Abstract
Purpose
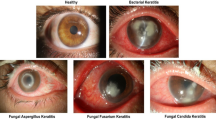
Fungal keratitis is a common cause of blindness worldwide. Timely identification of the causative fungal genera is essential for clinical management. In vivo confocal microscopy (IVCM) provides useful information on pathogenic genera. This study attempted to apply deep learning (DL) to establish an automated method to identify pathogenic fungal genera using IVCM images.
Methods
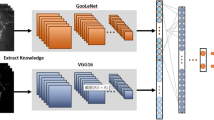
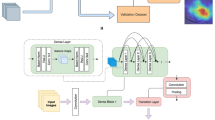
Deep learning networks were trained, validated, and tested using a data set of 3364 IVCM images that collected from 100 eyes of 100 patients with culture-proven filamentous fungal keratitis. Two transfer learning approaches were investigated: one was a combined framework that extracted features by a DL network and adopted decision tree (DT) as a classifier; another was a complete supervised DL model which used DL-based fully connected layers to implement the classification.
Results
The DL classifier model revealed better performance compared with the DT classifier model in an independent testing set. The DL classifier model showed an area under the receiver operating characteristic curves (AUC) of 0.887 with an accuracy of 0.817, sensitivity of 0.791, specificity of 0.831, G-mean of 0.811, and F1 score of 0.749 in identifying Fusarium, and achieved an AUC of 0.827 with an accuracy of 0.757, sensitivity of 0.756, specificity of 0.759, G-mean of 0.757, and F1 score of 0.716 in identifying Aspergillus.
Conclusion
The DL model can classify Fusarium and Aspergillus by learning effective features in IVCM images automatically. The automated IVCM image analysis suggests a noninvasive identification of Fusarium and Aspergillus with clear potential application in early diagnosis and management of fungal keratitis.







Similar content being viewed by others
Abbreviations
- IVCM:
-
In vivo confocal microscopy
- AI:
-
Artificial intelligence
- DL:
-
Deep learning
- Grad-CAM:
-
Gradient-weighted class activation mapping
- DT:
-
Decision tree
- PCA:
-
Principal component analysis
- LightGBM:
-
Light gradient boosting machine
- G-mean:
-
Geometric mean
- ROC:
-
Receiver operating characteristic
- AUC:
-
Area under the ROC curve
- CI:
-
Confidence interval
- DET:
-
Detection error tradeoff
References
Thomas PA (2003) Current perspectives on ophthalmic mycoses. Clin Microbiol Rev 16(4):730–797. https://doi.org/10.1128/CMR.16.4.730-797.2003
Acharya Y, Acharya B, Karki P (2017) Fungal keratitis: study of increasing trend and common determinants. Nepal J Epidemiol 7(2):685–693. https://doi.org/10.3126/nje.v7i2.17975
Kredics L, Narendran V, Shobana CS, Vágvölgyi C, Manikandan P (2015) Indo-Hungarian fungal keratitis working group. Filamentous fungal infections of the cornea: a global overview of epidemiology and drug sensitivity. Mycoses 58(4):243–60. https://doi.org/10.1111/myc.12306
Ahmadikia K, Aghaei Gharehbolagh S, Fallah B, Naeimi Eshkaleti M, Malekifar P, Rahsepar S, Getso MI, Sharma S, Mahmoudi S (2021) Distribution, prevalence, and causative agents of fungal keratitis: a systematic review and meta-analysis (1990 to 2020). Front Cell Infect Microbiol 11:698780. https://doi.org/10.3389/fcimb.2021.698780
Nath R, Baruah S, Saikia L, Devi B, Borthakur AK, Mahanta J (2011) Mycotic corneal ulcers in upper Assam. Indian J Ophthalmol 59:367–371. https://doi.org/10.4103/0301-4738.83613
Leck AK, Thomas PA, Hagan M, Kaliamurthy J, Ackuaku E, John M, Newman MJ, Codjoe FS, Opintan JA, Kalavathy CM, Essuman V, Jesudasan CA, Johnson GJ (2002) Aetiology of suppurative corneal ulcers in Ghana and south India, and epidemiology of fungal keratitis. Br J Ophthalmol 86:1211–1215. https://doi.org/10.1136/bjo.86.11.1211
Chen CA, Hsu SL, Hsiao CH, Ma DH, Sun CC, Yu HJ, Fang PC, Kuo MT (2020) Comparison of fungal and bacterial keratitis between tropical and subtropical Taiwan: a prospective cohort study. Ann Clin Microbiol Antimicrob 19(1):11. https://doi.org/10.1186/s12941-020-00353-3
Brown GD (2011) Innate antifungal immunity: the key role of phagocytes. Annu Rev Immunol 29:1–21. https://doi.org/10.1146/annurev-immunol-030409-101229
Gupta MK, Chandra A, Prakash P, Tilak R (2018) Necessity to identify the causative agent for appropriate treatment in fungal corneal ulcer: an in vitro study. J Mycol Med 28(1):201–205. https://doi.org/10.1016/j.mycmed.2017.07.009
Harbiyeli İİ, Erdem E, Görkemli N, İbayev A, Kandemir H, Açıkalın A, İlkit M, Yağmur M (2022) Clinical and mycological features of fungal keratitis: A retrospective single-center study (2012–2018). Turk J Ophthalmol 52(2):75–85. https://doi.org/10.4274/tjo.galenos.2021.09515
Vemuganti GK, Garg P, Gopinathan U, Naduvilath TJ, John RK, Buddi R, Rao GN (2002) Evaluation of agent and host factors in progression of mycotic keratitis: a histologic and microbiologic study of 167 corneal buttons. Ophthalmology 109(8):1538–1546. https://doi.org/10.1016/s0161-6420(02)01088-6
Ung L, Bispo PJM, Shanbhag SS, Gilmore MS, Chodosh J (2019) The persistent dilemma of microbial keratitis: global burden, diagnosis, and antimicrobial resistance. Surv Ophthalmol 64:255–271. https://doi.org/10.1016/j.survophthal.2018.12.003
Das S, Samant M, Garg P, Vaddavalli PK, Vemuganti GK (2009) Role of confocal microscopy in deep fungal keratitis. Cornea 28(1):11–13. https://doi.org/10.1097/ICO.0b013e318181cff7
Takezawa Y, Shiraishi A, Noda E, Hara Y, Yamaguchi M, Uno T, Ohashi Y (2010) Effectiveness of in vivo confocal microscopy in detecting filamentous fungi during clinical course of fungal keratitis. Cornea 29(12):1346–52. https://doi.org/10.1097/ICO.0b013e3181cd3c84
Chidambaram JD, Prajna NV, Larke N, Macleod D, Srikanthi P, Lanjewar S, Shah M, Lalitha P, Elakkiya S, Burton MJ (2017) In vivo confocal microscopy appearance of Fusarium and Aspergillus species in fungal keratitis. Br J Ophthalmol 101(8):1119–1123. https://doi.org/10.1136/bjophthalmol-2016-309656
Avunduk AM, Beuerman RW, Varnell ED, Kaufman HE (2003) Confocal microscopy of Aspergillus fumigatus keratitis. Br J Ophthalmol 87(4):409–410. https://doi.org/10.1136/bjo.87.4.409
Brasnu E, Bourcier T, Dupas B, Degorge S, Rodallec T, Laroche L, Borderie V, Baudouin C (2007) In vivo confocal microscopy in fungal keratitis. Br J Ophthalmol 91(5):588–591. https://doi.org/10.1136/bjo.2006.107243
Lv J, Zhang K, Chen Q, Chen Q, Huang W, Cui L, Li M, Li J, Chen L, Shen C, Yang Z, Bei Y, Li L, Wu X, Zeng S, Xu F, Lin H (2020) Deep learning-based automated diagnosis of fungal keratitis with in vivo confocal microscopy images. Ann Transl Med 8(11):706. https://doi.org/10.21037/atm.2020.03.134
Xu F, Jiang L, He W, Huang G, Hong Y, Tang F, Lv J, Lin Y, Qin Y, Lan R, Pan X, Zeng S, Li M, Chen Q, Tang N (2021) The clinical value of explainable deep learning for diagnosing fungal keratitis using in vivo confocal microscopy images. Front Med Lausanne 14(8):797616. https://doi.org/10.3389/fmed.2021.797616
Xu F, Qin Y, He W, Huang G, Lv J, Xie X, Diao C, Tang F, Jiang L, Lan R, Cheng X, Xiao X, Zeng S, Chen Q, Cui L, Li M, Tang N (2021) A deep transfer learning framework for the automated assessment of corneal inflammation on in vivo confocal microscopy images. PLoS ONE 16(6):e0252653. https://doi.org/10.1371/journal.pone.0252653
Xie L, Zhong W, Shi W, Sun S (2006) Spectrum of fungal keratitis in north China. Ophthalmology 113(11):1943–1948. https://doi.org/10.1016/j.ophtha.2006.05.035
Jayalakshmi T, Santhakumaran A (2011) Statistical normalization and back propagation for classification. Int J Comput Theory Eng 3:89. https://doi.org/10.7763/IJCTE
Weiss K, Khoshgoftaar TM, Wang D (2016) A survey of transfer learning. J Big Data 3:9. https://doi.org/10.1186/s40537-016-0043-6
Deng J, Dong W, Socher R, Li LJ, Li K, Fei Fei L (2009) Imagenet: a large-scale hierarchical image database. IEEE Conf Comput Vis Pattern Recognit 2009:248–255. https://doi.org/10.1109/CVPR.2009.5206848
Szegedy C, Ioffe S, Vanhoucke V, Alemi AA (2017) Inception-v4, inception-resnet and the impact of residual connections on learning. Thirty first AAAI Conf Artif Intell 31:4278–4284. https://doi.org/10.1609/aaai.v31i1.11231
Karamizadeh S, Abdullah SM, Manaf AA, Zamani M, Hooman A (2020) An overview of principal component analysis. J Signal Inf Process 4:173–175. https://doi.org/10.4236/jsip.2013.43B031
Jolliffe IT, Cadima J (2016) Principal component analysis: a review and recent developments. Philos Trans R Soc Math Phys Eng Sci 374(2065):20150202. https://doi.org/10.1098/rsta.2015.0202
Ke G, Meng Q, Finley T, Wang T, Chen W, Wa M, Ye Q, Liu T (2017) Lightgbm: a highly efficient gradient boosting decision tree. Adv Neural Inf Process Syst 30:3146–3154. https://doi.org/10.5555/3294996.3295074
Duchi J, Hazan E, Singer Y (2011) Adaptive subgradient methods for online learning and stochastic optimization. J Mach Learn Res 12(7):68. https://doi.org/10.5555/1953048.2021068
Umemneku Chikere CM, Wilson K, Graziadio S, Vale L, Allen AJ (2019) Diagnostic test evaluation methodology: a systematic review of methods employed to evaluate diagnostic tests in the absence of gold standard—an update. PLoS ONE 14(10):e0223832. https://doi.org/10.1371/journal.pone.0223832
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44:837–845. https://doi.org/10.2307/2531595
Liu Z, Cao Y, Li Y, Xiao X, Qiu Q, Yang M, Zhao Y, Cui L (2020) Automatic diagnosis of fungal keratitis using data augmentation and image fusion with deep convolutional neural network. Comput Meth Programs Biomed 187:105019. https://doi.org/10.1016/j.cmpb.2019.105019
Hou H, Cao Y, Cui X, Liu Z, Xu H, Wang C, Zhang W, Zhang Y, Fang Y, Geng Y, Liang W, Cai T, Lai H (2021) Medical image management and analysis system based on web for fungal keratitis images. Math Biosci Eng 18(4):3667–3679. https://doi.org/10.3934/mbe.2021183
Funding
This study was supported by Guangxi Science and Technology Base and Talent Special Fund (Grant numbers [GuikeAD22035011]), Guangxi Clinical Ophthalmic Research Center (Grant numbers [GuikeAD19245193]), Guangxi Promotion of Appropriate Health Technologies Project (Grant numbers [S2019084]), and Guangxi Zhuang Autonomous Region Health Committee's Self-financing Project (Grant numbers [Z20201322]).
Author information
Authors and Affiliations
Contributions
The first draft of the manuscript was written by N.T., and all authors commented on previous versions of the manuscript. G.H., D.L., and L.J. performed the analyses. Q.C., W.H., F.T., Y.H., J.L., Y.Q., Y.L., and Q.L. contributed to data collection and measurements. Y.Q., R.L., and X.P. contributed to algorithm optimization. M.L. and P.L. were involved quality management. F.X. conceived the research, provided overall supervision, and undertook the responsibility of submitting the manuscript for publication. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
This study was approved by the ethics committee of the People’s Hospital of Guangxi Zhuang Autonomous Region, China. The approval number is KY-SY-2020–1.
Consent to participate
Informed consent was granted exemption by ethics committee of the People’s Hospital of Guangxi Zhuang Autonomous Region. All IVCM images applied in the study were completely anonymized. The submission does not include information that may identify the participant.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tang, N., Huang, G., Lei, D. et al. An artificial intelligence approach to classify pathogenic fungal genera of fungal keratitis using corneal confocal microscopy images. Int Ophthalmol 43, 2203–2214 (2023). https://doi.org/10.1007/s10792-022-02616-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-022-02616-8