Abstract
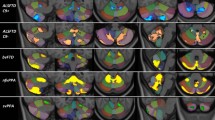
Frontotemporal dementia (FTD) is a neurodegenerative brain disorder primarily affecting the frontal and/or temporal lobes. Three main subtypes have been recognized: behavioural-variant FTD (bvFTD), semantic dementia (SD), and progressive nonfluent aphasia (PNFA), each of which has a distinct clinical and cognitive profile. Although the role of the cerebellum in cognition is increasingly accepted, knowledge of cerebellar changes across neuroimaging modalities and their contribution to behavioural and cognitive changes in FTD syndromes is currently scant. We conducted an anatomical/activation likelihood estimation (ALE) meta-analysis in 53 neuroimaging studies (structural MRI: 42; positron emission tomography: 6; functional MRI: 4; single-photon emission computed tomography: 1) to identify the patterns of cerebellar changes and their relations to profiles of behavioural and cognitive deficits in FTD syndromes. Overall, widespread bilateral cerebellar changes were found in FTD and notably the patterns were subtype specific. In bvFTD, ALE peaks were identified in the bilateral Crus, left lobule VI, right lobules VIIb and VIIIb. In SD, focal cerebellar changes were located in the left Crus I and lobule VI. A separate ALE meta-analysis on PNFA studies was not performed due to the limited number of studies available. In addition, the ALE analysis indicated that bilateral Crus I and Crus II were associated with behavioural disruption and cognitive dysfunction. This ALE meta-analysis provides the quantification of the location and extent of cerebellar changes across the main FTD syndromes, which in turn provides evidence of cerebellar contributions to behavioural and cognitive changes in FTD. These results bring new insights into the mechanisms mediating FTD symptomatology.


Similar content being viewed by others
References
References Marked with an Asterisk Indicate Studies Included in the Meta-Analysis
Acar, F., Seurinck, R., Eickhoff, S. B., & Moerkerke, B. (2018). Assessing robustness against potential publication bias in activation likelihood estimation (ALE) meta-analyses for fMRI. PLoS One, 13(11), e0208177. https://doi.org/10.1371/journal.pone.0208177
Addis, D. R., Moloney, E. E., Tippett, L. J., & Hach, S. (2016). Characterizing cerebellar activity during autobiographical memory retrieval: ALE and functional connectivity investigations. Neuropsychologia, 90, 80–93. https://doi.org/10.1016/j.neuropsychologia.2016.05.025
*Ahmed, R. M., Irish, M., Henning, E., Dermody, N., Bartley, L., Kiernan, M. C., Piguet O., Farooqi S., Hodges J. R. (2016). Assessment of eating behavior disturbance and associated neural networks in frontotemporal dementia. JAMA Neurology, 73(3), 282–290, doi:https://doi.org/10.1001/jamaneurol.2015.4478.
*Amanzio, M., D'Agata, F., Palermo, S., Rubino, E., Zucca, M., Galati, A., et al. (2016). Neural correlates of reduced awareness in instrumental activities of daily living in frontotemporal dementia. Experimental Gerontology, 83, 158–164, doi:https://doi.org/10.1016/j.exger.2016.08.008.
Andreasen, N. C., & Pierson, R. (2008). The role of the cerebellum in schizophrenia. Biological Psychiatry, 64(2), 81–88. https://doi.org/10.1016/j.biopsych.2008.01.003
Belzil, V. V., Bauer, P. O., Prudencio, M., Gendron, T. F., Stetler, C. T., Yan, I. K., … Petrucelli, L. (2013). Reduced C9orf72 gene expression in c9FTD/ALS is caused by histone trimethylation, an epigenetic event detectable in blood. Acta Neuropathologica, 126(6), 895–905. https://doi.org/10.1007/s00401-013-1199-1
Bernard, J. A., & Mittal, V. A. (2015). Dysfunctional activation of the cerebellum in schizophrenia: A functional neuroimaging meta-analysis. Clinical Psychological Science: A Journal of the Association for Psychological Science, 3(4), 545–566. https://doi.org/10.1177/2167702614542463
*Bertoux, M. F.;Hobbs, M.;Ruiz-Tagle, A.;Delgado, C.;Miranda, M.;Ibanez, A.;Slachevsky, A.;Hornberger, M. (2018). Structural anatomical investigation of long-term memory deficit in behavioral frontotemporal dementia. Journal of Alzheimer's Disease, 62(4), 1887–1900, doi:https://doi.org/10.3233/jad-170771.
Boeve, B. F., Boylan, K. B., Graff-Radford, N. R., DeJesus-Hernandez, M., Knopman, D. S., Pedraza, O., … Rademakers, R. (2012). Characterization of frontotemporal dementia and/or amyotrophic lateral sclerosis associated with the GGGGCC repeat expansion in C9ORF72. Brain, 135(Pt 3), 765–783. https://doi.org/10.1093/brain/aws004
Bossier, H., Seurinck, R., Kuhn, S., Banaschewski, T., Barker, G. J., Bokde, A. L. W., et al. (2017). The influence of study-level inference models and study set size on coordinate-based fMRI meta-analyses. Frontiers in Neuroscience, 11, 745. https://doi.org/10.3389/fnins.2017.00745
*Chen, Y., Kumfor, F., Landin-Romero, R., Irish, M., Hodges, J. R., & Piguet, O. (2018). Cerebellar atrophy and its contribution to cognition in frontotemporal dementias. Annals of Neurology, 84(1), 98–109, doi:https://doi.org/10.1002/ana.25271.
Cheng, D. T., Meintjes, E. M., Stanton, M. E., Dodge, N. C., Pienaar, M., Warton, C. M. R., … Jacobson, S. W. (2017). Functional MRI of human Eyeblink classical conditioning in children with fetal alcohol Spectrum disorders. Cerebral Cortex, 27(7), 3752–3767. https://doi.org/10.1093/cercor/bhw273
*Cistaro, A., Pagani, M., Montuschi, A., Calvo, A., Moglia, C., Canosa, A., Restagno G., Brunetti M., Traynor B. J., Nobili F., Carrara G., Fania P., Lopiano L., Valentini M. C., Chiò A. (2014). The metabolic signature of C9ORF72-related ALS: FDG PET comparison with nonmutated patients. European Journal of Nuclear Medicine and Molecular Imaging, 41(5), 844–852, doi:https://doi.org/10.1007/s00259-013-2667-5.
Colloby, S. J., O'Brien, J. T., & Taylor, J. P. (2014). Patterns of cerebellar volume loss in dementia with Lewy bodies and Alzheimers disease: A VBM-DARTEL study. Psychiatry Research, 223(3), 187–191. https://doi.org/10.1016/j.pscychresns.2014.06.006
Coyle-Gilchrist, I. T., Dick, K. M., Patterson, K., Vazquez Rodriquez, P., Wehmann, E., Wilcox, A., et al. (2016). Prevalence, characteristics, and survival of frontotemporal lobar degeneration syndromes. Neurology, 86(18), 1736–1743. https://doi.org/10.1212/WNL.0000000000002638
de Azevedo, P. C., Guimaraes, R. P., Piccinin, C. C., Piovesana, L. G., Campos, L. S., Zuiani, J. R., et al. (2017). Cerebellar Gray Matter Alterations in Huntington Disease: A Voxel-Based Morphometry Study. In Cerebellar gray matter alterations in Huntington. Disease: A Voxel-Based Morphometry Study. Cerebellum. https://doi.org/10.1007/s12311-017-0865-6
*De Winter, F. L., Timmers, D., de Gelder, B., Van Orshoven, M., Vieren, M., Bouckaert, M., et al. (2016). Face shape and face identity processing in behavioral variant fronto-temporal dementia: A specific deficit for familiarity and name recognition of famous faces. NeuroImage: Clinical, 11, 368–377.
DeJesus-Hernandez, M., Mackenzie, I. R., Boeve, B. F., Boxer, A. L., Baker, M., Rutherford, N. J., … Rademakers, R. (2011). Expanded GGGGCC hexanucleotide repeat in noncoding region of C9ORF72 causes chromosome 9p-linked FTD and ALS. Neuron, 72(2), 245–256. https://doi.org/10.1016/j.neuron.2011.09.011
*Dermody, N., Wong, S., Ahmed, R., Piguet, O., Hodges, J. R., & Irish, M. (2016). Uncovering the neural bases of cognitive and affective empathy deficits in Alzheimer's disease and the behavioral-variant of frontotemporal dementia. Journal of Alzheimer's Disease, 53(3), 801–816, doi:https://doi.org/10.3233/jad-160175.
Devenney, E., Hornberger, M., Irish, M., Mioshi, E., Burrell, J., Tan, R., … Hodges, J. R. (2014). Frontotemporal dementia associated with the C9ORF72 mutation: A unique clinical profile. JAMA Neurology, 71(3), 331–339. https://doi.org/10.1001/jamaneurol.2013.6002
*Devenney, E., Landin-Romero, R., Irish, M., Hornberger, M., Mioshi, E., Halliday, G. M., et al. (2017). The neural correlates and clinical characteristics of psychosis in the frontotemporal dementia continuum and the C9orf72 expansion. Neuroimage Clin, 13, 439–445, doi:https://doi.org/10.1016/j.nicl.2016.11.028.
Dogan, I., Tinnemann, E., Romanzetti, S., Mirzazade, S., Costa, A. S., Werner, C. J., … Reetz, K. (2016). Cognition in Friedreich's ataxia: A behavioral and multimodal imaging study. Annals of Clinical Translational Neurology, 3(8), 572–587. https://doi.org/10.1002/acn3.315
Dukart, J., Mueller, K., Horstmann, A., Barthel, H., Moller, H. E., Villringer, A., et al. (2011). Combined evaluation of FDG-PET and MRI improves detection and differentiation of dementia. PLoS One, 6(3), e18111. https://doi.org/10.1371/journal.pone.0018111
Dukart, J., Mueller, K., Horstmann, A., Vogt, B., Frisch, S., Barthel, H., … Schroeter, M. L. (2010). Differential effects of global and cerebellar normalization on detection and differentiation of dementia in FDG-PET studies. Neuroimage, 49(2), 1490–1495. https://doi.org/10.1016/j.neuroimage.2009.09.017
Eickhoff, S. B., Bzdok, D., Laird, A. R., Kurth, F., & Fox, P. T. (2012). Activation likelihood estimation meta-analysis revisited. Neuroimage, 59(3), 2349–2361. https://doi.org/10.1016/j.neuroimage.2011.09.017
Eickhoff, S. B., Laird, A. R., Grefkes, C., Wang, L. E., Zilles, K., & Fox, P. T. (2009). Coordinate-based activation likelihood estimation meta-analysis of neuroimaging data: A random-effects approach based on empirical estimates of spatial uncertainty. Human Brain Mapping, 30(9), 2907–2926. https://doi.org/10.1002/hbm.20718
*Farb, N. A., Grady, C. L., Strother, S., Tang-Wai, D. F., Masellis, M., Black, S., et al. (2013). Abnormal network connectivity in frontotemporal dementia: Evidence for prefrontal isolation. Cortex, 49(7), 1856–1873, doi:https://doi.org/10.1016/j.cortex.2012.09.008.
Ferrer, I., Legati, A., Garcia-Monco, J. C., Gomez-Beldarrain, M., Carmona, M., Blanco, R., et al. (2015). Familial behavioral variant frontotemporal dementia associated with astrocyte-predominant tauopathy. Journal of Neuropathology and Experimental Neurology, 74(4), 370–379.
Gao, L., Zhang, J., Hou, Y., Hallett, M., Chan, P., & Wu, T. (2017). The cerebellum in dual-task performance in Parkinson's disease. Scientific Reports, 7(1), 45662. https://doi.org/10.1038/srep45662
Gellersen, H. M., Guo, C. C., O'Callaghan, C., Tan, R. H., Sami, S., & Hornberger, M. (2017). Cerebellar atrophy in neurodegeneration-a meta-analysis. Journal of Neurology, Neurosurgery, and Psychiatry, 88(9), 780–788. https://doi.org/10.1136/jnnp-2017-315607
Gorno-Tempini, M. L., Hillis, A. E., Weintraub, S., Kertesz, A., Mendez, M., Cappa, S. F., … Grossman, M. (2011). Classification of primary progressive aphasia and its variants. Neurology, 76(11), 1006–1014. https://doi.org/10.1212/WNL.0b013e31821103e6
Gross-Tsur, V., Ben-Bashat, D., Shalev, R. S., Levav, M., & Sira, L. B. (2006). Evidence of a developmental cerebello-cerebral disorder. Neuropsychologia, 44(12), 2569–2572. https://doi.org/10.1016/j.neuropsychologia.2006.04.028
*Grossman, M., McMillan, C., Moore, P., Ding, L. J., Glosser, G., Work, M., et al. (2004). What's in a name: Voxel-based morphometric analyses of MRI and naming difficulty in Alzheimer's disease, frontotemporal dementia and corticobasal degeneration. Brain, 127, 628–649, doi:https://doi.org/10.1093/brain/awh075, 3.
*Guo, C. C., Tan, R., Hodges, J. R., Hu, X., Sami, S., & Hornberger, M. (2016). Network-selective vulnerability of the human cerebellum to Alzheimer's disease and frontotemporal dementia. Brain, 139(Pt 5), 1527–1538, doi:https://doi.org/10.1093/brain/aww003.
*Henley, S. M., Downey, L. E., Nicholas, J. M., Kinnunen, K. M., Golden, H. L., Buckley, A., et al. (2014). Degradation of cognitive timing mechanisms in behavioural variant frontotemporal dementia. Neuropsychologia, 65, 88–101, doi:https://doi.org/10.1016/j.neuropsychologia.2014.10.009.
*Hutchings, R. P.;Bruggemann, J.;Hodges, J. R.;Piguet, O.;Kumfor, F. (2018). Looking but not seeing: Increased eye fixations in behavioural-variant frontotemporal dementia. Cortex, 103, 71–81, doi:https://doi.org/10.1016/j.cortex.2018.02.011.
*Irish, M., Devenney, E., Wong, S., Dobson-Stone, C., Kwok, J. B., Piguet, O., Hodges J. R., Hornberger M. (2013). Neural substrates of episodic memory dysfunction in behavioural variant frontotemporal dementia with and without C9ORF72 expansions. Neuroimage Clin, 2, 836–843, doi:https://doi.org/10.1016/j.nicl.2013.06.005.
Jacobs, H. I. L., Hopkins, D. A., Mayrhofer, H. C., Bruner, E., van Leeuwen, F. W., Raaijmakers, W., & Schmahmann, J. D. (2017). The cerebellum in Alzheimer’s disease: Evaluating its role in cognitive decline. Brain, 141(1), 37–47. https://doi.org/10.1093/brain/awx194
Jiskoot, L. C. P., Meeter, L. H., Dopper, E. G. P., Donker Kaat, L., Franzen, S., van der Ende, E. L., … van Swieten, J. C. (2019). Longitudinal multimodal MRI as prognostic and diagnostic biomarker in presymptomatic familial frontotemporal dementia. Brain, 142(1), 193–208. https://doi.org/10.1093/brain/awy288
Jissendi, P., Baudry, S., & Baleriaux, D. (2008). Diffusion tensor imaging (DTI) and tractography of the cerebellar projections to prefrontal and posterior parietal cortices: A study at 3T. Journal of Neuroradiology, 35(1), 42–50. https://doi.org/10.1016/j.neurad.2007.11.001
Kelly, R. M., & Strick, P. L. (2003). Cerebellar loops with motor cortex and prefrontal cortex of a nonhuman primate. The Journal of Neuroscience, 23(23), 8432–8444.
*Kloeters, S., Bertoux, M., O'Callaghan, C., Hodges, J. R., & Hornberger, M. (2013). Money for nothing - atrophy correlates of gambling decision making in behavioural variant frontotemporal dementia and Alzheimer's disease. Neuroimage Clin, 2, 263–272, doi:https://doi.org/10.1016/j.nicl.2013.01.011.
Krienen, F. M., & Buckner, R. L. (2009). Segregated fronto-cerebellar circuits revealed by intrinsic functional connectivity. Cerebral Cortex, 19(10), 2485–2497. https://doi.org/10.1093/cercor/bhp135
*Kumfor, F., Honan, C., McDonald, S., Hazelton, J. L., Hodges, J. R., & Piguet, O. (2017). Assessing the "social brain" in dementia: Applying TASIT-S. Cortex, 93, 166–177, doi:https://doi.org/10.1016/j.cortex.2017.05.022.
Kumfor, F., Ibanez, A., Hutchings, R., Hazelton, J. L., Hodges, J. R., & Piguet, O. (2018a). Beyond the face: How context modulates emotion processing in frontotemporal dementia subtypes. Brain, 141(4), 1172–1185. https://doi.org/10.1093/brain/awy002
*Kumfor, F., Irish, M., Hodges, J. R., & Piguet, O. (2013a). Discrete neural correlates for the recognition of negative emotions: Insights from frontotemporal dementia. PLoS One, 8(6), e67457, doi:https://doi.org/10.1371/journal.pone.0067457.
*Kumfor, F., Irish, M., Hodges, J. R., & Piguet, O. (2013b). The orbitofrontal cortex is involved in emotional enhancement of memory: Evidence from the dementias. Brain, 136(Pt 10), 2992–3003, doi:https://doi.org/10.1093/brain/awt185.
Kumfor, F., Landin-Romero, R., Devenney, E., Hutchings, R., Grasso, R., Hodges, J. R., & Piguet, O. (2016). On the right side? A longitudinal study of left- versus right-lateralized semantic dementia. Brain, 139(Pt 3), 986–998. https://doi.org/10.1093/brain/awv387
*Kumfor, F., Zhen, A., Hodges, J. R., Piguet, O., & Irish, M. (2018b). Apathy in Alzheimer's disease and frontotemporal dementia: Distinct clinical profiles and neural correlates. Cortex, 103, 350–359, doi:https://doi.org/10.1016/j.cortex.2018.03.019.
Laidi, C., Boisgontier, J., Chakravarty, M. M., Hotier, S., d'Albis, M. A., Mangin, J. O., et al. (2017). Cerebellar anatomical alterations and attention to eyes in autism. Scientific Reports, 7(1), 12008. https://doi.org/10.1038/s41598-017-11883-w
*Laisney, M., Matuszewski, V., Mezenge, F., Belliard, S., de la Sayette, V., Eustache, F., et al. (2009). The underlying mechanisms of verbal fluency deficit in frontotemporal dementia and semantic dementia. Journal of Neurology, 256(7), 1083–1094, doi:https://doi.org/10.1007/s00415-009-5073-y.
Lancaster, J. L., Tordesillas-Gutierrez, D., Martinez, M., Salinas, F., Evans, A., Zilles, K., et al. (2007). Bias between MNI and Talairach coordinates analyzed using the ICBM-152 brain template. Human Brain Mapping, 28(11), 1194–1205. https://doi.org/10.1002/hbm.20345
Lange, I., Kasanova, Z., Goossens, L., Leibold, N., De Zeeuw, C. I., van Amelsvoort, T., et al. (2015). The anatomy of fear learning in the cerebellum: A systematic meta-analysis. Neuroscience and Biobehavioral Reviews, 59, 83–91. https://doi.org/10.1016/j.neubiorev.2015.09.019
Lee, S. E., Khazenzon, A. M., Trujillo, A. J., Guo, C. C., Yokoyama, J. S., Sha, S. J., … Seeley, W. W. (2014). Altered network connectivity in frontotemporal dementia with C9orf72 hexanucleotide repeat expansion. Brain, 137(Pt 11), 3047–3060. https://doi.org/10.1093/brain/awu248
*Meijboom, R., Steketee, R. M., de Koning, I., Osse, R. J., Jiskoot, L. C., de Jong, F. J., et al. (2016). Functional connectivity and microstructural white matter changes in phenocopy frontotemporal dementia. European Radiology, doi:https://doi.org/10.1007/s00330-016-4490-4, 27, 4, 1352, 1360.
Muller, V. I., Cieslik, E. C., Laird, A. R., Fox, P. T., Radua, J., Mataix-Cols, D., et al. (2018). Ten simple rules for neuroimaging meta-analysis. Neuroscience and Biobehavioral Reviews, 84, 151–161. https://doi.org/10.1016/j.neubiorev.2017.11.012
Neary, D., Snowden, J. S., Gustafson, L., Passant, U., Stuss, D., Black, S., … Benson, D. F. (1998). Frontotemporal lobar degeneration: a consensus on clinical diagnostic criteria. Neurology, 51(6), 1546–1554.
Petacchi, A., Laird, A. R., Fox, P. T., & Bower, J. M. (2005). Cerebellum and auditory function: An ALE meta-analysis of functional neuroimaging studies. Human Brain Mapping, 25(1), 118–128. https://doi.org/10.1002/hbm.20137
Ramnani, N. (2006). The primate cortico-cerebellar system: Anatomy and function. Nature Reviews. Neuroscience, 7(7), 511–522. https://doi.org/10.1038/nrn1953
Ramnani, N. (2012). Frontal lobe and posterior parietal contributions to the cortico-cerebellar system. Cerebellum, 11(2), 366–383. https://doi.org/10.1007/s12311-011-0272-3
Ramnani, N., Behrens, T. E., Johansen-Berg, H., Richter, M. C., Pinsk, M. A., Andersson, J. L., et al. (2006). The evolution of prefrontal inputs to the cortico-pontine system: Diffusion imaging evidence from macaque monkeys and humans. Cerebral Cortex, 16(6), 811–818. https://doi.org/10.1093/cercor/bhj024
Rascovsky, K., Hodges, J. R., Kipps, C. M., Johnson, J. K., Seeley, W. W., Mendez, M. F., … Miller, B. M. (2007). Diagnostic criteria for the behavioral variant of frontotemporal dementia (bvFTD): Current limitations and future directions. Alzheimer Disease and Associated Disorders, 21(4), S14–S18. https://doi.org/10.1097/WAD.0b013e31815c3445
Rascovsky, K., Hodges, J. R., Knopman, D., Mendez, M. F., Kramer, J. H., Neuhaus, J., … Miller, B. L. (2011). Sensitivity of revised diagnostic criteria for the behavioural variant of frontotemporal dementia. Brain, 134(Pt 9), 2456–2477. https://doi.org/10.1093/brain/awr179
Ratnavalli, E., Brayne, C., Dawson, K., & Hodges, J. R. (2002). The prevalence of frontotemporal dementia. Neurology, 58(11), 1615–1621.
Renton, A. E., Majounie, E., Waite, A., Simon-Sanchez, J., Rollinson, S., Gibbs, J. R., et al. (2011). A hexanucleotide repeat expansion in C9ORF72 is the cause of chromosome 9p21-linked ALS-FTD. Neuron, 72(2), 257–268. https://doi.org/10.1016/j.neuron.2011.09.010
Riedel, M. C., Ray, K. L., Dick, A. S., Sutherland, M. T., Hernandez, Z., Fox, P. M., … Laird, A. R. (2015). Meta-analytic connectivity and behavioral parcellation of the human cerebellum. Neuroimage, 117, 327–342. https://doi.org/10.1016/j.neuroimage.2015.05.008
Rosen, H. J., Gorno-Tempini, M. L., Goldman, W. P., Perry, R. J., Schuff, N., Weiner, M., et al. (2002). Patterns of brain atrophy in frontotemporal dementia and semantic dementia. Neurology, 58(2), 198–208.
Savica, R., Adeli, A., Vemuri, P., Knopman, D. S., Dejesus-Hernandez, M., Rademakers, R., et al. (2012). Characterization of a family with c9FTD/ALS associated with the GGGGCC repeat expansion in C9ORF72. Archives of Neurology, 69(9), 1164–1169. https://doi.org/10.1001/archneurol.2012.772
Schmahmann, J. D., & Pandya, D. N. (1995). Prefrontal cortex projections to the basilar pons in rhesus monkey: Implications for the cerebellar contribution to higher function. Neuroscience Letters, 199(3), 175–178.
Schmahmann, J. D., & Pandya, D. N. (1997a). Anatomic organization of the basilar pontine projections from prefrontal cortices in rhesus monkey. The Journal of Neuroscience, 17(1), 438–458.
Schmahmann, J. D., & Pandya, D. N. (1997b). The cerebrocerebellar system. International Review of Neurobiology, 41, 31–60.
Schmahmann, J. D., & Sherman, J. C. (1998). The cerebellar cognitive affective syndrome. Brain, 121(4), 561–579.
*Seelaar, H., Papma, J. M., Garraux, G., de Koning, I., Reijs, A. E., Valkema, R., Rozemuller A. J. M., Salmon E., van Swieten J. C. (2011). Brain perfusion patterns in familial frontotemporal lobar degeneration. Neurology, 77(4), 384–392, doi:https://doi.org/10.1212/WNL.0b013e3182270456.
Seeley, W. W., Crawford, R., Rascovsky, K., Kramer, J. H., Weiner, M., Miller, B. L., & Gorno-Tempini, M. L. (2008). Frontal paralimbic network atrophy in very mild behavioral variant frontotemporal dementia. Archives of Neurology, 65(2), 249–255. https://doi.org/10.1001/archneurol.2007.38
Sha, S. J., Takada, L. T., Rankin, K. P., Yokoyama, J. S., Rutherford, N. J., Fong, J. C., … Boxer, A. L. (2012). Frontotemporal dementia due to C9ORF72 mutations: Clinical and imaging features. Neurology, 79(10), 1002–1011. https://doi.org/10.1212/WNL.0b013e318268452e
Shinn, A. K., Roh, Y. S., Ravichandran, C. T., Baker, J. T., Ongur, D., & Cohen, B. M. (2017). Aberrant cerebellar connectivity in bipolar disorder with psychosis. Biol Psychiatry Cogn Neurosci Neuroimaging, 2(5), 438–448. https://doi.org/10.1016/j.bpsc.2016.07.002
Stoodley, C. J., & Schmahmann, J. D. (2009). Functional topography in the human cerebellum: A meta-analysis of neuroimaging studies. Neuroimage, 44(2), 489–501. https://doi.org/10.1016/j.neuroimage.2008.08.039
Strenziok, M., Pulaski, S., Krueger, F., Zamboni, G., Clawson, D., & Grafman, J. (2011). Regional brain atrophy and impaired decision making on the balloon analog risk task in behavioral variant frontotemporal dementia. Cognitive and Behavioral Neurology, 24(2), 59–67. https://doi.org/10.1097/WNN.0b013e3182255a7c
Strick, P. L., Dum, R. P., & Fiez, J. A. (2009). Cerebellum and nonmotor function. Annual Review of Neuroscience, 32(1), 413–434. https://doi.org/10.1146/annurev.neuro.31.060407.125606
Strong, M. J., Grace, G. M., Freedman, M., Lomen-Hoerth, C., Woolley, S., Goldstein, L. H., … Figlewicz, D. (2009). Consensus criteria for the diagnosis of frontotemporal cognitive and behavioural syndromes in amyotrophic lateral sclerosis. Amyotrophic Lateral Sclerosis, 10(3), 131–146.
*Sturm, V. E., Yokoyama, J. S., Eckart, J. A., Zakrzewski, J., Rosen, H. J., Miller, B. L., Seeley W. W., Levenson R. W. (2015). Damage to left frontal regulatory circuits produces greater positive emotional reactivity in frontotemporal dementia. Cortex, 64, 55–67, doi:https://doi.org/10.1016/j.cortex.2014.10.002.
Suarez-Calvet, M., Camacho, V., Gomez-Anson, B., Anton, S., Vives-Gilabert, Y., Dols-Icardo, O., et al. (2015). Early cerebellar Hypometabolism in patients with frontotemporal dementia carrying the C9orf72 expansion. Alzheimer Disease and Associated Disorders, 29(4), 353–356. https://doi.org/10.1097/WAD.0000000000000056
*Synn, A., Mothakunnel, A., Kumfor, F., Chen, Y., Piguet, O., Hodges, J. R., et al. (2017). Mental states in moving shapes: Distinct cortical and subcortical contributions to theory of mind impairments in dementia. Journal of Alzheimer's Disease, 61(2), 521-535, doi: https://doi.org/10.3233/JAD-170809.
Synn, A., Mothakunnel, A., Kumfor, F., Chen, Y., Piguet, O., Hodges, J. R., & Irish, M. (2018). Mental states in moving shapes: Distinct cortical and subcortical contributions to theory of mind impairments in dementia. Journal of Alzheimer's Disease, 61(2), 521–535. https://doi.org/10.3233/JAD-170809
Tan, R. H., Devenney, E., Dobson-Stone, C., Kwok, J. B., Hodges, J. R., Kiernan, M. C., … Hornberger, M. (2014). Cerebellar integrity in the amyotrophic lateral sclerosis-frontotemporal dementia continuum. PLoS One, 9(8), e105632. https://doi.org/10.1371/journal.pone.0105632
*Tan, R. H., Devenney, E., Kiernan, M. C., Halliday, G. M., Hodges, J. R., & Hornberger, M. (2015). Terra incognita-cerebellar contributions to neuropsychiatric and cognitive dysfunction in behavioral variant frontotemporal dementia. Frontiers in Aging Neuroscience, 7, 121, doi:https://doi.org/10.3389/fnagi.2015.00121.
Turkeltaub, P. E., Eden, G. F., Jones, K. M., & Zeffiro, T. A. (2002). Meta-analysis of the functional neuroanatomy of single-word reading: Method and validation. Neuroimage, 16(3 Pt 1), 765–780.
Turkeltaub, P. E., Eickhoff, S. B., Laird, A. R., Fox, M., Wiener, M., & Fox, P. (2012). Minimizing within-experiment and within-group effects in activation likelihood estimation meta-analyses. Human Brain Mapping, 33(1), 1–13. https://doi.org/10.1002/hbm.21186
Van Overwalle, F., Baetens, K., Marien, P., & Vandekerckhove, M. (2014). Social cognition and the cerebellum: A meta-analysis of over 350 fMRI studies. Neuroimage, 86, 554–572. https://doi.org/10.1016/j.neuroimage.2013.09.033
Van Overwalle, F., D'Aes, T., & Marien, P. (2015). Social cognition and the cerebellum: A meta-analytic connectivity analysis. Human Brain Mapping, 36(12), 5137–5154. https://doi.org/10.1002/hbm.23002
Vemuri, P., Simon, G., Kantarci, K., Whitwell, J. L., Senjem, M. L., Przybelski, S. A., … Jack, C. R., Jr. (2011). Antemortem differential diagnosis of dementia pathology using structural MRI: Differential-STAND. Neuroimage, 55(2), 522–531. https://doi.org/10.1016/j.neuroimage.2010.12.073
Whitwell, J. L., Avula, R., Senjem, M. L., Kantarci, K., Weigand, S. D., Samikoglu, A., … Jack, C. R. (2010). Gray and white matter water diffusion in the syndromic variants of frontotemporal dementia. Neurology, 74(16), 1279–1287. https://doi.org/10.1212/WNL.0b013e3181d9edde
Whitwell, J. L., Weigand, S. D., Boeve, B. F., Senjem, M. L., Gunter, J. L., DeJesus-Hernandez, M., … Josephs, K. A. (2012). Neuroimaging signatures of frontotemporal dementia genetics: C9ORF72, tau, progranulin and sporadics. Brain, 135(Pt 3), 794–806. https://doi.org/10.1093/brain/aws001
*Wong, S., Irish, M., O'Callaghan, C., Kumfor, F., Savage, G., Hodges, J. R., et al. (2017). Should I trust you? Learning and memory of social interactions in dementia. Neuropsychologia, 104, 157–167, doi:https://doi.org/10.1016/j.neuropsychologia.2017.08.016.
Acknowledgements
The authors are grateful for the kind assistance of the authors of the publications that were included in this study. We would like to thank Chengtao Liang for his help with ALE pipeline establishment. The authors wish to acknowledge the Sydney Informatics Hub at the University of Sydney for providing access to High Performance Computing (HPC). This work was supported in part by funding to Forefront, a collaborative research group specialised in the study of frontotemporal dementia and motor neuron disease, from the National Health and Medical Research Council (NHMRC) of Australia program grant (APP1037746) and the Australian Research Council (ARC) Centre of Excellence in Cognition and its Disorders Memory Program (CE110001021). YC is supported by the State Scholarship Fund of China (No. 201608200010). FK is supported by an NHMRC-ARC Dementia Research Development Fellowship (APP1097026). RLR is supported by the Appenzeller Neuroscience Fellowship in Alzheimer’s Disease and the ARC Centre of Excellence in Cognition and its Disorders Memory Program (CE110001021). MI is supported by an ARC Future Fellowship (FT160100096). OP is supported by an NHMRC Senior Research Fellowship (APP1103258).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 1181 kb)
Rights and permissions
About this article
Cite this article
Chen, Y., Kumfor, F., Landin-Romero, R. et al. The Cerebellum in Frontotemporal Dementia: a Meta-Analysis of Neuroimaging Studies. Neuropsychol Rev 29, 450–464 (2019). https://doi.org/10.1007/s11065-019-09414-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11065-019-09414-7