Abstract
Purpose
As per the 2016 World Health Organization (WHO) guidelines on the classification of central nervous system tumors, solitary fibrous tumors (SFTs) and hemangiopericytomas (HPCs) constitute a single disease entity, known as SFT/HPC. This study provides a clinical analysis of these tumors and describes the treatment outcomes of SFT/HPCs.
Methods
This retrospective study included 76 patients with histopathologically proven SFT/HPC. Reclassification according to the 2016 WHO guideline was done for patients who were diagnosed with SFT or HPC based on the 2007 WHO classification. Recurrence-free survival (RFS) and overall survival (OS) were evaluated for all patients and subgroups.
Results
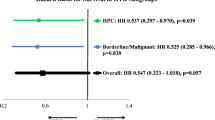
The median follow-up period was 77.9 months. The median RFS and OS were 126.5 and 136.8 months, respectively. The 1-, 5-, 10-, and 15-year RFS rates were 93%, 72%, 40%, and 40%, respectively. The 1-, 5-, 10- and 15-year OS rates were 97%, 89%, 54%, and 35%, respectively. In multivariable analyses, stereotactic radiosurgery (SRS; p = 0.009, hazard ratio [HR] 6.986), female sex (p = 0.023, HR 1.76), and age over 45 (p = 0.037, HR 2.74) were associated with shorter RFS. Patients who underwent SRS as initial treatment had a shorter OS than that of patients who underwent primary resection (p < 0.001, HR 12.86).
Conclusions
High-grade tumors tended to have worse OS and occur extracranial metastases earlier than low-grade tumors. The median RFS was not different between grade II and III tumors. Male sex, younger age, and GTR were associated with a better RFS. A history of SRS before tumor resection was associated with a shorter RFS and OS.

Similar content being viewed by others
References
Schiariti M, Goetz P, El-Maghraby H, Tailor J, Kitchen N (2011) Hemangiopericytoma: long-term outcome revisited. Clinical article. J Neurosurg 114(3):747–755. https://doi.org/10.3171/2010.6.JNS091660
Dufour H, Métellus P, Fuentes S, Murracciole X, Régis J, Figarella-Branger D, Grisoli F (2001) Meningeal hemangiopericytoma: a retrospective study of 21 patients with special review of postoperative external radiotherapy. Neurosurgery 48(4):756–762. https://doi.org/10.1097/00006123-200104000-00011discussion 762-753
Guthrie BL, Ebersold MJ, Scheithauer BW, Shaw EG (1989) Meningeal hemangiopericytoma: histopathological features, treatment, and long-term follow-up of 44 cases. Neurosurgery 25(4):514–522
Shnayder Y, Greenfield BJ, Oweity T, DeLacure MD (2003) Malignant solitary fibrous tumor of the tongue. Am J Otolaryngol 24(4):246–249. https://doi.org/10.1016/s0196-0709(03)00007-3
Vimi S, Punnya VA, Kaveri H, Rekha K (2008) An aggressive solitary fibrous tumor with evidence of malignancy: a rare case report. Head Neck Pathol 2(3):236–241. https://doi.org/10.1007/s12105-008-0073-2
Louis DN, Perry A, Reifenberger G, von Deimling A, Figarella-Branger D, Cavenee WK, Ohgaki H, Wiestler OD, Kleihues P, Ellison DW (2016) The 2016 World Health Organization Classification of Tumors of the Central Nervous System: a summary. Acta Neuropathol 131(6):803–820. https://doi.org/10.1007/s00401-016-1545-1
Kim BS, Kim Y, Kong DS, Nam DH, Lee JI, Suh YL, Seol HJ (2018) Clinical outcomes of intracranial solitary fibrous tumor and hemangiopericytoma: analysis according to the 2016 WHO classification of central nervous system tumors. J Neurosurg 129(6):1384–1396. https://doi.org/10.3171/2017.7.JNS171226
Kinslow CJ, Bruce SS, Rae AI, Sheth SA, McKhann GM, Sisti MB, Bruce JN, Sonabend AM, Wang TJC (2018) Solitary-fibrous tumor/hemangiopericytoma of the central nervous system: a population-based study. J Neurooncol 138(1):173–182. https://doi.org/10.1007/s11060-018-2787-7
Sung KS, Moon JH, Kim EH, Kang SG, Kim SH, Suh CO, Kim SH, Lee KS, Chang WS, Chang JH (2018) Solitary fibrous tumor/hemangiopericytoma: treatment results based on the 2016 WHO classification. J Neurosurg. https://doi.org/10.3171/2017.9.jns171057
Zeng L, Wang Y, Wang Y, Han L, Niu H, Zhang M, Ke C, Chen J, Lei T (2017) Analyses of prognosis-related factors of intracranial solitary fibrous tumors and hemangiopericytomas help understand the relationship between the two sorts of tumors. J Neurooncol 131(1):153–161. https://doi.org/10.1007/s11060-016-2282-y
Kim JH, Jung H-W, Kim Y-S, Kim CJ, Hwang S-K, Paek SH, Kim DG, Kwun BD (2003) Meningeal hemangiopericytomas. Surg Neurol 59(1):47–53. https://doi.org/10.1016/s0090-3019(02)00917-5
Trifiletti DM, Mehta GU, Grover S, Sheehan JP (2017) Clinical management and survival of patients with central nervous system hemangiopericytoma in the National Cancer Database. J Clin Neurosci 44:169–174. https://doi.org/10.1016/j.jocn.2017.06.036
Lee EJ, Kim JH, Park ES, Khang SK, Cho YH, Hong SH, Kim CJ (2016) The impact of postoperative radiation therapy on patterns of failure and survival improvement in patients with intracranial hemangiopericytoma. J Neurooncol 127(1):181–190. https://doi.org/10.1007/s11060-015-2030-8
Jeon SH, Park SH, Kim JW, Park CK, Paek SH, Kim IH (2018) Efficacy of adjuvant radiotherapy in the intracranial hemangiopericytoma. J Neurooncol 137(3):567–573. https://doi.org/10.1007/s11060-018-2746-3
Ratneswaren T, Hogg FRA, Gallagher MJ, Ashkan K (2018) Surveillance for metastatic hemangiopericytoma-solitary fibrous tumors-systematic literature review on incidence, predictors and diagnosis of extra-cranial disease. J Neurooncol 138(3):447–467. https://doi.org/10.1007/s11060-018-2836-2
Giordan E, Marton E, Wennberg AM, Guerriero A, Canova G (2020) A review of solitary fibrous tumor/hemangiopericytoma tumor and a comparison of risk factors for recurrence, metastases, and death among patients with spinal and intracranial tumors. Neurosurg Rev. https://doi.org/10.1007/s10143-020-01335-x
Cohen-Inbar O, Lee CC, Mousavi SH, Kano H, Mathieu D, Meola A, Nakaji P, Honea N, Johnson M, Abbassy M, Mohammadi AM, Silva D, Yang HC, Grills I, Kondziolka D, Barnett GH, Lunsford LD, Sheehan J (2017) Stereotactic radiosurgery for intracranial hemangiopericytomas: a multicenter study. J Neurosurg 126(3):744–754. https://doi.org/10.3171/2016.1.JNS152860
Funding
There are no funding sources to report.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
There is no conflict of interest.
Consent to participate
Because of its retrospective manner, informed consent was waived.
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee (Asan Medical Center, reference No. 2020-1882) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shin, DW., Kim, J.H., Chong, S. et al. Intracranial solitary fibrous tumor/hemangiopericytoma: tumor reclassification and assessment of treatment outcome via the 2016 WHO classification. J Neurooncol 154, 171–178 (2021). https://doi.org/10.1007/s11060-021-03733-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-021-03733-7