Abstract
The concomitant use of low-dose aspirin for cardioprotection and non-steroidal anti-inflammatory agents for pain relief is prevalent, particularly in the elderly for whom cardiovascular disease and pain are common co-morbidities. Non-selective non-steroidal anti-inflammatory drugs (NSAIDs) are known to interfere with the antiplatelet effect of aspirin through competitive binding with COX-1. While the clinical significance of this interference is still unclear, this review sought to assess the body of literature which has evaluated the potential attenuation of the anti-platelet effect of aspirin when dosed concomitantly with an NSAID. This review supports that the pharmacodynamic interaction between aspirin and non-selective NSAIDs occurs, but finds that the interaction varies amongst agents, and is highly dependent on numerous factors including: dose timing, dose of aspirin, and dose of the NSAID in question. Recent findings suggest that patient factors, such as body weight may also be indicators of aspirin’s cardiovascular effectiveness. Ultimately, the clinical decision making for concomitant NSAID and low-dose aspirin regimens remains at the patient level.

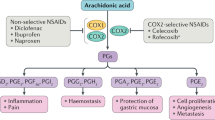
Reproduced with permission from Goodman and Gilman [25]
Similar content being viewed by others
References
Awtry EH, Loscalzo J (2000) Aspirin. Circulation 101:1206–1218
Bibbins-Domingo K, U.S. Preventive Services Task Force (2016) Aspirin use for the primary prevention of cardiovascular disease and colorectal cancer: U.S. preventive services task force recommendation statement. Ann Intern Med 164:836–845
Smith SC Jr et al (2011) AHA/ACCF secondary prevention and risk reduction therapy for patients with coronary and other atherosclerotic vascular disease: 2011 update: a guideline from the American Heart Association and American College of Cardiology Foundation. Circulation 124:2458–2473
McNeil JJ, Nelson MR, Woods RL, ASPREE Investigator Group et al (2018) Effect of aspirin on all-cause mortality in the healthy elderly. N Engl J Med 379:1519–1528
Zhou Y, Boudreau DM, Freedman AN (2014) Trends in the use of aspirin and nonsteroidal anti-inflammatory drugs in the general U.S. population. Pharmacoepidemiol Drug Saf 23:43–50
Sopena F, Lanas A (2007) How to advise aspirin use in patients who need NSAIDs. Curr Pharm Des 13:2248–2260
FDA Information for Healthcare Professionals (2006) Concomitant use of ibuprofen and aspirin new information. http://www.fda.gov/Drugs/DrugSafety/PostmarketDrugSafetyInformationforPatientsandProviders/ucm. Accessed 12 Aug 2018
Farkouh ME, Greenberg JD, Jeger RV et al (2007) Cardiovascular outcomes in high risk patients with osteoarthritis treated with ibuprofen, naproxen or lumiracoxib. Ann Rheum Dis 66:764–770
Hernandez-Diaz S, Varas-Lorenzo C, Garcia Rodriguez LA (2006) Non-steroidal antiinflammatory drugs and the risk of acute myocardial infarction. Basic Clin Pharmacol Toxicol 98:266–274
Varas-Lorenzo C, Riera-Guardia N, Calingaert B et al (2013) Myocardial infarction and individual nonsteroidal anti-inflammatory drugs meta-analysis of observational studies. Pharmacoepidemiol Drug Saf 22:559–570
Yokoyama H, Ito N, Soeda S, Ozaki M, Suzuki Y, Watanabe M, Kashiwakura E, Kawada T, Yamada Y (2013) et al. Influence of non-steroidal anti-inflammatory drugs on antiplatelet effect of aspirin. J Clin Pharm Ther 38:12–15
Patrono C, García Rodríguez LA, Landolfi R, Baigent C (2005) Low-dose aspirin for the prevention of atherothrombosis. N Engl J Med 353:2373–2383
Catella-Lawson F, Reilly MP et al (2001) Cyclooxygenase inhibitors and the antiplatelet effects of aspirin. N Engl J Med 345:1809–1817
Capone ML, Sciulli MG, Tacconelli S, Grana M, Ricciotti E, Renda G, DiGregorio P, Merciaro G, Patrignani P (2005) Pharmacodynamic interaction of naproxen with low-dose aspirin in healthy subjects. J Am Coll Cardiol 45:1295–1301
Gurbel PA, Bliden KP, Zhu J, Troullos E et al (2018) Thromboxane inhibition during concurrent therapy with low-dose aspirin and over-the-counter naproxen sodium. J Thromb Thrombolysis 45:18–26
Vane JR (1971) Inhibition of prostaglandin synthesis as a mechanism of action for the aspirin-like drugs. Nature 231:232–235
Sellers RS, Radi ZA, Khan NK (2010) Pathophysiology of cyclooxygenases in cardiovascular homeostasis. Vet Pathol 47:601–613
Tantry US, Mahla E, Gurbel PA (2009) Aspirin resistance. Prog Cardiovasc Dis 52:141–152
Kirkby NS, Lundberg MH, Harrington LS et al (2012) Cyclooxygenase-1, not cyclooxygenase-2, is responsible for physiological production of prostacyclin in the cardiovascular system. Proc Natl Acad Sci USA 109:17597–17602
Yu Y, Ricciotti E, Scalia R et al (2012) Vascular COX-2 modulates blood pressure and thrombosis in mice. Sci Transl Med 4:132ra154
Majed BH, Khalil RA (2012) Molecular mechanisms regulating the vascular prostacyclin pathways and their adaptation during pregnancy and in the newborn. Pharmacol Rev 64:540–582
Zarraga IG, Schwarz ER (2007) Coxibs and heart disease: what we have learned and what else we need to know. J Am Coll Cardiol 49:1–14
Wallace JL (2008) Prostaglandins, NSAIDs, and gastric mucosal protection: why doesn’t the stomach digest itself? Physiol Rev 88:1547–1565
Ghosh R, Alajbegovic A, Gomes AV (2015) NSAIDs and cardiovascular diseases: role of reactive oxygen species. Oxid Med Cell Longev 2015:536962
Goodman LS, Gilman A (eds) (2011) Anti-inflammatory, antipyretic, and analgesic agents; pharmacotherapy of gout. In: The pharmacological basis of therapeutics, 12th edn. Pergamon Press, New York
Cheema A (2004) Should people on aspirin avoid ibuprofen? A review of the literature. Cardiol Rev 12:174–176
FitzGerald GA, Oates JA, Hawiger J et al (1983) Endogenous biosynthesis of prostacyclin and thromboxane and platelet function during chronic administration of aspirin in man. J Clin Invest 71:676–688
Patrono C, Ciabattoni G, Patrignani P et al (1985) Clinical pharmacology of platelet cyclooxygenase inhibition. Circulation 72:177–184
Rao GH, Fareed J (2012) Aspirin prophylaxis for the prevention of thrombosis: expectations and limitations. Thrombosis 2012:104707
Patrono C, Ciabattoni G, Pinca E, Pugliese F et al (1980) Low dose aspirin and inhibition of thromboxane B2 production in healthy subjects. Thromb Res 17:317–327
Van Ryn J, Kink-Eiband M, Kuritsch I et al (2004) Meloxicam does not affect the antiplatelet effect of aspirin in healthy male and female volunteers. J Clin Pharmacol 44:777–784
Renda G, Tacconelli S, Capone ML, Sacchetta D et al (2006) Celecoxib, ibuprofen, and the antiplatelet effect of aspirin in patients with osteoarthritis and ischemic heart disease. Clin Pharmacol Ther 80:264–274
VanHecken A, Juliano ML, Depre M, Lepeleire ID, Arnout J, Dynder A, Wildonger L, Petty KJ, Gottesdiener K, Hoon JND (2002) Effects of enteric-coated, low-dose aspirin on parameters of platelet function. Aliment Pharmacol Ther 16:1683–1688
Gurbel PA, Bliden KP, DiChiara J, Newcomer J et al (2007) Evaluation of dose-related effects of aspirin on platelet function: results from the Aspirin-Induced Platelet Effect (ASPECT) study. Circulation 115:3156–3164
Reilly IA, FitzGerald GA (1987) Inhibition of thromboxane formation in vivo and ex vivo: implications for therapy with platelet inhibitory drugs. Blood 69:180–186
Rothwell PM, Cook NF, Gaziano M et al (2018) Effects of aspirin on the risks of vascular events and cancer according to bodyweight and dose: analysis of individual patient data from randomized trials. Lancet 392:387–399
Solomon D. NSAIDS (2013) Mechanism of action 2. http://www.uptodate.com/contents/nsaidsmechanism-of-action. Accessed on 10 Aug 2018
Capone ML, Tacconelli S, Sciulli MG et al (2004) Clinical pharmacology of platelet, monocyte, and vascular cyclooxygenase inhibition by naproxen and low-dose aspirin in healthy subjects. Circulation 109:1468–1471
Cryer B, Berlin RG, Cooper SA et al (2005) Double-blind, randomized, parallel, placebo-controlled study of ibuprofen effects on thromboxane B2 concentrations in aspirin-treated healthy adult volunteers. Clin Ther 27:185–191
Gengo FM, Rubin L, Robson M, Rainka M et al (2008) Effects of ibuprofen on the magnitude and duration of aspirin’s inhibition of platelet aggregation: clinical consequences in stroke prophylaxis. J Clin Pharmacol 48:117–122
Gladding PA, Webster MWI, Farrell HB et al (2008) The antiplatelet effect of six non-steroidal anti-inflammatory drugs and their pharmacodynamic interaction with aspirin in healthy volunteers. Am J Cardiol 101:1060–1063
Hong Y, Gengo FM, Rainka MM et al (2008) Population pharmacodynamic modelling of aspirin- and Ibuprofen-induced inhibition of platelet aggregation in healthy subjects. Clin Pharmacokinet 47:129–137
Galliard-Grigioni KS, Reinhart WH (2009) A randomized, controlled study on the influence of acetaminophen, diclofenac, or naproxen on aspirin-induced inhibition of platelet aggregation. Eur J Pharmacol 609:96–99
Schiff M, Hochberg MC, Oldenhof J, Brune K (2009) Platelet inhibitory effects of OTC doses of naproxen sodium compared with prescription dose naproxen sodium and low-dose aspirin. Curr Med Res Opin 25:2471–2477
Oldenhof J, Hochberg M, Schiff M, Brune K (2010) Effect of maximum OTC doses of naproxen sodium or acetaminophen on low-dose aspirin inhibition of serum thromboxane B2. Curr Med Res Opin 26:1497–1504
Schuijt MP, Huntjens-Fleuren HW, de Metz M, Vollaard EJ (2009) The interaction of ibuprofen and diclofenac with aspirin in healthy volunteers. Br J Pharmacol 157:931–934
Angiolillo DJ, Desai B, Hwang C et al (2011) Impact of a fixed-dose combination of naproxen and esomeprazole magnesium on serum thromboxane b2 inhibition by low-dose aspirin over 5 days in healthy adults: a phase I, randomized, double-blind, placebo-controlled, non-inferiority trial. Clin Ther 33:1883–1893
Anzellotti P, Capone ML, Jeyam A et al (2011) Low-dose naproxen interferes with the antiplatelet effects of aspirin in healthy subjects: recommendations to minimize the functional consequences. Arthritis Rheum 63:850–859
Meek IL, Vonkeman HE, Kasemier J et al (2013) Interference of NSAIDs with the thrombocyte inhibitory effect of aspirin: a placebo-controlled, ex vivo, serial placebo-controlled serial crossover study. Eur J Clin Pharmacol 69:365–371
Li X, Fries S, Li R, Lawson JA, Propert KJ et al (2014) Differential impairment of aspirin-dependent platelet cyclooxygenase acetylation by nonsteroidal antiinflammatory drugs. Proc Natl Acad Sci USA 111:16830–16835
Scheiman JM, Fendrick AM (2007) Summing the risk of NSAID therapy. Lancet 369:1580–1581
Saxena A, Balaramnavar VM, Hohlfeld T, Saxena AK (2013) Drug/drug interaction of common NSAIDs with antiplatelet effect of aspirin in human platelets. Eur J Pharmacol 721:215–224
Nalamachu S, Pergolizzi JV, Raffa RB et al (2014) Drug-drug interaction between NSAIDS and low-dose aspirin: a focus on cardiovascular and GI toxicity. Expert Opin Drug Saf 13:903–917
Fischer LM, Schlienger RG, Matter CM et al (2005) Current use of nonsteroidal antiinflammatory drugs and the risk of acute myocardial infarction. Pharmacotherapy 25:503–510
Hudson M, Baron M, Rahme E et al (2005) Ibuprofen may abrogate the benefits of aspirin when used for secondary prevention of myocardial infarction. J Rheumatol 32:1589–1593
Reed GW, Abdallah M, Shao M et al ( 2017) Effect of aspirin on the cardiovascular, gastrointestinal, and renal safety of celecoxib, naproxen, or ibuprofen. American Heart Association 2017 Scientific Sessions, Anaheim
Feldman M, Cryer B (1999) Aspirin absorption rates and platelet inhibition times with 325-mg buffered aspirin tablets (chewed or swallowed intact) and with buffered aspirin solution. Am J Cardiol 84:404–409
Brown N, May JA, Wilcox RG et al (1999) Comparison of antiplatelet activity of microencapsulated aspirin 162.5 mg (Caspac XL), with enteric coated aspirin 75 mg and 150 mg in patients with atherosclerosis. Br J Clin Pharmacol 48:57–62
Yokoyama H, Yaguchi T, Suzuki Y et al (2012) Theoretical investigation of aspirin dosage regimen to exhibit optimal antiplatelet effects and decrease risk of upper gastrointestinal lesions. Biol Phar Bull 35:2112–2118
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Gurbel reports receiving grants from the National Institutes of Health, Bayer, Medicure, Instrumentation labs, USWorldMeds, Haemonetics, Amgen, Idorsia, Ionis, Janssen, and Merck; receiving honoraria and payment for lectures, consultations including service on speakers’ bureaus from Bayer, Janssen, Merck, UptoDate, and Medicure; and holding patents in the area of personalized antiplatelet therapy and interventional cardiology. Dr. Tantry reports receiving honoraria from Medicure, AstraZeneca and Upto Date. Dr. Weisman is a consultant to Bayer.
Rights and permissions
About this article
Cite this article
Gurbel, P., Tantry, U. & Weisman, S. A narrative review of the cardiovascular risks associated with concomitant aspirin and NSAID use. J Thromb Thrombolysis 47, 16–30 (2019). https://doi.org/10.1007/s11239-018-1764-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-018-1764-5