Abstract
Purpose
Obstructive sleep apnea (OSA) is a common health problem that affects more than 2–4% of the US population. Polysomnography (PSG) is the gold standard for diagnosing OSA. PSG is, however, expensive, time-consuming, and not always readily accessible. Hence, alternative diagnostic methods such as home-based testing have been evaluated. We studied the ability of the REMstar Pro (RSP2, a brand of continuous positive airway pressure (CPAP) device) to identify abnormal breathing events in subjects with OSA and compared this with breathing events simultaneously determined by laboratory-based PSG.
Methods
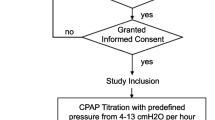
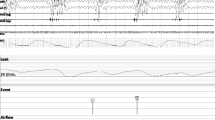
We evaluated 10 subjects previously diagnosed with OSA (apnea hypopnea index (AHI) > 15, known therapeutic level of CPAP). Subjects underwent attended PSG using the REMstar Pro M series machine and their prescribed interface/mask type. The first 3 h of the study were conducted using a subtherapeutic CPAP (4 cm H2O). The last 3 h or remaining portion of the PSG was completed using the previously determined therapeutic CPAP. Comparison of respiratory events detected by PSG vs the RSP2 was performed.
Results
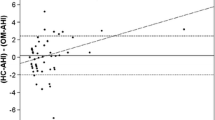
Subjects included four men and six women, aged 32 to 57 years and with a body mass index ranging from 29.5–66.4. The baseline AHI ranged from 18.3–93.1, with the AHI at therapeutic CPAP ranging from 0–3. Apnea counts at baseline and at therapeutic CPAP by manually scored PSG and REMstar were not significantly different (mean at subtherapeutic 11.7 vs 12.5, p = 0.76; median at therapeutic CPAP 2.0 vs 4.5, p = 0.15). Hypopnea counts at baseline and at effective CPAP by PSG and REMstar were not significantly different (mean at subtherapeutic 38.1 vs. 40.9, p = 0.72; median at therapeutic CPAP 5.0 vs. 2.5, p = 0.34). The correlation coefficient of REMstar and PSG for apnea and hypopnea was significant in subtherapeutic phase only (apnea r = 0.78, p = 0.007; hypopnea r = 0.76, p = 0.01). Agreement between the two methods declined for hypopnea detection at therapeutic CPAP.
Conclusions
The monitoring of residual sleep-disordered breathing on treatment, in addition to adherence, is an important objective therapeutic target in OSA. The REMstar Pro detects sleep-disordered breathing events similar to that of a manually scored PSG—for apnea but not for hypopnea—and merits further investigation as a device to determine disease severity and treatment efficacy.



Similar content being viewed by others
References
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328(17):1230–1235
Day R, Gerhardstein R, Lumley A, Roth T, Rosenthal L (1999) The behavioral morbidity of obstructive sleep apnea. Prog Cardiovasc Dis 41(5):341–354
D’Ambrosio C, Bowman T, Mohsenin V (1999) Quality of life in patients with obstructive sleep apnea: effect of nasal continuous positive airway pressure—a prospective study. Chest 115(1):123–129
Alghanim N, Comondore VR, Fleetham J, Marra CA, Ayas NT (2008) The economic impact of obstructive sleep apnea. Lung 186(1):7–12
Quan SF, Gersh BJ (2004) Cardiovascular consequences of sleep-disordered breathing: past, present and future: report of a workshop from the National Center on Sleep Disorders Research and the National Heart, Lung, and Blood Institute. Circulation 109(8):951–957
Nieto FJ, Young TB, Lind BK et al (2000) Association of sleep-disordered breathing, sleep apnea, and hypertension in a large community-based study. Sleep Heart Health Study. Jama 283(14):1829–1836
Yaggi HK, Concato J, Kernan WN, Lichtman JH, Brass LM, Mohsenin V (2005) Obstructive sleep apnea as a risk factor for stroke and death. N Engl J Med 353(19):2034–2041
Marshall NS, Wong KK, Liu PY, Cullen SR, Knuiman MW, Grunstein RR (2008) Sleep apnea as an independent risk factor for all-cause mortality: the Busselton Health Study. Sleep 31(8):1079–1085
Chesson AL Jr, Berry RB, Pack A (2003) Practice parameters for the use of portable monitoring devices in the investigation of suspected obstructive sleep apnea in adults. Sleep 26(7):907–913
Santamaria J, Iranzo A, Ma Montserrat J, de Pablo J (2007) Persistent sleepiness in CPAP treated obstructive sleep apnea patients: evaluation and treatment. Sleep Med Rev 11(3):195–207
Stradling JR, Smith D, Crosby J (2007) Post-CPAP sleepiness—a specific syndrome? J Sleep Res 16(4):436–438
Baltzan MA, Kassissia I, Elkholi O, Palayew M, Dabrusin R, Wolkove N (2006) Prevalence of persistent sleep apnea in patients treated with continuous positive airway pressure. Sleep 29(4):557–563
Portier F, Portmann A, Czernichow P et al (2000) Evaluation of home versus laboratory polysomnography in the diagnosis of sleep apnea syndrome. Am J Respir Crit Care Med 162(3 Pt 1):814–818
Iber C, Ancoli-Israel S, Chesson AL, Quan SF (2007) The AASM manual for the scoring of sleep and associated events. American Academy of Sleep Medicine, Westchester
Kushida CA, Chediak A, Berry RB et al (2008) Clinical guidelines for the manual titration of positive airway pressure in patients with obstructive sleep apnea. J Clin Sleep Med 4(2):157–171
Ikeda Y KT, Takaya H, Maeno K, Kawana F, Ishiwata S, Narui K (2008) Validation of breathing event detection of the REMstar auto M-series compared to clinical polysomnography ATS international conference abstracts, A212
Acknowledgment
The authors would like to thank the clinical and research staff of the Sleep Science Center and the Center for Narcolepsy, Sleep and Health Research at the University of Illinois at Chicago.
Disclosure
This study was funded by Respironics, Inc., Murrysville, PA, USA.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Prasad, B., Carley, D.W. & Herdegen, J.J. Continuous positive airway pressure device-based automated detection of obstructive sleep apnea compared to standard laboratory polysomnography. Sleep Breath 14, 101–107 (2010). https://doi.org/10.1007/s11325-009-0285-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-009-0285-z