Abstract
An increasing body of data has shown that erythropoietin (EPO) plays multiple roles in inflammation control and immunoregulation. However, less attention has been given to its effects on lupus nephritis (LN). In this study, we investigated the therapeutic effects of EPO on LN in MRL/lpr mice, a well-studied animal model for lupus. MRL/lpr mice were randomly divided into an EPO and control group. Mice in the EPO group were treated with EPO; saline was given to the control group. Both groups were treated for 10 weeks. We analyzed the differences of general disease condition, histopathologic changes, Th lymphocytes subsets, and the expression of inflammatory factors of mice between the groups. Compared to the control group, mice in the EPO group showed less spleen hyperplasia, less urinary protein, and lower serum anti-dsDNA antibody; they also had lower renal histopathologic scores and less deposition of IgG/C3 within glomeruli. Moreover, Th1 and Th17 levels were decreased, while Th2 and Treg levels were increased in the spleen, and the expression of inflammatory cytokines decreased in both the spleen and kidneys. EPO increased Th2 and Treg lymphocytes, decreased Th1, Th17 lymphocytes in the spleen, and inhibited the inflammatory reactions in both the spleen and kidneys, thus ameliorating LN of MRL/lpr mice.





Similar content being viewed by others
References
Lisnevskaia, Larissa, Grainne Murphy, and David Isenberg. 2014. Systemic lupus erythematosus. The Lancet 384 (9957): 1878–1888. https://doi.org/10.1016/s0140-6736(14)60128-8.
Hahn, B.H., M.A. McMahon, A. Wilkinson, W.D. Wallace, D.I. Daikh, J.D. Fitzgerald, G.A. Karpouzas, J.T. Merrill, D.J. Wallace, J. Yazdany, R. Ramsey-Goldman, K. Singh, M. Khalighi, S.I. Choi, M. Gogia, S. Kafaja, M. Kamgar, C. Lau, W.J. Martin, S. Parikh, J. Peng, A. Rastogi, W. Chen, J.M. Grossman, and American College of Rheumatology. 2012. American College of Rheumatology guidelines for screening, treatment, and management of lupus nephritis. Arthritis Care Res (Hoboken) 64 (6): 797–808. https://doi.org/10.1002/acr.21664.
Mohan, C., and C. Putterman. 2015. Genetics and pathogenesis of systemic lupus erythematosus and lupus nephritis. Nature Reviews. Nephrology 11 (6): 329–341. https://doi.org/10.1038/nrneph.2015.33.
Feldman, C.H., L.T. Hiraki, J. Liu, M.A. Fischer, D.H. Solomon, G.S. Alarcon, W.C. Winkelmayer, and K.H. Costenbader. 2013. Epidemiology and sociodemographics of systemic lupus erythematosus and lupus nephritis among US adults with Medicaid coverage, 2000–2004. Arthritis and Rheumatism 65 (3): 753–763. https://doi.org/10.1002/art.37795.
Schwartz, N., B. Goilav, and C. Putterman. 2014. The pathogenesis, diagnosis and treatment of lupus nephritis. Current Opinion in Rheumatology 26 (5): 502–509. https://doi.org/10.1097/BOR.0000000000000089.
Tsokos, G.C. 2011. Systemic_Lupus_Erythematosus. The New England Journal of Medicine 365 (22): 2110–2121.
Malvar, A., P. Pirruccio, V. Alberton, B. Lococo, C. Recalde, B. Fazini, H. Nagaraja, D. Indrakanti, and B.H. Rovin. 2017. Histologic versus clinical remission in proliferative lupus nephritis. Nephrology, Dialysis, Transplantation 32 (8): 1338–1344. https://doi.org/10.1093/ndt/gfv296.
Costenbader, K.H., A. Desai, G.S. Alarcon, L.T. Hiraki, T. Shaykevich, M.A. Brookhart, E. Massarotti, B. Lu, D.H. Solomon, and W.C. Winkelmayer. 2011. Trends in the incidence, demographics, and outcomes of end-stage renal disease due to lupus nephritis in the US from 1995 to 2006. Arthritis and Rheumatism 63 (6): 1681–1688. https://doi.org/10.1002/art.30293.
Grande, J.P. 2011. Experimental models of lupus nephritis. Contributions to Nephrology 169: 183–197.
Andrews, B.S., R.A. Eisenberg, A.N. Theofilopoulos, S. Izui, C.B. Wilson, P.J. McConahey, E.D. Murphy, J.B. Roths, and F.J. Dixon. 1978. Spontaneous murine lupus-like syndromes. Clinical and immunopathological manifestations in several strains. The Journal of Experimental Medicine 148 (5): 1198–1215.
Kelley, V.E., S. Sneve, and S. Musinski. 1986. Increased renal thromboxane production in murine lupus nephritis. The Journal of Clinical Investigation 77 (1): 252–259.
Moore, E.M., R. Bellomo, and A.D. Nichol. 2011. Erythropoietin as a novel brain and kidney protective agent. Anaesthesia and Intensive Care 39 (3): 356–372.
Miyake, T., C.K. Kung, and E. Goldwasser. 1977. Purification of human erythropoietin. The Journal of Biological Chemistry 252 (15): 5558–5564.
Weidemann, A., and R.S. Johnson. 2009. Nonrenal regulation of EPO synthesis. Kidney International 75 (7): 682–688. https://doi.org/10.1038/ki.2008.687.
Lin, F.K., S. Suggs, C.H. Lin, J.K. Browne, R. Smalling, J.C. Egrie, K.K. Chen, G.M. Fox, F. Martin, Z. Stabinsky, et al. 1985. Cloning and expression of the human erythropoietin gene. Proceedings of the National Academy of Sciences of the United States of America 82 (22): 5.
Bahlmann, F.H., and D. Fliser. 2009. Erythropoietin and renoprotection. Current Opinion in Nephrology and Hypertension 18 (1): 15–20. https://doi.org/10.1097/MNH.0b013e32831a9dde.
Choi, D., S.A. Schroer, S.Y. Lu, L. Wang, X. Wu, Y. Liu, Y. Zhang, H.Y. Gaisano, K.U. Wagner, H. Wu, R. Retnakaran, and M. Woo. 2010. Erythropoietin protects against diabetes through direct effects on pancreatic beta cells. The Journal of Experimental Medicine 207 (13): 2831–2842. https://doi.org/10.1084/jem.20100665.
Brines, M., and A. Cerami. 2008. Erythropoietin-mediated tissue protection: Reducing collateral damage from the primary injury response. Journal of Internal Medicine 264 (5): 405–432. https://doi.org/10.1111/j.1365-2796.2008.02024.x.
Parsa, C.J., A. Matsumoto, Jihee Kim, Ryan U. Riel, Laura S. Pascal, G. Brant Walton, Richard B. Thompson, J.A. Petrofski, B.H. Annex, J.S. Stamler, and W.J. Koch. 2003. A novel protective effect of erythropoietin in the infarcted heart. Journal of Clinical Investigation 112 (7): 999–1007. https://doi.org/10.1172/jci18200.
Cuzzocrea, S., E. Mazzon, R. di Paola, T. Genovese, N.S. Patel, D. Britti, M. de Majo, A.P. Caputi, and C. Thiemermann. 2005. Erythropoietin reduces the degree of arthritis caused by type II collagen in the mouse. Arthritis and Rheumatism 52 (3): 940–950. https://doi.org/10.1002/art.20875.
Johnson, D.W., C. Forman, and D.A. Vesey. 2006. Novel renoprotective actions of erythropoietin: New uses for an old hormone. Nephrology (Carlton) 11 (4): 306–312. https://doi.org/10.1111/j.1440-1797.2006.00585.x.
Wu, H., B. Ren, J. Zhu, G. Dong, B. Xu, C. Wang, X. Zheng, and H. Jing. 2006. Pretreatment with recombined human erythropoietin attenuates ischemia-reperfusion-induced lung injury in rats. European Journal of Cardio-Thoracic Surgery 29 (6): 902–907. https://doi.org/10.1016/j.ejcts.2006.02.036.
Wu, H., G. Dong, H. Liu, B. Xu, D. Li, and H. Jing. 2009. Erythropoietin attenuates ischemia-reperfusion induced lung injury by inhibiting tumor necrosis factor-alpha and matrix metalloproteinase-9 expression. European Journal of Pharmacology 602 (2–3): 406–412. https://doi.org/10.1016/j.ejphar.2008.11.037.
Austin, H.A., 3rd, L.R. Muenz, K.M. Joyce, T.A. Antonovych, M.E. Kullick, J.H. Klippel, J.L. Decker, and J.E. Balow. 1983. Prognostic factors in lupus nephritis. Contribution of renal histologic data. The American Journal of Medicine 75 (3): 382–391.
Yuan, R., Y. Maeda, W. Li, W. Lu, S. Cook, and P. Dowling. 2008. Erythropoietin: A potent inducer of peripheral immuno/inflammatory modulation in autoimmune EAE. PLoS One 3 (4): e1924. https://doi.org/10.1371/journal.pone.0001924.
Chen, H., B. Luo, X. Yang, J. Xiong, Z. Liu, M. Jiang, R. Shi, C. Yan, Y. Wu, and Z. Zhang. 2014. Therapeutic effects of nonerythropoietic erythropoietin analog ARA290 in experimental autoimmune encephalomyelitis rat. Journal of Neuroimmunology 268 (1–2): 64–70. https://doi.org/10.1016/j.jneuroim.2014.01.006.
Wofsy, D., J.L. Hillson, and B. Diamond. 2013. Comparison of alternative primary outcome measures for use in lupus nephritis clinical trials. Arthritis and Rheumatism 65 (6): 1586–1591. https://doi.org/10.1002/art.37940.
Lee, S.W., K.H. Park, S. Park, J.H. Kim, S.Y. Hong, S.K. Lee, D. Choi, and Y.B. Park. 2013. Soluble receptor for advanced glycation end products alleviates nephritis in (NZB/NZW)F1 mice. Arthritis and Rheumatism 65 (7): 1902–1912. https://doi.org/10.1002/art.37955.
Zhang, L.Y., H. Li, Y.W. Wu, L. Cheng, Y.X. Yan, X.Q. Yang, F.H. Zhu, S.J. He, W. Tang, and J.P. Zuo. 2017. (5R)-5-hydroxytriptolide ameliorates lupus nephritis in MRL/lpr mice by preventing infiltration of immune cells. American Journal of Physiology. Renal Physiology 312 (4): F769–F777. https://doi.org/10.1152/ajprenal.00649.2016.
Shao, W.H., and P.L. Cohen. 2011. Disturbances of apoptotic cell clearance in systemic lupus erythematosus. Arthritis Research & Therapy 13 (1): 202.
Kiefer, K., M.A. Oropallo, M.P. Cancro, and A. Marshak-Rothstein. 2012. Role of type I interferons in the activation of autoreactive B cells. Immunology and Cell Biology 90 (5): 498–504. https://doi.org/10.1038/icb.2012.10.
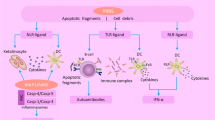
Luo, B., W. Gan, Z. Liu, Z. Shen, J. Wang, R. Shi, Y. Liu, Y. Liu, M. Jiang, Z. Zhang, and Y. Wu. 2016. Erythropoeitin signaling in macrophages promotes dying cell clearance and immune tolerance. Immunity 44 (2): 287–302. https://doi.org/10.1016/j.immuni.2016.01.002.
Lech, M., and H.J. Anders. 2013. The pathogenesis of lupus nephritis. J Am Soc Nephrol 24 (9): 1357–1366. https://doi.org/10.1681/ASN.2013010026.
Nowling, T.K., and G.S. Gilkeson. 2011. Mechanisms of tissue injury in lupus nephritis. Arthritis Research & Therapy 13 (6): 250.
Yap, D.Y., and K.N. Lai. 2015. Pathogenesis of renal disease in systemic lupus erythematosus—The role of autoantibodies and lymphocytes subset abnormalities. International Journal of Molecular Sciences 16 (4): 7917–7931. https://doi.org/10.3390/ijms16047917.
Tamiya, T., I. Kashiwagi, R. Takahashi, H. Yasukawa, and A. Yoshimura. 2011. Suppressors of cytokine signaling (SOCS) proteins and JAK/STAT pathways: Regulation of T-cell inflammation by SOCS1 and SOCS3. Arteriosclerosis, Thrombosis, and Vascular Biology 31 (5): 980–985. https://doi.org/10.1161/ATVBAHA.110.207464.
Okamoto, A., K. Fujio, N.H. Tsuno, K. Takahashi, and K. Yamamoto. 2012. Kidney-infiltrating CD4+ T-cell clones promote nephritis in lupus-prone mice. Kidney International 82 (9): 969–979. https://doi.org/10.1038/ki.2012.242.
Mitchell, S., J. Vargas, and A. Hoffmann. 2016. Signaling via the NFkappaB system. Wiley Interdisciplinary Reviews. Systems Biology and Medicine 8 (3): 227–241. https://doi.org/10.1002/wsbm.1331.
Hinz, M., and C. Scheidereit. 2014. The IkappaB kinase complex in NF-kappaB regulation and beyond. EMBO Reports 15 (1): 46–61. https://doi.org/10.1002/embr.201337983.
Ghosh, S., M.J. May, and E.B. Kopp. 1998. NF-kappa B and Rel proteins: Evolutionarily conserved mediators of immune responses. Annual Review of Immunology 16: 225–260. https://doi.org/10.1146/annurev.immunol.16.1.225.
Verstrepen, L., I. Carpentier, K. Verhelst, and R. Beyaert. 2009. ABINs: A20 binding inhibitors of NF-kappa B and apoptosis signaling. Biochemical Pharmacology 78 (2): 105–114. https://doi.org/10.1016/j.bcp.2009.02.009.
Lewis, M.J., S. Vyse, A.M. Shields, S. Boeltz, P.A. Gordon, T.D. Spector, P.J. Lehner, H. Walczak, and T.J. Vyse. 2015. UBE2L3 polymorphism amplifies NF-kappaB activation and promotes plasma cell development, linking linear ubiquitination to multiple autoimmune diseases. American Journal of Human Genetics 96 (2): 221–234. https://doi.org/10.1016/j.ajhg.2014.12.024.
Zheng, L., R. Sinniah, and S.I. Hsu. 2008. Pathogenic role of NF-kappaB activation in tubulointerstitial inflammatory lesions in human lupus nephritis. The Journal of Histochemistry and Cytochemistry 56 (5): 517–529. https://doi.org/10.1369/jhc.7A7368.2008.
Zheng, L., R. Sinniah, and S.I. Hsu. 2006. In situ glomerular expression of activated NF-kappaB in human lupus nephritis and other non-proliferative proteinuric glomerulopathy. Virchows Archiv 448 (2): 172–183. https://doi.org/10.1007/s00428-005-0061-9.
Alarcon-Segovia, D., M.E. Alarcon-Riquelme, M.H. Cardiel, F. Caeiro, L. Massardo, A.R. Villa, B.A. Pons-Estel, and Eritematoso Grupo Latinoamericano de Estudio del Lupus. 2005. Familial aggregation of systemic lupus erythematosus, rheumatoid arthritis, and other autoimmune diseases in 1,177 lupus patients from the GLADEL cohort. Arthritis and Rheumatism 52 (4): 1138–1147. https://doi.org/10.1002/art.20999.
You, Y., Y. Qin, X. Lin, F. Yang, J. Li, S.R. Sooranna, and L. Pinhu. 2015. Methylprednisolone attenuates lipopolysaccharide-induced Fractalkine expression in kidney of Lupus-prone MRL/lpr mice through the NF-kappaB pathway. BMC Nephrology 16: 148. https://doi.org/10.1186/s12882-015-0145-y.
Ding, Y., W. Liao, X. He, W. Xiang, and Q. Lu. 2016. CSTMP exerts anti-inflammatory effects on LPS-induced human renal proximal tubular epithelial cells by inhibiting TLR4-mediated NF-kappaB pathways. Inflammation 39 (2): 849–859. https://doi.org/10.1007/s10753-016-0315-5.
Jiang, T., F. Tian, H. Zheng, S.A. Whitman, Y. Lin, Z. Zhang, N. Zhang, and D.D. Zhang. 2014. Nrf2 suppresses lupus nephritis through inhibition of oxidative injury and the NF-kappaB-mediated inflammatory response. Kidney International 85 (2): 333–343. https://doi.org/10.1038/ki.2013.343.
Funding
This work was supported by a grant from The Doctor Initial Funding of Liaoning Province (No. 201501019).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic Supplementary Material
Supplementary Table 1
(PDF 118 kb)
Rights and permissions
About this article
Cite this article
Zhang, Z., Liu, D., Zhang, X. et al. Erythropoietin Treatment Ameliorates Lupus Nephritis of MRL/lpr Mice. Inflammation 41, 1888–1899 (2018). https://doi.org/10.1007/s10753-018-0832-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-018-0832-5