare (<8%). (5) After resection of invasive IPMN, recurrence occurs in 50–65% of patients.
Similar content being viewed by others
References
Ohashi K, Murakami Y, Takekoshi T, et al. Four cases of ‘mucin-producing’ cancer of the pancreas on specific findings of the papilla of Vater. Prog Dig Endosc 1982;20:348–351.
Carbognin G, Zamboni G, Pinali L, et al. Branch duct IPMTs: Value of cross-sectional imaging in the assessment of biological behavior and follow-up. Abdom Imaging 2006;31:320–325.
Sperti C, Pasquali C, Decet G, et al. F-18-fluorodeoxyglucose positron emission tomography in differentiating malignant from benign pancreatic cysts: A prospective study. J Gastrointest Surg 2005;9:22–28.
Kloppel G, Solcia E, Longnecker DS, et al. Histologic typing of tumors of the exocrine pancreas. In: World Health Organization ed. International Classification of Tumors, 2nd ed. Berlin: Springer, 1996, pp 11–20.
Wada K, Takada T, Yasuda H, et al. Does “clonal progression” relate to the development of intraductal papillary mucinous tumors of the pancreas? J Gastrointest Surg 2004;8:289–296.
Sahani DV, Kadavigere R, Blake M, et al. Intraductal papillary mucinous neoplasm of pancreas: Multi-detector row CT with 2D curved reformations—Correlation with MRCP. Radiology 2006;238:560–569.
Sauvanet A, Partensky C, Sastre B, et al. Medial pancreatectomy: A multi-institutional retrospective study of 53 patients by the French Pancreas Club. Surgery 2002;132:836–843.
Couvelard A, Sauvanet A, Kianmanesh R, et al. Frozen sectioning of the pancreatic cut surface during resection of intraductal papillary mucinous neoplasms of the pancreas is useful and reliable. A prospective evaluation. Ann Surg 2005;242:774–780.
Eguchi H, Ishikawa O, Ohigashi H, et al. Role of intraoperative cytology combined with histology in detecting continuous and skip type intraductal cancer existence for intraductal papillary mucinous carcinoma of the pancreas. Cancer 2006;107:2567–2575.
Rodriguez JR, Salvia R, Crippa S, et al. Branch-duct intraductal papillary mucinous neoplasms: Observations in 145 patients who underwent resection. Gastroenterology 2007;133:72–79.
D’Angelica M, Brennan MF, Suriawinata AA, et al. Intraductal papillary mucinous neoplasms of the pancreas. Ann Surg 2004;239:400–408.
Bernard P, Scoazec JY, Joubert M, et al. Intraductal papillary–mucinous tumors of the pancreas: Predictive criteria of malignancy according to pathological examination of 53 cases. Arch Surg 2002;137:1274–1278.
Chari ST, Yadav D, Smyrk TC, et al. Study of recurrence after surgical resection of intraductal papillary mucinous neoplasm of the pancreas. Gastroenterology 2002;123:1500–1507.
Wada K, Kozarek RA, Traverso LW. Outcomes following resection of invasive and noninvasive intraductal papillary mucinous neoplasms of the pancreas. Am J Surg 2005;189:632–636.
Raut CP, Cleary KR, Staerkel GA, et al. Intraductal papillary mucinous neoplasms of the pancreas: Effect of invasion and pancreatic margin status on recurrence and survival. Ann Surg Oncol 2006;13:582–594.
Yamao K, Ohashi K, Nakamura T, et al. The prognosis of intraductal papillary mucinous tumors of the pancreas. Hepatogastroenterology 2000;47:1129–1134.
Sohn TA, Yeo CJ, Cameron JL, et al. Intraductal papillary mucinous neoplasms of the pancreas: An updated experience. Ann Surg 2004;239:788–797.
Sugiyama M, Atomi Y. Intraductal papillary mucinous tumors of the pancreas: Imaging studies and treatment strategies. Ann Surg 1998;228:685–691.
Mattsumoto T, Aramaki M, Yada K, et al. Optimal management of the branch duct type intraductal papillary mucinous neoplasms of the pancreas. J Clin Gastroenterol 2003;36:261–265.
Falconi M, Salvia R, Bassi C, et al. Clinicopathological features and treatment of intraductal papillary mucinous tumour of the pancreas. Br J Surg 2001;88:376–381.
Kawai M, Uchiyama K, Tani M, et al. Clinicopathological features of malignant intraductal papillary mucinous tumors of the pancreas: The differential diagnosis from benign entities. Arch Surg 2004;139:188–192.
Zamora C, Sahel J, Cantu DG, et al. Intraductal papillary or mucinous tumors (IPMT) of the pancreas: Report of a case series and review of the literature. Am J Gastroenterol 2001;96:1441–1447.
Paye F, Sauvanet A, Terris B, et al. Intraductal papillary mucinous tumors of the pancreas: Pancreatic resections guided by preoperative morphological assessment and intraoperative frozen section examination. Surgery 2000;127:536–544.
Salvia R, Fernandez-del Castillo C, Bassi C, et al. Main-duct intraductal papillary mucinous neoplasms of the pancreas: Clinical predictors of malignancy and long-term survival following resection. Ann Surg 2004;239:678–687.
Suzuki Y, Atomi Y, Sugiyama M, et al. Cystic neoplasm of the pancreas: A Japanese multiinstitutional study of intraductal papillary mucinous tumor and mucinous cystic tumor. Pancreas 2004;28:241–246.
Obara T, Maguchi H, Saitoh Y, et al. Mucin-producing tumor of the pancreas: A unique clinical entity. Am J Gastroenterol 1991;86:1619–1625.
Yamaguchi K, Sugitani A, Chijiiwa K, et al. Intraductal papillary–mucinous tumor of the pancreas: Assessing the grade of malignancy from natural history. Am Surg 2001;67:400–406.
Levy P, Jouannaud V, O’Toole D, et al. Natural history of intraductal papillary mucinous tumors of the pancreas: Actuarial risk of malignancy. Clin Gastroenterol Hepatol 2006;4:460–468.
Traverso LW, Peralta EA, Ryan JA Jr, et al. Intraductal neoplasms of the pancreas. Am J Surg 1998;175:426–432.
Sho M, Nakajima Y, Kanehiro H, et al. Pattern of recurrence after resection for intraductal papillary mucinous tumors of the pancreas. World J Surg 1998;22:874–878.
Kobari M, Egawa S, Shibuya K, et al. Intraductal papillary mucinous tumors of the pancreas comprise 2 clinical subtypes: Differences in clinical characteristics and surgical management. Arch Surg 1999;134:1131–1136.
Salvia R, Crippa S, Falconi M, et al. Branch-duct intraductal papillary mucinous neoplasms of the pancreas: To operate or not to operate? Gut 2007,56:1086–1090.
Jang JY, Kim SW, Ahn YJ, et al. Multicenter analysis of clinicopathologic features of intraductal papillary mucinous tumor of the pancreas: Is it possible to predict the malignancy before surgery? Ann Surg Oncol 2005;12:124–132.
Terris B, Ponsot P, Paye F, et al. Intraductal papillary mucinous tumors of the pancreas confined to secondary ducts show less aggressive pathologic features as compared with those involving the main pancreatic duct. Am J Surg Pathol 2000;24:1372–1377.
Tanaka M, Chari S, Adsay V, et al. International consensus guidelines for management of intraductal papillary mucinous neoplasms and mucinous cystic neoplasms of the pancreas. Pancreatology 2005;6:17–32.
Sarr MG, Murr M, Smyrk TC, Yeo CJ, Fernadez-del Castillo C, Hawes RH, Freeny PC. Primary cystic neoplasms of the pancreas: Neoplastic disorders of emerging importance—current state-of-the-art and unanswered questions. J Gastrointest Surg 2003;7:417–428.
Wakabayashi T, Kawaura Y, Morimoto H, et al. Clinical management of intraductal papillary mucinous tumors of the pancreas based on imaging findings. Pancreas 2001;22:370–377.
Irie H, Yoshimitsu K, Aibe H, et al. Natural history of pancreatic intraductal papillary mucinous tumor of branch duct type: Follow-up study by magnetic resonance cholangiopancreatography. J Comput Assist Tomogr 2004;28:117–122.
Acknowledgments
Thanks to Roberto Salvia M.D. Ph.D. for the daily job carried out on the “Verona pancreatic cystic data base” and the outstanding collaboration with the MGH he started and that now still runs thanks to Stefano Crippa M.D. Thanks to Andrew Warshaw; Carlos Fernandez De Castillo; and, for the active discussion and precious suggestions in the preparation of the present manuscript, William Traverso. Thanks to the whole “Pancreatic Interdisciplinary Team” of the Verona Centre and to their boss, Prof. Paolo Pederzoli.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bassi, C., Sarr, M.G., Lillemoe, K.D. et al. Natural History of Intraductal Papillary Mucinous Neoplasms (IPMN): Current Evidence and Implications for Management. J Gastrointest Surg 12, 645–650 (2008). https://doi.org/10.1007/s11605-007-0447-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-007-0447-x