Abstract
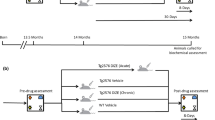
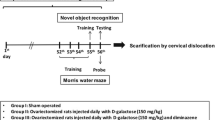
Accumulating evidence indicates that over-stimulation of angiotensin-converting enzyme 1 (ACE1) activity is associated with β-amyloid (Aβ) and phosphorylated tau (p-tau)-induced apoptosis, oxido-nitrosative neuroinflammatory stress and neurodegeneration in Alzheimer’s disease (AD). Alternatively, activation of the ACE2, the metalloprotease neprilysin (Neutral Endopeptidase; NEP) and the insulin-degrading enzyme (IDE) could oppose the effects of ACE1 activation. We aim to investigate the relationship between ACE1/ACE2/NEP/IDE and amyloidogenic/hyperlipidemic-lipid raft signaling in hyperlipidemic AD model. Induction of AD was performed in ovariectomized female rats with high-fat high fructose diet (HFFD) feeding after 4 weeks following d-galactose injection (150 mg/kg). The brain-penetrating ACE1 inhibitor perindopril (0.5 mg/kg/day, p.o.) was administered on a daily basis for 30 days. Perindopril significantly decreased hippocampal expression of ACE1 and increased expression of ACE2, NEP and IDE. Perindopril markedly decreased Aβ1–42, improved lipid profile and ameliorated the lipid raft protein markers caveolin1 (CAV1) and flotillin 1 (FLOT1). This was accompanied by decreased expression of p-tau and enhancement of cholinergic neurotransmission, coupled with decreased oxido-nitrosative neuroinflammatory stress, enhancement of blood–brain barrier (BBB) functioning and lower expression of the apoptotic markers glial fibrillary acidic protein (GFAP), Bax and β-tubulin. In addition, perindopril ameliorated histopathological damage and improved learning, cognitive and recognition impairment as well as depressive behavior in Morris water maze, Y maze, novel object recognition and forced swimming tests, respectively. Conclusively, perindopril could improve cognitive defects in AD rats, at least through activation of ACE2/NEP/IDE and inhibition of ACE1 and subsequent modulation of amyloidogenic/hyperlipidemic-lipid raft signaling and oxido-nitrosative stress.
















Similar content being viewed by others
References
Abareshi A, Anaeigoudari A, Norouzi F, Marefati N, Beheshti F, Saeedjalali M, Hosseini M (2019) The effects of captopril on lipopolysaccharide-induced sickness behaviors in rats. Vet Res 10:199–205. https://doi.org/10.30466/vrf.2018.90760.2198
AbdAlla S, El Hakim A, Abdelbaset A, Elfaramawy Y, Quitterer UJB (2015) Inhibition of ACE retards tau hyperphosphorylation and signs of neuronal degeneration in aged rats subjected to chronic mild stress. BioMed Res Int. https://doi.org/10.1155/2015/917156
Alawdi SH, El-Denshary ES, Safar MM, Eidi H, David M-O, Abdel-Wahhab MA (2017) Neuroprotective effect of nanodiamond in alzheimer’s disease rat model: a pivotal role for modulating NF-κB and STAT3 signaling. Mol Neurobiol 54:1906–1918. https://doi.org/10.1007/s12035-016-9762-0
Ali MRA-A, Abo-Youssef AMH, Messiha BAS, Khattab MM (2016) Tempol and perindopril protect against lipopolysaccharide-induced cognition impairment and amyloidogenesis by modulating brain-derived neurotropic factor, neuroinflammation and oxido-nitrosative stress. N-S Arch Pharmacol 389:637–656. https://doi.org/10.1007/s00210-016-1234-6
Amiya EJW (2016) Interaction of hyperlipidemia and reactive oxygen species: insights from the lipid-raft platform. World J Cardiol 8:689–694. https://doi.org/10.1007/s00210-016-1234-6
Amtul Z, Wang L, Westaway D, Rozmahel RJN (2010) Neuroprotective mechanism conferred by 17beta-estradiol on the biochemical basis of Alzheimer's disease. Neuroscience 169:781–786. https://doi.org/10.1016/j.neuroscience.2010.05.031
Bedard K, Krause K (2007) The NOX family of ROS-generating NADPH oxidases: physiology and pathophysiology. Physiol Rev 87:245–313. https://doi.org/10.1152/physrev.00044.2005
Begum G, Hamid K, Choudhuri MJJPS, Research (2015) Changes in lipid profile of rat plasma after chronic administration of Mallasindura (MSL)-an ayurvedic metallic preparation. J Pharm Sci and Res 7:123–126
Bevins RA, Besheer J (2006) Object recognition in rats and mice: a one-trial non-matching-to-sample learning task to study 'recognition memory'. Nat Protoc 1:1306–1311. https://doi.org/10.1038/nprot.2006.205
Brendel M et al (2018) Efficacy of chronic BACE1 inhibition in PS2APP mice depends on the regional Aβ deposition rate and plaque burden at treatment initiation. Theranostics 8:4957–4968. https://doi.org/10.7150/thno.27868
Brosnihan KB, Li P, Ganten D, Ferrario CM, Integrative Physiology C (1997) Estrogen protects transgenic hypertensive rats by shifting the vasoconstrictor-vasodilator balance of RAS. Am J Physiol 273:R1908–R1915. https://doi.org/10.1152/ajpregu.1997.273.6.R1908
Busquets O et al (2017) Long-term exposition to a high fat diet favors the appearance of β-amyloid depositions in the brain of C57BL/6J mice. A potential model of sporadic Alzheimer’s disease. Mech Ageing Dev 162:38–45. https://doi.org/10.1016/j.mad.2016.11.002
Calil CM, Marcondes FKJ (2006) The comparison of immobility time in experimental rat swimming models. Life Sci 79:1712–1719. https://doi.org/10.1016/j.lfs.2006.06.003
Calsolaro V, Edison P (2016) Neuroinflammation in Alzheimer's disease: current evidence and future directions. Alzheimer's Dement 12:719–732. https://doi.org/10.1016/j.jalz.2016.02.010
Canerina-Amaro A, Hernandez-Abad LG, Ferrer I, Quinto-Alemany D, Mesa-Herrera F, Ferri C, Marin RJFB (2017) Lipid raft ER signalosome malfunctions in menopause and Alzheimer’s disease. Front Biosci 9:111–126
Claflin KE, Grobe JLJ (2015) Control of energy balance by the brain renin-angiotensin system. Hypertens Brain 17:38. https://doi.org/10.1007/s11906-015-0549-x
Cocchetto DM, Bjornsson TDJ (1983) Methods for vascular access and collection of body fluids from the laboratory rat. J Pharm Sci 72:465–492. https://doi.org/10.1002/jps.2600720503
de Dios C, Bartolessis I, Roca-Agujetas V, Barbero-Camps E, Mari M, Morales A (2019) Oxidative inactivation of amyloid beta-degrading proteases by cholesterol-enhanced mitochondrial stress. Redox Biol 26:101283. https://doi.org/10.1016/j.redox.2019.101283
Do Carmo S, Cuello AC (2013) Modeling Alzheimer’s disease in transgenic rats. Mol Neurodegen 8:37. https://doi.org/10.1186/1750-1326-8-37
Dong Y-F et al (2011) Perindopril, a centrally active angiotensin-converting enzyme inhibitor, prevents cognitive impairment in mouse models of Alzheimer's disease. FASEB 25:2911–2920. https://doi.org/10.1096/fj.11-182873
Drury R, Wallington E (1983) Carleton's histological technique. Oxford University Press, New York
Erickson MA, Banks WA (2013) Blood–brain barrier dysfunction as a cause and consequence of Alzheimer's disease. J Cereb Blood Flow Metab 33:1500–1513. https://doi.org/10.1038/jcbfm.2013.135
Fischer R, Maier O (2015) Interrelation of oxidative stress and inflammation in neurodegenerative disease: role of TNF. Oxid Med Cell Longev. https://doi.org/10.1155/2015/610813
Fleming I (2006) Signaling by the angiotensin-converting enzyme. Circ Res 98:887–896. https://doi.org/10.1161/01.RES.0000217340.40936.53
Garcia LS et al (2008) Acute administration of ketamine induces antidepressant-like effects in the forced swimming test and increases BDNF levels in the rat hippocampus. Prog Neuropsychopharmacol Biol Psychiatry 32:140–144. https://doi.org/10.1016/j.pnpbp.2007.07.027
Gaudreault SB, Dea D, Poirier J (2004) Increased caveolin-1 expression in Alzheimer's disease brain. Neurobiol Aging 25:753–759. https://doi.org/10.1016/j.neurobiolaging.2003.07.004
Gebre AK, Altaye BM, Atey TM, Tuem KB, Berhe DF (2018) Targeting renin-angiotensin system against alzheimer’s disease. Front Pharmacol 9:440. https://doi.org/10.3389/fphar.2018.00440
Goyal BR, Patel M, Bhadada S (2011) Comparative evaluation of spironolactone, atenolol, metoprolol, ramipril and perindopril on diabetes induced cardiovascular complications in type 1 diabetes in rats. Int J Diabetes and Metab 19:11–18
Grimm M, Mett J, Stahlmann C, Haupenthal V, Zimmer V, Hartmann T (2013a) Neprilysin and Aβ clearance: impact of the APP intracellular domain in NEP regulation and implications in Alzheimer’s disease. Front Aging Neurosci. https://doi.org/10.3389/fnagi.2013.00098
Henderson L et al (2017) Enhanced phosphorylation of Bax and its translocation into mitochondria in the brains of individuals affiliated with Alzheimer’s disease. Open Neurol J 11:48–58
Hernández-Espinosa DR, Massieu L, Montiel T, Morán J (2019) Role of NADPH oxidase-2 in the progression of the inflammatory response secondary to striatum excitotoxic damage. J Neuroinflammation 16:91. https://doi.org/10.1186/s12974-019-1478-4
Herr D, Bekes I, Wulff C (2013) Local renin-angiotensin system in the reproductive system. Front Endocrinol. https://doi.org/10.3389/fendo.2013.00150
Hidaka N, Suemaru K, Takechi K, Li B, Araki H (2011) Inhibitory effects of valproate on impairment of Y-maze alternation behavior induced by repeated electroconvulsive seizures and c-Fos protein levels in rat brains. Acta Med Okayama 65:269–277. https://doi.org/10.18926/AMO/46853
Hirano T, Ran J, Adachi M (2006) Opposing actions of angiotensin II type 1 and 2 receptors on plasma cholesterol levels in rats. J Hypertension 24:103–108. https://doi.org/10.1097/01.hjh.0000198030.30095.98
Hua X, Lei M, Zhang Y, Ding J, Han Q, Hu G, Xiao M (2007) Long-term D-galactose injection combined with ovariectomy serves as a new rodent model for Alzheimer's disease. Life Sci 80:1897–1905. https://doi.org/10.1016/j.lfs.2007.02.030
Huang ML et al (2010) Upregulation of angiotensin-converting enzyme (ACE) 2 in hepatic fibrosis by ACE inhibitors. Clin Exp Pharmacol 37:1–6. https://doi.org/10.1111/j.1440-1681.2009.05302.x
Ibrahim WW, Abdelkader NF, Ismail HM, Khattab MM (2019) Escitalopram ameliorates cognitive impairment in D-galactose-injected ovariectomized rats: modulation of JNK, GSK-3β, and ERK signalling pathways. Sci Rep 9:10056. https://doi.org/10.1038/s41598-019-46558-1
Jawaid T, Jahan S, Kamal M (2015) A comparative study of neuroprotective effect of angiotensin converting enzyme inhibitors against scopolamine-induced memory impairments in rats. J Adv Pharm Technol Res 6:130–135. https://doi.org/10.4103/2231-4040.161514
Jha NK, Jha SK, Kumar D, Kejriwal N, Sharma R, Ambasta RK, Kumar P (2015) Impact of Insulin Degrading Enzyme And Neprilysin in Alzheimer's disease biology: characterization of putative cognates for therapeutic applications. J Alzheimers Dis 48:891–917. https://doi.org/10.3233/jad-150379
Kafkafi N, Lipkind D, Benjamini Y, Mayo CL, Elmer GI, Golani I (2003) SEE locomotor behavior test discriminates C57BL/6J and DBA/2J mouse inbred strains across laboratories and protocol conditions. Behav Neurosci 117:464–477. https://doi.org/10.1037/0735-7044.117.3.464
Kamel AS, Abdelkader NF, El-Rahman SSA, Emara M, Zaki HF, Khattab MM (2018) Stimulation of ACE2/ANG (1–7)/Mas axis by diminazene ameliorates Alzheimer’s disease in the D-galactose-ovariectomized rat model: role of PI3K/Akt pathway. Mol Neurobiol 55:8188–8202. https://doi.org/10.1007/s12035-018-0966-3
Kandeil MA, Hashem RM, Mahmoud MO, Hetta MH, Tohamy MA (2019) Zingiber officinale extract and omega-3 fatty acids ameliorate endoplasmic reticulum stress in a nonalcoholic fatty liver rat model. J Food Biochem. https://doi.org/10.1111/jfbc.13076
Kehoe PG, Wong S, Mulhim NA, Palmer LE, Miners JS (2016) Angiotensin-converting enzyme 2 is reduced in Alzheimer’s disease in association with increasing amyloid-β and tau pathology. Alzheimers Res Ther 8:50. https://doi.org/10.1186/s13195-016-0217-7
Khajuria DK, Razdan R, Mahapatra DR (2012) Description of a new method of ovariectomy in female rats. Revista brasileira de reumatologia 52:466–470
Kirsch C, Eckert GP, Mueller WE (2003) Statin effects on cholesterol micro-domains in brain plasma membranes. Biochem Pharmacol 65:843–856. https://doi.org/10.1016/S0006-2952(02)01654-4
Ledreux A, Wang X, Schultzberg M, Granholm A-C, Freeman LR (2016) Detrimental effects of a high fat/high cholesterol diet on memory and hippocampal markers in aged rats. Behav Brain Res 312:294–304. https://doi.org/10.1016/j.bbr.2016.06.012
Leszek J et al (2018) Late-life depression and Alzheimer disease: a potential synergy of the underlying mechanisms. Curr Med Chem 25:5389–5394. https://doi.org/10.2174/0929867323666160902152829
Li R, Cui J, Shen Y (2014) Brain sex matters: estrogen in cognition and Alzheimer’s disease. Mol Cell Endocrinol 389:13–21. https://doi.org/10.1016/j.mce.2013.12.018
Lin B, Hasegawa Y, Takane K, Koibuchi N, Cao C, Kim-Mitsuyama S (2016) High-fat-diet intake enhances cerebral amyloid angiopathy and cognitive impairment in a mouse model of Alzheimer's disease, independently of metabolic disorders. J Am Heart Assoc 5:e003154. https://doi.org/10.1161/JAHA.115.003154
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2− ΔΔCT method. Methods Mol (Clifton, NJ) 25:402–408. https://doi.org/10.1006/meth.2001.1262
Lowry OH, Rosebrough NJ, Farr AL (1951) Protein measurement with the Folin phenol reagent. J BiologChem 193:265–275
Lu Q, Ke Y, Cheng W, Wang Y, Yu C, Wen J (2008) Effects of perindopril and enalapril on atherosclerosis development of apolipoprotein E knockout mice. Zhonghua xin xue guan bing za zhi 36:350–354
Ma MW, Wang J, Zhang Q, Wang R, Dhandapani KM, Vadlamudi RK, Brann DW (2017) NADPH oxidase in brain injury and neurodegenerative disorders. Mol Neurodegener 12:7. https://doi.org/10.1186/s13024-017-0150-7
Martin L, Latypova X, Wilson CM, Magnaudeix A, Perrin M-L, Terro F (2013a) Tau protein phosphatases in Alzheimer's disease: the leading role of PP2A. Ageing Res Rev 12:39–49. https://doi.org/10.1016/j.arr.2012.06.008
Martin L, Latypova X, Wilson CM, Magnaudeix A, Perrin M-L, Yardin C, Terro F (2013b) Tau protein kinases: involvement in Alzheimer's disease. Ageing Res Rev 12:289–309. https://doi.org/10.1016/j.arr.2012.06.003
Mateos L, Ismail M-A-M, Gil-Bea F-J, Leoni V, Winblad B, Bjoerkhem I, Cedazo-Minguez A (2011) Upregulation of brain renin angiotensin system by 27-hydroxycholesterol in Alzheimer's disease. J Alzheimers Dis 24:669–679. https://doi.org/10.3233/JAD-2011-101512
Mathiasen JR, DiCamillo A (2010) Novel object recognition in the rat: a facile assay for cognitive function. Curr protoc pharmacol. https://doi.org/10.1002/0471141755.ph0559s49
McGuinn KP, Mahoney MG (2014) Lipid rafts and detergent-resistant membranes in epithelial keratinocytes. Methods Mol (Clifton, NJ) 1195:133–144. https://doi.org/10.1007/7651_2014_71
Miners J, Baig S, Tayler H, Kehoe P, Love S (2009) Neprilysin and insulin-degrading enzyme levels are increased in Alzheimer disease in relation to disease severity. J Neuropathol Exp Neurol 68:902–914. https://doi.org/10.1097/NEN.0b013e3181afe475
Miners JS, Van Helmond Z, Kehoe PG, Love S (2010) Changes with age in the activities of β-secretase and the Aβ-degrading enzymes neprilysin, insulin-degrading enzyme and angiotensin-converting enzyme. Brain Pathol 20:794–802. https://doi.org/10.1111/j.1750-3639.2010.00375.x
Mohamed HE, Abo EDM, Mesbah NM, Saleh SM, Ali AA, Sakr AT (2018) Raspberry ketone preserved cholinergic activity and antioxidant defense in obesity induced Alzheimer disease in rats. Biomed Pharmacother 107:1166–1174. https://doi.org/10.1016/j.biopha.2018.08.034
Mullins RJ, Diehl TC, Chia CW, Kapogiannis D (2017) Insulin resistance as a link between amyloid-beta and Tau pathologies in Alzheimer’s disease. Front Aging Neurosci 9:118. https://doi.org/10.3389/fnagi.2017.00118
Nade V, Kawale L, Valte K, Shendye N (2015) Cognitive enhancing effect of angiotensin-converting enzyme inhibitors and angiotensin receptor blockers on learning and memory. Indian J Pharmacol 47:263–269. https://doi.org/10.4103/0253-7613.157114
Ni J et al (2013) Activation of renin-angiotensin system is involved in dyslipidemia-mediated renal injuries in apolipoprotein E knockout mice and HK-2 cells. Lipids Health Dis 12:49. https://doi.org/10.1186/1476-511X-12-49
Niu L et al (2016) A high-sugar high-fat diet induced metabolic syndrome shows some symptoms of Alzheimer’s disease in rats. J Nutr Health Aging 20:509–513. https://doi.org/10.1007/s12603-015-0601-1
O'Hagan TS, Wharton W, Kehoe PG (2012) Interactions between oestrogen and the renin angiotensin system—potential mechanisms for gender differences in Alzheimer's disease. Am J Neurodegen Dis 1:266–279
Pendergrass KD, Pirro NT, Westwood BM, Ferrario CM, Brosnihan KB, Chappell MC (2008) Sex differences in circulating and renal angiotensins of hypertensive mRen. Lewis but not normotensive Lewis rats. Am J Physiol-Heart Circ Physiol 295:H10–H20. https://doi.org/10.1152/ajpheart.01277.2007
Popp J et al (2012) Cholesterol metabolism is associated with soluble amyloid precursor protein production in Alzheimer's disease. J Neurochem 123:310–316. https://doi.org/10.1111/j.1471-4159.2012.07893.x
Popp J et al (2013) Cerebral and extracerebral cholesterol metabolism and CSF markers of Alzheimer's disease. J Neurochem 86:37–42. https://doi.org/10.1111/j.1471-4159.2012.07893.x
Qin L et al (2004) NADPH oxidase mediates lipopolysaccharide-induced neurotoxicity and proinflammatory gene expression in activated microglia. J Biol Chem 279:1415–1421. https://doi.org/10.1074/jbc.M307657200
Quitterer U, AbdAlla S (2019) Improvements of symptoms of Alzheimer’s disease by inhibition of the angiotensin system. Pharmacol Res. https://doi.org/10.1016/j.phrs.2019.04.014
Rasband WS (1997–2018) ImageJ, U. S. National Institutes of Health, Bethesda, Maryland, USA, https://imagej.nih.gov/ij/
Roselli CE, Liu M, Hurn PD (2009) Brain aromatization: classic roles and new perspectives. Semin Reprod Med 27:207–217. https://doi.org/10.1055/s-0029-1216274
Rozen S, Skaletsky HJ (1998) Primer3. Code available at https://www-genome.wi.mit.edu/genome_software/other/primer3.html
Rushworth JV, Hooper NM (2010) Lipid rafts: linking alzheimer's amyloid-β production, aggregation, and toxicity at neuronal membranes. Int J Alzheimers Dis 2011:603052–603052. https://doi.org/10.4061/2011/603052
Sato A et al (2010) Antiobesity effect of eicosapentaenoic acid in high-fat/high-sucrose diet–induced obesity: importance of hepatic lipogenesis. Diabetes 59:2495–2504. https://doi.org/10.2337/db09-1554
Schengrund C-L (2010) Lipid rafts: keys to neurodegeneration. Brain Res Bull 82:7–17. https://doi.org/10.1016/j.brainresbull.2010.02.013
Selkoe DJ, Hardy J (2016) The amyloid hypothesis of Alzheimer's disease at 25 years. EMBO Mol Med 8:595–608. https://doi.org/10.15252/emmm.201606210
Shen J, Wu J (2015) Nicotinic cholinergic mechanisms in Alzheimer's disease. International review of neurobiology. Elsevier, Amsterdam, pp 275–292. https://doi.org/10.1016/bs.irn.2015.08.002
Slattery DA, Cryan JF (2012) Using the rat forced swim test to assess antidepressant-like activity in rodents. Nat Protoc 7:1009–1014. https://doi.org/10.1038/nprot.2012.044
Uddin M, Haque A, Mamun A, Iqbal M, Kabir M, Rony R, Begum M (2016) Searching the linkage between high fat diet and Alzheimer’s disease: a debatable proof stand for ketogenic diet to alleviate symptoms of Alzheimer’s patient with APOE ε4 allele. J Neurol Neurophysiol 7:1–9. https://doi.org/10.4172/2155-9562.1000397
Vorhees CV, Williams MT (2006) Morris water maze: procedures for assessing spatial and related forms of learning and memory. Nat Protoc 1:848–858. https://doi.org/10.1038/nprot.2006.116
Wang YJ et al (2016) Escitalopram attenuates beta-amyloid-induced tau hyperphosphorylation in primary hippocampal neurons through the 5-HT1A receptor mediated Akt/GSK-3beta pathway. Oncotarget 7:13328–13339. https://doi.org/10.18632/oncotarget.7798
Wood WG, Li L, Müller WE, Eckert GP (2014) Cholesterol as a causative factor in Alzheimer's disease: a debatable hypothesis. J Neurochem 129:559–572. https://doi.org/10.1111/jnc.12637
Wyssenbach A, Quintela T, Llavero F, Zugaza JL, Matute C, Alberdi E (2016) Amyloid β-induced astrogliosis is mediated by β1-integrin via NADPH oxidase 2 in Alzheimer's disease. Aging Cell 15:1140–1152. https://doi.org/10.1111/acel.12521
Yamada K et al (2011) Effect of a centrally active angiotensin converting enzyme inhibitor, perindopril, on cognitive performance in chronic cerebral hypo-perfusion rats. Brain Res 1421:110–120. https://doi.org/10.1016/j.brainres.2011.09.016
Yamamoto M, Kiyota T, Horiba M, Buescher JL, Walsh SM, Gendelman HE, Ikezu T (2007) Interferon-γ and tumor necrosis factor-α regulate amyloid-β plaque deposition and β-secretase expression in Swedish mutant APP transgenic mice. Am J Pathol 170:680–692
Yang W-N, Han H, Hu X-D, Feng G-F, Qian Y-H (2013) The effects of perindopril on cognitive impairment induced by d-galactose and aluminum trichloride via inhibition of acetylcholinesterase activity and oxidative stress. Pharmacol Biochem Behav 114:31–36. https://doi.org/10.1016/j.pbb.2013.10.027
Yang W, Shi L, Chen L, Zhang B, Ma K, Liu Y, Qian Y (2014) Protective effects of perindopril on d-galactose and aluminum trichloride induced neurotoxicity via the apoptosis of mitochondria-mediated intrinsic pathway in the hippocampus of mice. Brain Res Bull 109:46–53. https://doi.org/10.1016/j.brainresbull.2014.09.010
Zhao XS et al (2017) Hyperlipidemia-induced apoptosis of hippocampal neurons in apoE (−/−) mice may be associated with increased PCSK9 expression. Mol Med Rep 15:712–718. https://doi.org/10.3892/mmr.2016.6055
Zhu D, Shi J, Zhang Y, Wang B, Liu W, Chen Z, Tong Q (2011) Central angiotensin II stimulation promotes β amyloid production in Sprague Dawley rats. PLoS ONE 6:e16037. https://doi.org/10.1371/journal.pone.0016037
Zhu Y, Liu F, Zou X, Torbey M (2015) Comparison of unbiased estimation of neuronal number in the rat hippocampus with different staining methods. J Neurosci Methods 254:73–79. https://doi.org/10.1016/j.jneumeth.2015.07.022
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Messiha, B.A.S., Ali, M.R.A., Khattab, M.M. et al. Perindopril ameliorates experimental Alzheimer’s disease progression: role of amyloid β degradation, central estrogen receptor and hyperlipidemic-lipid raft signaling. Inflammopharmacol 28, 1343–1364 (2020). https://doi.org/10.1007/s10787-020-00724-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-020-00724-4