Abstract
Purpose
To identify and develop a conceptual map of prioritized areas and to determine their relative importance for outcome measurement in clinical Parkinson’s disease (PD) trials, from the perspectives of health care professionals and people with PD.
Method
We used concept mapping, a qualitative/quantitative method consisting of three steps: item generation through focus groups (n = 27; 12 people with PD, 12 health care professionals, 3 researchers), item sorting and rating (n = 38; 19 people with PD, 19 health care professionals), and data analysis (multidimensional scaling, cluster analysis).
Results
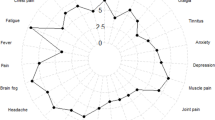
Ninety-nine items and eight clusters were generated. Clusters representing Participation; Mobility and motor functioning; Cognitive and executive functioning; and Emotions were the most homogenous. Statements within clusters representing Energy and abilities; Autonomic dysfunctions; Sensory, speech and swallowing problems; and Neuropsychiatric symptoms also related to statements outside their respective clusters. Clusters rated most important were Participation and Mobility and motor functioning, and the highest rated items were quality of life, walking ability, and sleeping problems.
Conclusion
By the use of concept mapping, a multi-perspective conceptual map of prioritized aspects for the outcome measurement in PD was defined. These findings provide an initial conceptual basis toward improved outcome measurement priorities in clinical PD trials.


Similar content being viewed by others
References
Lees, A. J., Hardy, J., & Revesz, T. (2009). Parkinson’s disease. Lancet, 373(9680), 2055–2066.
Chaudhuri, K. R., Healy, D. G., & Schapira, A. H. (2006). Non-motor symptoms of Parkinson’s disease: Diagnosis and management. Lancet Neurology, 5(3), 235–245.
Karlsen, K. H., Larsen, J. P., Tandberg, E., & Maeland, J. G. (1999). Influence of clinical and demographic variables on quality of life in patients with Parkinson’s disease. Journal of Neurology, Neurosurgery and Psychiatry, 66(4), 431–435.
Soh, S. E., Morris, M. E., & McGinley, J. L. (2011). Determinants of health-related quality of life in Parkinson’s disease: A systematic review. Parkinsonism and Related Disorders, 17(1), 1–9.
Gruber-Baldini, A. L., Ye, J., Anderson, K. E., & Shulman, L. M. (2009). Effects of optimism/pessimism and locus of control on disability and quality of life in Parkinson’s disease. Parkinsonism and Related Disorders, 15(9), 665–669.
Koplas, P. A., Gans, H. B., Wisely, M. P., Kuchibhatla, M., Cutson, T. M., Gold, D. T., et al. (1999). Quality of life and Parkinson’s disease. Journals of Gerontology. Series A, Biological Sciences and Medical Sciences, 54(4), M197–M202.
Wallhagen, M. I., & Brod, M. (1997). Perceived control and well-being in Parkinson’s disease. Western Journal of Nursing Research, 19(1), 11–25. (discussion 25–31).
Charlton, G. S., & Barrow, C. J. (2002). Coping and self-help group membership in Parkinson’s disease: An exploratory qualitative study. Health & Social Care in the Community, 10(6), 472–478.
Andersson, I., & Sidenvall, B. (2001). Case studies of food shopping, cooking and eating habits in older women with Parkinson’s disease. Journal of Advanced Nursing, 35(1), 69–78.
Keller, H. H., Edward, H. G., & Cook, C. (2006). Mealtime experiences of families with dementia. American Journal of Alzheimers Disease and Other dementias, 21(6), 431–438.
Lim, A., Leow, L., Huckabee, M. L., Frampton, C., & Anderson, T. (2008). A pilot study of respiration and swallowing integration in Parkinson’s disease: “On” and “off” levodopa. Dysphagia, 23(1), 76–81.
Miller, N., Noble, E., Jones, D., & Burn, D. (2006). Hard to swallow: Dysphagia in Parkinson’s disease. Age and Ageing, 35(6), 614–618.
Low, J. (2006). Communication problems between researchers and informants with speech difficulties: Methodological and analytic issues. Field Methods, 18(2), 153–171.
Hobart, J. C., Cano, S. J., Zajicek, J. P., & Thompson, A. J. (2007). Rating scales as outcome measures for clinical trials in neurology: Problems, solutions, and recommendations. Lancet Neurology, 6(12), 1094–1105.
Mitchell, S. L., Harper, D. W., Lau, A., & Bhalla, R. (2000). Patterns of outcome measurement in Parkinson’s disease clinical trials. Neuroepidemiology, 19(2), 100–108.
Chalmers, I. (2007). The Alzheimer’s society, drug firms, and public trust. BMJ, 335, 400.
Food and Drug Administration. (2009). Patient-reported outcome measures: Use in medicinal product development to support labelling claims. Washington, DC.
Nisenzon, A. N., Robinson, M. E., Bowers, D., Banou, E., Malaty, I., & Okun, M. S. (2011). Measurement of patient-centered outcomes in Parkinson’s disease: What do patients really want from their treatment? Parkinsonism and Related Disorders, 17(2), 89–94.
Kane, M., & Trochim, W. M. K. (2007). Concept mapping for planning and evaluation. Thousand Oaks: Sage Publications, Inc.
Trochim, W. M. K. (1989). An introduction to concept mapping for planning and evaluation. Evaluation and Program Planning, 12(1), 1–16.
Akhtar-Danesh, N., Baumann, A., & Cordingley, L. (2008). Q-methodology in nursing research: A promising method for the study of subjectivity. Western Journal of Nursing Research, 30(6), 759–773.
Patton, M. Q. (2002). Qualitative evaluation and research methods (3rd ed.). Thousand Oaks: Sage Publications.
Hoehn, M. M., & Yahr, M. D. (1967). Parkinsonism: Onset, progression and mortality. Neurology, 17(5), 427–442.
Goetz, C. G., Poewe, W., Rascol, O., Sampaio, C., Stebbins, G. T., Counsell, C., et al. (2004). Movement Disorder Society Task Force report on the Hoehn and Yahr Staging Scale: Status and recommendations. Movement Disorders, 19(9), 1020–1028.
Hagell, P., & Sandlund, B. (2000). Patients’ self-assessment of disease and symptom severity in Parkinson’s disease. Quality of Life Research, 9(3), 285.
Hobson, J. P., Edwards, N. I., & Meara, R. J. (2001). The Parkinson’s Disease Activities of Daily Living Scale: A new simple and brief subjective measure of disability in Parkinson’s disease. Clinical Rehabilitation, 15(3), 241–246.
Severens, P. (1995). Handbook: Concept mapping. Amsterdam: National Centre for Mental Health/Talcott BV.
Knutsson, I., Rydstrom, H., Reimer, J., Nyberg, P., & Hagell, P. (2010). Interpretation of response categories in patient-reported rating scales: A controlled study among people with Parkinson’s disease. Health and Quality of Life Outcomes, 8, 61.
Trochim, W. M., Stillman, F. A., Clark, P. I., & Schmitt, C. L. (2003). Development of a model of the tobacco industry’s interference with tobacco control programmes. Tobacco Control, 12(2), 140–147.
Rahman, S., Griffin, H. J., Quinn, N. P., & Jahanshahi, M. (2008). Quality of life in Parkinson’s disease: The relative importance of the symptoms. Movement Disorders, 23(10), 1428–1434.
Friedman, J. H., Brown, R. G., Comella, C., Garber, C. E., Krupp, L. B., Lou, J. S., et al. (2007). Fatigue in Parkinson’s disease: A review. Movement Disorders, 22(3), 297–308.
Peto, V., Jenkinson, C., Fitzpatrick, R., & Greenhall, R. (1995). The development and validation of a short measure of functioning and well being for individuals with Parkinson’s disease. Quality of Life Research, 4(3), 241–248.
Ware, J. E., Jr., & Sherbourne, C. D. (1992). The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Medical Care, 30(6), 473–483.
Hagell, P., Reimer, J., & Nyberg, P. (2009). Whose quality of life? Ethical implications in patient-reported health outcome measurement. Value Health, 12(4), 613–617.
Lee, M. A., Walker, R. W., Hildreth, A. J., & Prentice, W. M. (2006). Individualized assessment of quality of life in idiopathic Parkinson’s disease. Movement Disorders, 21(11), 1929–1934.
Osborne, R. H., Elsworth, G. R., & Whitfield, K. (2007). The Health Education Impact Questionnaire (heiQ): An outcomes and evaluation measure for patient education and self-management interventions for people with chronic conditions. Patient Education and Counseling, 66(2), 192–201.
Acknowledgments
The authors wish to thank all participants for their cooperation, J. Reimer, S. Lindskov, and K. Wictorin for assistance in recruiting participants, and M. Miller and S. Smith for valuable discussions. The study was conducted within the BAGADILICO (the Basal Ganglia Disorders Linnaeus Consortium) research group at Lund University, Sweden. The study was supported by the Swedish Research Council, the Swedish Parkinson Academy, and the Faculty of Medicine at Lund University, Lund, Sweden. MHN was partly funded by the Strategic Research Area MultiPark at Lund University, and by the Swedish Council for Working Life and Social Research within the context of the Centre for Ageing and Supportive Environments (CASE), Lund University, Sweden.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sjödahl Hammarlund, C., Nilsson, M.H. & Hagell, P. Measuring outcomes in Parkinson’s disease: a multi-perspective concept mapping study. Qual Life Res 21, 453–463 (2012). https://doi.org/10.1007/s11136-011-9995-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-011-9995-3