Abstract
Introduction
The treatment of neurogenic dysfunctions of micturition, both surgical and conservative, aims primarily to protect upper urinary tract function. This goal can be achieved by lowering intravesical pressure and increasing urinary bladder capacity in the urine collection phase or by facilitating bladder emptying.
Objective
The objective of this paper was to assess the outcome of transcutaneous stimulation of the urinary bladder in the treatment of neurogenic disorders of micturition.
Materials and methods
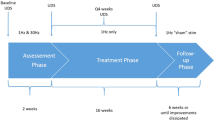
The effect of urinary bladder stimulation was assessed in 22 patients (4 females, 18 males) with spinal injuries (19 with injuries to the lumbo-sacral spine and 3 with cervical spine injuries) treated at the Department of Rehabilitation of the Military Hospital in Bydgoszcz, Poland, in 2006 and 2007. The treatment consisted of 30 procedures of transcutaneous electrical stimulation of the urinary bladder. A pulsed sinusoid current was used with a pulse duration of 200 ms, break duration of 1,000 ms, intensity of 15–20 mA, frequency of 50 Hz, and duration of stimulation of 15 min. A urodynamic study was carried out in each patient at baseline and on completion of the electrical stimulation therapy (immediately and after 2 months).
Results
Electrical stimulation of the neurogenic urinary bladder produced increases in the cystometric bladder capacity and reduction in the amount of residual urine (72% of patients), with reduction of intravesical pressure at peak urine flow (59% of the patients). The dynamic aspects of micturition also improved with increased peak voiding velocity in 77.3% of the patients. More than half of the patients (57%) still had elevated intravesical pressures during micturition that posed a risk to the function of the upper urinary tract despite significant decreases following the stimulation therapy. Micturition, which was absent at baseline, was restored in three patients. No local complications were observed.
Conclusions
Transcutaneous electrical stimulation of the urinary bladder in patients with neurogenic bladder dysfunction improves lower urinary tract function. Urodynamic studies executed 2 months after finishing TES show persistent results.



Similar content being viewed by others
References
Lee BB, Haran MJ, Hunt LM, Simpson JM, Marial O, Rutkowski SB et al (2007) Spinal-injured neuropathic bladder antisepsis (SINBA) trial. Spinal Cord 45(8):542–550. doi:10.1038/sj.sc.3101974
Blok BF, Sturms LM, Holstege G (1998) Brain activation during micturition in women. Brain 121:2031–2032. doi:10.1093/brain/121.11.2033
Hruz P, Lövblad KO, Nirkko AC, Thoeny H, El-Koussy M, Danuser H (2008) Identification of brain structures involved in micturition with functional magnetic resonance imaging (fMRI). J Neuroradiol 35(3):144–149. doi:10.1016/j.neurad.2007.11.008
Perneczky R, Diehl-Schmid J, Förstl H, Drzezga A, May F, Kurz A (2008) Urinary incontinence and its functional anatomy in frontotemporal lobar degenerations. Eur J Nucl Med Mol Imaging 35(3):605–610. doi:10.1007/s00259-007-0626-8
Samson G, Cardenas DD (2007) Neurogenic bladder in spinal cord injury. Phys Med Rehabil Clin N Am 18(2):255–274. doi:10.1016/j.pmr.2007.03.005
Nosseir M, Hinkel A, Pannek J (2007) Clinical usefulness of urodynamic assessment for maintenance of bladder function in patients with spinal cord injury. Neurourol Urodyn 26(2):228–233. doi:10.1002/nau.20319
Schmid DM, Reitz A, Curt A, Hauri D, Schurch B (2004) Urethral evoked sympathetic skin responses and viscerosensory evoked potentials as diagnostic tools to evaluate urogenital autonomic afferent innervation in spinal cord injured patients. J Urol 171(3):1156–1160. doi:10.1097/01.ju.0000111809.81966.8b
Abrams P (1997) Urodynamics, vol 2. Springer-Verlag, Berlin
Freeman R, Malvern J (1989) The Unstable Bladder. Butterworth & Co (Publishers) Ltd, London
Lewis JM, Cheng EY (2007) Non-traditional management of the neurogenic bladder: tissue engineering and neuromodulation. Sci World J 7:1230–1241
Pugach JL, Salvin L, Steinhardt GF (2000) Intravesical electrostimulation in pediatric patients with spinal cord defects. J Urol 164(3):956–958. doi:10.1016/S0022-5347(05)67227-8
Amarenco G, Ismael SS, Even-Schneider A, Raibaut P, Demaille-Wlodyka S, Parratte B et al (2003) Urodynamic effect of acute transcutaneous posterior tibial nerve stimulation in overactive bladder. J Urol 169(6):2210–2215. doi:10.1097/01.ju.0000067446.17576.bd
Hagerty JA, Richards I, Kaplan WE (2007) Intravesical electrotherapy for neurogenic bladder dysfunction: a 22-year experience. J Urol 178(4):1680–1683. doi:10.1016/j.juro.2007.03.188
Huber ER, Kiss G, Berger T, Rehder P, Madersbacher H (2007) The value of intravesical electrostimulation in the treatment of acute prolonged bladder overdistension. Urology 46(6):662–666. doi:10.1007/s00120-007-1312-y
Dolezel J, Cejpek P, Miklánek D (2002) Sacral deafferentation and neurostimulation of anterior spinal roots in the treatment of neurogenic bladder in patients with complete transverse spinal lesions – initial clinical experience. Rozhl Chir 81(4):203–209
Lazzeri M (1997) Urodynamic effects of intravesical resinferatoxin in humans: preliminary results in stable and unstable detrusor. J Urol 158:2093–2096. doi:10.1016/S0022-5347(01)68164-3
Brubaker L (2000) Electrical stimulation in overactive bladder. Urology 55(5A Suppl):17–23
Vandoninck V (2003) Percutaneous tibial nerve stimulation in treatment of overactive bladder; urodynamic data. BJU Int 91(7):711–715. doi:10.1046/j.1464-410X.2003.04185.x
Dalmose A, Rijkhoff NJ, Kirkeby HJ, Nohr M, Sinkjaer T, Djurhuus JC (2003) Conditional stimulation of dorsal penile/clitoral nerve may increase cystometric capacity in patients with spinal cord injury. Neurourol Urodyn 22:130–137
Lee YH. (2003) Detrusor and blood pressure responses to dorsal penile nerve stimulation during hyperreflectic contraction of the bladder in patients with cervical cord injury. Neurourol Urodyn 84(1):136–140. doi:10.1002/nau.10031
Vastenholt JM (2003) A 7-year follow-up of sacral anterior root stimulation for bladder control in patients wih a spinal cord injury: quality of life and users experiences. Spinal Cord 41(7):397–402. doi:10.1038/sj.sc.3101465
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Radziszewski, K., Zielinski, H., Radziszewski, P. et al. Transcutaneous electrical stimulation of urinary bladder in patients with spinal cord injuries. Int Urol Nephrol 41, 497–503 (2009). https://doi.org/10.1007/s11255-008-9488-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-008-9488-7