Abstract
Ulcerative colitis (UC) is an idiopathic, chronic and relapsing colonic inflammatory disease. Despite the involvement of diverse intricate mechanisms, COX mediated inflammatory pathway is crucial in the pathophysiology of colitis. Thus, COX inhibition is imperative for managing colitis-associated inflammation. However, the use of COX inhibitory classical non-steroidal anti-inflammatory drugs (NSAIDs) for inflammation resolution has been linked to sudden increased flare-ups. Therefore, considering the anti-inflammatory and pro-resolution effects of antioxidant and essential trace element Selenium (Se), a Seleno-derivative of Celecoxib called Selenocoxib-3 was characterized and evaluated for its favourable pharmacokinetics, safety margins and anti-inflammatory therapeutic potential in DSS-induced experimental colitis. The serum pharmacokinetic profiling [elimination rate constant (K) and clearance (Cl) and toxicity profiling suggested enhanced efficacy, therapeutic potential and lesser toxicity of Selenocoxib-3 as compared to its parent NSAID Celecoxib. In vivo studies demonstrated that Selenocoxib-3 efficiently resolves the gross morphological signs of DSS-induced colitis such as diarrhoea, bloody stools, weight loss and colon shortening. Further, intestinal damage evaluated by H & E staining and MPO activity suggested of histopathological disruptions, such as neutrophil infiltration, mucodepletion and cryptitis, by Selenocoxib-3. The expression profiles of COX-1/2 demonstrated mitigation of pro-inflammatory mediators thereby promoting anti-inflammatory efficacy of Selenocoxib-3 when compared with Celecoxib. The current study suggests translational applicability of Se-containing novel class of COX inhibitors for efficiently managing inflammatory disorders such as UC.









Similar content being viewed by others
Data availability
The authors declare that all data supporting the findings of this study are available within the article.
References
Long MD, Kappelman MD, Martin CF, Chen W, Anton K, Sandler RS et al (2016) Role of non-steroidal anti-inflammatory drugs in exacerbations of inflammatory bowel disease. J Clin Gastroenterol 50(2):152–156. https://doi.org/10.1097/MCG.0000000000000421
Klein A, Eliakim R (2010) Non steroidal anti-inflammatory drugs and inflammatory bowel disease. Pharmaceuticals 3(4):1084–1092. https://doi.org/10.3390/ph3041084
Garcίa-Rayado G, Navarro M, Lanas A (2018) NSAID induced gastrointestinal damage and designing GI-sparing NSAIDs. Expert Rev Clin Pharmacol 11(10):1031–1043. https://doi.org/10.1080/17512433.2018.1516143
Bjarnason I, Scarpignato C, Holmgren E, Olszewski M, Rainsford KD, Lanas A (2018) Mechanisms of damage to the gastrointestinal tract from nonsteroidal anti-inflammatory drugs. Gastroenterology 154(3):500–514. https://doi.org/10.1053/j.gastro.2017.10.049
Brune K, Patrignani P (2015) New insights into the use of currently available non-steroidal anti-inflammatory drugs. J Pain Res 8:105–118. https://doi.org/10.2147/JPR.S75160
Luo C, Zhang H (2017) The role of proinflammatory pathways in the pathogenesis of colitis-associated colorectal cancer. Mediat Inflamm 2017:1–8. https://doi.org/10.1155/2017/5126048
Whitfield-cargile CM, Cohen ND, Chapkin RS, Weeks BR, Davidson LA, Goldsby JS et al (2016) The microbiota-derived metabolite indole decreases mucosal inflammation and injury in a murine model of NSAID enteropathy. Gut Microbes 7(3):246–261. https://doi.org/10.1080/19490976.2016.1156827
Li Y, Soendergaard C, Bergenheim FH, Aronoff DM, Milne G, Riis LB, Seidelin JB, Jensen KB, Neilson OH (2018) COX-2–PGE2 signaling impairs intestinal epithelial regeneration and associates with TNF inhibitor responsiveness in ulcerative colitis. EBioMedicine 36:497–507. https://doi.org/10.1016/j.ebiom.2018.08.040
Pal S, Bhattacharjee A, Ali A, Mandal NC, Mandal SC, Pal M (2014) Chronic inflammation and cancer: potential chemoprevention through nuclear factor kappa B and p53 mutual antagonism. J Inflamm 11(23):1–28. https://doi.org/10.1186/1476-9255-11-23
Landskron G, De la Fuente M, Thuwajit P, Thuwajit C, Hermoso MA (2014) Chronic inflammation and cytokines in the tumor microenvironment. J Immunol Res 2014:1–19. https://doi.org/10.1155/2014/149185
Kefalakes H, Stylianides TJ, Amanakis G, Kolios G (2009) Exacerbation of inflammatory bowel diseases associated with the use of nonsteroidal anti-inflammatory drugs: myth or reality? Eur J Clin Pharmacol 65:963–970. https://doi.org/10.1007/s00228-009-0719-3
Beales ILP (2018) Time to reappraise the therapeutic place of celecoxib. Ther Adv Chronic Dis 9(5):107–110. https://doi.org/10.1080/10717544.2016.117882
Grosser T, Ricciotti E, FitzGerald GA (2017) The cardiovascular pharmacology of nonsteroidal anti-inflammatory drugs. Trends Pharmacol Sci 38(8):733–748. https://doi.org/10.1016/j.tips.2017.05.008
Kaushal N, Kudva AK, Patterson AD, Chiaro C, Kennett MJ, Desai D (2014) Crucial role of macrophage selenoproteins in experimental colitis. J Immunol 193(7):3683–3692. https://doi.org/10.4049/jimmunol.1400347
Barrett CW, Singh KS, Motley AK, Lintel MK, Matafonova E, Bradley AM et al (2013) Dietary selenium deficiency exacerbates DSS-induced epithelial injury and AOM/DSS-induced tumorigenesis. PLoS ONE 8(7):e67845. https://doi.org/10.1371/journal.pone.0067845
Krehl S, Loewinger M, Florian S, Kipp AP, Banning A, Wessjohann LA (2012) Glutathione peroxidase-2 and selenium decreased inflammation and tumors in a mouse model of inflammation-associated carcinogenesis whereas sulforaphane effects differed with selenium supply. Carcinogenesis 33(3):620–628. https://doi.org/10.1093/carcin/bgr288
Desai D, Kaushal N, Gandhi UH, Arner RJ, D’Souza C, Chen G et al (2010) Synthesis and evaluation of the anti-inflammatory properties of selenium-derivatives of celecoxib. Chem Biol Interact 188(3):446–456. https://doi.org/10.1016/j.cbi.2010.09.021
Malhotra S, Welling MN, Mantri SB, Desai K (2016) In vitro and in vivo antioxidant, cytotoxic, and anti-chronic inflammatory arthritic effect of selenium nanoparticles: in vitro and in vivo effect of SeNP. J Biomed Mater Res Appl Biomater 104(5):993–1003. https://doi.org/10.1002/jbm.b.33448
Tagaram HRS, Desai D, Li G, Liu D, Rountree CB, Gowda K et al (2016) A selenium containing inhibitor for the treatment of hepatocellular cancer. Pharmaceuticals 9(2):18. https://doi.org/10.3390/ph9020018
Scholz M, Ulbrich HK, Dannhardt G (2008) Investigations concerning the COX/5-LOX inhibiting and hydroxyl radical scavenging potencies of novel 4,5-diaryl isoselenazoles. Eur J Med Chem 43(6):1152–1159. https://doi.org/10.1016/j.ejmech.2007.09.007
Gandhi UH, Kaushal N, Ravindra KC, Hegde S, Nelson SM, Narayan V et al (2011) Selenoprotein-dependent up-regulation of hematopoietic prostaglandin D2 synthase in macrophages is mediated through the activation of peroxisome proliferator-activated receptor (PPAR) gamma. J Biol Chem 286(31):27471–27482. https://doi.org/10.1074/jbc.M111.260547
Kaur R, Thakur S, Rastogi P, Kaushal N (2018) Resolution of Cox mediated inflammation by Se supplementation in mouse experimental model of colitis. PLoS ONE 13(7):e0201356. https://doi.org/10.1371/journal.pone.0201356
Desai D, Sihna I, Null K, Wolter W, Suckow MA, King T et al (2010) Synthesis and antitumor properties of selenocoxib-1 against rat prostate adenocarcinoma cells. Int J Cancer 127(1):230–238. https://doi.org/10.1002/ijc.25033
Mamidi RNVS, Mullangi R, Kota J, Bhamidipati R, Khan AA, Katneni K et al (2002) Pharmacological and pharmacokinetic evaluation of celecoxib prodrugs in rats. Biopharm Drug Dispos 23(7):273–282. https://doi.org/10.1002/bdd.319
Mouillé B, Delpal S, Mayeur C, Blachier F (2003) Inhibition of human colon carcinoma cell growth by ammonia: a non-cytotoxic process associated with polyamine synthesis reduction. Biochim Biophys Acta 1624(1–3):88–97
Piplani H, Vaish V, Sanyal S (2012) Dolastatin 15, a mollusk linear peptide, and celecoxib, a selective cyclooxygenase-2 inhibitor, prevent preneoplastic colonic lesions and induce apoptosis through inhibition of the regulatory transcription factor NF-κB and an inflammatory protein, iNOS. Eur J Cancer Prev 21(6):511–522
Winter CA, Risley EA, Nuss GW (1962) Carrageenin-induced edema in hind paw of the rat as an assay for antiiflammatory drugs. Proc Soc Exp Biol Med 111:544–7. https://doi.org/10.3181/00379727-111-27849
Cong HH, Khaziakhmetova VN, Zigashina LE (2015) Rat paw oedema modeling and NSAIDs: timings of effects. Int J Risk Saf Med 27(1):S76–S77. https://doi.org/10.3233/JRS-150697
Hess SM, Milonig RC (1972) Assay for anti-inflammatory drugs. In: Lepow IH, Ward PA (eds) Inflammation, mechanisms and control. Academic Press, New York, pp 1–22
Re R, Pellegrini N, Proteggente A, Yang M, Rice-Evans C (1999) Antioxidant activity applying an improved ABTS radical cation decolorization assay. Free Radic Biol Med 26:1231–7. https://doi.org/10.1016/S0891-5849(98)00315-3
Brand-Williams W, Cuvelier ME, Berset C (1995) Use of a free radical method to evaluate antioxidant activity. LWT 28:25–30. https://doi.org/10.1016/S0023-6438(95)80008-5
Taghipour N, Molaei M, Mosaffa N, Rostami-Nejad M, Aghdaei HA, Anissian A et al (2016) An experimental model of colitis induced by dextran sulfate sodium from acute progresses to chronicity in C57BL/6: correlation between conditions of mice and the environment. Gastroenterol Hepatol Bed Bench 9(1):45–52
Sklyarov AY, Panasyuk NB, Fomenko IS (2011) Role of nitric oxide-synthase and cyclooxygenase/lipooxygenase systems in development of experimental ulcerative colitis. J Physiol Pharmacol 62(1):65–73
Zhang C, He A, Liu S, He Q, Luo Y, He Z et al (2019) Inhibition of HtrA2 alleviated dextran sulfate sodium (DSS)-induced colitis by preventing necroptosis of intestinal epithelial cells. Cell Death Dis 10:344. https://doi.org/10.1038/s41419-019-1580-7
Istrate C, Hagbom M, Vikström E, Magnusson K, Svensson L (2014) Rotavirus infection increases intestinal motility but not permeability at the onset of diarrhea. J Virol 88(6):3161–3169. https://doi.org/10.1128/JVI.02927-13
Siegmund B, Zeitz M (2009) Clinical aspects of inflammatory bowel disease. Eur J Immunol 39(8):2026–2030. https://doi.org/10.1002/eji.200939601
Kim Y, Wu AG, Jaja-Chimedza A, Graf BL, Waterman C, Verzi MP et al (2017) Isothiocyanate-enriched moringa seed extract alleviates ulcerative colitis symptoms in mice. PLoS ONE 12(9):e0184709. https://doi.org/10.1371/journal.pone.0184709
Bradley PP, Priebat DA, Christensen RD, Rothstein G (1982) Measurement of cutaneous inflammation: estimation of neutrophil content with an enzyme marker. J Investig Dermatol 78(3):206–209. https://doi.org/10.1111/1523-1747.ep12506462
Balasubramaniam P, Malathi A (1992) Comparative study of hemoglobin estimated by Drabkin’s and Sahli’s methods. J Postgrad Med 38:8–9
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with Folin phenol reagent. J Biol Chem 193:265–275
Ranawat P, Bansal MP (2010) Modulatory effects of selenium on spermatogenesis: involvement of transcription factors CREB and CREM. J Biomed Sci 2(4):329–341
Jacoby RF, Seibert K, Cole CE, Kelloff G, Lubet RA (2000) The cyclooxygenase-2 inhibitor celecoxib is a potent preventive and therapeutic agent in the min mouse model of adenomatous polyposis. Cancer Res 60(18):5040–5044
Bazan L, Bendas ER, El Gazayerly ON, Badawy SS (2016) Comparative pharmaceutical study on colon targeted micro-particles of celecoxib: in-vitro-in-vivo evaluation. Drug Deliv 23(9):3339–3349
Pirlamarla P, Bond RM (2016) FDA labeling of NSAIDs: review of nonsteroidal anti-inflammatory drugs in cardiovascular disease. Trends Cardiovasc Med 26(8):675–680. https://doi.org/10.1016/j.tcm.2016.04.011
Miao X, Li J, Ouyang Q, Hu R, Zhang Y, Li H (2014) Tolerability of selective cyclooxygenase 2 inhibitors used for the treatment of rheumatological manifestations of inflammatory bowel disease. Cochrane Database Syst Rev 23(10):CD007744.10. https://doi.org/10.1002/14651858.CD007744.pub2
Park K, Choi J, Kim W, Min J, Park S, Cho C (2012) The efficacy of tramadol/acetaminophen combination tablets (Ultracet ®) as add-on and maintenance therapy in knee osteoarthritis pain inadequately controlled by nonsteroidal anti-inflammatory drugs (NSAID). Clin Rheumatol 31(2):317–323. https://doi.org/10.1007/s10067-011-1818-y
El Hajj II, Malik SM, Alwakeel HR, Shaikh OS, Sasatomi E, Kandil HM (2009) Celecoxib-induced cholestatic liver failure requiring orthotopic liver transplantation. World J Gastroenterol 15(31):3937–3939. https://doi.org/10.3748/wjg.15.3937
Aziz ND, Ouda MH, Ubaid MM (2018) Comparing the toxic effects of nonsteroidal anti-inflammatory drugs (celecoxib and ibuprofen) on heart, liver, and kidney in rats. Asian J Pharm Clin Res 11(6):482–485. https://doi.org/10.22159/ajpcr.2018.v11i6.25487
Bykov IL, Palmen M, Rainsford KD, Lindros KO (2006) Chronic effects of celecoxib, a cyclooxygenase-2 inhibitor, cause enhanced alcohol-induced liver steatosis in rats. Inflammopharmacology 14(1–2):36–41. https://doi.org/10.1007/s10787-006-1506-8
Carrillo-Jimenez R, Nurnberger M (2000) Celecoxib-induced acute pancreatitis hepatitis: a case report. Arch Intern Med 160(4):553–554. https://doi.org/10.1001/archinte.160.4.553
Gong L, Thorn CF, Bertagnolli MM, Grosser T, Altman RB, Klein TE (2012) Celecoxib pathways: pharmacokinetics and pharmacodynamics. Pharmacogenet Genomics 22(4):310–318. https://doi.org/10.1097/FPC.0b013e32834f94cb
Yu Y, Stubbe J, Ibrahim S, Song WL, Symth EM, Funk CD et al (2010) Cyclooxygenase-2-dependent prostacyclin formation and blood pressure homeostasis: targeted exchange of cyclooxygenase isoforms in mice. Circ Res 106(2):337–345. https://doi.org/10.1161/CIRCRESAHA.109.204529
Hörl WH (2010) Nonsteroidal anti-inflammatory drugs and the kidney. Pharmaceuticals 3(7):2291–2321. https://doi.org/10.3390/ph3072291
Dinchuk JE, Car BD, Focht RJ, Johnston JJ, Jaffee BD, Covington MB et al (1995) Renal abnormalities and an altered inflammatory response in mice lacking cyclooxygenase II. Nature 378(6555):406–409. https://doi.org/10.1038/378406a0
Davis B, Morris T (1993) Physiological parameters in laboratory animals and humans. Pharm Res 10(7):1093–1095. https://doi.org/10.1023/A:1018943613122
Saad J, Mathew D (2020) Nonsteroidal anti-inflammatory drugs (NSAID) toxicity. StatPearls, Treasure Island
Palleria C, Paolo AD, Giofŕe C, Caglioti C, Leuzzi G, Siniscalchi A et al (2013) Pharmacokinetics drug–drug interaction and their implication in clinical. J Res Med Sci 18(7):601–610
Gonzalez D, Schmidt S, Derendorf H (2013) Importance of relating efficacy measures to unbound drug concentrations for anti-infective agents. Clin Microbio Rev 26(2):274–288. https://doi.org/10.1128/CMR.00092-12
Calatayud S, Esplugues JV (2016) Chemistry, pharmacodynamics, and pharmacokinetics of NSAIDs. In: Lanas A (ed) NSAIDS and aspirin. Springer, Cham, pp 3–16. https://doi.org/10.1007/978-3-319-33889-7_1
Malik MY, Jaiswal S, Sharma A, Shukla M, Lal J (2016) Role of enterohepatic recirculation in drug disposition: cooperation and complications. Drug Metab Rev 48(2):281–327. https://doi.org/10.3109/03602532.2016.1157600
Xiao L, Pan G (2017) An important intestinal transporter that regulates the enterohepatic circulation of bile acids and cholesterol homeostasis: the apical sodium-dependent dile acid transporter (SLC10A2/ASBT). Clin Res Hepatol Gastroenterol 41(5):509–515. https://doi.org/10.1016/j.clinre.2017.02.001
Davies NM, McLachlan AJ, Williams Day RO, KM, (2000) Clinical pharmacokinetics and pharmacodynamics of celecoxib. Clin Pharmacokinet 38(3):225–242. https://doi.org/10.2165/00003088-200038030-00003
Moore RA, Derry S, McQuay HJ (2007) Cyclo-oxygenase-2 selective inhibitors and nonsteroidal anti-inflamatory drugs: balancing gastrointestinal and cardiovascular risk. BMC Musculoskelet Disor 8:73. https://doi.org/10.1186/1471-2474-8-73
Sheta NM, Boshra SA (2021) Fabrication and evaluation of celecoxib oral oleogel to reduce the inflammation of ulcerative colitis. AAPS PharmSciTech 22:180. https://doi.org/10.1208/s12249-021-02042-6
Mishra RK, Ahmad A, Kumar A, Vyawahare A, Raza SS, Khan R (2020) Lipid-based nanocarrier-mediated targeted delivery of celecoxib attenuate severity of ulcerative colitis. Mater Sci Eng C 116:111103. https://doi.org/10.1016/j.msec.2020.111103
Guirguis MS, Sattari S, Jamali F (2001) Pharmacokinetics of celecoxib in the presence and absence of interferon induced acute inflammation in the rat: application of a novel HPLC assay. J Pharm Pharmaceut Sci 4(1):1–6
Bertagnolli MM, Eagle CJ, Zauber AG, Redston M, Breazna A, Kim K et al (2009) Five-year efficacy and safety analysis of the adenoma prevention with celecoxib trial. Cancer Prev Res 2(4):310–321. https://doi.org/10.1158/1940-6207.CAPR-08-0206
Ghanghas P, Sharma M, Desai D, Raza K, Bhalla A, Kumar P et al (2021) Selenium-based novel epigenetic regulators offer effective chemotherapeutic alteranative with wider safety margins in experimental colorectal cancer. Biol Trace Elem Res. https://doi.org/10.1007/s12011-021-02659-5
Miao X, Xu J, Lin A, Wu X, Wu L, Xie W (2018) Recent advances for the synthesis of selenium-containing small molecules as potent antitumor agents. Curr Med Chem 25(17):2009–2033. https://doi.org/10.2174/0929867325666171129220544
Alcoleo V, Plano D, Karelia DN, Palop JA, Amin S, Sanmartin C et al (2016) Novel seleno- and thio-urea derivatives with potent in vitro activities against several cancer cell lines. Eur J Med Chem 113:134–144. https://doi.org/10.1016/j.ejmech.2016.02.042
Okayasu I, Hatakeyama S, Yamada M, Ohkusa T, Inagaki Y, Nakaya R (1990) A novel method in the induction of reliable experimental acute and chronic ulcerative colitis in mice. Gastroenterology 98:694–702. https://doi.org/10.1016/0016-5085(90)90290-h
Chandna N, Kumar S, Kaushik P, Kaushik D, Roy SK, Gupta GK, Jachak SM, Kapoor JK, Sharma PK (2013) Synthesis of novel celecoxib analogues by bioisosteric replacement of sulfonamide as potent anti-inflammatory agents and cyclooxygenase inhibitors. Bioorg Med Chem 21(15):4581–4590. https://doi.org/10.1002/jmv.23282
Süleyman H, Demircan B, Karagöz Y, Oztaşan N, Süleyman B (2004) Anti-inflammatory effects of selective COX-2 inhibitors. Pol J Pharmacol 56(6):775–780
Oertel S, Scholich K, Weigert A, Thomas D, Schmetzer J, Trautmann S et al (2017) Ceramide synthase 2 deficiency aggravates AOM-DSS-induced colitis in mice: role of colon barrier integrity. Cell Mol Life Sci 74(16):3039–3055. https://doi.org/10.1007/s00018-017-2518-9
Song C, Kim N, Sohn SH, Lee SM, Nam RH, Na HY, Lee DH, Surh Y (2018) Effects of 17β-estradiol on colonic permeability and inflammation in an azoxymethane/dextran sulfate sodium-induced colitis mouse model. Gut Liver 12(6):682–693. https://doi.org/10.5009/gnl18221
Ringstad J, Kildebo S, Thomassen Y (1993) Serum selenium, copper, and zinc concentrations in crohn’s disease and ulcerative colitis. Scand J Gastroenterol 28(7):605–608. https://doi.org/10.3109/00365529309096096
Tozaki H, Odoriba T, Okada N, Fujita T, Terabe A, Suzuki T et al (2002) Chitosan capsules for colon-specific drug delivery: enhanced localization of 5-aminosalicylic acid in the large intestine accelerates healing of TNBS-induced colitis in rats. J Control Release 82(1):51–61. https://doi.org/10.1016/S0168-3659(02)00084-6
Elsherif Y, Alexakis C, Mendall M (2014) Determinants of weight loss prior to diagnosis in inflammatory bowel disease: a retrospective observational study. Gastroenterol Res Pract 2014:762191. https://doi.org/10.1155/2014/762191
Olesen M, Ericksson S, Bohr J, Järnerot G, Tysk C (2004) Lymphocytic colitis: a retrospective clinical study of 199 Swedish patients. Gut 53(4):536–541. https://doi.org/10.1136/gut.2003.023440
Aviello G, Knaus UG (2017) ROS in gastrointestinal inflammation: rescue or sabotage? Br J Pharmacol 174(12):1704–1718. https://doi.org/10.1111/bph.13428
Dalton TP, Chen Y, Schneider SN, Nebert DW, Shertzer HG (2004) Genetically altered mice to evaluate glutathione homeostasis in health and disease. Free Radic Biol Med 37(10):1511–1526. https://doi.org/10.1016/j.freeradbiomed.2004.06.040
Bhattacharyya S, Dudeja PK, Tobacman JK (2009) ROS, Hsp27, and IKK mediate dextran sodium sulfate (DSS) activation of IBa, NFB, and IL-8. Inflamm Bowel Dis 15(5):673–683
Acknowledgements
Dr. Pulkit Rastogi [Assistant Professor, Department of Haematology, Post Graduate Institute of Medical Education and Research (PGIMER)], for histopathological analysis of colon sections.
Funding
The work was supported by Senior Research Fellowship (SRF) sanctioned to Ms. Ramanpreet Kaur by Indian Council of Medical Research (ICMR) (No. 45/42/2019-BIO/BMS).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
11010_2022_4532_MOESM1_ESM.tif
Supplementary file1 (TIF 450 KB)—Figure S1. a–c Shows comparison of in vitro cytotoxicity of Selenocoxib-3 and Celecoxib using MTT assay at a time interval of 12 h. The data are expressed as mean ± SD of at four independent observations and analyzed using one-way ANOVA (Tukey’s multiple comparison method). a Represents p < 0.05 when compared between Selenocoxib-3 vs Celecoxib at any time interval.
11010_2022_4532_MOESM2_ESM.tif
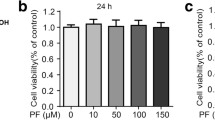
Supplementary file2 (TIF 464 KB)—Figure S2. a–c Shows comparison of in vitro cytotoxicity of Selenocoxib-3 and Celecoxib using MTT assay at a time interval of 24 h. The data are expressed as mean ± SD of at four independent observations and analyzed using one-way ANOVA (Tukey’s multiple comparison method). a Represents p < 0.05 when compared between Selenocoxib-3 vs Celecoxib at any time interval.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kaur, R., Desai, D., Amin, S. et al. Selenocoxib-3, a novel anti-inflammatory therapeutic effectively resolves colitis. Mol Cell Biochem 478, 621–636 (2023). https://doi.org/10.1007/s11010-022-04532-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-022-04532-y