Abstract
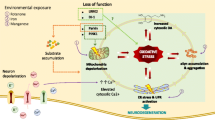
Dopaminergic neurons die in Parkinson’s disease (PD) due to oxidative stress and mitochondrial dysfunction in the substantia nigra (SN). We evaluated if oxidative stress occurs in other brain regions like the caudate nucleus (CD), putamen (Put) and frontal cortex (FC) in human postmortem PD brains (n = 6). While protein oxidation was elevated only in CD (P < 0.05), lipid peroxidation was increased only in FC (P < 0.05) and protein nitration was unchanged in PD compared to controls. Interestingly, mitochondrial complex I (CI) activity was unaffected in PD compared to controls. There was a 3–5 fold increase in the total glutathione (GSH) levels in the three regions (P < 0.01 in FC and CD; P < 0.05 in Put) but activities of antioxidant enzymes catalase, superoxide dismutase, glutathione reductase and glutathione-s-tranferase were not increased. Total GSH levels were elevated in these areas because of decreased activity of gamma glutamyl transpeptidase (γ-GT) (P < 0.05) activity suggesting a decreased breakdown of GSH. There was an increase in expression of glial fibrillary acidic protein (GFAP) (P < 0.001 in FC; P < 0.05 in CD) and glutathione peroxidase (P < 0.05 in CD and Put) activity due to proliferation of astrocytes. We suggest that increased GSH and astrocytic proliferation protects non-SN brain regions from oxidative and mitochondrial damage in PD.






Similar content being viewed by others
Abbreviations
- PD:
-
Parkinson’s disease
- AD:
-
Alzheimer’s disease
- SN:
-
Substantia nigra
- CI:
-
Mitochondrial complex I
- ROS:
-
Reactive oxygen species
- GSH:
-
Glutathione reduced
- PMI:
-
Postmortem interval
- FC:
-
Frontal cortex
- CD:
-
Caudate nucleus
- Put:
-
Putamen
- SN:
-
Substantia Nigra
- 3-NT:
-
3-nitrotyrosine
- GFAP:
-
Glial Fibrillary acidic protein
- SOD:
-
Superoxide dismutase
- GST:
-
Glutathione-s-transferase
- GR:
-
Glutathione reductase
- γ-GCL:
-
Gamma glutamyl cysteine ligase
- γGT:
-
Gamma glutamyl transpeptidase
- GPx:
-
Glutathione peroxidase
References
Hoehn MM, Yahr MD (1967) Parkinsonism: onset, progression and mortality. Neurology 17:427–442
Adams JD Jr, Chang ML, Klaidman L (2001) Parkinson’s disease–redox mechanisms. Curr Med Chem 8:809–814
Beal MF (1992) Does impairment of energy metabolism result in excitotoxic neuronal death in neurodegenerative illnesses? Ann Neurol 31:119–130
Jenner P, Dexter DT, Sian J et al. (1992) Oxidative stress as a cause of nigral cell death in Parkinson’s disease and incidental Lewy body disease. The Royal Kings and Queens Parkinson’s Disease Research Group. Ann Neurol 32(Suppl): S82–S87
Koiliatsos VE (1998) Parkinson’s disease. In: Burke RE (ed) Cell death and disease of the nervous system. Humana Press, Totowa, pp 459–475
Sayre LM, Smith MA, Perry G (2001) Chemistry and biochemistry of oxidative stress in neurodegenerative disease. Curr Med Chem 8:721–738
Bharath S, Hsu M, Kaur D et al (2002) Glutathione, iron and Parkinson’s disease. Biochem Pharmacol 64:1037–1048
Dexter DT, Carter CJ, Wells FR et al (1989) Basal lipid peroxidation in substantia nigra is increased in Parkinson’s disease. J Neurochem 52:381–389
Yoritaka A, Hattori N, Uchida K et al (1996) Immunohistochemical detection of 4-hydroxynonenal protein adducts in Parkinson disease. Proc Natl Acad Sci USA 93:2696–2701
Alam ZI, Jenner A, Daniel SE et al (1997) Oxidative DNA damage in the parkinsonian brain: an apparent selective increase in 8-hydroxyguanine levels in substantia nigra. J Neurochem 69:1196–1203
Dexter DT, Wells FR, Lees AJ et al (1989) Increased nigral iron content and alterations in other metal ions occurring in brain in Parkinson’s disease. J Neurochem 52:1830–1836
Sofic E, Paulus W, Jellinger K et al (1991) Selective increase of iron in substantia nigra zona compacta of parkinsonian brains. J Neurochem 56:978–982
Alam ZI, Daniel SE, Lees AJ et al (1997) A generalised increase in protein carbonyls in the brain in Parkinson’s but not incidental Lewy body disease. J Neurochem 69:1326–1329
Floor E, Wetzel MG (1998) Increased protein oxidation in human substantia nigra pars compacta in comparison with basal ganglia and prefrontal cortex measured with an improved dinitrophenylhydrazine assay. J Neurochem 70:268–275
Good PF, Hsu A, Werner P et al (1998) Protein nitration in Parkinson’s disease. J Neuropathol Exp Neurol 57:338–342
Blanchard-Fillion B, Prou D, Polydoro M et al (2006) Metabolism of 3-nitrotyrosine induces apoptotic death in dopaminergic cells. J Neurosci 26:6124–6130
Danielson SR, Andersen JK (2008) Oxidative and nitrative protein modifications in Parkinson’s disease. Free Radic Biol Med 44:1787–1794
Ferrante RJ, Hantraye P, Brouillet E et al (1999) Increased nitrotyrosine immunoreactivity in substantia nigra neurons in MPTP treated baboons is blocked by inhibition of neuronal nitric oxide synthase. Brain Res 823:177–182
Hasegawa E, Takeshige K, Oishi T et al (1990) 1-Methyl-4-phenylpyridinium (MPP+) induces NADH-dependent superoxide formation and enhances NADH-dependent lipid peroxidation in bovine heart submitochondrial particles. Biochem Biophys Res Commun 170:1049–1055
Ischiropoulos H, Beckman JS (2003) Oxidative stress and nitration in neurodegeneration: cause, effect, or association? J Clin Invest 111:163–169
Pennathur S, Jackson-Lewis V, Przedborski S et al (1999) Mass spectrometric quantification of 3-nitrotyrosine, ortho-tyrosine, and o, o’-dityrosine in brain tissue of 1-methyl-4-phenyl-1, 2, 3, 6-tetrahydropyridine-treated mice, a model of oxidative stress in Parkinson’s disease. J Biol Chem 274:34621–34628
Keeney PM, Xie J, Capaldi RA et al (2006) Parkinson’s disease brain mitochondrial complex I has oxidatively damaged subunits and is functionally impaired and misassembled. J Neurosci 26:5256–5264
Schapira AH, Cooper JM, Dexter D et al (1990) Mitochondrial complex I deficiency in Parkinson’s disease. J Neurochem 54:823–827
Jagatha B, Mythri RB, Vali S et al (2008) Curcumin treatment alleviates the effects of glutathione depletion in vitro and in vivo: therapeutic implications for Parkinson’s disease explained via in silico studies. Free Radic Biol Med 44:907–917
Rogers J, Mastroeni D, Leonard B et al (2007) Neuroinflammation in Alzheimer’s disease and Parkinson’s disease: are microglia pathogenic in either disorder? Int Rev Neurobiol 82:235–246
Werner CJ, Heyny-von Haussen R, Mall G et al (2008) Proteome analysis of human substantia nigra in Parkinson’s disease. Proteome Sci 6:8
Braak H, Del Tredici K, Rub U et al (2003) Staging of brain pathology related to sporadic Parkinson’s disease. Neurobiol Aging 24:197–211
Alladi PA, Mahadevan A, Shankar SK et al (2010) Expression of GDNF receptors GFRalpha1 and RET is preserved in substantia nigra pars compacta of aging Asian Indians. J Chem Neuroanat 40:43–52
Alladi PA, Mahadevan A, Vijayalakshmi K et al (2010) Ageing enhances alpha-synuclein, ubiquitin and endoplasmic reticular stress protein expression in the nigral neurons of Asian Indians. Neurochem Int 57:530–539
Alladi PA, Mahadevan A, Yasha TC et al (2009) Absence of age-related changes in nigral dopaminergic neurons of Asian Indians: relevance to lower incidence of Parkinson’s disease. Neuroscience 159:236–245
Karunakaran S, Saeed U, Mishra M et al (2008) Selective activation of p38 mitogen-activated protein kinase in dopaminergic neurons of substantia nigra leads to nuclear translocation of p53 in 1-methyl-4-phenyl-1, 2, 3, 6-tetrahydropyridine-treated mice. J Neurosci 28:12500–12509
Karunakaran S, Saeed U, Ramakrishnan S et al (2007) Constitutive expression and functional characterization of mitochondrial glutaredoxin (Grx2) in mouse and human brain. Brain Res 1185:8–17
Agarwal V, Kommaddi RP, Valli K et al (2008) Drug metabolism in human brain: high levels of cytochrome P4503A43 in brain and metabolism of anti-anxiety drug alprazolam to its active metabolite. PLoS One 3:e2337
Chinta SJ, Kommaddi RP, Turman CM et al (2005) Constitutive expression and localization of cytochrome P-450 1A1 in rat and human brain: presence of a splice variant form in human brain. J Neurochem 93:724–736
Chandana R, Mythri RB, Mahadevan A et al (2009) Biochemical analysis of protein stability in human brain collected at different post-mortem intervals. Indian J Med Res 129:189–199
Ohkawa H, Ohishi N, Yagi K (1979) Assay for lipid peroxides in animal tissues by thiobarbituric acid reaction. Anal Biochem 95:351–358
Mythri RB, Jagatha B, Pradhan N et al (2007) Mitochondrial complex I inhibition in Parkinson’s disease: how can curcumin protect mitochondria? Antioxid Redox Signal 9:399–408
Trounce IA, Kim YL, Jun AS et al (1996) Assessment of mitochondrial oxidative phosphorylation in patient muscle biopsies, lymphoblasts, and transmitochondrial cell lines. Methods Enzymol 264:484–509
Aebi H (1984) Catalase in vitro. Methods Enzymol 105:121–126
Bagnyukova TV, Storey KB, Lushchak VI (2003) Induction of oxidative stress in Rana ridibunda during recovery from winter hibernation. J Therm Biol 28:21–28
Guthenberg C, Alin P, Mannervik B (1985) Glutathione transferase from rat testis. Methods Enzymol 113:507–510
Carlberg I, Mannervik B (1985) Glutathione reductase. Methods Enzymol 113:484–490
Flohe L, Gunzler WA (1984) Assays of glutathione peroxidase. Methods Enzymol 105:114–121
Tietze F (1969) Enzymic method for quantitative determination of nanogram amounts of total and oxidized glutathione: applications to mammalian blood and other tissues. Anal Biochem 27:502–522
Seelig GF, Meister A (1985) Glutathione biosynthesis; gamma-glutamylcysteine synthetase from rat kidney. Methods Enzymol 113:379–390
Sian J, Dexter DT, Lees AJ et al (1994) Glutathione-related enzymes in brain in Parkinson’s disease. Ann Neurol 36:356–361
Albers DS, Beal MF (2000) Mitochondrial dysfunction and oxidative stress in aging and neurodegenerative disease. J Neural Transm Suppl 59:133–154
Banerjee R, Starkov AA, Beal MF et al (2009) Mitochondrial dysfunction in the limelight of Parkinson’s disease pathogenesis. Biochim Biophys Acta 1792:651–663
Lin MT, Beal MF (2006) Mitochondrial dysfunction and oxidative stress in neurodegenerative diseases. Nature 443:787–795
Schapira AH, Cooper JM, Dexter D et al (1989) Mitochondrial complex I deficiency in Parkinson’s disease. Lancet 1:1269
Schapira AH, Mann VM, Cooper JM et al (1990) Anatomic and disease specificity of NADH CoQ1 reductase (complex I) deficiency in Parkinson’s disease. J Neurochem 55:2142–2145
Jenner P (1993) Altered mitochondrial function, iron metabolism and glutathione levels in Parkinson’s disease. Acta Neurol Scand Suppl 146:6–13
Damier P, Hirsch EC, Zhang P et al (1993) Glutathione peroxidase, glial cells and Parkinson’s disease. Neuroscience 52:1–6
Mann VM, Cooper JM, Daniel SE et al (1994) Complex I, iron, and ferritin in Parkinson’s disease substantia nigra. Ann Neurol 36:876–881
Pearce RK, Owen A, Daniel S et al (1997) Alterations in the distribution of glutathione in the substantia nigra in Parkinson’s disease. J Neural Transm 104:661–677
Perry TL, Godin DV, Hansen S (1982) Parkinson’s disease: a disorder due to nigral glutathione deficiency? Neurosci Lett 33:305–310
Perry TL, Yong VW (1986) Idiopathic Parkinson’s disease, progressive supranuclear palsy and glutathione metabolism in the substantia nigra of patients. Neurosci Lett 67:269–274
Chinta SJ, Andersen JK (2006) Reversible inhibition of mitochondrial complex I activity following chronic dopaminergic glutathione depletion in vitro: implications for Parkinson’s disease. Free Radic Biol Med 41:1442–1448
Hsu M, Srinivas B, Kumar J et al (2005) Glutathione depletion resulting in selective mitochondrial complex I inhibition in dopaminergic cells is via an NO-mediated pathway not involving peroxynitrite: implications for Parkinson’s disease. J Neurochem 92:1091–1103
Clementi E, Brown GC, Feelisch M et al (1998) Persistent inhibition of cell respiration by nitric oxide: crucial role of S-nitrosylation of mitochondrial complex I and protective action of glutathione. Proc Natl Acad Sci USA 95:7631–7636
Bharath S, Andersen JK (2005) Glutathione depletion in a midbrain-derived immortalized dopaminergic cell line results in limited tyrosine nitration of mitochondrial complex I subunits: implications for Parkinson’s disease. Antioxid Redox Signal 7:900–910
Greenamyre JT, Sherer TB, Betarbet R et al (2001) Complex I and Parkinson’s disease. IUBMB Life 52:135–141
Sian J, Dexter DT, Lees AJ et al (1994) Alterations in glutathione levels in Parkinson’s disease and other neurodegenerative disorders affecting basal ganglia. Ann Neurol 36:348–355
Riederer P, Sofic E, Rausch WD et al (1989) Transition metals, ferritin, glutathione, and ascorbic acid in parkinsonian brains. J Neurochem 52:515–520
Adams JD Jr, Klaidman LK, Odunze IN et al (1991) Alzheimer’s and Parkinson’s disease. Brain levels of glutathione, glutathione disulfide, and vitamin E. Mol Chem Neuropathol 14:213–226
Chinta SJ, Kumar JM, Zhang H et al (2006) Up-regulation of gamma-glutamyl transpeptidase activity following glutathione depletion has a compensatory rather than an inhibitory effect on mitochondrial complex I activity: implications for Parkinson’s disease. Free Radic Biol Med 40:1557–1563
Frade J, Pope S, Schmidt M et al (2008) Glutamate induces release of glutathione from cultured rat astrocytes–a possible neuroprotective mechanism? J Neurochem 105:1144–1152
Gegg ME, Beltran B, Salas-Pino S et al (2003) Differential effect of nitric oxide on glutathione metabolism and mitochondrial function in astrocytes and neurones: implications for neuroprotection/neurodegeneration? J Neurochem 86:228–237
Sagara J, Makino N, Bannai S (1996) Glutathione efflux from cultured astrocytes. J Neurochem 66:1876–1881
Shih AY, Johnson DA, Wong G et al (2003) Coordinate regulation of glutathione biosynthesis and release by Nrf2-expressing glia potently protects neurons from oxidative stress. J Neurosci 23:3394–3406
Ramsey CP, Glass CA, Montgomery MB et al (2007) Expression of Nrf2 in neurodegenerative diseases. J Neuropathol Exp Neurol 66:75–85
McGeer PL, Itagaki S, Boyes BE et al (1988) Reactive microglia are positive for HLA-DR in the substantia nigra of Parkinson’s and Alzheimer’s disease brains. Neurology 38:1285–1291
Mirza B, Hadberg H, Thomsen P et al (2000) The absence of reactive astrocytosis is indicative of a unique inflammatory process in Parkinson’s disease. Neuroscience 95:425–432
Bertrand E, Lechowicz W, Szpak GM et al (1997) Qualitative and quantitative analysis of locus coeruleus neurons in Parkinson’s disease. Folia Neuropathol 35:80–86
Martin HL, Teismann P (2009) Glutathione–a review on its role and significance in Parkinson’s disease. FASEB J 23:3263–3272
Lin LF, Doherty DH, Lile JD et al (1993) GDNF: a glial cell line-derived neurotrophic factor for midbrain dopaminergic neurons. Science 260:1130–1132
Acknowledgments
This work was financially supported by the Department of Science and Technology (DST) (fast-track grant no.SR/FT/L-152/2005), India and Indian Council of Medical Research (ICMR IRIS ID No. 2009-07710), India, both to MMSB. RM was supported by a senior research fellowship from Council of Scientific and Industrial Research (CSIR), India. GH is a senior research fellow of ICMR, India. We thank all the donors and their relatives for donating human brain tissue samples for this study. Human brain tissue for the study is sourced from Human Brain Tissue Repository for Neurobiological Studies (A National Research Facility), Department of Neuropathology, NIMHANS, Bangalore 560 029.
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
11064_2011_471_MOESM1_ESM.tif
Supplementary Fig. 1 Analysis of markers of oxidative/nitrosative stress in the SN region of postmortem human brains (PD (representative PD sample no. 6 in Table 1) and controls (C)). a Total GSH was estimated in C vs PD in SN. b Estimation of lipid peroxidation in SN from C and PD samples. c Total protein extract after DNP-derivatization (~10 μg) in SN from C and PD samples were spotted on nitrocellulose membrane in triplicate followed by anti-DNP western blot (Oxyblot) and the quantitative plot of anti-DNP signal (normalized with β-actin signal) in C and PD SN regions is shown. d Total protein extracts (~25 μg) from SN from C and PD samples were spotted on nitrocellulose membrane followed by anti-3NT western blot and the quantitative plot of 3-NT signal (normalized with β-actin signal) in C and PD SN region are shown. All the samples were tested for oxidative markers in multiple experiments (n ≥ 3). **P < 0.01 and ***P < 0.001 in PD compared to C (TIFF 2409 kb)
Rights and permissions
About this article
Cite this article
Mythri, R.B., Venkateshappa, C., Harish, G. et al. Evaluation of Markers of Oxidative Stress, Antioxidant Function and Astrocytic Proliferation in the Striatum and Frontal Cortex of Parkinson’s Disease Brains. Neurochem Res 36, 1452–1463 (2011). https://doi.org/10.1007/s11064-011-0471-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-011-0471-9