ABSTRACT
Purpose
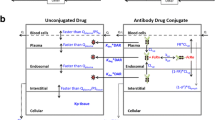
THIOMAB™ drug conjugates (TDCs) with engineered cysteine residues allow site-specific drug conjugation and defined Drug-to-Antibody Ratios (DAR). In order to help elucidate the impact of drug-loading, conjugation site, and subsequent deconjugation on pharmacokinetics and efficacy, we have developed an integrated mathematical model to mechanistically characterize pharmacokinetic behavior and preclinical efficacy of MMAE conjugated TDCs with different DARs. General applicability of the model structure was evaluated with two different TDCs.
Method
Pharmacokinetics studies were conducted for unconjugated antibody and purified TDCs with DAR-1, 2 and 4 for trastuzumab TDC and Anti-STEAP1 TDC in mice. Total antibody concentrations and individual DAR fractions were measured. Efficacy studies were performed in tumor-bearing mice.
Results
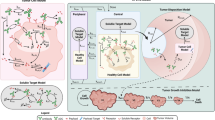
An integrated model consisting of distinct DAR species (DAR0-4), each described by a two-compartment model was able to capture the experimental data well. Time series measurements of each Individual DAR species allowed for the incorporation of site-specific drug loss through deconjugation and the results suggest a higher deconjugation rate from heavy chain site HC-A114C than the light chain site LC-V205C. Total antibody concentrations showed multi-exponential decline, with a higher clearance associated with higher DAR species. The experimentally observed effects of TDC on tumor growth kinetics were successfully described by linking pharmacokinetic profiles to DAR-dependent killing of tumor cells.
Conclusion
Results from the integrated model evaluated with two different TDCs highlight the impact of DAR and site of conjugation on pharmacokinetics and efficacy. The model can be used to guide future drug optimization and in-vivo studies.





Similar content being viewed by others
REFERENCES
Senter PD. Potent antibody drug conjugates for cancer therapy. Curr Opin Chem Biol. 2009;13:235–44.
Ballantyneand A, Dhillon S. Trastuzumab emtansine: first global approval. Drugs. 2013;73:755–65.
Singhand R, Erickson HK. Antibody-cytotoxic agent conjugates: preparation and characterization. Methods Mol Biol. 2009;525:445–67. xiv.
Carterand PJ, Senter PD. Antibody-drug conjugates for cancer therapy. Cancer J. 2008;14:154–69.
Schrama D, Reisfeld RA, Becker JC. Antibody targeted drugs as cancer therapeutics. Nat Rev Drug Discov. 2006;5:147–59.
Boswell CA, Mundo EE, Zhang C, Bumbaca D, Valle NR, Kozak KR, et al. Impact of drug conjugation on pharmacokinetics and tissue distribution of anti-STEAP1 antibody-drug conjugates in rats. Bioconjug Chem. 2011;22:1994–2004.
Linand K, Tibbitts J. Pharmacokinetic considerations for antibody drug conjugates. Pharm Res. 2012;29:2354–66.
Hamblett KJ, Senter PD, Chace DF, Sun MM, Lenox J, Cerveny CG, et al. Effects of drug loading on the antitumor activity of a monoclonal antibody drug conjugate. Clin Cancer Res. 2004;10:7063–70.
Junutula JR, Raab H, Clark S, Bhakta S, Leipold DD, Weir S, et al. Site-specific conjugation of a cytotoxic drug to an antibody improves the therapeutic index. Nat Biotechnol. 2008;26:925–32.
Behrensand, CR, Liu B. Methods for site-specific drug conjugation to antibodies. MAbs. 2013; 6.
Shen BQ, Xu K, Liu L, Raab H, Bhakta S, Kenrick M, et al. Conjugation site modulates the in vivo stability and therapeutic activity of antibody-drug conjugates. Nat Biotechnol. 2012;30:184–9.
Junutula JR, Bhakta S, Raab H, Ervin KE, Eigenbrot C, Vandlen R, et al. Rapid identification of reactive cysteine residues for site-specific labeling of antibody-Fabs. J Immunol Methods. 2008;332:41–52.
Alley SC, Benjamin DR, Jeffrey SC, Okeley NM, Meyer DL, Sanderson RJ, et al. Contribution of linker stability to the activities of anticancer immunoconjugates. Bioconjug Chem. 2008;19:759–65.
Xu K, Liu L, Saad OM, Baudys J, Williams L, Leipold D, et al. Characterization of intact antibody-drug conjugates from plasma/serum in vivo by affinity capture capillary liquid chromatography-mass spectrometry. Anal Biochem. 2011;412:56–66.
Chudasama VL, Schaedeli Stark F, Harrold JM, Tibbitts J, Girish SR, Gupta M, et al. Semi-mechanistic population pharmacokinetic model of multivalent trastuzumab emtansine in patients with metastatic breast cancer. Clin Pharmacol Ther. 2012;92:520–7.
Shah DK, Haddish-Berhane N, Betts A. Bench to bedside translation of antibody drug conjugates using a multiscale mechanistic PK/PD model: a case study with brentuximab-vedotin. J Pharmacokinet Pharmacodyn. 2012;39:643–59.
Wang W, Wang EQ, Balthasar JP. Monoclonal antibody pharmacokinetics and pharmacodynamics. Clin Pharmacol Ther. 2008;84:548–58.
Koch G, Walz A, Lahu G, Schropp J. Modeling of tumor growth and anticancer effects of combination therapy. J Pharmacokinet Pharmacodyn. 2009;36:179–97.
Simeoni M, Magni P, Cammia C, De Nicolao G, Croci V, Pesenti E, et al. Predictive pharmacokinetic-pharmacodynamic modeling of tumor growth kinetics in xenograft models after administration of anticancer agents. Cancer Res. 2004;64:1094–101.
Doronina SO, Toki BE, Torgov MY, Mendelsohn BA, Cerveny CG, Chace DF, et al. Development of potent monoclonal antibody auristatin conjugates for cancer therapy. Nat Biotechnol. 2003;21:778–84.
Bhakta S, Raab H, Junutula JR. Engineering THIOMABs for site-specific conjugation of thiol-reactive linkers. Methods Mol Biol. 2013;1045:189–203.
King HD, Yurgaitis D, Willner D, Firestone RA, Yang MB, Lasch SJ, et al. Monoclonal antibody conjugates of doxorubicin prepared with branched linkers: a novel method for increasing the potency of doxorubicin immunoconjugates. Bioconjug Chem. 1999;10:279–88.
ACKNOWLEDGMENTS AND DISCLOSURES
The authors would like to thank Paul J. Fielder and other PKPD colleagues for their constructive input to this work.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOCX 219 kb)
Rights and permissions
About this article
Cite this article
Sukumaran, S., Gadkar, K., Zhang, C. et al. Mechanism-Based Pharmacokinetic/Pharmacodynamic Model for THIOMAB™ Drug Conjugates. Pharm Res 32, 1884–1893 (2015). https://doi.org/10.1007/s11095-014-1582-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-014-1582-1