Abstract
Objectives
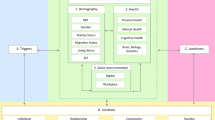
To develop a measure of natural environment and human-made change features (Chapter 2 of the international classification of functioning, disability, and health) and evaluate the influence of perceived barriers on health-related quality of life.
Methods
A sample of 570 adults with stroke, spinal cord injury, and traumatic brain injury residing in community settings reported their functioning in home, outdoor, and community settings (mean age = 47.0 years, SD = 16.1). They rated 18 items with a 5-point rating scale to describe the influence of barriers to moving around, seeing objects, hearing sounds, hearing conversations, feeling safe, and regulating temperature and indicated whether any difficulties were due to environmental features. We used Rasch analysis to identify misfitting items and evaluate differential item functioning (DIF) across impairment groups. We computed correlations between barriers and patient-reported outcomes measurement information system (PROMIS) social domain measures and community participation indicators (CPI) measures.
Results
The 18 items demonstrated person reliability of .70, discriminating nearly three levels of barriers. All items fit the Rasch model; impairment-related DIF was negligible. Ceiling effects were negligible, but 25 % of the respondents were at the floor, indicating that they did not experience barriers that they attributed to the built and natural environment. As anticipated, barriers correlated moderately with PROMIS and CPI variables, suggesting that although this new item bank measures a construct that is related to participation and health-related quality of life, it also captures something unique. Known-groups validity was supported by wheelchair users reporting a higher level of barriers than did ambulatory respondents.
Conclusions
Preliminary evidence supports the reliability and validity of this new measure of barriers to the built and natural environment. This measure allows investigators and clinicians to measure perceptions of the natural environment and human-made changes, providing information that can guide interventions to reduce barriers. Moderate relationships between barriers and PROMIS and CPI variables provide support for the measurement and theory of environmental influences on social health and participation.




Similar content being viewed by others
References
Field, M. J., & Jette, A. (2007). The future of disability in America. Washington, DC: National Academies Press.
United Nations General Assembly. (2003). Final report of the Ad Hoc Committee on a comprehensive and integral international convention on the protection and promotion of the rights and dignity of persons with disabilities. http://www.un.org/disabilities/convention/conventionfull.shtml.
Wright, B. (1983). Physical disability: A psychosocial approach. New York: Harper and Row.
Albrecht, G. L., Seelman, K. T., & Bury, M. (2001). Handbook of disability studies. Thousand Oaks, CA: Sage Publications.
Commission on Social Determinants of Health. (2013). Closing the gap in a generation: Health equity through action on the social determinants of health. Geneva: World Health Organisation.
Lawton, M. P., & Nahemow, L. (1973). Ecology and the aging process. In M. P. Eisdorfer (Ed.), The psychology of adult development and aging (pp. 619–674). Washington, DC: American Psychological Association.
Lewin, K. (1951). Field theory in social science. New York: Harper.
Marmot, M., et al. (2008). Closing the gap in a generation: Health equity through action on the social determinants of health. The Lancet, 372(9650), 1661–1669.
Dickinson, H. O., & Colver, A. F. (2010). Measurement of the environment of people with disabilities. Archives of Physical Medicine and Rehabilitation, 91(8), 1310–1311.
World Health Organization. (2001). International classification of functioning, disability and health (pp. 1–303). Geneva: World Health Organization.
Levasseur, M., Desrosiers, J., & St-Cyr, T. D. (2007). Comparing the disability creation process and international classification of functioning, disability and health models. Canadian Journal of Occupational Therapy, 74(3 suppl), 233–242.
Cerniauskaite, M., et al. (2011). Systematic literature review on ICF from 2001 to 2009: its use, implementation and operationalisation. Disability and Rehabilitation, 33(4), 281–309.
Schneidert, M., et al. (2003). The role of environment in the international classification of functioning, disability and health (ICF). Disability and Rehabilitation, 25(11–12), 588–595.
Alvarelhão, J., et al. (2012). Comparing the content of instruments assessing environmental factors using the international classification of functioning, disability and health. Journal of Rehabilitation Medicine, 44(1), 1–6.
Hammel, J., et al. (2015). Environmental barriers and supports to everyday participation: A qualitative insider perspective from people with disabilities. Archives of Physical Medicine and Rehabilitation, 96(4), 578–588.
Choppin, B. (1968). Item bank using sample-free calibration. Nature, 219(5156), 870–872.
Choppin, B. (1981). Educational measurement and the item bank model. In: C. Lacey & D. Lawton (Eds.), Issues in evaluation and accountability (pp. 204–221). England: Methuen.
Donnan, G. A., et al. (2008). Stroke. Lancet, 371(9624), 1612–1623.
Coffey, C. E., & Cummings, J. L. (2000). The American Psychiatric Press textbook of geriatric neuropsychiatry. Washington, DC: American Psychiatric Press.
Centers for Disease Control and Prevention. (2015). Report to congress on traumatic brain injury in the United States: Epidemiology and rehabilitation. Atlanta, GA: National Center for Injury Prevention and Control.
National Spinal Cord Injury Statistical Center. (2015). Facts and figures at a glance. Birmingham, AL: University of Alabama.
Hollingsworth, H., & Gray, D. B. (2010). Structural equation modeling of the relationships between participation in leisure activities and community environments by people with mobility impairments. Archives of Physical Medicine and Rehabilitation, 91(8), 1174–1181.
Clarke, P., et al. (2008). Mobility disability and the urban built environment. American Journal of Epidemiology, 168(5), 506–513.
Gray, D. B., Gould, M., & Bickenbach, J. E. (2003). Environmental barriers and disability. Journal of Architectural and Planning Research, 20, 29–37.
Bricout, J. C., & Gray, D. B. (2006). Community receptivity: The ecology of disabled persons’ participation in the physical, political and social environments. Scandinavian Journal of Disability Research, 8(1), 1–21.
Alvarelhao, J., et al. (2012). Comparing the content of instruments assessing environmental factors using the international classification of functioning, Disability and Health. Journal of Rehabilitation Medicine, 44(1), 1–6.
Stark, S., et al. (2007). Development of a measure of receptivity of the physical environment. Disability and Rehabilitation, 29(2), 123–137.
Reeve, B. B., et al. (2007). Psychometric evaluation and calibration of health-related quality of life item banks: plans for the patient-reported outcomes measurement information system (PROMIS). Medical Care, 45(5 Suppl 1), S22–S31.
Velozo, C. A., et al. (2012). Improving measurement methods in rehabilitation: Core concepts and recommendations for scale development. Archives of Physical Medicine and Rehabilitation, 93(8 Suppl), S154–S163.
Tulsky, D. S., et al. (2015). Developing an item bank to measure economic quality of life for individuals with disabilities. Archives of Physical Medicine and Rehabilitation, 96(4), 604–613.
Garcia, S. F., et al. (2015). Development of self-report measures of social attitudes that act as environmental barriers and facilitators for people with disabilities. Archives of Physical Medicine and Rehabilitation, 96(4), 596–603.
Heinemann, A. W., et al. (2015). Environmental factors item development for persons with stroke, traumatic brain injury, and spinal cord injury. Archives of Physical Medicine and Rehabilitation, 96(4), 589–595.
Hammel, J., et al. (2015). Environmental barriers and supports to everyday participation: a qualitative insider perspective from people with disabilities. Archives of Physical Medicine and Rehabilitation, 96(4), 578–588.
Magasi, S., et al. (2015). Theoretical foundations for the measurement of environmental factors and their impact on participation among people with disabilities. Archives of Physical Medicine and Rehabilitation, 96(4), 569–577.
Bailey, I. L., & Lovie, J. E. (1976). New design principles for visual acuity letter charts. The American Journal of Optometry and Physiol Optometry, 53(11), 740–745.
Wilkinson, G. S., & Robertson, G. J. (2006). WRAT4: Wide range achievement test. Lutz, FL: Psychological Assessment Resources.
Enderby, P. M., Wood, V. A., Wade, D. T., & Hewer, R. L. (1986). The Frenchay Aphasia Screening Test: A short, simple test for aphasia appropriate for non-specialists. Disability and Rehabilitation, 8(4), 166–170.
DeWalt, D. A., et al. (2007). Evaluation of item candidates: The PROMIS qualitative item review. Medical Care, 45(5 Suppl 1), S12–S21.
Cieza, A., et al. (2005). ICF linking rules: An update based on lessons learned. Journal of Rehabilitation Medicine, 37(4), 212–218.
Heinemann, A. W., et al. (2013). Measuring enfranchisement: Importance of and control over participation by people with disabilities. Archives of Physical Medicine and Rehabilitation, 94(11), 2157–2165.
Hammel, J., Magasi, S., Heinemann, A. W., Whiteneck, G., Bogner, J., & Rodriguez, E. (2008). What does participation mean? An insider perspective from people with disabilities. Disability and Rehabilitation, 30(19), 1445–1460.
Magasi, S., et al. (2009). Participation: A comparative analysis of multiple rehabilitation stakeholders’ perspectives. Journal of Rehabilitation Medicine, 41(11), 936–944.
Hahn, E. A., et al. (2014). New English and Spanish social health measures will facilitate evaluating health determinants. Health Psychology, 33(5), 490–499.
Fisher, W. P. J. (2007). Rating scale instrument quality criteria. Rasch Measurement Transactions, 21(1), 1095.
Baker, F. (2001). The basics of item response theory, ERIC clearinghouse on assessment and evaluation. College Park, MD: University of Maryland.
Lai, J.-S., Butt, Z., Zelko, F., Cella, D., Krull, K., Kieran, M., & Goldman, S. (2011). Development of a parent-reported cognitive function item bank using item response theory and exploration of its clinical utility in computerized adaptive testing. Journal of Pediatric Psychology, 36(7), 766–779.
Linacre, J. M. (2016). WINSTEPS: Rasch measurement computer program. 3.91.0 ed. Beaverton, Oregon: Winsteps.com.
Terwee, C. B., et al. (2007). Quality criteria were proposed for measurement properties of health status questionnaires. Journal of Clinical Epidemiology, 60(1), 34–42.
Fisher, W. P. Jr. (1992). Reliability, separation, strata statistics. Rasch Measurement Transactions, 6, 238.
Magasi, S., et al. (2015). Theoretical foundations for the measurement of environmental factors and their impact on participation among people with disabilities. Archives of Physical Medicine and Rehabilitation, 96(4), 569–577.
Reeve, B. B., et al. (2007). Psychometric evaluation and calibration of health-related quality of life item banks: Plans for the patient-reported outcomes measurement information system (PROMIS). Medical Care, 45(5), S22–S31.
Whiteneck, G., & Dijkers, M. P. (2009). Difficult to measure constructs: Conceptual and methodological issues concerning participation and environmental factors. Archives of Physical Medicine and Rehabilitation, 90(11 Suppl), S22–S35.
Funding
This study was funded by the National Institute on Disability, Independent Living, and Rehabilitation Research (H133B090024) through a Rehabilitation Research and Training Center on Improving Measurement of Medical Rehabilitation Outcomes grant awarded to the Rehabilitation Institute of Chicago. The National Institute on Disability, Independent Living, and Rehabilitation Research (H133F140037) and Craig H. Neilsen Foundation (290474) supported a portion of Alex Wong’s effort.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
All participants included in the study provided informed consent.
Additional information
Suppliers: Winsteps - Multiple-Choice, Rating Scale, and Partial Credit Rasch Analysis. www.winsteps.com/index.htm.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Heinemann, A.W., Lai, JS., Wong, A. et al. Using the ICF’s environmental factors framework to develop an item bank measuring built and natural environmental features affecting persons with disabilities. Qual Life Res 25, 2775–2786 (2016). https://doi.org/10.1007/s11136-016-1314-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-016-1314-6