Abstract
Background
Acetabular osteophytes are common findings during total hip arthroplasty (THA).
Purpose
This study was designed to determine the extent to which osteophytes may limit range of motion (ROM) and in which locations impingement is likely to occur if osteophytes are not removed during surgery.
Methods
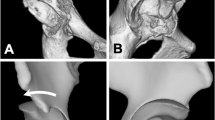
Computer-aided design was used to compare ROM of a modern hip implant in four cadaver models with and without 10-mm acetabular rim osteophytes added. A clock face, with 12 o’clock at the superior pole of the right acetabulum, was used to map impingement.
Results
The osteophyte model limited ROM in flexion (101° v. 113°, p = 0.03), 90° of flexion with internal rotation (16.7° v. 31.6°, p = 0.01), and external rotation (30.4° v. 49.5°, p = 0.01). Impingement occurred between 7 and 8 o’clock in external rotation and 1 and 2 o’clock in the other two motions.
Conclusions
Osteophytes in these positions have the greatest impact on ROM and should be removed during THA.




Similar content being viewed by others
References
Ali Khan MA, Brakenbury PH, Reynolds IS. Dislocation following total hip replacement. J Bone Joint Surg Br. 1981;63:214-218.
Amstutz HC, Campbell PA, Le Duff MJ. Fracture of the neck of the femur after surface arthroplasty of the hip. J Bone Joint Surg [Am]. 2004;86(9):1874-1877.
Amstutz H, Lodwig R, Schurman D, Hodgson AG. Range of motion studies for total hp replacements. A comparative study with a new experimental apparatus. Clin Orthop Relat Res. 1975;111:124.
Barrack RL, Butler RA, Laster DR, Andrews P. Stem design and dislocation after revision total hip arthroplasty: clinical results and computer modeling. J Arthroplasty. 2001;16(8 Suppl 1):8.
Chandler D, Glousman R, Hull D, et al. Prosthetic hip range of motion and impingement. The effects of head and neck geometry. Clin Orthop Relat Res. 1982;166:284.
Cobb J, Logishetty K, Davda K, Iranpour F. Cams and pincer impingement are distinct, not mixed: the acetabular pathomorphology of femoroacetabular impingement. Clin Orthop Relat Res. 2010;468(8):2143-2151.
Czubak J, Sionek A, Czwojdziński A. New concepts in the aetiology of primary osteoarthritis of the hip caused by femoroacetabular impingement. Ortop Traumatol Rehabil. 2010;12(6):479-492.
DeWal H, Su E, DiCesare PE. Instability following total hip arthroplasty. Am J Orthop (Belle Mead NJ). 2003;32(8):377-382.
Dorr LD, Wolf AW, Chandler R, Conaty JP. Classification and treatment of dislocations of total hip arthroplasty. Clin Orthop Rel Res. 1983;173:151.
Fackler C, Poss R. Dislocation in total hip arthroplasties. Clin Orthop Relat Res. 1980;151:169.
Hedlundh U, Ahnfelt L, Hybbinette CH, Weckstrom J, Fredin H. Surgical experience related to dislocations after total hip arthroplasty. J Bone Joint Surg Br. 1996;78:206.
Jolles BM, Zangger P, Leyvraz PF. Factors predisposing to dislocation after primary total hip arthroplasty: a multivariate analysis. J Arthroplasty. 2002;17:282.
Kaplan SJ, Thomas WH, Poss R. Trochanteric advancement for recurrent dislocation after total hip arthroplasty. J Arthroplasty. 1987;2:119.
Kassarjian A, Brisson M, Palmer WE. Femoroacetabular impingement. Eur J Radiol. 2007;63(1):29-35.
Katz JN, Losina E, Barrett J, et al. Association between hospital and surgeon procedure volume and outcomes of total hip replacement in the United States medicare population. J Bone Joint Surg [Am]. 2001;83:1622.
Kreder HJ, Deyo RA, Koepsell T, Swiontkowski MF, Kreuter W. Relationship between the volume of total hip replacements performed by providers and the rates of postoperative complications in the state of Washington. J Bone Joint Surg [Am]. 1997;79:485.
Krushell R, Burke D, Harris W. Range of motion in contemporary total hip arthroplasty. The impact of modular head-neck components. J Arthroplasty. 1991;6(2):97.
Kurtz WB, Ecker TM, Reichmann WM, Murphy SB. Factors affecting bony impingement in hip arthroplasty. J Arthroplasty. 2010;25(4):624-634.
Lewinnek GE, Lewis JL, Tarr R, Compere CL, Zimmerman JR. Dislocations after total hip-replacement arthroplasties. J Bone Joint Surg [Am]. 1978;60:217.
Malik A, Maheshwari A, Dorr LD. Impingement with total hip replacement. J Bone Joint Surg [Am]. 2007;89:1832-1842.
Nolan D, Fitzgerald R, Beckenbaugh R, Coventry MB. Complications of total hip arthroplasty treated by reoperation. J Bone Joint Surg [Am]. 1975;57:977.
Padgett DE, Warashina H. The unstable total hip replacement. Clin Orthop Relat Res. 2004;420:72.
Patel PD, Potts A, Froimson MI. The dislocating hip arthroplasty: prevention and treatment. J Arthroplasty. 2007;22(4 Suppl 1):86-90.
Scifert CF, Brown TD, Pedersen DR, Callaghan JJ. A finite element analysis of factors influencing total hip dislocation. Clin Orthop Rel Res. 1998;355:152.
Soong M, Rubash HE, Macaulay W. Dislocation after total hip arthroplasty. J Am Acad Orthop Surg. 2004;12(5):314-321.
Vendittoli P-A, Ganapathi M, Nuño N, Plamondon D, Lavigne M. Factors affecting hip range of motion in surface replacement arthroplasty. Clin Biomech. 2007;22(9):1004-1012.
Wheeless CR III: Wheeless’ textbook of orthopaedics. Data Trace Internet Publishing, Durham. 11 Apr 2011. <http://www.wheelessonline.com>.
Woo RY, Morrey BF. Dislocations after total hip arthroplasty. J Bone Joint Surg [Am]. 1982;64:1295.
Wright AA, Cook C, Abbott JH. Variables associated with the progression of hip osteoarthritis: a systematic review. Arthritis Rheum. 2009;61(7):925-936.
Acknowledgments
This study was partially funded by the generous donation of Dr. Alberto Foglia and his wife Maria Pia. Study was supported by a grant from Stryker Orthopedics.
Disclosure
ᅟ
Conflict of Interest:
Sebastian Rodriguez-Elizalde, MD, Alyssa M. Yeager, BA, Bheeshma Ravi, MD, Eduardo A. Salvati, MD have declared that they have no conflict of interest. Geoffrey H. Westrich, MD received research grant from Stryker Orthopedics in support of the study; is a paid consultant for Stryker Orthopedics, outside the work. Joseph D. Lipman, MS is a paid consultant for Ivy Sport Medicine; employee of Hospital for Special Surgery; has the following patents: Posterior Stabilized Knee Prosthesis, Self-aligning knee prosthesis, Dual radius glenoid prosthetic component for total shoulder arthroplasty, Pelvic Positioner, Trochlear Clamp, Patella Resection Drill and Prosthesis Implantation Device; has pending patents for Constrained Condylar Knee Device, Prosthetic Condylar Joints With Articulating Bearing Surfaces Having A Translating Contact Point During Rotation Thereof, Elbow Replacement Apparatus And Methods, Expanding Cannula And Retractor Device And Methods Of Use and External fixation devices and methods of use; receives royalties payment from Mathys Inc. and Ortho Development Corp; has received travel support for travel to meetings from Chinese Orthopaedic Association, outside the work.
Human/Animal Rights:
This article does not contain any studies with human or animal subjects performed by the any of the authors.
Informed Consent:
Informed consent was obtained from all patients for being included in the study.
Required Author Forms
Disclosure forms provided by the authors are available with the online version of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rodriguez-Elizalde, S., Yeager, A.M., Ravi, B. et al. Computerized Virtual Surgery Demonstrates Where Acetabular Rim Osteophytes Most Reduce Range of Motion Following Total Hip Arthroplasty. HSS Jrnl 9, 223–228 (2013). https://doi.org/10.1007/s11420-013-9337-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11420-013-9337-9