Abstract
Objective
Fibroblast growth factor (FGF) 23 is a circulating factor that regulates phosphate (P) metabolism. Since higher P levels are associated with vascular calcification, we examined the role of serum FGF-23 levels in P metabolism and vascular calcification in hemodialysis (HD) patients with and without diabetes mellitus (DM).
Materials and methods
Chronic HD patients with DM (n = 39) and without DM (n = 50) were enrolled. Serum samples were obtained before the start of dialysis sessions, and the FGF-23 levels were determined by enzyme-linked immunosorbent assay. Abdominal computed tomography (CT) scan was performed, and the aortic calcification index (ACI) was determined by one examiner, blinded to the patient characteristics. Measurements of bone mineral density (BMD) were performed at the time of ACI estimation.
Results
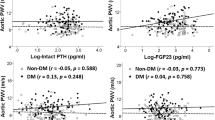
Log plasma FGF-23 levels were higher in non-DM (3.74 ± 0.71 pg/ml) than in DM (3.35 ± 0.74 pg/ml) patients. The log FGF-23 correlated positively with serum creatinine (r = 0.424, P < 0.0001), albumin (r = 0.225, P = 0.0337), Ca (r = 0.392, P = 0.0001), P (r = 0.735, P < 0.0001), and Ca × P product (r = 0.780, P < 0.0001). There were negative correlations between log FGF-23 and age (r = −0.208, P = 0.0497), glucose (r = −0.231, P = 0.0294), and CRP (r = −0.222, P = 0.0359). Multiple regression analyses were performed to explore the correlations between plasma FGF-23 and other factors associated with vascular calcification in all HD patients. Independent variables were selected based on the results of univariate analyses. The significant factors associated with FGF-23 in HD patients were age, serum levels of creatinine, albumin, glucose, Ca, P, and Ca × P product. Plasma FGF levels did not correlate significantly with either ACI or BMD in these patients.
Conclusion
Our findings indicate that the plasma FGF-23 level is associated with calcium-phosphate metabolism disorders, but not with aortic calcification, in both non-DM and DM patients on chronic HD. In addition, plasma FGF-23 is associated with serum levels of creatinine and albumin. Therefore, the plasma FGF-23 level may provide a reliable marker for Ca and P imbalance and nutritional status in HD patients.



Similar content being viewed by others
References
Foley RN, Murray AM, Li S et al (2005) Chronic kidney disease and the risk factor for cardiovascular disease, renal replacement, and death in the United States Medicare population, 1998–1999. J Am Soc Nephrol 16:489–495. doi:10.1681/ASN.2004030203
Goodman WG, Goldin J, Kuizon BD et al (2000) Coronary-artery calcification in young adults with end-stage renal disease who are undergoing dialysis. N Engl J Med 342:1478–1483. doi:10.1056/NEJM200005183422003
Raggi P, Boulay A, Chasan-Taber S et al (2002) Cardiac calcification in adult hemodialysis patients. A link between end-stage renal disease and cardiovascular disease? J Am Coll Cardiol 39:695–701. doi:10.1016/S0735-1097(01)01781-8
Moe SM, Chen NX (2008) Mechanisms of vascular calcification in chronic kidney disease. J Am Soc Nephrol 19:213–216. doi:10.1681/ASN.2007080854
Massy ZA, Mentaverri R, Mozar A et al (2008) The pathophysiology of vascular calcification: are osteoclast-like cells the missing link? Diabetes Metab 34(Suppl 1):S16–S20. doi:10.1016/S1262-3636(08)70098-3
Guerin AP, London GM, Marchais SJ, Metivier F (2000) Arterial stiffening and vascular calcifications in end-stage renal disease. Nephrol Dial Transplant 15:1014–1021. doi:10.1093/ndt/15.7.1014
Giachelli CM, Jono S, Shioi A et al (2001) Vascular calcification and inorganic phosphate. Am J Kidney Dis 38(4 Suppl 1):S34–S37. doi:10.1053/ajkd.2001.27394
Davies MR, Hruska KA (2001) Pathophysiological mechanisms of vascular calcification in end stage renal disease. Kidney Int 60:472–479. doi:10.1046/j.1523-1755.2001.060002472.x
Lehto S, Niskanen L, Suhonen M, Ronnemaa T, Laakso M (1996) Medial artery calcification. A neglected harbinger of cardiovascular complications in non-insulin-dependent diabetes mellitus. Arterioscler Thromb Vasc Biol 16:978–983
Nitta K, Akiba T, Uchida K et al (2003) The progression of vascular calcification and serum osteoprotegerin levels in patients on long-term hemodialysis. Am J Kidney Dis 42:303–309. doi:10.1016/S0272-6386(03)00655-3
Chertow GM, Raggi P, Chasan-Taber S et al (2004) Determinants of progressive vascular calcification in haemodialysis patients. Nephrol Dial Transplant 19:1489–1496. doi:10.1093/ndt/gfh125
Ishimura E, Okuno S, Kitatani K et al (2002) Different risk factors for peripheral vascular calcification between diabetic and non-diabetic haemodialysis patients-importance of glycaemic control. Diabetologia 45:1446–1448. doi:10.1007/s00125-002-0920-8
Kimura K, Saika Y, Otani H et al (1999) Factors associated with calcification of the abdominal aorta in hemodialysis patients. Kidney Int Suppl 71:S238–S241. doi:10.1046/j.1523-1755.1999.07163.x
Yamashita T, Yoshioka M, Itoh N (2000) Identification of a novel fibroblast growth factor, FGF-23, preferentially expressed in the ventrolateral thalamic nucleus of the brain. Biochem Biophys Res Commun 277:494–498. doi:10.1006/bbrc.2000.3696
Yamashita T, Konishi M, Miyake A et al (2002) Fibroblast growth factor (FGF)-23 inhibits renal phosphate reabsorption by activation of the mitogen-activated protein kinase pathway. J Biol Chem 277:28265–28270. doi:10.1074/jbc.M202527200
Imanishi Y, Inaba M, Nakatsuka K et al (2004) FGF-23 in patients with end-stage renal disease on hemodialysis. Kidney Int 65:1943–1946. doi:10.1111/j.1523-1755.2004.00604.x
Fukagawa M, Hamada Y, Nakanishi S, Tanaka M (2006) The kidney and bone metabolism: nephrologists’ point of view. J Bone Miner Metab 24:434–438. doi:10.1007/s00774-006-0719-7
Mirams M, Robinson BG, Mason RS, Nelson AE (2004) Bone as a source of FGF-23: regulation by phosphate? Bone 35:1192–1199. doi:10.1016/j.bone.2004.06.014
Nishizawa Y, Jono S, Ishimura E, Shioi A (2005) Hyperphosphatemia and vascular calcification in end-stage renal disease. J Ren Nutr 15:178–182. doi:10.1053/j.jrn.2004.09.027
Alberti KG, Zimmet PZ (1998) Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med 15:539–553. doi:10.1002/(SICI)1096-9136(199807)15:7<539::AID-DIA668>3.0.CO;2-S
Takei T, Otsubo S, Uchida K et al (2008) Effects of sevelamer on the progression of vascular calcification in patients on chronic haemodialysis. Nephron Clin Pract 108:c278–c283. doi:10.1159/000127361
Hayashi Y, Yamamoto K, Fukunaga M et al (1990) Assessment of bone mass by image analysis of metacarpal bone roentgenograms: a quantitative digital image processing (DIP) method. Radiat Med 8:173–178
Ishikawa K, Ohta T (1999) Radial and metacarpal bone mineral density and calcaneal quantitative ultrasound bone mass in normal Japanese women. Calcif Tissue Int 65:112–116. doi:10.1007/s002239900666
Inaba M, Okuno S, Kumeda Y et al (2007) Glycated albumin is a better glycemic indicator than glycated hemoglobin values in hemodialysis patients with diabetes: effect of anemia and erythropoietin injection. J Am Soc Nephrol 18:896–903. doi:10.1681/ASN.2006070772
Yamazaki Y, Okazaki R, Shibata M et al (2002) Increased circulatory level of biologically active full-length FGF-23 in patients with hypophosphatemic rickets/osteomalacia. J Clin Endocrinol Metab 87:4957–4960. doi:10.1210/jc.2002-021105
Miwa N, Nitta K, Kimata N et al (2003) An evaluation of 1–84 PTH measurement in relation to bone alkaline phosphatase and bone Gla protein in hemodialysis patients. Nephron Clin Pract 94:c29–c32. doi:10.1159/000071278
Sezer S, Ozdemir FN, Arat Z et al (2002) Triad of malnutrition, inflammation, and atherosclerosis in hemodialysis patients. Nephron 91:456–462. doi:10.1159/000064287
Inaba M, Okuno S, Imanishi Y et al (2006) Role of fibroblast growth factor-23 in peripheral vascular calcification in non-diabetic and diabetic hemodialysis patients. Osteoporos Int 17:1506–1513. doi:10.1007/s00198-006-0154-6
Gupta A, Winer K, Econs MJ, Marx SJ, Collins MT (2004) FGF-23 is elevated by chronic hyperphosphatemia. J Clin Endocrinol Metab 89:4489–4492. doi:10.1210/jc.2004-0724
Imel EA, Econs MJ (2005) Fibroblast growth factor 23: roles in health and disease. J Am Soc Nephrol 16:2565–2575. doi:10.1681/ASN.2005050573
Taniwaki H, Ishimura E, Tabata T et al (2005) Aortic calcification in haemodialysis patients with diabetes mellitus. Nephrol Dial Transplant 20:2472–2478. doi:10.1093/ndt/gfi039
Benet-Pages A, Orlik P, Strom TM, Lorenz-Depiereux B (2005) An FGF23 missense mutation causes familial tumoral calcinosis with hyperphosphatemia. Hum Mol Genet 14:385–390. doi:10.1093/hmg/ddi034
Shimada T, Kakitani M, Yamazaki Y et al (2004) Targeted ablation of Fgf23 demonstrates an essential physiological role of FGF23 in phosphate and vitamin D metabolism. J Clin Invest 113:561–568
Razzaque MS, St-Arnaud R, Taguchi T, Lanske B (2005) FGF-23, vitamin D and calcification: the unholy triad. Nephrol Dial Transplant 20:2032–2035. doi:10.1093/ndt/gfh991
London GM, Marty C, Marchais SJ et al (2004) Arterial calcification and bone histomorphometry in end-stage renal disease. J Am Soc Nephrol 15:1943–1951. doi:10.1097/01.ASN.0000129337.50739.48
Spasovski GB (2007) Bone health and vascular calcification relationships in chronic kidney disease. Int Urol Nephrol 39:1209–1216. doi:10.1007/s11255-007-9276-9
Acknowledgements
We thank all medical personnel of the dialysis Units in Koshin Clinic for collecting the medical records. This work was supported by grants from the Japan Research Promotion Society for Cardiovascular Diseases the International Research and the Educational Institute and for Integrated Medical Sciences (IREIMS).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kojima, F., Uchida, K., Ogawa, T. et al. Plasma levels of fibroblast growth factor-23 and mineral metabolism in diabetic and non-diabetic patients on chronic hemodialysis. Int Urol Nephrol 40, 1067–1074 (2008). https://doi.org/10.1007/s11255-008-9462-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-008-9462-4