Abstract
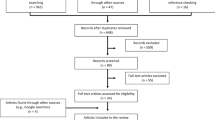
Epidemiologic and animal data indicate that night shift work might increase the risk for breast cancer. We evaluated the association of night work with different clinical types of breast cancer in a population based case–control study (MCC-Spain study) taking into account chronotype, an individual characteristic that may relate to night shift work adaptation. Lifetime occupational history was assessed by face-to-face interviews and shift work information was available for 1708 breast cancer cases and 1778 population controls from 10 Spanish regions, enrolled from 2008 to 2013. We evaluated three shift work domains, including shift work type (permanent vs rotating), lifetime cumulative duration and frequency. We estimated odds ratios (OR) for night work compared to day work using unconditional logistic regression models adjusting for confounders. Having ever worked permanent or rotating night shift was associated with an increased risk for breast cancer compared to day workers [odds ratio (OR) 1.18; 95 % CI 0.97, 1.43]. Chronotype was differentially associated with breast cancer depending on the duration of night shift work. Risk was higher in women with invasive tumors (OR 1.23; 95 % CI 1.00, 1.51) and for estrogen and progestagen positive tumors among premenopausal women (OR 1.44; 95 % CI 1.05, 1.99). Having ever performed night shift was associated with a small increased risk for breast cancer and especially in subgroups of women with particular hormone related characteristics.
Similar content being viewed by others
References
Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM. Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. Int J Cancer. 2010;127(12):2893–917.
Colditz GB, Baer HJ, Tamimi RM. Breast cancer. In: Schottenfeld D, Fraumeni JF, editors. Cancer epidemiology and prevention, 3rd ed. New York: Oxford University Press; 2006. p. 995–1012.
Bonde JP, Hansen J, Kolstad HA, Mikkelsen S, Olsen JH, Blask DE, Harma M, Kjuus H, de Koning HJ, Olsen J, Moller M, Schernhammer ES, Stevens RG, Akerstedt T. Work at night and breast cancer-report on evidence-based options for preventive actions. Scand J Work Environ Health. 2012;38(4):380–90.
Costa G. Shift work and health: current problems and preventive actions. Saf Health Work. 2010;1(2):112–23.
IARC. Painting, firefighting and shiftwork. IARC Monogr. 2010;98:561–764.
Ijaz S, Verbeek J, Seidler A, Lindbohm ML, Ojajarvi A, Orsini N, Costa G, Neuvonen K. Night-shift work and breast cancer—a systematic review and meta-analysis. Scand J Work Environ Health. 2013;39(5):431–47.
Jia Y, Lu Y, Wu K, Lin Q, Shen W, Zhu M, Huang S, Chen J. Does night work increase the risk of breast cancer? A systematic review and meta-analysis of epidemiological studies. Cancer Epidemiol. 2013;37(3):197–206.
Kamdar BB, Tergas AI, Mateen FJ, Bhayani NH, Oh J. Night-shift work and risk of breast cancer: a systematic review and meta-analysis. Breast Cancer Res Treat. 2013;138(1):291–301.
Wang F, Yeung KL, Chan WC, Kwok CC, Leung SL, Wu C, Chan EY, Yu IT, Yang XR, Tse LA. A meta-analysis on dose–response relationship between night shift work and the risk of breast cancer. Ann Oncol. 2013;24(11):2724–32.
Stevens RG, Hansen J, Costa G, Haus E, Kauppinen T, Aronson KJ, Castano-Vinyals G, Davis S, Frings-Dresen MH, Fritschi L, Kogevinas M, Kogi K, Lie JA, Lowden A, Peplonska B, Pesch B, Pukkala E, Schernhammer E, Travis RC, Vermeulen R, Zheng T, Cogliano V, Straif K. Considerations of circadian impact for defining ‘shift work’ in cancer studies: IARC working group report. Occup Environ Med. 2010;68(2):154–62.
Roenneberg T, Wirz-Justice A, Merrow M. Life between clocks: daily temporal patterns of human chronotypes. J Biol Rhythms. 2003;18(1):80–90.
Erren TC. Shift work and cancer research: can chronotype predict susceptibility in night-shift and rotating-shift workers? Occup Environ Med. 2013;70(4):283–4.
Fritschi L, Glass DC, Heyworth JS, Aronson K, Girschik J, Boyle T, Grundy A, Erren TC. Hypotheses for mechanisms linking shiftwork and cancer. Med Hypotheses. 2011;77(3):430–6.
Hansen J, Lassen CF. Nested case-control study of night shift work and breast cancer risk among women in the Danish military. Occup Environ Med. 2012;69(8):551–6.
Ramin C, Devore EE, Pierre-Paul J, Duffy JF, Hankinson SE, Schernhammer ES. Chronotype and breast cancer risk in a cohort of US nurses. Chronobiol Int. 2013;30(9):1181–6.
Yang XR, Sherman ME, Rimm DL, Lissowska J, Brinton LA, Peplonska B, Hewitt SM, Anderson WF, Szeszenia-Dabrowska N, Bardin-Mikolajczak A, Zatonski W, Cartun R, Mandich D, Rymkiewicz G, Ligaj M, Lukaszek S, Kordek R, Garcia-Closas M. Differences in risk factors for breast cancer molecular subtypes in a population-based study. Cancer Epidemiol Biomarkers Prev. 2007;16(3):439–43.
Menegaux F, Truong T, Anger A, Cordina-Duverger E, Lamkarkach F, Arveux P, Kerbrat P, Fevotte J, Guenel P. Night work and breast cancer: a population-based case-control study in France (the CECILE study). Int J Cancer. 2013;132(4):924–31.
Ramin C, Devore EE, Wang W, Pierre-Paul J, Wegrzyn LR, Schernhammer ES. Night shift work at specific age ranges and chronic disease risk factors. Occup Environ Med. 2015;72(2):100–7.
Castano-Vinyals G, Aragones N, Perez-Gomez B, Martin V, Llorca J, Moreno V, Altzibar JM, Ardanaz E, de Sanjose S, Jimenez-Moleon JJ, Tardon A, Alguacil J, Peiro R, Marcos-Gragera R, Navarro C, Pollan M, Kogevinas M. Population-based multicase–control study in common tumors in Spain (MCC-Spain): rationale and study design. Gac Sanit. 2015;29(4):308–15.
Weng HY, Hsueh YH, Messam LL, Hertz-Picciotto I. Methods of covariate selection: directed acyclic graphs and the change-in-estimate procedure. Am J Epidemiol. 2009;169(10):1182–90.
White IR, Royston P, Wood AM. Multiple imputation using chained equations: issues and guidance for practice. Stat Med. 2011;30(4):377–99.
Fritschi L, Erren TC, Glass DC, Girschik J, Thomson AK, Saunders C, Boyle T, El-Zaemey S, Rogers P, Peters S, Slevin T, D’Orsogna A, de Vocht F, Vermeulen R, Heyworth JS. The association between different night shiftwork factors and breast cancer: a case–control study. Br J Cancer. 2013;109(9):2472–80.
Grundy A, Richardson H, Burstyn I, Lohrisch C, SenGupta SK, Lai AS, Lee D, Spinelli JJ, Aronson KJ. Increased risk of breast cancer associated with long-term shift work in Canada. Occup Environ Med. 2013;70(12):831–8.
Hansen J, Stevens RG. Case–control study of shift-work and breast cancer risk in Danish nurses: impact of shift systems. Eur J Cancer. 2012;48(11):1722–9.
Lie JA, Kjuus H, Zienolddiny S, Haugen A, Stevens RG, Kjaerheim K. Night work and breast cancer risk among Norwegian nurses: assessment by different exposure metrics. Am J Epidemiol. 2011;173(11):1272–9.
Pesch B, Harth V, Rabstein S, Baisch C, Schiffermann M, Pallapies D, Bonberg N, Heinze E, Spickenheuer A, Justenhoven C, Brauch H, Hamann U, Ko Y, Straif K, Bruning T. Night work and breast cancer—results from the German GENICA study. Scand J Work Environ Health. 2010;36(2):134–41.
Knutsson A, Alfredsson L, Karlsson B, Akerstedt T, Fransson EI, Westerholm P, Westerlund H. Breast cancer among shift workers: results of the WOLF longitudinal cohort study. Scand J Work Environ Health. 2013;39(2):170–7.
Li W, Ray RM, Thomas DB, Davis S, Yost M, Breslow N, Gao DL, Fitzgibbons ED, Camp JE, Wong E, Wernli KJ, Checkoway H. Shift work and breast cancer among women textile workers in Shanghai, China. Cancer Causes Control. 2015;26(1):143–50.
Pronk A, Ji BT, Shu XO, Xue S, Yang G, Li HL, Rothman N, Gao YT, Zheng W, Chow WH. Night-shift work and breast cancer risk in a cohort of Chinese women. Am J Epidemiol. 2010;171(9):953–9.
Schernhammer ES, Kroenke CH, Laden F, Hankinson SE. Night work and risk of breast cancer. Epidemiology. 2006;17(1):108–11.
Folkard S. Do permanent night workers show circadian adjustment? A review based on the endogenous melatonin rhythm. Chronobiol Int. 2008;25(2):215–24.
Lie JA, Roessink J, Kjaerheim K. Breast cancer and night work among Norwegian nurses. Cancer Causes Control. 2006;17(1):39–44.
Schernhammer ES, Laden F, Speizer FE, Willett WC, Hunter DJ, Kawachi I, Colditz GA. Rotating night shifts and risk of breast cancer in women participating in the nurses’ health study. J Natl Cancer Inst. 2001;93(20):1563–8.
Archer SN, Robilliard DL, Skene DJ, Smits M, Williams A, Arendt J, von Schantz M. A length polymorphism in the circadian clock gene Per3 is linked to delayed sleep phase syndrome and extreme diurnal preference. Sleep. 2003;26(4):413–5.
Lie JA, Kjuus H, Zienolddiny S, Haugen A, Kjaerheim K. Breast cancer among nurses: is the intensity of night work related to hormone receptor status? Am J Epidemiol. 2013;178(1):110–7.
Rabstein S, Harth V, Pesch B, Pallapies D, Lotz A, Justenhoven C, Baisch C, Schiffermann M, Haas S, Fischer HP, Heinze E, Pierl C, Brauch H, Hamann U, Ko Y, Bruning T. Night work and breast cancer estrogen receptor status–results from the German GENICA study. Scand J Work Environ Health. 2013;39(5):448–55.
Terry PD, Rohan TE. Cigarette smoking and the risk of breast cancer in women: a review of the literature. Cancer Epidemiol Biomark Prev. 2002;11(10 Pt 1):953–71.
Petrausch U, Pestalozzi BC. Distinct clinical and prognostic features of invasive lobular breast cancer. Breast Dis. 2008;30:39–44.
Filipski E, King VM, Li X, Granda TG, Mormont MC, Liu X, Claustrat B, Hastings MH, Levi F. Host circadian clock as a control point in tumor progression. J Natl Cancer Inst. 2002;94(9):690–7.
Hansen J. 0200 Night shiftwork and breast cancer survival in Danish women. Occup Environ Med. 2014;71(Suppl 1):A26.
Acknowledgments
We would like to acknowledge the participants in the study, the data manager and all the interviewers and technicians involved in the data collection. We would also like to thank Juan Alguacil, Miguel Santibañez, Victor Moreno and Laura Costas for their valuable comments in the text.
Funding
The study was funded by the “Accion Transversal del Cancer”, approved on the Spanish Ministry Council on the 11th October 2007, by the Instituto de Salud Carlos III-FEDER (PI08/1770, PI08/0533, PI08/1359, PI09/00773-Cantabria, PI09/01286-León, PI09/01903-Valencia, PI09/02078-Huelva, PI09/01662-Granada, PI11/01403, PI11/01889-FEDER, PI11/00226, PI11/01810, PI11/02213, PI12/00488, PI12/00265, PI12/01270, PI12/00715, PI12/00150), by the Fundación Marqués de Valdecilla (API 10/09), by the ICGC International Cancer Genome Consortium CLL (The ICGC CLL-Genome Project is funded by Spanish Ministerio de Economía y Competitividad (MINECO) through the Instituto de Salud Carlos III (ISCIII) and Red Temática de Investigación del Cáncer (RTICC) del ISCIII (RD12/0036/0036)), by the Junta de Castilla y León (LE22A10-2), by the Consejería de Salud of the Junta de Andalucía (2009-S0143), by the Conselleria de Sanitat of the Generalitat Valenciana (AP_061/10), by the Recercaixa (2010ACUP 00310), by the European Commission Grants FOOD-CT-2006-036224-HIWATE, by the Spanish Association Against Cancer (AECC) Scientific Foundation, by the Catalan Government DURSI Grant 2009SGR1489, and by a predoctoral Grant PFIS (FI09/00385).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Papantoniou, K., Castaño-Vinyals, G., Espinosa, A. et al. Breast cancer risk and night shift work in a case–control study in a Spanish population. Eur J Epidemiol 31, 867–878 (2016). https://doi.org/10.1007/s10654-015-0073-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10654-015-0073-y