Abstract
Introduction
Palliative care (PC) for patients with neuro-oncological diseases positively impacts morbidity and mortality. No studies have evaluated whether neuro-oncology fellows receive formal PC education during fellowship. The purpose of this study was to describe the PC education and identify education needs of US neuro-oncology fellowship programs.
Methods
Program directors (PDs) of US neuro-oncology fellowships were surveyed. The electronic survey included qualitative and quantitative questions.
Results
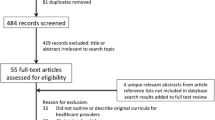
Of 26 programs with fellows, 17 completed surveys (65% response rate) of which 3 (18%) offered no formal PC education. The methods most utilized were formal didactics (seminars/conferences) and self-directed reading materials. One-third of programs have developed their own teaching materials. Communication was the domain identified as most important, the domain fellows were most well-trained in, and the domain PDs felt most comfortable providing for their own patients. Addressing spiritual distress and initiating life-prolonging therapies were the domains PDs identified as being least important, fellows were least well trained in, and PDs were least comfortable providing for their own patients. Most programs (83%) were satisfied with the PC education available at their program. Time for teaching and faculty availability were the most common barriers.
Conclusions
Neuro-oncology PDs recognize the need for PC education, which is currently offered in some form by most programs, but the content and methods of delivery are heterogenous. Interdisciplinary educational teams and nationally-available PC educational material may improve implementation of PC education in neuro-oncology.




Similar content being viewed by others
References
Robinson MT, Holloway RG (2017) Palliative care in neurology. Mayo Clin Proc 92:1592–1601. https://doi.org/10.1016/j.mayocp.2017.08.003
Holloway RG, Ladwig S, Robb J et al (2010) Palliative care consultations in hospitalized stroke patients. J Palliat Med 13:407–412. https://doi.org/10.1089/jpm.2009.0278
Creutzfeldt CJ, Engelberg RA, Healey L et al (2015) Palliative care needs in the neuro-ICU. Crit Care Med 43:1677–1684. https://doi.org/10.1097/CCM.0000000000001018
Holloway RG, Gramling R, Kelly AG (2013) Estimating and communicating prognosis in advanced neurologic disease. Neurology 80:764–772. https://doi.org/10.1212/WNL.0b013e318282509c
Habibi A, Wu SP, Gorovets D et al (2018) Early palliative care for patients with brain metastases decreases inpatient admissions and need for imaging studies. Am J Hosp Palliat Med. https://doi.org/10.1177/1049909118765405
Weissman DE, Block SD (2002) ACGME requirements for end-of-life training in selected residency and fellowship programs: a status report. Acad Med 77:299–304. https://doi.org/10.1097/00001888-200204000-00008
Schuh LA, Adair JC, Drogan O (2009) Education research: neurology residency training in the new millennium. Neurology 72:15–20. https://doi.org/10.1212/01.wnl.0000342389.60811.ca
Provinciali L, Carlini G, Tarquini D et al (2016) Need for palliative care for neurological diseases. Neurol Sci 37:1581–1587. https://doi.org/10.1007/s10072-016-2614-x
Lin E, Rosenthal MA, Le BH, Eastman P (2012) Neuro-oncology and palliative care: a challenging interface. Neuro-Oncology 14:3–7. https://doi.org/10.1093/neuonc/nos209
ACGME program requirements for graduate medical education in neurology [Internet] (2017) Available from: http://www.acgme.org/Portals/0/PFAssets/ProgramRequirements/180_neurology_2017-07-01.pdf?ver=2017-05-25-083934-447. Accessed 24 Oct 2017
Creutzfeldt CJ, Holloway RG, Curtis JR (2015) Palliative care: a core competency for stroke neurologists. Stroke 46:2714–2719. https://doi.org/10.1161/STROKEAHA.115.008224
Mehta AK, Najjar S, May N et al A needs assessment of palliative care education among U.S. adult neurology residency programs. J Palliat Med (in press)
Kraus CK, Greenberg MR, Ray DE, Dy SM (2016) Palliative care education in emergency medicine residency training: a survey of program directors, associate program directors, and assistant program directors. J Pain Symptom Manage 51:898–906. https://doi.org/10.1016/j.jpainsymman.2015.12.334
Irwin SA, Montross LP, Bhat RG et al (2011) Psychiatry resident education in palliative care: opportunities, desired training, and outcomes of a targeted educational intervention. Psychosomatics 52:530–536. https://doi.org/10.1016/j.psym.2011.08.002
Lefkowits C, Sukumvanich P, Claxton R et al (2014) Needs assessment of palliative care education in gynecologic oncology fellowship: we’re not teaching what we think is most important. Gynecol Oncol 135:255–260. https://doi.org/10.1016/j.ygyno.2014.08.016
Richman PS, Saft HL, Messina CR et al (2016) Palliative and end-of-life educational practices in US pulmonary and critical care training programs. J Crit Care 31:172–177. https://doi.org/10.1016/j.jcrc.2015.09.029
Hussain J, Adams D, Campbell C (2013) End-of-life care in neurodegenerative conditions: outcomes of a specialist palliative neurology service. Int J Palliat Nurs 19:162–169. https://doi.org/10.12968/ijpn.2013.19.4.162
Schuh LA, Biondo A, An A et al (2007) Neurology resident learning in an end-of-life/palliative care course. J Palliat Med 10:178–181. https://doi.org/10.1089/jpm.2006.0089
Robinson K, Sutton S, von Gunten CF et al (2004) Assessment of the education for physicians on end-of-life care (EPEC) project. J Palliat Med 7:637–645
Catt S, Chalmers A, Fallowfield L (2008) Psychosocial and supportive-care needs in high-grade glioma. Lancet Oncol 9:884–891. https://doi.org/10.1016/S1470-2045(08)70230-4
Walbert T, Glantz M, Schultz L, Puduvalli VK (2016) Impact of provider level, training and gender on the utilization of palliative care and hospice in neuro-oncology: a North-American survey. J Neuro-Oncol 126:337–345
Walbert T (2014) Integration of palliative care into the neuro-oncology practice: patterns in the United States. Neuro-Oncol Pract 1:3–7
Von Gunten CF, Twaddle M, Preodor M et al (2005) Evidence of improved knowledge and skills after an elective rotation in a hospice and palliative care program for internal medicine residents. Am J Hosp Palliat Med 22:195–203. https://doi.org/10.1177/104990910502200309
Carver AC, Vickrey BG, Bernat JL et al (1999) End-of-life care: a survey of US neurologists’ attitudes, behavior, and knowledge. Neurology 53:284–293. https://doi.org/10.1212/WNL.53.2.284
Author information
Authors and Affiliations
Contributions
AKM: conceptualized, developed and wrote the survey, and wrote this manuscript. NM: developed and wrote the survey and reviewed the final manuscript. SV: assisted with review and formatting of the final manuscript. CEF: assisted with the distribution, writing, and review of the survey and contributed to the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest to disclose. This study was not industry-sponsored.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mehta, A.K., May, N., Verga, S. et al. Palliative care education in U.S. adult neuro-oncology fellowship programs. J Neurooncol 140, 377–383 (2018). https://doi.org/10.1007/s11060-018-2963-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-018-2963-9