Abstract
Introduction
Vascular access site complications are among the most frequently observed complications after catheter ablation of atrial fibrillation (AF). We sought to determine whether implementation of a three-point strategy would reduce major vascular complications resulting from catheter ablation of atrial fibrillation.
Methods
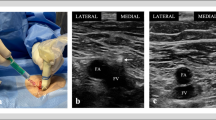
Three hundred twenty-four consecutive patients undergoing catheter ablation of AF were studied: 162 in each group (with and without the test strategy). The three-point test strategy included the following: (1) performing the procedure on Warfarin with an INR from 2.0 to 3.5 (mean INR of 2.44), rather than stopping Warfarin prior to the procedure and bridging the patient back to Warfarin with low molecular heparin, (2) using a small 21 G needle to obtain femoral vein access rather than a larger 18 G needle, and (3) eliminating the use of femoral arterial access. Major vascular complications were defined as complications requiring either blood transfusion or surgical/percutaneous repair.
Results
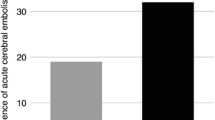
Major vascular complications were identified in 6/162 (3.7%) of the control patients without the strategy listed above compared to 0/162 (0%) in the test patients with implementations of this strategy (p = 0.03). The frequency of other complications was comparable between the two groups (tamponade requiring drainage: 1/162 control, 1/162 test; pericardial effusion not requiring drainage: 0/162 control, 1/162 test; transient ischemic attack: 1/162 control and 1/162 test; stroke: 1/162 control, 0/162 test): (p = NS for each).
Conclusions
A three-point strategy including performing procedures with therapeutic Warfarin, using a small gauge needle to obtain vascular access and eliminating femoral arterial access significantly reduced major vascular access complications and did not affect other major complications, during catheter ablation of AF. Implementation of this strategy may be useful to reduce groin complications resulting from AF ablation.

Similar content being viewed by others
References
Fuster, V., Ryden, L. E., Cannom, D. S., Crinjs, H. J., Curtis, A. B., Ellenbogen, K. A., et al. (2006). ACC/AHA/ESC 2006 Guidelines for the management of patients with atrial fibrillation: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 2001 Guidelines for the management of patients with atrial fibrillation): Developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society. Circulation, 114, e257–e354.
Natale, A., Raviele, A., Arentz, T., Calkins, H., Chen, S. A., & Haissaguerre, M. (2007). Venice Chart International Consensus Document on Atrial Fibrillation Ablation. Journal of Cardiovascular Electrophysiology, 18, 560–580.
Cappato, R., Calkins, H., Chen, S., Davies, W., Yoshito, I., Kalman, J., et al. (2005). Skanes A: worldwide survey on the methods, efficacy and safety of catheter ablation for human atrial fibrillation. Circulation, 111, 1100–1105.
Prudente, L. A., Moorman, J. R., Lake, D., Xiao, Y., Greebaum, H., Mangrum, J. M., et al. (2009). Femoral vascular complications following catheter ablation of atrial fibrillation. Journal of Interventional Cardiovascular Electrophysiology, 26, 59–64.
Dagres, N., Hindricks, G., Kottkamp, H., Sommer, P., Gaspar, T., Bode, K., et al. (2009). Complications of atrial fibrillation ablation in a high- volume center in 1000 procedures: still cause for concern? Journal of Cardiovascular Electrophysiology, 20, 1014–1019.
Ren, J. F., Marchlinski, F. E., Callans, D. J., Gernstenfield, E. P., Dixit, S., Lin, D., et al. (2005). Increased intensity of anticoagulation may reduce the risk of thrombus during atrial fibrillation ablation procedures in patients with spontaneous echocardiographic contrast. Journal of Cardiovascular Electrophysiology, 16, 474–477.
Lemola, K., Desjardin, B., Sneider, M., Case, I., Chugh, A., Good, E., et al. (2005). Effect of Left atrial circumferential ablation for atrial fibrillation on left atrial transport function. Heart Rhythm, 2, 923–928.
Nolan, O., Lashevsky, I., Hamad, A., & Crystal, E. (2005). Non Pharmacologic stroke prevention in atrial fibrillation. Expert Reviews in Cardiovascular Therapeutics, 3, 619–633.
Mortada, M. E., Chandrasekaran, K., Nangia, V., Dhala, A., Blanck, Z., & Cooley, R. (2008). Periprocedural anticoagulation for atrial fibrillation ablation. Journal of Cardiovascular Electrophysiology, 19, 362–366.
Oral, H., Chugh, A., Ozyadin, M., Good, E., Fortino, J., Sankaran, S., et al. (2006). Risk of thromboembolic events after percutaneous left atrial radiofrequency ablation of atrial fibrillation. Circulation, 114, 759–765.
Hussein, A. A., Martin, D. O., Saliba, W., Patel, D., Karim, S., Batal, O., et al. (2009). Radiofrequency ablation of atrial fibrillation under therapeutic international normalized ration: A safe and efficacious periprocedural anticoagulation strategy. Heart Rhythm, 6, 1425–1429.
Wazni, O. M., Beheiry, S., Fahmy, T., Barrett, C., Hao, S., Patel, D., et al. (2007). Atrial Fibrillation Ablation in Patients with therapeutic international normalized Ratio: Comparison of strategies of anticoagulation management in the periprocedural period. Circulation, 116, 2531–2534.
Scherr, D., Sharma, K., Dalal, D., Spragg, D., Chilukuri, K., Cheng, A., et al. (2009). Marine JE etal: Incidence and predictors of periprocedural cerebrovascular accident in patients undergoing catheter ablation of atrial fibrillation. Journal of Cardiovascular Electrophysiology, 20, 1357–1363.
Schimdt, M., Segerson, N. M., Marschang, H., Akoum, N., Rittger, H., Clifford, S. M., et al. (2009). Atrial Fibrillation ablation in patients with therapeutic International normalized ratios. Pacing and Cardiovascular Electrophysiology, 32, 995–999.
Kwak, J. J., Pak, H. N., Jang, J. K., Kim, S. K., Park, J. H., Choi, J. I., et al. (2010). Safety and convenience of continuous Warfarin strategy during the periprocedural period in patients who underwent catheter ablation of atrial fibrillation. Journal of Cardiovascular Electrophysiology, 21(6), 620–625.
Shapiro, M., Cohen, H. L., Crystal, K., & Katz, D. (1992). Ultrasound—guided compression of femoral artery pseudoaneurysm. Journal of Ultrasound in Medicine, 11, 182–183.
Iwashima, S., Ishikawa, T., & Ohzeki, T. (2008). Ultrasound—guided versus landmark—guided femoral vein access in pediatric cardiac catheterization. Pediatric Cardiology, 29, 339–342.
Prabhu, M. V., Juneja, D., Gopal, P. B., Sathyanarayanan, M., Subhramanyam, S., Gandhe, S., et al. (2010). Ultrasound—guided femoral dialysis access placement: A single- center randomized trial. Clinical Journal of the American Society of Nephrology, 5, 235–239.
Dudeck, O., Teichgraeber, U., Podrabsky, P., Haenninen, E. L., Soersensen, R., & Ricke, J. (2004). A Randomized trial assessing the value of ultrasound—guided puncture of the femoral artery for interventional investigations. The International Journal of Cardiovascular Imaging, 20, 363–368.
Financial Disclosure
FA: none, EKH: Boston Scientific (consultant/honoraria/research grants), St. Jude Medical (consultant/honoraria/research grant), CB: St. Jude Medical (research grants),SD: none, DB: none, CC: none, ZK: none, JNR: Biosense Webster (consultant, fellowship support), Boston Scientific (fellowship support), CardioFocus (clinical oversight committee—no compensation), CardioInsight (scientific advisory board), CryoCath (scientific steering committee—no compensation), Medtronic (consultant, fellowship support), St. Jude Medical (fellowship support), MM: St. Jude Medical (research grants), Biosense-Webster (research grants).
Author information
Authors and Affiliations
Corresponding author
Additional information
Fnu Abhishek and E. Kevin Heist contributed equally to this manuscript.
This study was supported in part by MGH Deane Institute for Integrative Research in Atrial Fibrillation and Stroke.
Rights and permissions
About this article
Cite this article
Abhishek, F., Heist, E.K., Barrett, C. et al. Effectiveness of a strategy to reduce major vascular complications from catheter ablation of atrial fibrillation. J Interv Card Electrophysiol 30, 211–215 (2011). https://doi.org/10.1007/s10840-010-9539-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-010-9539-8