Abstract
Purpose
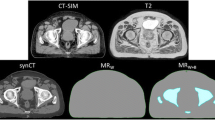
MR-guided radiotherapy (MRgRT) relies on the daily assignment of a relative electron density (RED) map to allow the fraction specific dose calculation. One approach to assign the RED map consists of segmenting the daily magnetic resonance image into five different density levels and assigning a RED bulk value to each level to generate a synthetic CT (sCT). The aim of this study is to evaluate the dose calculation accuracy of this approach for applications in MRgRT.
Methods
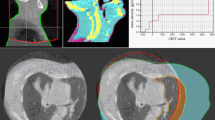
A planning CT (pCT) was acquired for 26 patients with abdominal and pelvic lesions and segmented in five levels similar to an online approach: air, lung, fat, soft tissue and bone. For each patient, the median RED value was calculated for fat, soft tissue and bone. Two sCTs were generated assigning different bulk values to the segmented levels on pCT: The sCTICRU uses the RED values recommended by ICRU46, and the sCTtailor uses the median patient-specific RED values. The same treatment plan was calculated on two the sCTs and the pCT. The dose calculation accuracy was investigated in terms of gamma analysis and dose volume histogram parameters.
Results
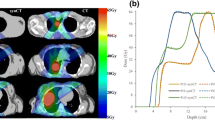
Good agreement was found between dose calculated on sCTs and pCT (gamma passing rate 1%/1 mm equal to 91.2% ± 6.9% for sCTICRU and 93.7% ± 5.3% b or sCTtailor). The mean difference in estimating V95 (PTV) was equal to 0.2% using sCTtailor and 1.2% using sCTICRU, respect to pCT values
Conclusions
The bulk sCT guarantees a high level of dose calculation accuracy also in presence of magnetic field, making this approach suitable to MRgRT. This accuracy can be improved by using patient-specific RED values.






Similar content being viewed by others
Abbreviations
- ART:
-
Adaptive radiotherapy
- BMI:
-
Body mass index
- CT:
-
Computed tomography
- DVH:
-
Dose volume histogram
- GPU:
-
Graphical processing unit
- HU:
-
Hounsfield unit
- IMRT:
-
Intensity modulated radiation therapy
- MRI:
-
Magnetic resonance imaging
- MR:
-
Magnetic resonance
- MRgRT:
-
MR-guided radiotherapy
- OARs:
-
Organs at risk
- sCTtailor:
-
pCT uses the median patient-specific RED values
- sCTICRU:
-
pCT uses the RED values recommended by ICRU46
- pCT:
-
Planning CT
- PTV:
-
Planning target volume
- RT:
-
Radiation treatment
- RED:
-
Relative electron density
- sCT:
-
Synthetic CT
- WMW:
-
Wilcoxon–Mann–Whitney
References
Yan D, Vicini F, Wong J, Martinez A (1997) Adaptive radiation therapy. Phys Med Biol 42:123–132
Lim-Reinders S, Keller BM, Al-Ward S et al (2017) Online adaptive radiation therapy. Int J Radiat Oncol Biol Phys 99:994–1003. https://doi.org/10.1016/j.ijrobp.2017.04.023
Bohoudi O, Bruynzeel AME, Senan S et al (2017) Fast and robust online adaptive planning in stereotactic MR-guided adaptive radiation therapy (SMART) for pancreatic cancer. Radiother Oncol 125:439–444. https://doi.org/10.1016/j.radonc.2017.07.028
Acharya S, Fischer-Valuck BW, Kashani R et al (2016) Online magnetic resonance image guided adaptive radiation therapy: first clinical applications. Int J Radiat Oncol Biol Phys 94:394–403. https://doi.org/10.1016/j.ijrobp.2015.10.015
Mutic S, Dempsey JF (2014) The ViewRay system: magnetic resonance-guided and controlled radiotherapy. Semin Radiat Oncol 24:196–199. https://doi.org/10.1016/j.semradonc.2014.02.008
Lagendijk JJW, Raaymakers BW, van Vulpen M (2014) The magnetic resonance imaging-linac system. Semin Radiat Oncol 24:207–209. https://doi.org/10.1016/j.semradonc.2014.02.009
van der Heide UA (2016) MR-guided radiation therapy. Phys Med 32:175. https://doi.org/10.1016/j.ejmp.2016.07.284
Edmund JM, Nyholm T (2017) A review of substitute CT generation for MRI-only radiation therapy. Radiat Oncol 12:28. https://doi.org/10.1186/s13014-016-0747-y
Raaijmakers AJE, Raaymakers BW, Lagendijk JJW (2005) Integrating a MRI scanner with a 6 MV radiotherapy accelerator: dose increase at tissue-air interfaces in a lateral magnetic field due to returning electrons. Phys Med Biol 50:1363–1376. https://doi.org/10.1088/0031-9155/50/7/002
Raaijmakers AJE, Raaymakers BW, van der Meer S, Lagendijk JJW (2007) Integrating a MRI scanner with a 6 MV radiotherapy accelerator: impact of the surface orientation on the entrance and exit dose due to the transverse magnetic field. Phys Med Biol 52:929–939. https://doi.org/10.1088/0031-9155/52/4/005
Raaijmakers AJE, Raaymakers BW, Lagendijk JJW (2007) Experimental verification of magnetic field dose effects for the MRI-accelerator. Phys Med Biol 52:4283–4291. https://doi.org/10.1088/0031-9155/52/14/017
Cusumano D, Teodoli S, Greco F et al (2018) Experimental evaluation of the impact of low tesla transverse magnetic field on dose distribution in presence of tissue interfaces. Phys Med 53:80–85. https://doi.org/10.1016/j.ejmp.2018.08.007
Kraus KM, Jäkel O, Niebuhr NI, Pfaffenberger A (2017) Generation of synthetic CT data using patient specific daily MR image data and image registration. Phys Med Biol 62:1358–1377. https://doi.org/10.1088/1361-6560/aa5200
Paradis E, Cao Y, Lawrence TS et al (2015) Assessing the dosimetric accuracy of magnetic resonance-generated synthetic CT images for focal brain VMAT radiation therapy. Int J Radiat Oncol Biol Phys 93:1154–1161. https://doi.org/10.1016/j.ijrobp.2015.08.049
Wachowicz K, De Zanche N, Yip E et al (2016) CNR considerations for rapid real-time MRI tumor tracking in radiotherapy hybrid devices: effects of B0 field strength. Med Phys 43:4903. https://doi.org/10.1118/1.4959542
Kim J, Garbarino K, Schultz L et al (2015) Dosimetric evaluation of synthetic CT relative to bulk density assignment-based magnetic resonance-only approaches for prostate radiotherapy. Radiat Oncol 10:239. https://doi.org/10.1186/s13014-015-0549-7
Lambert J, Greer PB, Menk F et al (2011) MRI-guided prostate radiation therapy planning: Investigation of dosimetric accuracy of MRI-based dose planning. Radiother Oncol 98:330–334. https://doi.org/10.1016/j.radonc.2011.01.012
Wang H, Chandarana H, Block KT et al (2017) Dosimetric evaluation of synthetic CT for magnetic resonance-only based radiotherapy planning of lung cancer. Radiat Oncol 12:108. https://doi.org/10.1186/s13014-017-0845-5
Jonsson JH, Karlsson MG, Karlsson M, Nyholm T (2010) Treatment planning using MRI data: an analysis of the dose calculation accuracy for different treatment regions. Radiat Oncol 5:62. https://doi.org/10.1186/1748-717X-5-62
Prior P, Chen X, Botros M et al (2016) MRI-based IMRT planning for MR-linac: comparison between CT- and MRI-based plans for pancreatic and prostate cancers. Phys Med Biol 61:3819–3842. https://doi.org/10.1088/0031-9155/61/10/3819
Hu Y, Zhao W, Du D et al (2015) Magnetic resonance imaging-based treatment planning for prostate cancer: use of population average tissue densities within the irradiated volume to improve plan accuracy. Pract Radiat Oncol 5:248–256. https://doi.org/10.1016/j.prro.2014.12.005
Cusumano D, Dinapoli N, Boldrini L et al (2018) Fractal-based radiomic approach to predict complete pathological response after chemo-radiotherapy in rectal cancer. Radiol Med 123:286–295. https://doi.org/10.1007/s11547-017-0838-3
Gatta R, Vallati M, Dinapoli N et al (2018) Towards a modular decision support system for radiomics: a case study on rectal cancer. Artif Intell Med. https://doi.org/10.1016/j.artmed.2018.09.003
Maspero M, Seevinck PR, Schubert G et al (2017) Quantification of confounding factors in MRI-based dose calculations as applied to prostate IMRT. Phys Med Biol 62:948. https://doi.org/10.1088/1361-6560/aa4fe7
International Commission on Radiation Units and Measurements (ICRU) (1992) Photon, electron, proton and neutron interaction data for body tissues. ICRU Report 46. Bethesda: International Commission on Radiation Units and Measurements
Taylor J (1997) An introduction to error analysis: the study of uncertainties in physical measurements, II. University Science Books, Sausalito
Wang Y, Mazur TR, Green O et al (2016) A GPU-accelerated Monte Carlo dose calculation platform and its application toward validating an MRI-guided radiation therapy beam model. Med Phys 43:4040. https://doi.org/10.1118/1.4953198
Low DA, Harms WB, Mutic S, Purdy JA (1998) A technique for the quantitative evaluation of dose distributions. Med Phys 25:656–661. https://doi.org/10.1118/1.598248
Hoffmann L, Alber M, Söhn M, Elstrøm UV (2018) Validation of the Acuros XB dose calculation algorithm versus Monte Carlo for clinical treatment plans. Med Phys. https://doi.org/10.1002/mp.13053
Song J-H, Kim M-J, Park S-H et al (2015) Gamma analysis dependence on specified low-dose thresholds for VMAT QA. J Appl Clin Med Phys 16:263–272. https://doi.org/10.1120/jacmp.v16i6.5696
Prior P, Chen X, Gore E et al (2017) Technical note: Is bulk electron density assignment appropriate for MRI-only based treatment planning for lung cancer? Med Phys 44:3437–3443. https://doi.org/10.1002/mp.12267
Prior P, Chen X, Botros M et al (2016) MRI-based IMRT planning for MR-linac: comparison between CT- and MRI-based plans for pancreatic and prostate cancers. Phys Med Biol 61:3819–3842. https://doi.org/10.1088/0031-9155/61/10/3819
Taylor J (1997) An introduction to error analysis: the study of uncertainties in physical measurements, II. University Science Books, Sausalito
Armstrong RA (2014) When to use the Bonferroni correction. Ophthalmic Physiol Opt 34:502–508. https://doi.org/10.1111/opo.12131
McHugh ML (2011) Multiple comparison analysis testing in ANOVA. Biochem Med (Zagreb) 21:203–209
Maspero M, Savenije MHF, Dinkla AM et al (2018) Dose evaluation of fast synthetic-CT generation using a generative adversarial network for general pelvis MR-only radiotherapy. Phys Med Biol 63:185001. https://doi.org/10.1088/1361-6560/aada6d
Riggs BL, Wahner HW, Dunn WL et al (1981) Differential changes in bone mineral density of the appendicular and axial skeleton with aging: relationship to spinal osteoporosis. J Clin Invest 67:328–335. https://doi.org/10.1172/JCI110039
Yao WJ, Wu CH, Wang ST et al (2001) Differential changes in regional bone mineral density in healthy Chinese: age-related and sex-dependent. Calcif Tissue Int 68:330–336. https://doi.org/10.1007/s002230001210
Beranger JS, Maqdes A, Pujol N et al (2016) Bone mineral density of the coracoid process decreases with age. Knee Surg Sports Traumatol Arthrosc 24:502–506. https://doi.org/10.1007/s00167-014-3483-6
Liu L, Jolly S, Cao Y et al (2017) Female pelvic synthetic CT generation based on joint intensity and shape analysis. Phys Med Biol 62:2935–2949. https://doi.org/10.1088/1361-6560/62/8/2935
Bredfeldt JS, Liu L, Feng M et al (2017) Synthetic CT for MRI-based liver stereotactic body radiotherapy treatment planning. Phys Med Biol 62:2922–2934. https://doi.org/10.1088/1361-6560/aa5059
Funding
This study was not funded by any company.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. L. Boldrini, Dr. D. Cusumano, Dr. F. Cellini and Dr. N. Dinapoli have received speaker honorarium ViewRay Technologies, Inc. The other authors do not have no conflicts of interest to disclose.
Ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all the individual participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Cusumano, D., Placidi, L., Teodoli, S. et al. On the accuracy of bulk synthetic CT for MR-guided online adaptive radiotherapy. Radiol med 125, 157–164 (2020). https://doi.org/10.1007/s11547-019-01090-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-019-01090-0