Abstract
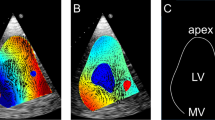
Our institution is developing a non-invasive Diastolic Timed Vibrator (DTV) to enhance emergency clearance of acute coronary thrombosis. Sonic frequency diastolic vibro-percussion (i.e. 50 Hz, 2 mm amplitude) applied upon the rib-spaces of the left sternal border has shown to improve left ventricular performance and coronary flow in human volunteers. However, therapeutic acoustic penetrability cannot be assumed depending on varying chest size and lung position which attenuates acoustic transmissions. Furthermore, chest locations enabling a direct lung free pathway overlying the base of the heart (wherein the coronaries arise) should be promoted, while locations overlying the left ventricular apex (site of potential thrombus formation) should be avoided. We therefore set out to determine preferred chest wall placement positions for a vibratory interface suitable for treatment of ST Elevation Myocardial Infarction (STEMI). Inter-Costal Space (ICS) positions to the left or right of the sternum were interrogated in 90 adults following routine Echocardiography to ascertain whether the base of the heart could be imaged (hence inferring acoustic transmissibility), and to determine over what part of the heart each transducer position was overlying. The third and fourth ICS proximate the left sternal border provided acoustic transmissibility in 96 and 100% of cases respectively, with only one unwanted occurrence from the fourth ICS where the transducer overlaid the apical third of the left ventricle. Acoustic transmissibility from third and fourth ICS right sternal border was documented in 53 and 85% of cases respectively. A vibration interface in STEMI treatment should allow for contact overlying the left and right third and fourth ICS generally proximate the sternal borders. As vibration transmission to the cardiac apex and/or left atrium cannot be completely avoided, vibration therapy should be contra-indicated in late presenters for antero-septal apical STEMI, and in cases of new onset atrial fibrillation persisting greater than 48 h which have not been adequately anti-coagulated.








Similar content being viewed by others
References
Writing Group members et al. (2010) Heart disease and stroke statistics—2010 update a report from the American Heart Association. Circulation 121:e46–e215. doi: 10.1161/CIRCULATIONAHA.109.192667
Lincoff AM, Topol EJ (1993) Illusion of reperfusion. Does anyone achieve optimal reperfusion during acute myocardial infarction? Circulation 88:1361–1374
The American Heart Association’s Acute Myocardial Infarction (AMI) Advisory Working Group, Jacobs AK, Antman EM, Ellrodt G et al (2006) Recommendation to develop strategies to increase the number of ST-segment-elevation myocardial infarction patients with timely access to primary percutaneous coronary intervention. Circulation 113:2152–2163. doi:10.1161/CIRCULATIONAHA.106.174477
Van de Werf F, Ardissino D, Betriu A, Cokkinos DV, Falk E, Fox KA, Julian D, Lengyel M, Neumann FJ, Ruzyllo W, Thygesen C, Underwood SR, Vahanian A, Verheugt FWA, Wijns W (2003) Management of acute myocardial infarction in patients presenting with ST-segment elevation. The Task force on the management of acute myocardial infarction of the European Society of Cardiology. Eur Heart J 24:28–66. doi:10.1016/S0195-668X(02)00618-8
GUSTO The investigators (1993) An international randomized trial comparing four thrombolytic strategies for acute myocardial infarction. N Engl J Med 329:673–682. doi:10.1056/NEJM199309023291001
Siegel R, Luo H (2008) Ultrasound Thrombolysis. Ultrasonics 48(4): 312–320 (Epub 2008 March 28). doi:10.1016/j.ultras.2008.03.010
Yohannes FG, Hoffmann AK (2008) Non-invasive low frequency vibration as a potential adjunctive treatment for heart attack and stroke an in vitro flow model. J Thromb Thrombolysis 25(3):251–258
Thomas J, Cook DJ, Brooks D (1995) Chest physical therapy management of patients with cystic fibrosis: a meta analysis. Am J Respir Crit Care Med 151:846–850
Koiwa Y, Hashiguchi R, Ohyama T et al (1986) Measurement of instantaneous viscoelastic properties by impedance-frequency curve of the ventricle. Am J Physiol 250:H672–H684
Hashiguchi R, Koiwa Y, Ohyama T et al (1988) Dependence of instantaneous transfer function on regional ischemic myocardial volume. Circ Res 63:1003–1011
Smith D, Ishimitsu T, Craige E (1984) Mechanical vibration transmission characteristics of the left ventricle Implication with regard to auscultation and phonocardiography. J Am Coll Cordiol 4(3):517–521
Farber JJ, Purvis JH (1963) Conduction of cardiovascular sound along arteries. Circ Res 12:308–316
Koiwa Y et al (1996) Precordial or epicardial input of phase-controlled minute vibration: effect on coronary flow rate in regional ischemia. In: Sasayama S (ed) New horizons for failing heart syndrome. Springer-Verlag, Tokyo, pp 117–130
Koiwa Y, Honda H, Takagi T, Kikuchi J, Hoshi N, Takishima T (1997) Modification of human left ventricular relaxation by small-amplitude, phase–controlled mechanical vibration on the chest wall. Circulation 95:156–162
Takagi T, Koiwa Y, Kikuchi J et al (1992) Diastolic vibration improves systolic function in cases of incomplete relaxation. Circulation 86:1955–1964
Dubrul WR, Evans MA (2001) Motion catheter. US Patent 6,287,271
Arko F, Davis C, Murphy E, Smith S, Timaran C, Modrall G, Valentine R, Clagett G (2007) Aggressive percutaneous mechanical thrombectomy of deep venous thrombosis. Arch Surg 142:513–519
Greaves et al (1997) Incidence and Natural History of Left Ventricular Thrombus Following Anterior Wall Acute Myocardial Infarction. Am J Cardiol 80:442–448
Hoffmann A, Gill H (2010) The Timing of onset of mechanical systole and diastole in reference to the QRS-T complex: a study to determine performance criteria for a non-invasive diastolic timed vibration massage system in treatment of potentially unstable cardiac disorders. Cardiovasc Eng 10:235–245. doi:10.1007/s10558-010-9108-x
Zaidi SA, Marzencki M, Menon C, Kaminska B (2010) Non-invasive method for pre-hospitalization treatment of heart attack patients. In: The 3rd international multi-conference on engineering and technological innovation (IMETI), Orlando, USA
Disclaimer
The Author’s caution the public that the technique of using a low frequency vibrator applied to the upper torso in treatment of heart attack is purely experimental and still requiring clinical trials, and hence cannot be warranted at this time for safe clinical use.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure: Various patents and patents pending relating to use of low frequency vibration to assist thrombolysis in the setting of acute arterial thrombosis, including preferred vibration chest wall vibratory interfaces, are owned and controlled by Simon Fraser University in a revenue sharing partnership with Ahof Biophysical Systems Inc. The novel engineering concepts disclosed in this article have been published in patent application(s) prior to the submission and publication date of this article.
Rights and permissions
About this article
Cite this article
Hoffmann, A.K., Gill, H. A study to determine chest wall vibratory attachment interface locations for a low frequency sonic vibrator in treatment of acute coronary thrombosis. J Thromb Thrombolysis 32, 167–176 (2011). https://doi.org/10.1007/s11239-011-0589-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-011-0589-2